02 March 2022: Clinical Research
Retrospective Study of the Association Between Platelet-to-Lymphocyte Ratio in Patients with Acute Coronary Syndrome on Admission to a Rural Referral Center in East Java, Indonesia, and the Incidence of New Symptomatic Heart Failure at 6 Months
Ryan Enast Intan1ACEF, Firas Farisi AlkaffDOI: 10.12659/MSM.935002
Med Sci Monit 2022; 28:e935002
Abstract
BACKGROUND: This was a retrospective study conducted at a rural referral center in East Java, Indonesia, to evaluate the association between the platelet-to-lymphocyte ratio (PLR) on hospital admission and the incidence of new symptomatic heart failure (HF) within 6 months in patients with acute coronary syndrome (ACS).
MATERIAL AND METHODS: The study population consisted of all ACS patients who were hospitalized between 1 January and 31 December 2018 at a non-percutaneous coronary intervention-capable secondary referral hospital and came for a routine follow-up until 6 months afterwards. The diagnosis of new symptomatic HF was based on International Classification of Diseases 10th revision code I50.9.
RESULTS: From 126 hospitalized patients, 92 patients were included in the analysis. The incidence rate of new symptomatic HF at 6 months was 70.65%. High PLR upon initial admission was significantly associated with new symptomatic HF incidence (odds ratio=1.70, P<0.001). PLR was also able to discriminate new symptomatic HF incidence at 6 months with area under the curve of 0.83 (P=0.001). Multivariate Cox regression analysis showed that PLR was an independent predictor for new symptomatic HF incidence (hazard ratio=4.5, P=0.001).
CONCLUSIONS: In a rural center in Indonesia, the PLR was independently correlated with the onset of new symptomatic HF in patients with ACS 6 months after hospital admission. The PLR may be a supplementary biomarker for clinical outcomes in patients with ACS for use in resource-limited regions.
Keywords: acute coronary syndrome, Female, Follow-Up Studies, Hospitalization, Humans, Incidence, Indonesia, Lymphocyte Count, Male, Platelet Count, Risk Factors, Rural Population
Background
Acute coronary syndrome (ACS) is a leading cause of mortality worldwide. It is a group of conditions caused by reduction of blood flow to the heart, including ST elevation myocardial infarction (STEMI), non-ST elevation myocardial infarction (NSTEMI), and unstable angina [1]. ACS can cause a number of complications, and one of the major complications is heart failure (HF) [2,3]. It is associated with high in-hospital mortality and poor long-term survival [4]. A population-based study in Saudi Arabian patients revealed that in-hospital mortality and cardiogenic shock were significantly higher if HF was presented [5]. A prospective cohort registry in the UK that evaluated the long-term prognosis of HF patients after ACS found that new-onset heart failure was associated with a 4-fold increased risk of death at 6 months [6]. Moreover, even in a stable condition, HF could lead to a dimnished quality of life [7]. Thus, it is very important to predict symptomatic HF occurrence in patients who survived ACS.
It has been proposed that inflammation plays an important role in both ACS and HF [8,9]. Various types of inflammatory biomarkers have been developed to predict the outcome of these diseases, such as N-terminal prohormone of brain natriuretic peptide (NT pro-BNP), high-sensitivity C-reactive protein (hs-CRP), lipoprotein-associated phospholipase A2, and homocysteine [10–12]. Unfortunately, these biomarkers are still scarce and are even unaffordable in areas with limited resources. Therefore, a biomarker that is cheap and widely available is needed.
Platelet-to-lymphocyte ratio (PLR) is a new inflammatory biomarker that can be used to predict morbidity and mortality. It can be easily calculated from complete blood count analysis. Recent studies showed that higher PLR levels reflected a more severe inflammation process and was associated with higher in-hospital and long-term mortality and major adverse cardiovascular events (MACE) in ACS patients [13–15]. Another study also found that higher PLR was corelated with worse 6-month survival rate in patients with acute HF and might be a novel marker in AHF management [16]. However, to the best of our knowledge, only a few studies have used PLR to predict HF incidence following ACS [17,18]. Therefore, this retrospective study was conducted at a rural referral center in East Java, Indonesia, to evaluate the association between the PLR on hospital admission and the incidence of HF at 6 months in patients with ACS
Material and Methods
STATISTICAL ANALYSIS:
For descriptive analysis, continuous data were given as mean±standard deviation (SD) or median [interquartile range (IQR)] depending on data distribution, while categorical data were given as n (%). For univariate analysis, the chi-square test was used for analyzing categorical data, and the independent t test or Mann-Whitney U test was used for continuous data, as appropriate. Variables with P value <0.25 from univariate analysis were then included in multivariate logistic regression analysis using the backward selection method [25]. Model calibration was tested using the Hosmer-Lemeshow test. Area under the curve (AUC) was used to determine whether PLR can be used to predict outcome incidence at 6 months or not. To determine the best PLR cut-off value, Youden Index was used [26]. Cox proportional multivariate hazards regression model was used to determine the hazard ratio of the PLR cut-off for outcome incidence at 6 months. P value <0.05 was considered as statistically significant [27]. All statistical analysis were done using SPSS for Windows version 21.0 (IBM Corp., Armonk, New York).
Results
BASELINE CHARACTERISTIC:
Patients’ baseline characteristic is presented based on the low level (<108) and high level of PLR value (≥108) based on median PLR level in this population (Table 1). Upon ACS presentation, patients with high PLR level were older and more of them had a history of hypertension compared to patients with low PLR level (P=0.041 and 0.001, respectively). Patients in the high PLR group also had higher GRACE score on admission (119±28.21 vs 102±34.68, P<0.001). All patients were treated regularly with optimal medication for ACS, including statin, anti-platelet, beta-blocker, and ace inhibitor. Thrombolytic was performed in all patients with STEMI that fulfilled the indication criteria for this procedure (34 patients), and was successful in 15 (44%) patients. Baseline TTE showed that 95% patients had diastolic dysfunction, 93% patients had LV dysfunction (LVEF <55%), and 99% patients had regional wall motion abnormality.
