27 December 2021: Clinical Research
A Retrospective Single-Center Study of 23 Patients to Compare Gait Before and After Total Hip Arthroplasty Using the S-ROM Modular Hip System
Jacqueline Bahr1BCDEF, Dietmar Rosental2C, Tim Classen3E, Sonja Krebs1E, Marcus Jäger4AG*DOI: 10.12659/MSM.934558
Med Sci Monit 2021; 27:e934558
Abstract
BACKGROUND: This retrospective study used the Harris hip score (HHS) and range of motion (ROM) to compare gait before and after total hip arthroplasty using the modular S-ROM® hip prosthesis in 23 patients treated at a single center.
MATERIAL AND METHODS: For this study, 23 patients with severe hip deformity, who were treated with a total hip replacement using the S-ROM® modular hip system by DePuy® in the period from 2003 until 2008, underwent a 3-dimensional gait analysis before and after surgery. Values were compared with a validated data set of healthy subjects. Gait analysis took place using 8 infrared cameras (50 Hz), 2 force platforms of Advanced Medical Technology, Inc. (AMTI)®, and the Vicon® 512 system. The HHS and ROM of the hip joint were determined preoperatively and postoperatively. The follow-up period was 16.7±15.2 months.
RESULTS: A healthy gait pattern is characterized by an even stride length of both legs in relation to body height and relative symmetry of certain gait phases. These characteristics are influenced by the range of motion of the hip joint and by pelvic tilt. Symmetry could be achieved postoperatively in the stance phase and in the single-leg stance phase. However, the gait phases could not normalize. HHS and ROM improved postoperatively.
CONCLUSIONS: The findings from this retrospective study showed that ROM and HHS significantly improved following THA with the S-ROM® hip prosthesis, but that gait did not completely return to normal.
Keywords: Arthroplasty, Replacement, Hip, Biomechanical Phenomena, gait analysis, Female, Hip Prosthesis, Humans, Male, Prosthesis Design
Background
The aim of endoprosthetic joint replacement is to free patients from pain and to restore mobility so that they can cope with everyday stresses and strains and, in young patients, regain the ability to work [1]. Often, amazing athletic performance can be achieved again [1]. Total hip arthroplasty (THA) is successful in reducing pain and hip-related symptoms [2]. The hip disability and Osteoarthritis Outcome Score (HOOS) function in activities of daily living (ADL) and function in sports and recreation subscales also displays large effect sizes, indicating that surgery has a huge impact not only on pain and symptoms, but also on patient-reported function [2].
There are several studies that have shown an improvement in gait after THA [2–8]. In these studies, deformities were excluded and non-modular prosthesis systems were used [4,6,7,9]. The S-ROM prosthesis was developed for primary arthroplasty of deformities of the hip joint and is widely used [10–12]. Gait analyses of primary arthroplasty patients with deformities have not yet been published.
The aim of this study was to find out to what extent the gait pattern of patients with complex hip deformities approximates, after implantation of a modular hip endoprosthesis of the S-ROM type, the gait pattern of a healthy comparison collective, and in what aspects of the gait pattern the values of the comparison collective can be achieved.
The standard follow-up of patients after THA takes the form of X-ray checks and clinical examination, in which both passive and active mobility is tested [13]. Each clinical examination of the hip joint also includes a visual assessment of gait pattern [14,15]. The gait pattern reflects the function of the joint under everyday load. This examination technique is very subjective and therefore not comparable but can be objectified through 3-D analysis of gait [16]. This procedure is thus being adopted in an increasing number of clinical studies [5,6,17].
The DePuy S-ROM system is a cementless modular implant system introduced in 1984 [18]. Innovations include a fully polished distal stem, different neck lengths and offset variations on the stem, the possibility of independent rotational alignment of the stem and sleeve, and a variety of different proximal sleeves to ensure optimal adaptation to the proximal femur [10]. Bone ingrowth into a cementless prosthesis can be achieved by both porous and hydroxyapatite coatings [19]. Bolognesi et al compared the performance of a hydroxyapatite-coated proximal sleeve and a porous bead-coated sleeve in 52 patients performed with an S-ROM stem in a revision arthroplasty and found no difference with respect to bone ingrowth [19]. In this study, the S-ROM stem with a porous coated sleeve was used.
Distal stability without fixation is provided by the ribs and polished distal portion of the prosthesis. The slotting in the coronal plane helps to reduce bending stiffness. It also prevents distal fixation, which can lead to stress shielding. The proximal sleeves have a stepped surface to load the bone in compression and protect it from unphysiological ring stress. The steps counteract subsidence of the prosthesis without having to rely on a collar [10].
The independence of the sleeve and stem allows correction of excessive anteversion, as occurs with dysplasia and retroversion deformities, in revision hip arthroplasty. The fluted distal segment provides stability when a corrective osteotomy is required. The stem is a versatile tool in THA with unusual deformities and in revision surgery [20].
The S-ROM system is a popular choice for revision arthroplasty and proximal femoral deformity due to its modularity [21]. With independent rotational alignment of stem and sleeve and a variety of different proximal sleeves, optimal adaptation to the proximal femur can be ensured and can thus respond to a highly modified anatomy [22]. In this study, the S-ROM system was used as the primary implant system for complex hip joint deformities.
With the help of today’s data processing methods, elaborate and precise procedures of gait analysis methodology are possible [23]. Spatiotemporal parameters such as step length, step speed, step time fluctuations, and average step times, as well as joint position in space, angular velocity and acceleration, can be reliably determined parallel to electromyographic (EMG) activities in relation to the stance and swing phase [23]. Kinematic data collection can be carried out with various functional analysis systems, film-video (eg, Vicon, Oxford Metrics) optoelectrical systems or goniometry [23].
In the 1960s, a system of observational gait analysis was developed in Los Angeles at Rancho Los Amigos National Rehabilitation Center under the direction of Jacqueline Perry [16]. Motion analysis was initially performed using video cameras and video recorders and was gradually supplemented by kinematic and kinetic measurement systems, such as infrared ViconTM® cameras, floor-embedded force plates, and EMG. Her book “Ganganalyse”, published in 1992, has since become the standard work on instrumental gait analysis [16].
For the gait analysis system by Vicon®, (Oxford Metrics Ltd. Oxford, Great Britain) used in this study, a very high reliability level has been demonstrated before [24].