STUDY OUTCOMES:
There were no in-hospital outcome parameters associated with PLR (all P>0.05). For long-term outcomes, the incidence of 6-month new clinical symptomatic HF was significantly higher in patients with high PLR (odds ratio (OR)=1.70, 95% confidence interval=1.33–2.18, P<0.001) (Table 2).
The incidence rate of new clinical symptomatic HF at 6 months after ACS was 70% (65 patients). Among them, 41 patients (63%) developed early-onset symptomatic HF during the hospitalization (<7 days after ACS onset), and 24 patients (37%) developed late-onset symptomatic HF after hospitalization (≥7 days after ACS onset). The proportion of patients with diabetes mellitus or lower LVEF who develop symptomatic HF during hospitalization was significantly higher than after hospitalization (Table 3). On the contrary, the proportion of patients with hypertension who developed symptomatic HF during hospitalization was significantly lower. The PLR was significantly lower in patients who did not develop symptomatic HF compared to patients who developed acute-onset or late-onset symptomatic HF (both P<0.001) (Figure 1).
In the sub-analysis among patients with myocardial infarction, there was no significant difference between STEMI and NSTEMI in symptomatic HF incidence at 6-month follow-up (hazard ratio (HR)=1.15, 95% CI=0.81–1.57,
MULTIVARIATE ANALYSIS OF SYMPTOMATIC HF INCIDENCE PREDICTOR:
The association of different predictor variables with symptomatic HF incidence at 6 months was assessed in univariate and multivariate analyses (Table 4). In the multivariate logistic regression model for symptomatic HF incidence at 6 months after ACS, age, sex, myocardial infarction, in-hospital LV ejection fraction, circadian morning onset, admission PLR level, creatine kinase myocardial band (CKMB) level, hypertension status, smoking status, and family history of CVD were included. After adjusting for other factors, PLR level and LVEF remained significant (P<0.001). The Hosmer and Lemeshow test suggested the model had good fitness to the data (P=0.941). The model explained 65.9% (Nagelkerke R2) of the variance in symptomatic HF incidence and correctly classified 90.4% of the cases. As PLR level increase by 1 unit, the odds of having clinical symptomatic HF at 6 months also increased (adjusted OR=1.072, 95% CI=1.03–1.11, P<0.001). Meanwhile, higher baseline LVEF after ACS acted as a protective factor from symptomatic HF incidence at 6 months (adjusted OR=0.85, 95% CI=0.77–0.94, P=0.002). The final model showed that LVEF and PLR level had good discrimination for new symptomatic HF, with C statistic of 0.939 (P<0.001) (Figure 2).
PLR AS AN INDEPENDENT PREDICTOR FOR DYMPTOMATIC HF INCIDENCE AT 6 MONTHS:
PLR was able to positively discriminate new clinical symptomatic HF incidence at 6 months, with AUC of 0.83 (95% CI=0.75–0.92, P<0.001). The best cut-off for PLR level to predict new clinical symptomatic HF was 87 (sensitivity 0.89 [95% CI=0.82 to 0.94], specificity 0.63 [95% CI 0.53 to 0.72], positive likelihood ratio 2.41, positive predictive value 0.71 [95% CI=0.65 to 0.76], and negative predictive value 0.85 [95% CI=0.76 to 0.91]) (Figure 3). Using this cut-off, 58 out of 68 patients (85.3%) with PLR ≥87 had new symptomatic HF, whereas only 7 out of 24 (29.2%) with PLR <87 had new symptomatic HF (OR=2.92, 95% CI=1.55–5.50, P=0.001). Multivariate Cox regression was then used to calculate the hazard ratio for symptomatic HF incidence. After controlling for other confounding factors, PLR level ≥87 was shown to be an independent predictor of 6 months symptomatic HF incidence after ACS (HR=4.5, 95% CI=1.8–11, P=0.001) (Figure 4).
SECONDARY ANALYSIS:
In secondary analysis using Pearson correlation, PLR was positively correlated with GRACE score (p=0.004, r=0.27) and negatively correlated with LVEF (p=0.001, r=−0.39) (Figure 5).
Discussion
In this study, we found that 44.5% of the patients developed new symptomatic HF during admission. This incidence is higher than the previous study in Saudi Arabia that had 20% admission HF incidence [4]. This might be due to the long pre-hospital delay time (median 6.75 hours) in our study. Overall outcome at 6 months showed a 70% incidence rate of new clinical HF. This finding is higher than the result of the GRACE study with 17.6% and UK registry with 6.5% of new HF incidence rate at 6 months [6,28]. The high number of new HF cases in our study population might have been caused by a suboptimal revascularization therapy due to the absence of primary PCI strategy in our hospital. This hypothesis is also supported by the data from the GRACE study that showed patients with ACS who developed new HF were less likely to undergo cardiac catheterization [28].
From the onset of HF, our findings were similar to the population in the GRACE study [28], but with different risk factors. In our study, patients with early-onset HF were more likely to have diabetes and lower LVEF, and were less likely to have hypertension compared to the late-onset HF, whereas in the GRACE study, patients admitted with HF tended to be older and were more likely to have a history of coronary artery disease and atrial fibrillation [28].
From the univariate analysis, the risk factor predictor for developing new HF has some similarities to previous studies [6,28]. New findings in our study are the addition of GRACE score and biomarker from complete blood count and CKMB as a predictor of HF incidence. However, after multivariate logistic regression analysis, only LVEF and PLR remained significant as predictors of HF at 6 months after ACS. While previous studies only analyzed PLR either as an independent predictor for ACS [13–15] or acute HF outcome [16], our study is the first to show that PLR can also be used to predict symptomatic HF incidence at 6 months after ACS.
In regard to MACE outcome, many studies have analyzed PLR as an independent predictor for MACE and mortality in ACS or HF patient populations, including a meta-analysis of 8 studies involving 6627 participants [13,29–31]. Our study also showed that PLR had a weak correlation with GRACE mortality risk score at admission, which is a predictor of MACE within 6 months after ACS, similar to a previous study of STEMI patients [32]. However, the result of our study showed that MACE was not associated with higher PLR value. However, some studies reported that PLR value was a predictor of MACE in ACS patients [13,30]. These varied results might be caused by the difference in follow-up duration. While the observation period in our study was only 6 months, the follow-up duration in other studies were up to 5 years [13].
The cut-off points of PLR value for biomarker predictor risk group stratification varies across studies, depending on the disease, inflammation status, and population characteristics [13,33,34]. In our study, the cut-off PLR value for discriminating new symptomatic HF incidence at 6 months was lower than in previous studies. We hypothesized that patients who had an ACS event in a non-PCI facility or in a rural area were more prone to develop new HF at 6-month follow-up, despite optimal medication.
It is still not clear how the exact mechanism of PLR level is associated with adverse outcomes in ACS patients. Higher PLR value has been reported to be correlated with increased inflammatory activity and prothrombotic status due to relative thrombocytosis and megakaryocytic proliferation in ACS patients [29,35]. Furthermore, lower lymphocyte level due to increased cortisol in response to physiological stress can also be correlated with worse clinical outcomes in ACS patients [36]. Hence, PLR calculated from numbers of platelets and lymphocytes may be a novel indicator of inflammatory and prothrombotic status, and might be utilized to predict the outcome of ACS, including HF development. The mechanism involved in this includes the release of proteolytic enzymes and pro-inflammatory cytokines, secondary to the increased inflammatory state in ACS [37,38]. A previous study has shown that higher PLR is positively correlated with increased inflammatory cytokines such as interleukin-1 (IL-1), interleukin-6 (IL-6), and tumor necrotizing factor-α [39], which can damage the myocardium, resulting in reduced left ventricular function and HF [40]. High levels of pro-inflammatory cytokines might also lead to myocardial remodeling and cardiac arrhythmia, resulting in cardiac dysfunction [41]. Our secondary analysis also shows that PLR is negatively correlated with LVEF during hospitalization, which may affect the mechanism of HF development. This finding was in line with a previous study by Bekler et al (2015), which showed that high PLR was associated with left ventricular systolic dysfunction (LVEF <40%) in NSTEMI patients [17].
There were several limitations to this study. This study was a single-center study conducted in a rural area, which may be different than in an urban clinical setting. The relatively small number of samples compared to other studies might have caused several potential biases. The follow-up period was only 6 months, which may also have contributed to the non-significant result for MACE. Another limitation was that we had no comparable data on other biomarkers such as hs-CRP, IL-1, IL-6, or NT pro-BNP. Analysis of the correlation of PLR with these substances may have strengthened our study. However, despite the limitations, this is the first study to evaluate use of PLR as an independent predictor for new symptomatic HF after ACS.
Conclusions
In a rural center in Indonesia, PLR was independently correlated with the onset of symptomatic heart failure in patients with ACS 6 months after hospital admission. PLR may be a supplementary biomarker for clinical outcomes in patients with ACS for use in resource-limited regions. In patients with high PLR level, strict control of cardiovascular risk factors, routine follow-up visits, and close monitoring should be encouraged.
Figures
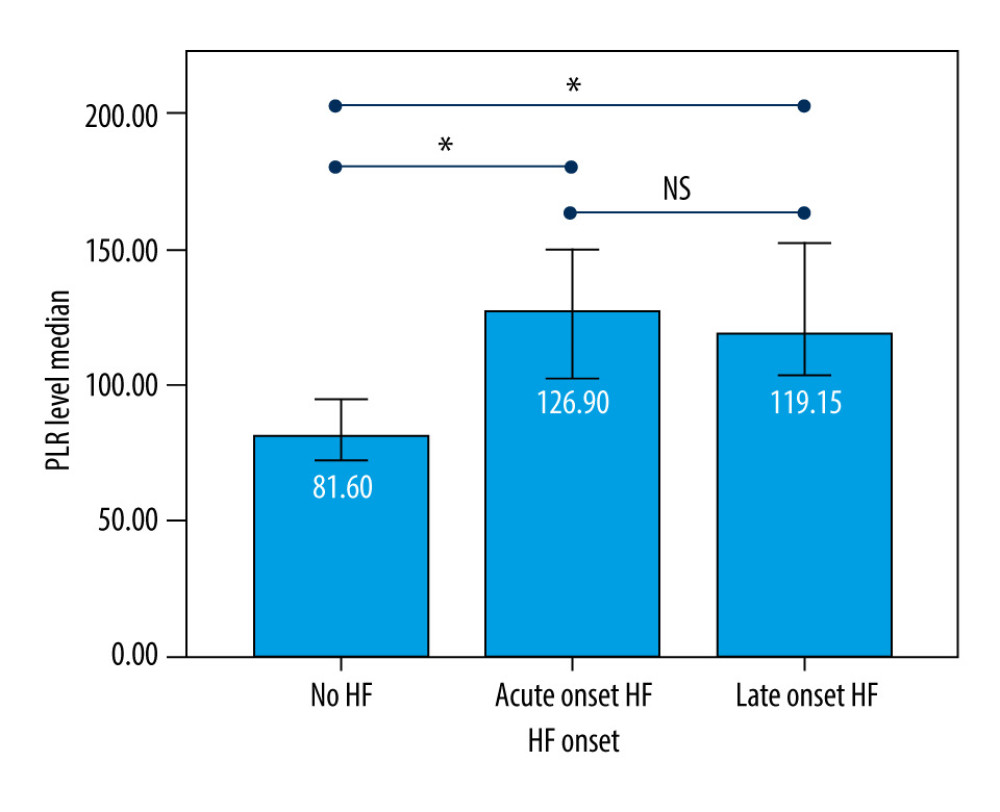 Figure 1. Platelet-to-lymphocyte ratio (PLR) difference based on heart failure (HF) onset. Acute-onset=HF occurred during the hospitalization and/or <7 days after acute coronary syndrome (ACS); Late-onset=HF occurred later after ACS hospitalization (≥7 days-6 months). P value <0.05 (*) was considered statistically significant, and P value >0.05 (NS) was considered not statistically significant.