The American Academy of Orthopedic Surgeons and the Société Internationale de Chirurgie Orthopèdique et de Traumatologie recommend that an assessment of clinical complications, a physical examination of the hip, radiographic studies, and an assessment of well-being (pain, gait, some activities of daily living, and overall satisfaction) as reported by the patient to be included in any outcome studies. A disease-specific measure should be included in all studies of outcome of the hip arthroplasty [25]. Harris introduced a rating scale with a maximum of 100 points, including the domains of pain, function, deformity, and motion [26]. The Harris hip score was compared with the Larson and Shepard system, and it was found to be “reproducible and reasonably objective” [26]. Therefore, the Harris hip score is one of the most widely used scoring systems [27].
Material and Methods
The Medical Ethics Committee of the University of Duisburg-Essen, Germany, approved the study on the following basis:
Gait analysis and clinical examinations are performed. Data from patient records and data from X-rays are collected and evaluated, with the aim of finding out whether reconstruction of the anatomical conditions at the hip joint leads to more physiological movement patterns, whether, in the case of a measurable improvement in passive mobility, this is also exploited under the everyday load of walking or whether the old movement pattern continues and whether consequences for rehabilitation can be derived from the results.
The patients were informed about the study and the procedure of the gait analysis during the presurgical preparations and agreed to participate by giving their written consent.
Patients were selected from the outpatient clinic population in case of matching the inclusion criteria listed below and being willing to participate.
The data were anonymized and forwarded to a statistician at the University Hospital in Düsseldorf for statistical analysis. Access to the data was given to the first author of the study and to the employees of the gait laboratory.
We defined inclusions criteria for this investigation as follows:
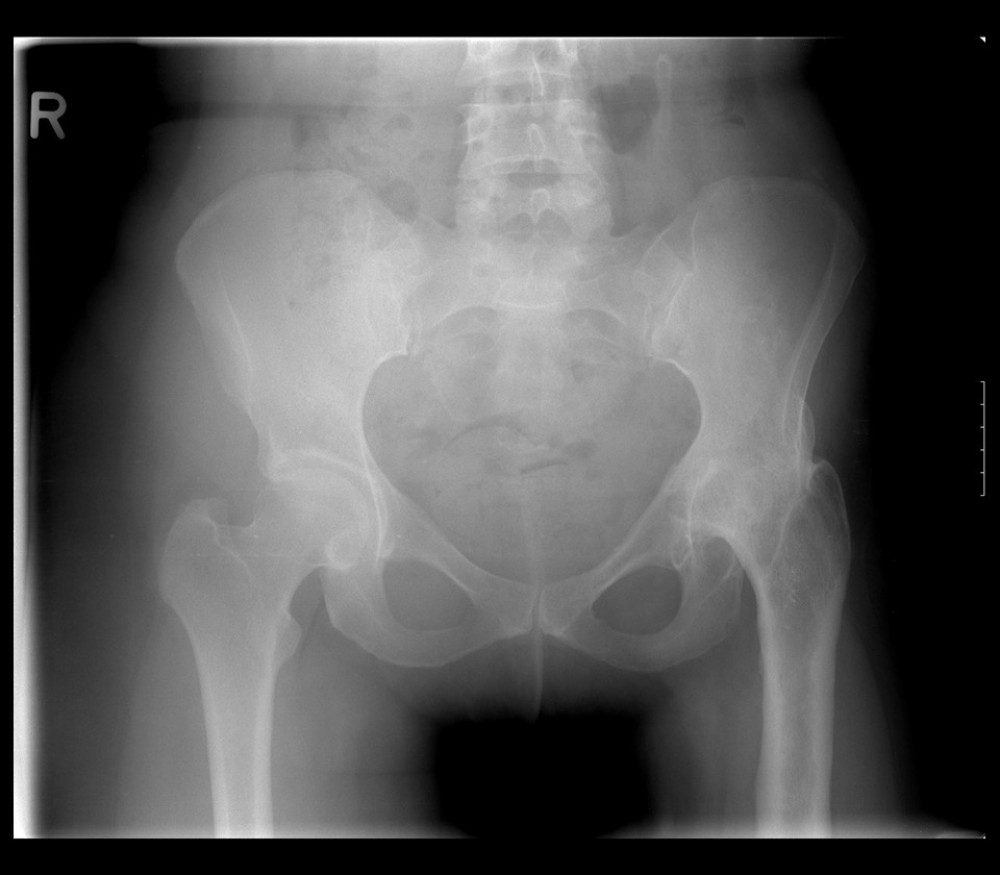
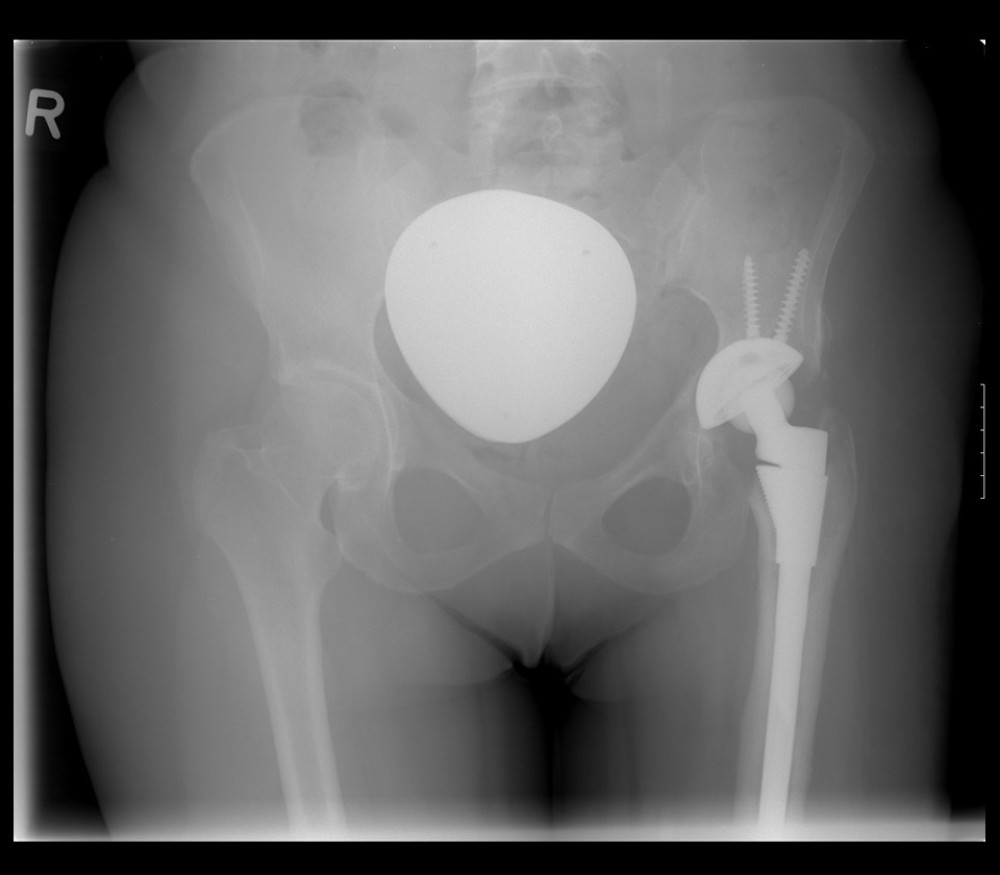
The indication for THA on one site together with a complex deformity, the use of an S-ROM shaft system, surgery to be performed by the corresponding author. Figure 1 shows the preoperative X-ray of a patient treated in this study. Figure 2 shows the postoperative X-ray of this patient. Exclusion criteria were: Patients over the age of 70, previous major orthopedic surgery in the lower limbs with exception of the hip joint to be operated on, other lower-extremity joint pain or severe back pain, rheumatoid arthritis, neurologic disease and/or other conditions affecting walking ability.