Figure 1. Platelet-to-lymphocyte ratio (PLR) difference based on heart failure (HF) onset. Acute-onset=HF occurred during the hospitalization and/or <7 days after acute coronary syndrome (ACS); Late-onset=HF occurred later after ACS hospitalization (≥7 days-6 months). P value <0.05 (*) was considered statistically significant, and P value >0.05 (NS) was considered not statistically significant. 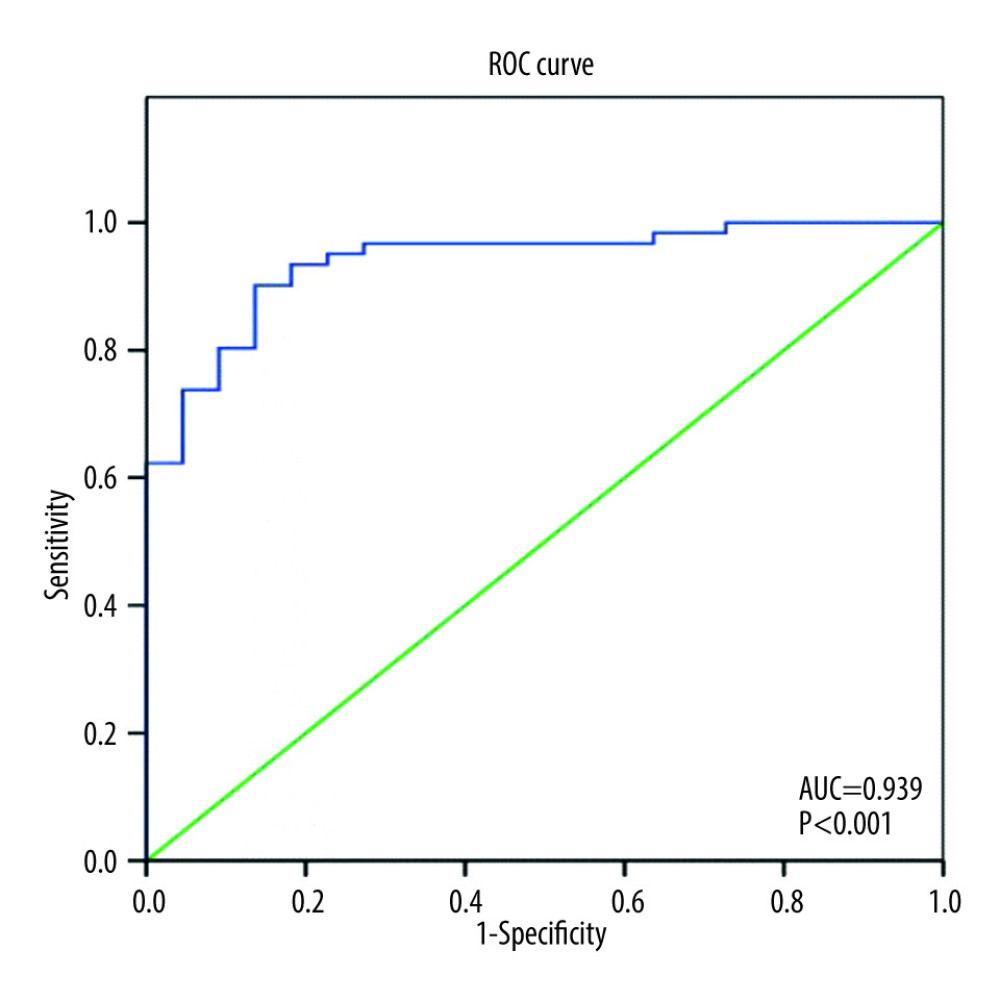 Figure 2. Receiver operating characteristic curve of the final model consist of left ventricular ejection fraction and platelet-to-lymphocyte ratio to predict heart failure incidence at 6 months after acute coronary syndrome. AUC – area under curve.
Figure 2. Receiver operating characteristic curve of the final model consist of left ventricular ejection fraction and platelet-to-lymphocyte ratio to predict heart failure incidence at 6 months after acute coronary syndrome. AUC – area under curve. 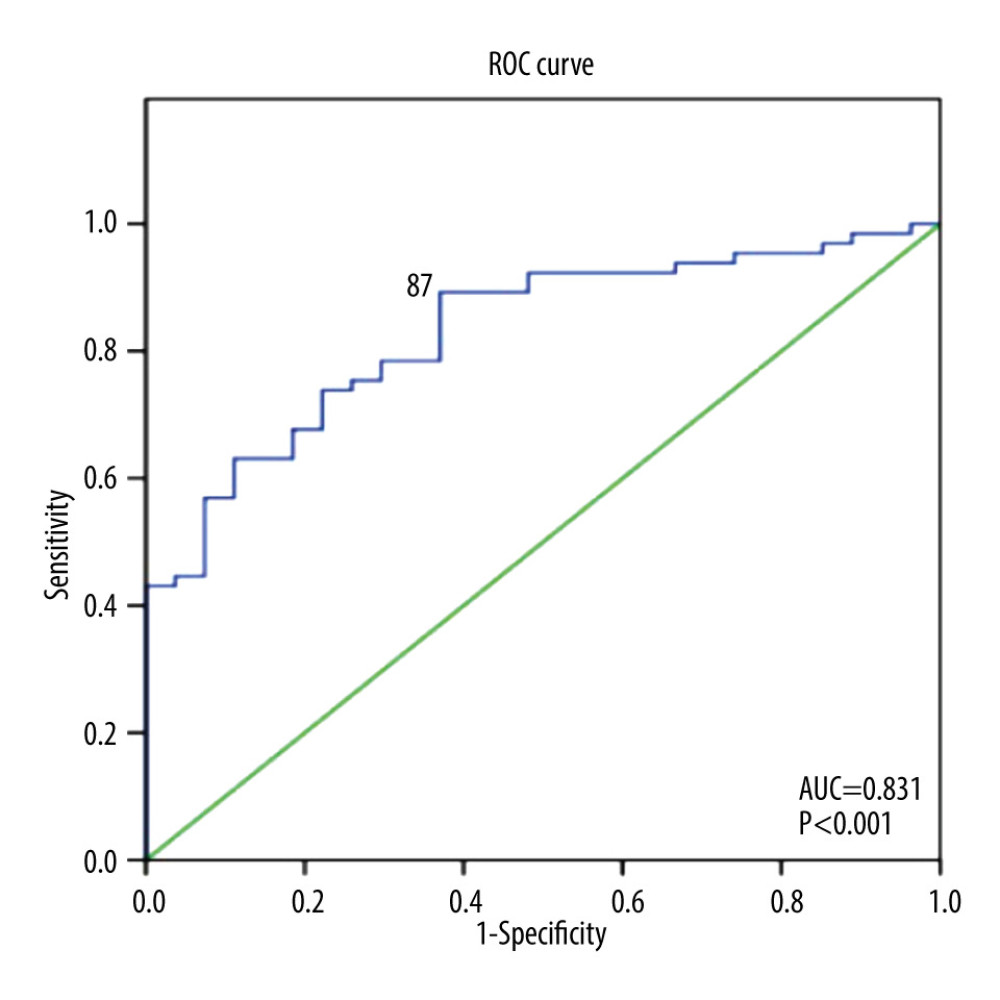 Figure 3. Receiver operating characteristic curve of platelet-to-lymphocyte ratio (PLR) as a predictor of heart failure (HF) incidence at 6 months. The best cut-off for PLR to discriminate 6-month HF is 87 (Sensitivity=89%, Specificity=63%, Odds ratio=2.92, 95% confidence interval 1.55–5.50, P<0.001). AUC – area under curve.
Figure 3. Receiver operating characteristic curve of platelet-to-lymphocyte ratio (PLR) as a predictor of heart failure (HF) incidence at 6 months. The best cut-off for PLR to discriminate 6-month HF is 87 (Sensitivity=89%, Specificity=63%, Odds ratio=2.92, 95% confidence interval 1.55–5.50, P<0.001). AUC – area under curve. 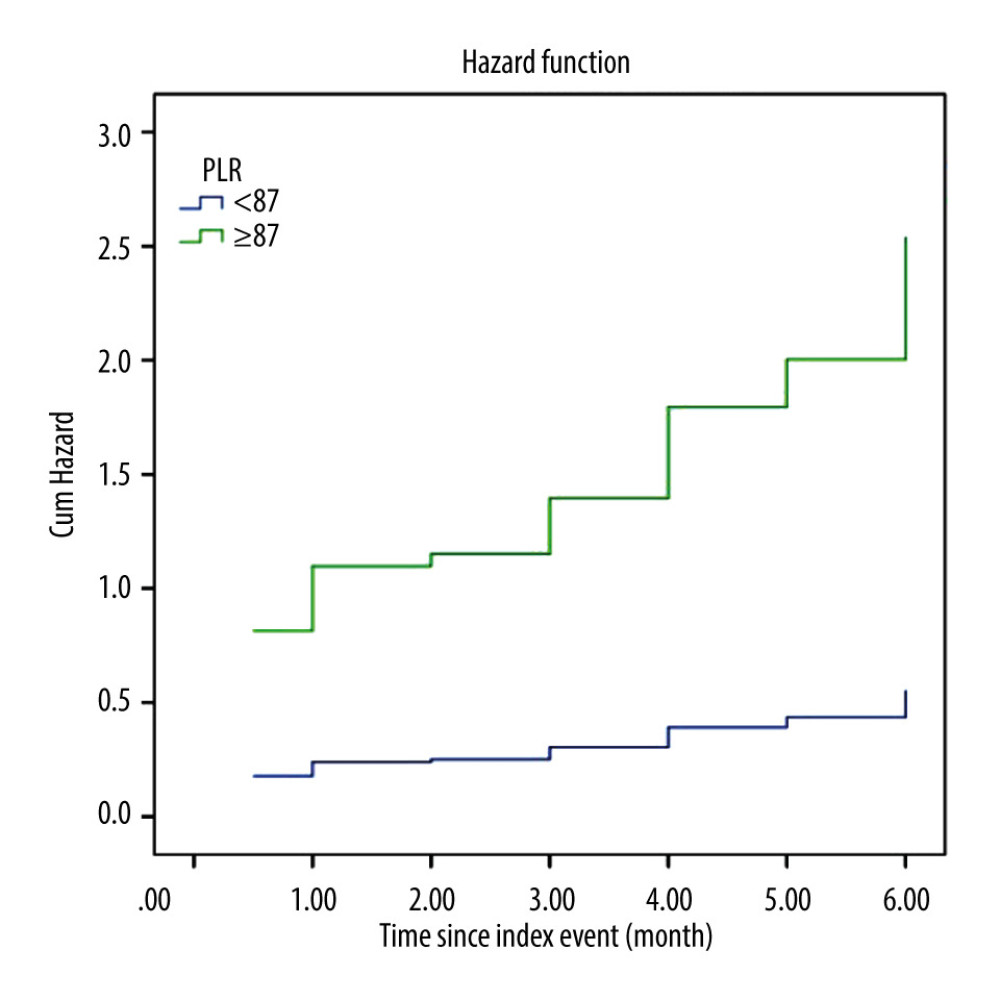 Figure 4. Multivariate Cox regression hazard function analysis showing differences between patients with high and low platelet-to-lymphocyte ratio (PLR) associated with the outcome of HF occurring within 6 months after hospital admission for acute coronary syndrome. The hazard ratio for high PLR (PLR ≥87) is 4.5 (95% confidence interval=1.8–11, P=0.001).