In the period from 2003 until 2008 23 Patients matched those criteria.
Before and after surgery, with a definition of after surgery as on average 16.7 months (±15.2 standard deviation), a clinical examination including ROM, X-ray, HHS, and gait analysis was performed.
Gait analysis took place using 8 infrared cameras (50 Hz) by Vicon® (Oxford Metrics Ltd. Oxford, Great Britain) and 2 force platforms by Advanced Medical Technology, Inc., Watertown, USA (AMTI)® situated at the mid-point of the 10-m-long level walkway and the Vicon 512 software system [28]. 22 Pearl Hard Reflective Marker by Vicon Oxford Metrix [29] in a diameter of 25 mm were fixed with double-sided tape at the points described by Kadaba et al [30]. Spatiotemporal gait parameters and kinetic and kinematic parameters were obtained.
Spatiotemporal gait parameters include relative stride length, as well as the duration of the stance phase, single-leg stance phase, and loading response. The duration of the gait phases is given as a percentage of the gait cycle.
The kinematic parameters include the angular position of the hip joint as well as the pelvic tilt and the position of the pelvis in relation to the position of the upper body at each phase of the gait cycle. The values are given in angular degrees. The measurement was made in sagittal, frontal, and transversal planes. The maximum measured value and the ROM were used for evaluation.
The kinetic parameters include the generated and absorbed power, which is determined by means of force plates and attributed to the hip joint, the knee joint and the ankle joint on the basis of the acting force vector.
The affected side was compared preoperatively with postoperatively, the affected side preoperatively with the opposite side preoperatively, the affected side postoperatively with the opposite side postoperatively, and the affected side and the opposite side with the healthy control group both preoperatively and postoperatively.
The HHS is a disease-specific test used to provide an evaluation system for various hip disabilities and methods of treatment [26]. This rating system is staff-administered, not self-administered. The Harris hip score gives a maximum of 100 points and the domains include pain, function, deformity, and motion. In the HHS, pain and function are the 2 basic considerations and receive the greatest weighting, with 44 and 20 points, respectively. ROM and deformity are seldom of primary importance and thus receive 5 and 4 points, respectively. Function is subdivided into activities of daily living (14 points) and gait (33 points) [27].
The Harris hip score was assessed and the preoperative and postoperative passive ROM of the hip joint were measured on the day of gait analysis.
The Wilcoxon test for dependent samples was used for the comparison between preoperative and postoperative data. It indicates whether 2 dependent samples differ significantly in their central difference [31]. For the comparison of the patients with the normal collective, the Mann-Whitney U test for independent samples was used. This test tests the null hypothesis that 2 independent samples come from ‘identically shaped’ distributed populations with identical median values [31].
SPSS Predictive Analysis Software statistics 18 for Windows by International Business Machines Corporation (SPSS PASW by IBM) was used for the statistical analyses.
A significance level α≤0.05 is assumed. The maximum tolerable risk for a wrong decision in favor of the alternative hypothesis is thus 5%. The significance level α is compared with the calculated p-value. If p≤0.05, the null hypothesis of equality can be discarded [31].
Results
SPATIOTEMPORAL GAIT PARAMETERS:
The one-legged stance phase of the affected side preoperatively was significantly shorter compared with the healthy control group (35.95%±3.14% vs 40.27%±1.37% [P<0.001]). The step length was also shorter (0.33±0.04 m vs 0.39±0.02 m). The loading response was significantly longer (12.2%±3.18% vs 9.69%±1.16% [P<0.001]). The total stance phase of the affected side shows normal values preoperatively (Table 1).
On the affected side, the one-legged stance phase was observed to be longer postoperatively (37-7%±3.32 vs 35.95%±3.14% [P=0.004]). Loading response, total stance and relative step length did not significantly changed when comparing preoperatively to postoperatively (Table 1). The values of the healthy control group could not be achieved.
The single-leg stance phase and the relative step length were shorter, the total stance phase and the loading response were longer on the affected side (cf. Table 1).
Compared with the opposite side the affected side showed that stance phase and the one-legged stance were preoperatively shorter (61.34%±2.03% and 37.70%±3.32% [P =0.001]) than on the opposite side (63.97%±3.04% and 38.91%±4.02% respectively [P <0.001]). Postoperatively there was no significant difference between the 2 sides (61.34%±2.03% and 37.70%±3.32% on the operated side compared to 62.29%±3.78% and 38.86%±2.09% on the opposite side) (Table 1).
The opposite side displayed longer stance (
KINEMATICS:
In the kinematic examination of the pelvis, pelvic tilt describes the relative movement of the pelvis in 3 dimensions. For anatomical reasons, it is not possible to perform an isolated pelvic tilt of one side. The opposite side automatically undergoes the same tilting of the reference side, so that only the values of the affected side are examined during evaluation. Differences in the measured values of the opposite side are evaluated as measurement inaccuracy.
In the sagittal plane, preoperatively and postoperatively, a significantly enlarged anteversion was found (21.92°±8.95° preoperatively with P <0.001 and 18.78°±7.25° postoperatively with P<0.001) compared with the healthy control group (12.62°±7.25°). After THA, the anteversion was reduced with an insignificant result (Table 2). The maximum pelvic tilt on the sagittal plane preoperatively and postoperatively was significantly higher (7.3°±4.48° preoperatively (P<0.001) and 4.93°±2.35° postoperatively (P<0.001)) than in the healthy control group (1.85°±0.87°) (Table 2). Examining the pelvic tilt in the sagittal plane in comparison preoperatively to postoperatively, a significantly lower pelvic tilt postoperatively was found (P=0.008).