Figure 4. Multivariate Cox regression hazard function analysis showing differences between patients with high and low platelet-to-lymphocyte ratio (PLR) associated with the outcome of HF occurring within 6 months after hospital admission for acute coronary syndrome. The hazard ratio for high PLR (PLR ≥87) is 4.5 (95% confidence interval=1.8–11, P=0.001). 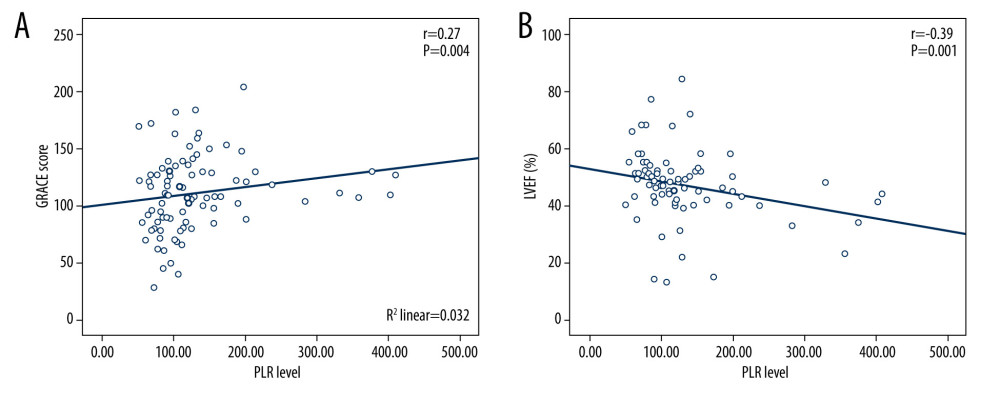 Figure 5. Scatter plots showing the association between (A) platelet-to-lymphocyte ratio (PLR) and Global Registry of Acute Coronary Events score (GRACE) risk score, (B) PLR and left ventricular ejection fraction (LVEF).
Figure 5. Scatter plots showing the association between (A) platelet-to-lymphocyte ratio (PLR) and Global Registry of Acute Coronary Events score (GRACE) risk score, (B) PLR and left ventricular ejection fraction (LVEF). Tables
Table 1. Baseline characteristics of study population.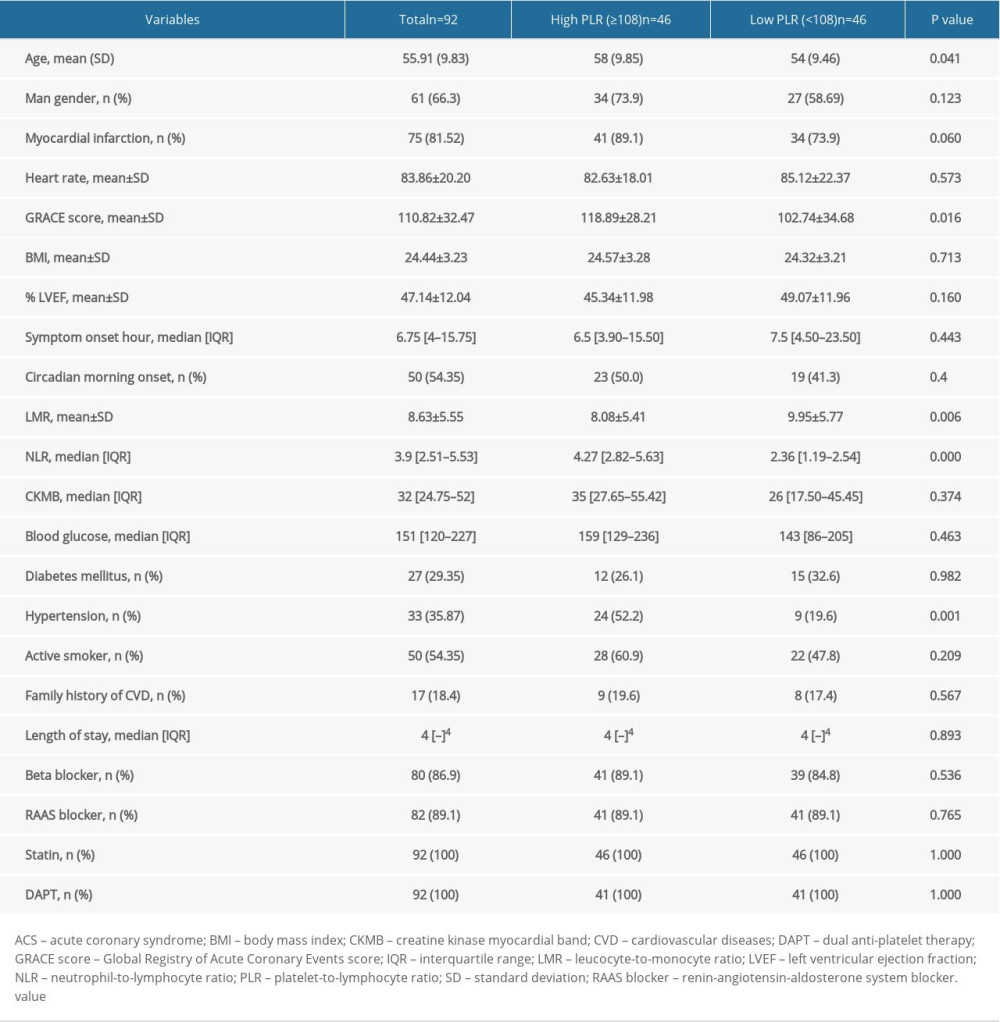 Table 2. In-hospital and long-term outcomes of patients with acute coronary syndrome.
Table 2. In-hospital and long-term outcomes of patients with acute coronary syndrome.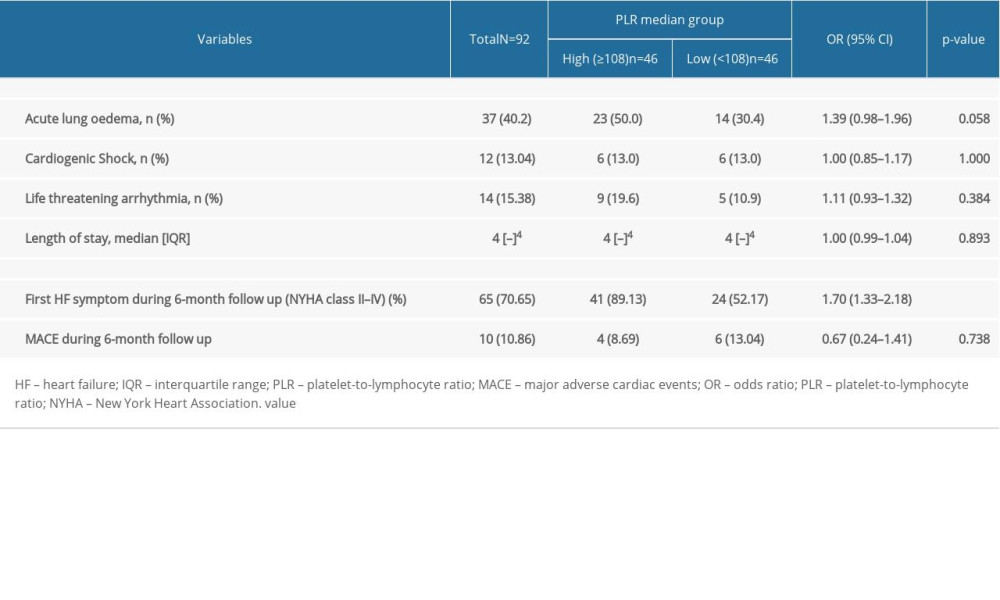 Table 3. Comparison of characteristics between acute coronary syndrome patients who develop heart failure during vs after hospitalization.
Table 3. Comparison of characteristics between acute coronary syndrome patients who develop heart failure during vs after hospitalization.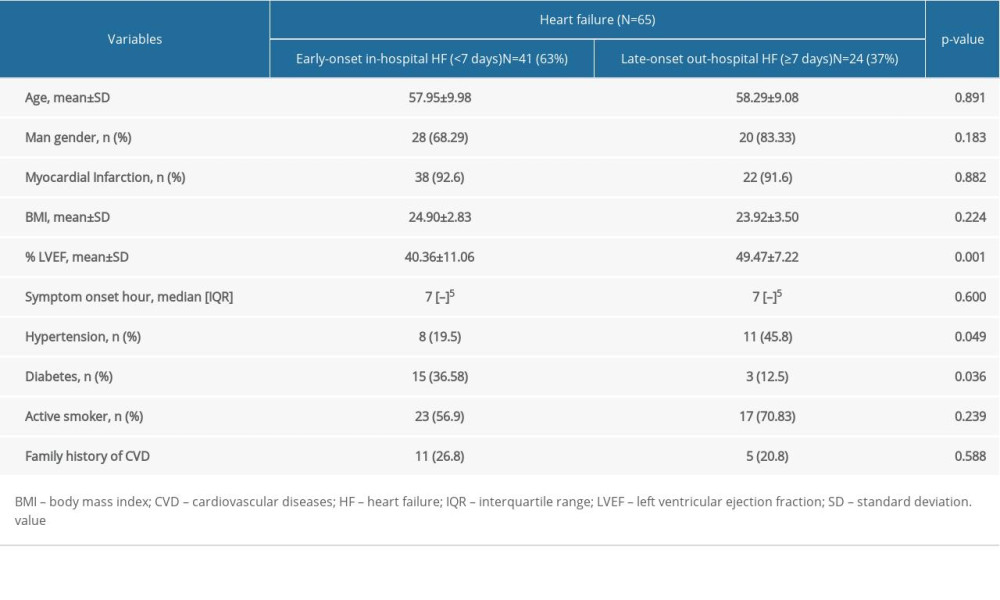 Table 4. Risk factors for developing heart failure at 6 months after acute coronary syndrome.