Kinematic examination of the hip joint showed that the maximum extension on the affected side preoperatively with 7.26° flexion (±15.09°) and postoperatively with 1.20° flexion (±11.10°) was significantly lower than in the healthy control group with −7.76° flexion (±4.10°) (
The affected side had a significantly higher extension postoperatively than preoperatively (P=0.021) (Table 2).
Preoperatively and postoperatively, the opposite side also showed a significantly lower extension (−0.02° flexion ±11.66° preoperatively [
The ROM of the affected side was preoperatively and postoperatively significantly smaller than in the control group (−25.27°±9.93° before THA [
The ROM on the affected side after THA was significantly higher than before (P<0.001) (Table 2).
In the frontal plane, the maximum abduction of the affected side (minimum adduction) was lower postoperatively (−3.53°±4.22°) in comparison with the control group (−6.14°±2.22° [
The ROM in the frontal plane was smaller both before and after THA on both sides, the affected and the opposite, in comparison with the control group (P<0.001 for the comparison of the affected side preoperatively with the control group; P<0.001 for the comparison of the affected side postoperatively with the control group; P<0.001 for comparison of the opposite side preoperatively with control group; P<0.001 for the comparison of the opposite side postoperatively with the control group) (Table 2).
In the transverse plane, greater internal rotation (
Postoperatively, the affected side continued to have less internal rotation (
On the opposite side, external rotation was greater postoperatively than in the control group (
ROM was significantly greater on the affected and opposite side than in the control group, both before and after THA (P<0.001 for the comparison of the affected side preoperatively with the control group; P=0.006 for the comparison of the affected side postoperatively with the control group; P<0.001 for the comparison of the opposite site preoperatively with the control group; P<0.001 for the comparison opposite site postoperatively with the control group) (Table 2).
The trunk in one-legged stance of the affected side in the frontal plane inclined toward the affected side both before and after THA when compared with the control group (P=0.002 preoperatively and P<0.001 postoperatively vs the control group) (Table 3).
In the single-leg stand phase of the opposite side, there was no difference in thoracic inclination preoperatively compared to the control group.
After THA, the opposite side displayed reduced inclination of the thorax in relation to the pelvis toward the same side (P=0.019). In addition, the opposite side showed increased inclination of the pelvis to the same side compared with the control group (P=0.003) (Table 3).
KINETICS:
Preoperatively, work performed in the hip joint was significantly lower compared with the control group (P<0.001). Postoperatively, the work performed in the hip joint was still significantly lower (0.15±0.07 J/kg [P =0.009]) compared with the control group (0.20±0.05 J/kg). Postoperatively, work of the affected hip joint was higher compared to preoperatively (P<0.001). In comparison with the opposite side (0.17± 0.10 J/kg), the work performed before THA was lower (0.09±0.05 J/kg [P<0.001]). After THA, there was no longer a significant difference between the side operated upon (0.15±0.07 J/kg) and the opposite side (0.21±0.14 J/kg) (Table 4).
When comparing the absorbed energy, the affected side showed a significantly reduced energy absorption in hip (
Before THA, significantly less energy was absorbed in the hip and knee joints of the affected side than on the opposite side. After THA, there was no longer a significant difference between the 2 sides (Table 5).
PASSIVE ROM:
After THA, the hip flexion (94.13°±15.86°) was significantly higher than before (82.39°±25.40° [P=0.002]). The abduction in the hip joint increased significantly after THA from 18.04° (± 7.03°) to 22.61° (±7.21°, P=0.014). The internal rotation (16.74°±12.02°) and the external rotation (16.30°±9.80°) both increased significantly after THA (27.61°±11.27° internal rotation and 23.04°±6.87° external rotation (P=0.001 for internal rotation and P =0.006 for external rotation) (Table 6).
HHS:
After THA, there were significantly higher values in all 4 areas of the Harris hip score and for the total score (Table 6). The value for pain increased from 12.38 (±8.31) preoperatively to 33.81 (±10.43) postoperatively (P<0.001). The value for function increased from preoperatively 12.81 (±3.98) to 19.52 (±4.09) postoperatively (P<0.001). The total score increased from 47.38 (±12.25) preoperatively to 79.19 (±15.75) postoperatively (P<0.001) (Table 6).
Discussion
LIMITATIONS OF THIS STUDY ARE:
This was a single-center, retrospective study of a small cohort of 23 patients. The Harris hip score (HHS) is commonly used to evaluate the outcomes of primary THA in clinical trials. However, the application of the HHS may be limited in studies that evaluate and compare new techniques [56].
Conclusions
The findings from this retrospective study showed that ROM, HHS, and gait pattern of patients with severe deformity improved following THA with the modular S-ROM hip prosthesis, but gait did not completely return to normal. Further investigations are needed to show how long gait patterns change postoperatively and whether specific training influences gait parameters positively.
Tables
Table 1. Spatiotemporal gait parameters.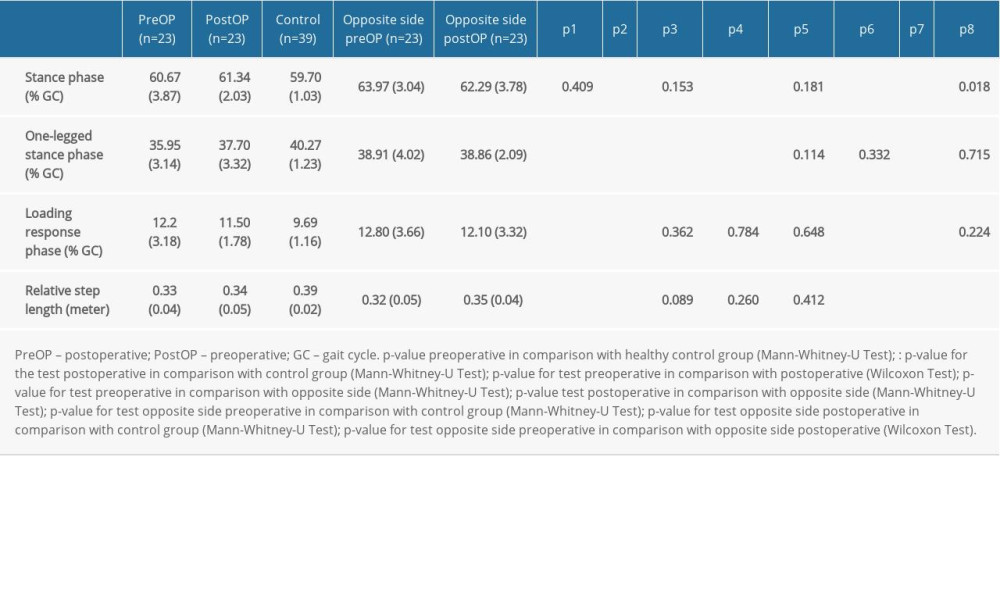 Table 2. Kinematics of the pelvis and the hip joint.
Table 2. Kinematics of the pelvis and the hip joint.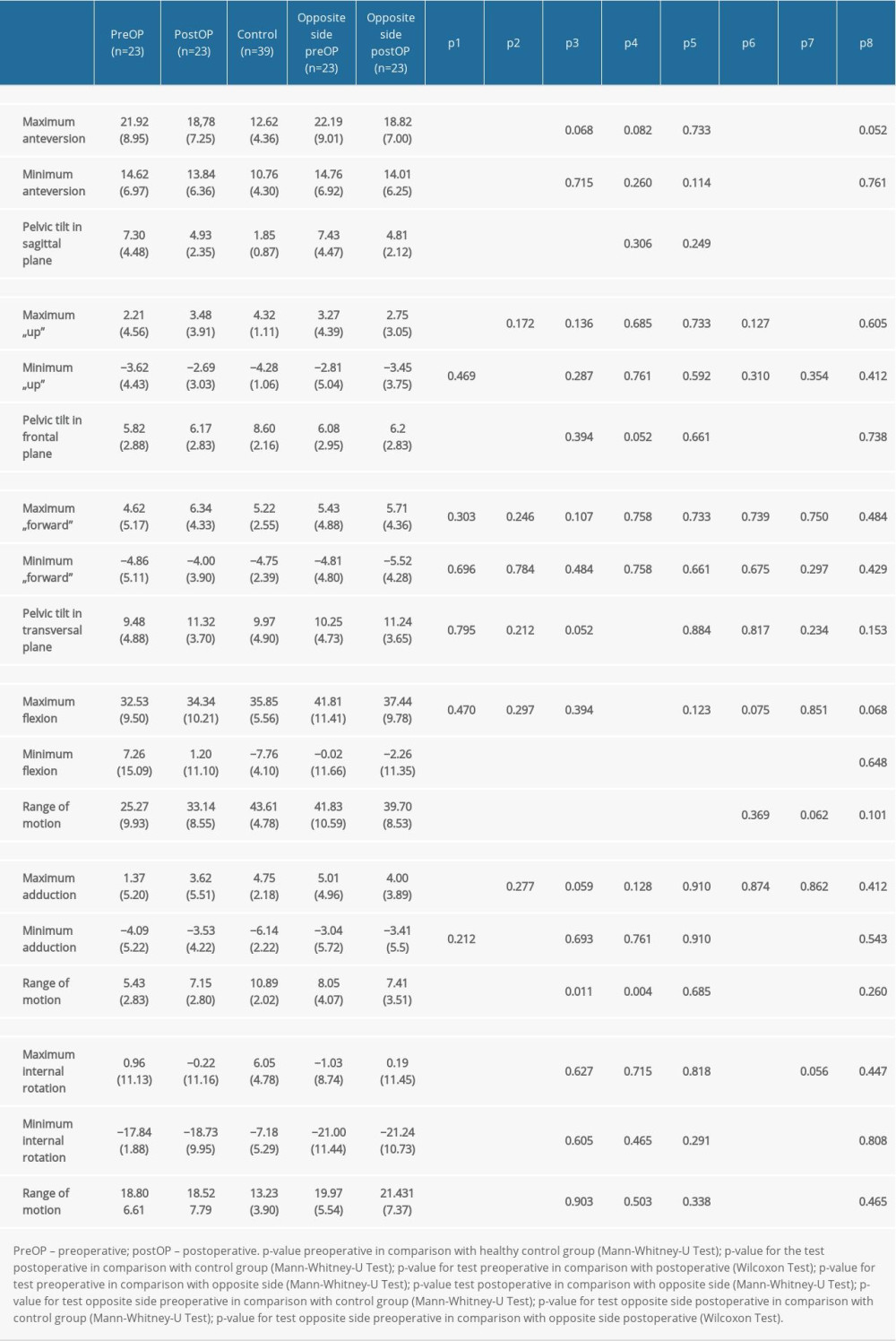 Table 3. Kinematics of trunk, pelvis and hip joint during the one-legged stance phase.
Table 3. Kinematics of trunk, pelvis and hip joint during the one-legged stance phase.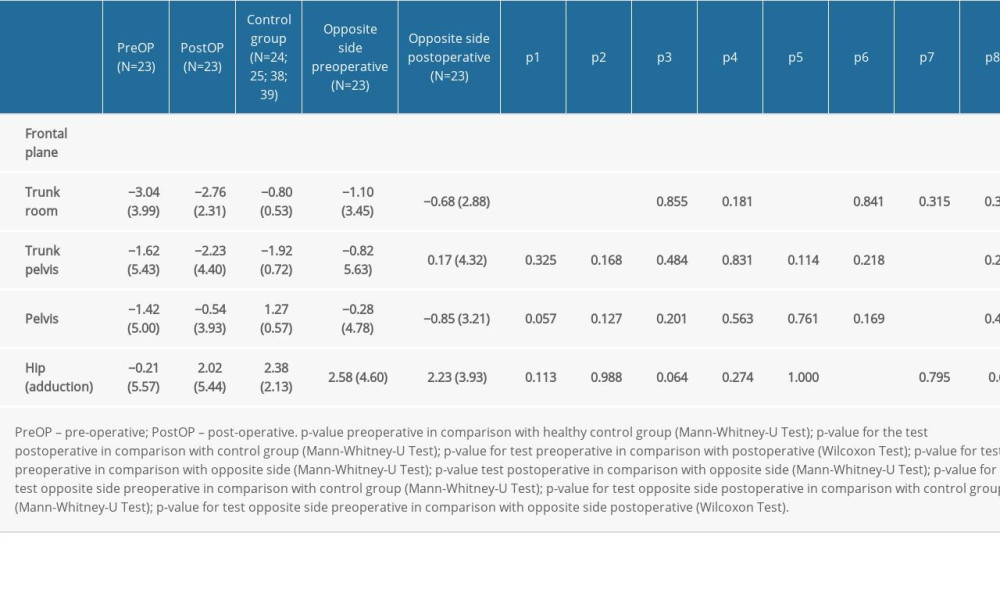 Table 4. Positive work.
Table 4. Positive work.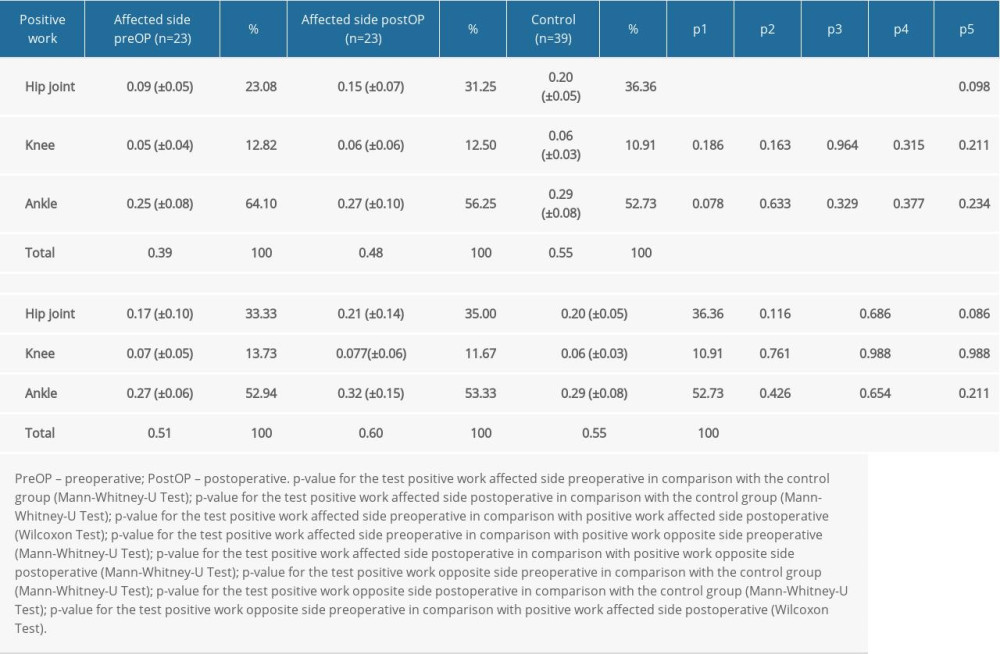 Table 5. Negative work.
Table 5. Negative work.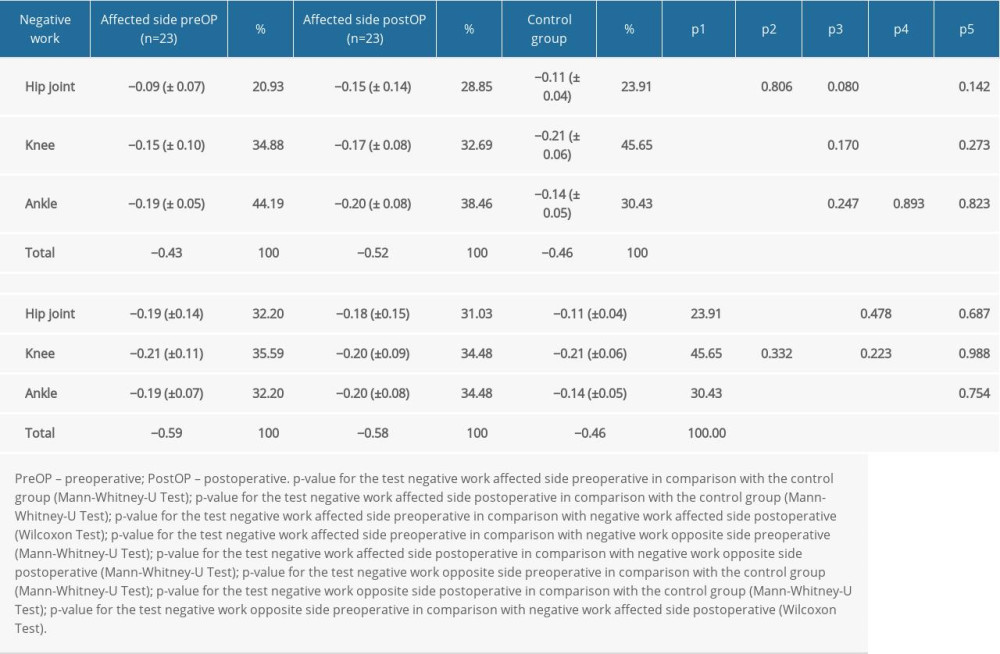 Table 6. Passive hip range of motion, leg length difference and Harris hip score.
Table 6. Passive hip range of motion, leg length difference and Harris hip score.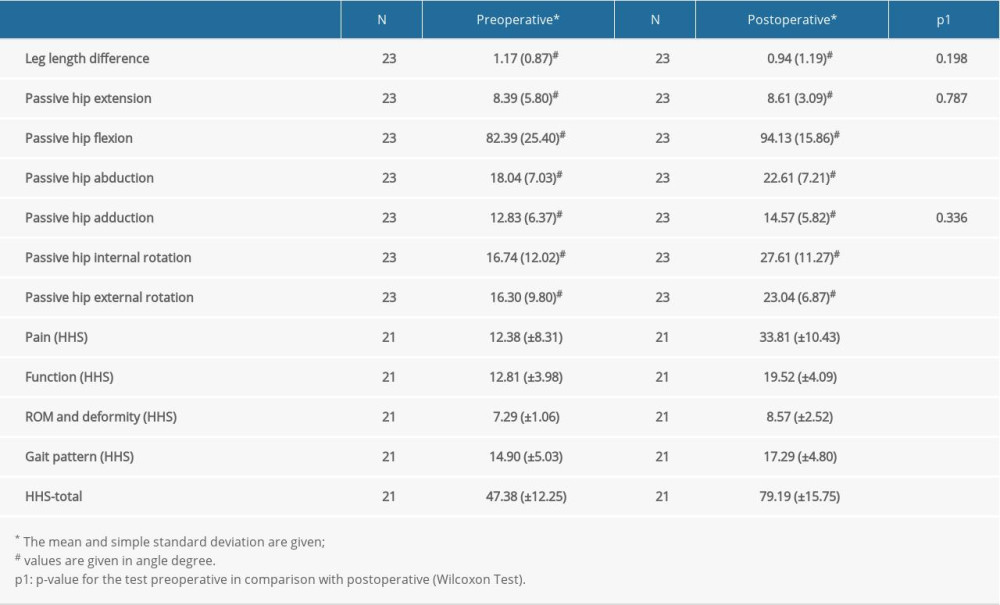
References
1. Debrunner A: Orthopädie, orthopädische chirurgie: Patientenorientierte diagnostik und therapie des bewegungsapparates, 2002, Huber [in German]
2. Naili JE, Hedström M, Broström EW, Changes of and interrelationships between performance-based function and gait and patient – reported function 1 year after total hip arthroplasty: J Orthop Traumatol, 2019; 20(1); 14
3. Mendiolagoitia L, Rodríguez MÁ, Crespo I, Kinematic gait analysis after primary total hip replacement: A systematic review: Gait after total hip replacement: A systematic review: Indian J Orthop, 2020; 54(6); 767-75
4. Clement ND, Patrick-Patel R, MacDonald D, Breusch SJ, Total hip replacement: Increasing femoral offset improves functional outcome: Arch Orthop Trauma Surg, 2016; 136(9); 1317-23
5. Esbjörnsson A-C, Kiernan S, Mattsson L, Flivik G, Geometrical restoration during total hip arthroplasty is related to change in gait pattern – a study based on computed tomography and three-dimensional gait analysis: BMC Musculoskelet Disord, 2021; 22(1); 369
6. Stief F, Schmidt A, van Drongelen S, Abnormal loading of the hip and knee joints in unilateral hip osteoarthritis persists two years after total hip replacement: J Orthop Res, 2018 [Online ahead of print]
7. Weber M, Suess F, Jerabek SA, Kinematic pelvic tilt during gait alters functional cup position in total hip arthroplasty: J Orthop Res, 2021 [Online ahead of print]
8. Petis S, Howard J, Lanting B, Comparing the anterior, posterior and lateral approach: Gait analysis in total hip arthroplasty: Can J Surg, 2018; 61(1); 50-57
9. Kiyohara M, Hamai S, Hara D, Do component position and muscle strength affect the cup-head translation during gait after total hip arthroplasty?: Eur J Orthop Surg Traumatol, 2019; 29(6); 1263-69
10. Alexander : S-ROM OP-Anleit_de_0107 [Internet], 2007 [updated 2007 Jan 5; cited 2012 Nov 21]: [24 p.]. Available from: [in German]http://www.depuy.de/file-download/S-ROM_0.pdf
11. Kang JS, Moon KH, Kim RS, Total hip arthroplasty using S-ROM prosthesis for dysplastic hip: Yonsei Med J, 2011; 52(4); 655
12. Park C-W, Lim S-J, Park Y-S, Modular stems: Advantages and current role in primary total hip arthroplasty: Hip Pelvis, 2018; 30(3); 147-55
13. Bretschneider H, Günther K-P, Hüftgelenk – arthrose und arthritis: Orthopädie und Unfallchirurgie up2date, 2015; 10(03); 231-56 [in German]
14. Lugeder A, Zeichen J, Klinische untersuchung des hüftgelenks und des beckengürtels: Orthopädie und Unfallchirurgie up2date, 2014; 9(3); 183-204 [in German]
15. Bretschneider H, Günther K-P, Hüftgelenk – arthrose und arthritis: Radiologie up2date, 2015; 15(04); 359-83 [in German]
16. Götz-Neumann K: Gehen verstehen: Ganganalyse in der physiotherapie; 18 Tabellen, 2011; 200, Stuttgart, Thieme (physiofachbuch) [in German]
17. Leijendekkers RA, Marra MA, Kolk S, Gait symmetry and hip strength in women with developmental dysplasia following hip arthroplasty compared to healthy subjects: A cross-sectional study: PLoS One, 2018; 13(2); 29474431
18. DePuy Synthes Companies Last Updated 2014 [cited 2014 Nov 20]. Available from:http://www.depuysynthes.com
19. Bolognesi MP, Pietrobon R, Clifford PE, Vail TP, Comparison of a hydroxyapatite-coated sleeve and a porous-coated sleeve with a modular revision hip stem. A prospective, randomized study: The J Bone Joint Surg Am, 2004; 86(12); 2720-25
20. Buly R, The S-ROM stem: Versatility of stem/sleeve combinations and head options: Orthopedics, 2005; 28(9 Suppl); s1025-32
21. Mertl P, Dehl M, Femoral stem modularity: Orthop Traumatol Surg Res, 2020; 106(1S); S35-42
22. DePuy Synthes Companies Last Updated 2014 [cited 2014 Nov 20]. Available from:https://emea.depuysynthes.com/hcp/hip/products/qs/corail-pinnacle-construct
23. Wiemann M, Kurzer abriss zur entwicklung der apparativen ganganalyse zwischen klassik und moderne: Phys Rehab Kur Med, 2000; 10(6); 227-30 [in German]
24. Westhoff B, Hirsch M, Hefter H, Wie reliabel sind informationen aus der 3D-ganganalyse?: Sportverletz Sportschaden, 2004; 18(02); 76-79 [in German]
25. Laupacis A, Bourne R, Rorabeck C, The effect of elective total hip replacement on health-related quality of life: J Bone Joint Surg Am, 1993; 75(11); 1619-26
26. Harris WH, Traumatic arthritis of the hip after dislocation and acetabular fractures: Treatment by mold arthroplasty. An end-result study using a new method of result evaluation: Bone Joint Surg Am, 1969; 51(4); 737-55
27. Söderman P, Malchau H, Is the Harris hip score system useful to study the outcome of total hip replacement?: Clin Orthop Relat Res, 2001; 2(384); 189-97
28. Vicon: Polygon | Reporting & Presentation | Vicon Motion Capture Software [Internet], 2021 [updated 2021 Aug 25; cited 2021 Sep 28]. Available from: https://www.vicon.com/software/polygon/?section=downloads
29. Vicon: Accessories For Vicon Systems | Everything Else You Need For Mocap [Internet], 2020 [updated 2020 Oct 30: cited 2021 Sep 28]. Available from: https://www.vicon.com/hardware/accessories/
30. Kadaba MP, Ramakrishnan HK, Wootten ME, Measurement of lower extremity kinematics during level walking: J Orthop Res, 1990; 8(3); 383-92
31. Bortz J, Lienert GA: Kurzgefasste statistik für die klinische forschung: Leitfaden für die verteilungsfreie analyse kleiner stichproben, 2008; xv, Berlin, Heidelberg, Springer Medizin Verlag Heidelberg 1 online resource
32. Isobe Y, Okumo M, Otsuki T, Yamamoto K, Clinical study of arthroplasties for osteoartritic hip by qantitative gait analysis: Comparison of total hip arthroplasty and biplar endoprosthetic arthroplasty: Biomed Mater Eng, 1998; 8(3–4); 167-75
33. Rompen JC, Ham SJ, Halbertsma JP, van Horn JR, Gait and function in patients with a femoral endoprosthesis after tumor resection: 18 patients evaluated 12 years after surgery: Acta Orthop Scand, 2002; 73(4); 439-46
34. Nagariya SP, Bhargava P, Shrivastava P, Assessment of changes in gait parameters and vertical ground reaction forces after total hip arthroplasty: Indian J Orthop, 2007; 41(2); 158
35. John S, Weizel D, Heumann AS, Persisting inter-limb differences in patients following total hip arthroplasty four to five years after surgery? A preliminary cross-sectional study: BMC Musculoskelet Disord, 2021; 22(1); 230
36. Agostini V, Ganio D, Facchin K, Gait parameters and muscle activation patterns at 3, 6 and 12 months after total hip arthroplasty: J Arthroplasty, 2014; 29(6); 1265-72
37. Eitzen I, Fernandes L, Nordsletten L, Risberg MA, Sagittal plane gait characteristics in hip osteoarthritis patients with mild to moderate symptoms compared to healthy controls: A cross-sectional study: BMC Musculoskelet Disord, 2012; 13(1); 258
38. Queen RM, Appleton JS, Butler RJ, Total hip arthroplasty surgical approach does not alter postoperative gait mechanics one year after surgery: PM R, 2014; 6(3); 221-26
39. Parratte S, Pagnano MW, Coleman-Wood K, The 2008 Frank Stinchfield award: Variation in postoperative pelvic tilt may confound the accuracy of hip navigation systems: Clin Orthop Relat Res, 2009; 467(1); 43-49
40. Weißgraeber P, Wall HVD, Khabbazeh S, Effect of the lateral rotators on load transfer in the human hip joint revealed by mechanical analysis: Ann Anat, 2012; 194(5); 461-66
41. Perry J: Ganganalyse: Norm und pathologie des gehens, 2003; IX, München, Jena, Urban und Fischer [in German]
42. Mahmood SS, Mukka SS, Crnalic S, Association between changes in global femoral offset after total hip arthroplasty and function, quality of life, and abductor muscle strength. A prospective cohort study of 222 patients: Acta Orthop, 2016; 87(1); 36-41
43. Kubota M, Shimada S, Kobayashi S, Quantitative gait analysis of patients with bilateral hip osteoarthritis excluding the influence of walking speed: J Orthop Sci, 2007; 12(5); 451-57
44. Arnold W, Schliebe GGait analysis in patients with total hip endoprosthesis. Part II: Pre- and postoperative gait analysis: Z Gesamte Inn Med, 1992; 47(1); 15-20 [in German]
45. Miltner O, Lange C, Zilkens K, Kinematische ganganalyse nach hüftendoprothese in abhängigkeit von der präoperativen schmerzdauer [Internet]. Deutsche gesellschaft für unfallchirurgie. 67. Jahrestagung der deutschen gesellschaft für unfallchirurgie, 89. Tagung der Deutschen gesellschaft für orthopädie und orthopädische chirurgie und 44: Tagung des berufsverbandes der fachärzte für orthopädie, 2003, Berlin, Düsseldorf, Köln [updated 2003 Nov 11]. Available from: [in German]www.egms.de/en/meetings/dgu2003/03dgu0707.shtml
46. Holzmann G, Meyer H, Schumpich G, Eller C: Technische mechanik kinematik und kinetik: Mit 138 beispielen und 172 aufgaben, 2010; XII, Wiesbaden, Vieweg + Teubner (Technische Mechanik) [in German]
47. Seichert N, Erhart P, Senn E, Die etablierung der instrumentierten ganganalyse (IGA) als verfahren zur unmittelbaren klinikrelevanten gangbeurteilung - darstellung der propulsiven und bremsenden muskelaktivitäten beim gehen: Phys Rehab Kur Med, 1997; 07(1); 1-11 [in German]
48. Rasch A, Dalén N, Berg HE, Muscle strength, gait, and balance in 20 patients with hip osteoarthritis followed for 2 years after THA: Acta Orthop, 2010; 81(2); 183-88
49. Bahl JS, Arnold JB, Taylor M, Lower functioning patients demonstrate atypical hip joint loading before and following total hip arthroplasty for osteoarthritis: J Orthop Res, 2020; 38(7); 1550-58
50. Bhargava P, Shrivastava P, Nagariya S, Assessment of changes in gait parameters and vertical ground reaction forces after total hip arthroplasty: Indian J Orthop, 2007; 41(2); 158-62
51. Bhave A, Marker DR, Seyler TM, Functional problems and treatment solutions after total hip arthroplasty: J Arthroplasty, 2007; 22(6 Suppl 2); 116-24
52. Windhager R, Mayer J, Bohn J, Mentales gehtraining – wirksamkeit eines therapieverfahrens in der rehabilitation nach hüftendoprothetik: Z Orthop Ihre Grenzgeb, 2005; 143(4); 419-23
53. Onodera S, Majima T, Ito H, Cementless total hip arthroplasty using the modular S-ROM prosthesis combined with corrective proximal femoral osteotomy: J Arthroplasty, 2006; 21(5); 664-69
54. Smith JA, Dunn HK, Manaster BJ, Cementless femoral revision arthroplasty. 2- to 5-year results with a modular titanium alloy stem: J Arthroplasty, 1997; 12(2); 194-201
55. Tanzer M, Chan S, Brooks CE, Bobyn JD, Primary cementless total hip arthroplasty using a modular femoral component: a minimum 6-year follow-up: J Arthroplasty, 2001; 16(8 Suppl 1); 64-70
56. Wamper KE, Sierevelt IN, Poolman RW, The Harris hip score: Do ceiling effects limit its usefulness in orthopedics?: Acta Orthop, 2010; 81(6); 703-7
Tables
 Table 1. Spatiotemporal gait parameters.
Table 1. Spatiotemporal gait parameters. Table 2. Kinematics of the pelvis and the hip joint.
Table 2. Kinematics of the pelvis and the hip joint. Table 3. Kinematics of trunk, pelvis and hip joint during the one-legged stance phase.
Table 3. Kinematics of trunk, pelvis and hip joint during the one-legged stance phase. Table 4. Positive work.
Table 4. Positive work. Table 5. Negative work.
Table 5. Negative work. Table 6. Passive hip range of motion, leg length difference and Harris hip score.
Table 6. Passive hip range of motion, leg length difference and Harris hip score. Table 1. Spatiotemporal gait parameters.
Table 1. Spatiotemporal gait parameters. Table 2. Kinematics of the pelvis and the hip joint.
Table 2. Kinematics of the pelvis and the hip joint. Table 3. Kinematics of trunk, pelvis and hip joint during the one-legged stance phase.
Table 3. Kinematics of trunk, pelvis and hip joint during the one-legged stance phase. Table 4. Positive work.
Table 4. Positive work. Table 5. Negative work.
Table 5. Negative work. Table 6. Passive hip range of motion, leg length difference and Harris hip score.
Table 6. Passive hip range of motion, leg length difference and Harris hip score. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387