Table 4. Risk factors for developing heart failure at 6 months after acute coronary syndrome.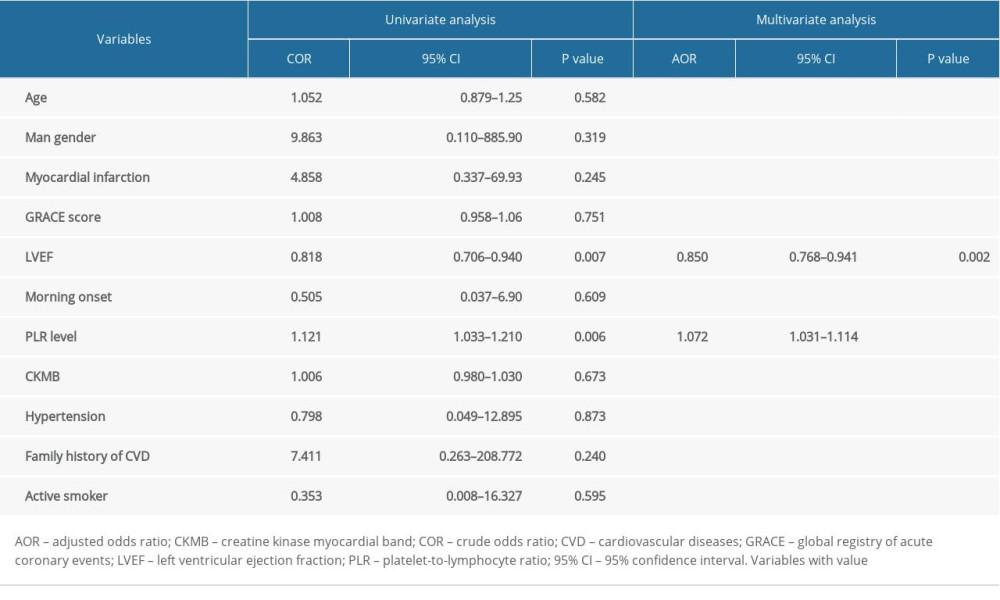
References
1. Singh A, Museedi AS, Grossman SA: Acute coronary syndrome, 2021, StatPearls, Treasure Island (FL)
2. Velazquez EJ, Pfeffer MA, Acute heart failure complicating acute coronary syndromes: A deadly intersection: Circulation, 2004; 109(4); 440-42
3. Pattanayak JM, Gelfand EV, Complications of acute coronary syndrome: Management of Acute Coronary Syndromes, 2009; 141-72
4. AlFaleh H, Elasfar AA, Ullah A, Acute heart failure with and without acute coronary syndrome: Clinical correlates and prognostic impact (from the HEARTS registry): BMC Cardiovasc Disord, 2016; 16; 98
5. Albackr HB, Alhabib KF, Ullah A, Prevalence and prognosis of congestive heart failure in Saudi patients admitted with acute coronary syndrome (from SPACE registry): Coron Artery Dis, 2013; 24(7); 596-601
6. Shibata MC, Collinson J, Taneja AK, Long term prognosis of heart failure after acute coronary syndromes without ST elevation: Postgrad Med J, 2006; 82(963); 55-59
7. Juenger J, Schellberg D, Kraemer S, Health related quality of life in patients with congestive heart failure: Comparison with other chronic diseases and relation to functional variables: Heart, 2002; 87(3); 235-41
8. Dick SA, Epelman S, Chronic heart failure and inflammation: Circ Res, 2016; 119(1); 159-76
9. Golia E, Limongelli G, Natale F, Inflammation and cardiovascular disease: From pathogenesis to therapeutic target: Curr Atheroscler Rep, 2014; 16(9); 435
10. Carlquist JF, Muhlestein JB, Anderson JL, Lipoprotein-associated phospholipase A2: A new biomarker for cardiovascular risk assessment and potential therapeutic target: Expert Rev Mol Diagn, 2007; 7(5); 511-17
11. Ganguly P, Alam SF, Role of homocysteine in the development of cardiovascular disease: Nutr J, 2015; 14; 6
12. Richards AM, New biomarkers in heart failure: Applications in diagnosis, prognosis and guidance of therapy: Rev Esp Cardiol, 2010; 63(6); 635-39
13. Li H, Zhou Y, Ma Y, The prognostic value of the platelet-to-lymphocyte ratio in acute coronary syndrome: A systematic review and meta-analysis: Kardiologia Polska, 2017; 666-73
14. Li X-T, Fang H, Li D, Association of platelet to lymphocyte ratio with in-hospital major adverse cardiovascular events and the severity of coronary artery disease assessed by the Gensini score in patients with acute myocardial infarction: Chin Med J (Engl), 2020; 133(4); 415-23
15. Ozcan Cetin EH, Cetin MS, Aras D, Platelet to lymphocyte ratio as a prognostic marker of in-hospital and long-term major adverse cardiovascular events in ST-segment elevation myocardial infarction: Angiology, 2016; 67(4); 336-45
16. Ye GL, Chen Q, Chen X, The prognostic role of platelet-to-lymphocyte ratio in patients with acute heart failure: A cohort study: Sci Rep, 2019; 9(1); 10639
17. Bekler A, Gazi E, Yılmaz M, Could elevated platelet-lymphocyte ratio predict left ventricular systolic dysfunction in patients with non-ST elevated acute coronary syndrome?: Anat J Cardiol, 2015; 15(5); 385-90
18. Li W, Liu Q, Tang Y, Platelet to lymphocyte ratio in the prediction of adverse outcomes after acute coronary syndrome: A meta-analysis: Sci Rep, 2017; 7; 40426
19. Ibanez B, James S, Agewall S, 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation: The Task Force for the management of acute myocardial infarction in patients presenting with ST-segment elevation of the European Society of Cardiology (ESC): Eur Heart J, 2018; 39(2); 119-77
20. Roffi M, Patrono C, Collet JP, 2015 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: Task Force for the Management of Acute Coronary Syndromes in Patients Presenting without Persistent ST-Segment Elevation of the European Society of Cardiology (ESC): Eur Heart J, 2016; 37(3); 267-315
21. Dolgin MartinNew York Heart Association Criteria Committee: Nomenclature and criteria for diagnosis of diseases of the heart and great vessels, 1994, Boston, Mass, Lippincott Williams and Wilkins
22. Pandhi J, Gottdiener JS, Bartz TM, Comparison of characteristics and outcomes of asymptomatic versus symptomatic left ventricular dysfunction in subjects 65 years old or older (from the Cardiovascular Health Study): Am J Cardiol, 2011; 107(11); 1667-74
23. World Health O: ICD-10: International statistical classification of diseases and related health problems: tenth revision, 2004, Geneva, World Health Organization
24. Abu-Assi E, Garcia-Acuna JM, Pena-Gil C, Gonzalez-Juanatey JR, Validation of the GRACE risk score for predicting death within 6 months of follow-up in a contemporary cohort of patients with acute coronary syndrome: Rev Esp Cardiol, 2010; 63(6); 640-48
25. Bursac Z, Gauss CH, Williams DK, Hosmer DW, Purposeful selection of variables in logistic regression: Source Code Biol Med, 2008; 3; 17
26. Youden WJ, Index for rating diagnostic tests: Cancer, 1950; 3(1); 32-35
27. Di Leo G, Sardanelli F, Statistical significance: p value, 0.05 threshold, and applications to radiomics-reasons for a conservative approach: Eur Radiol Exp, 2020; 4(1); 18
28. Steg PG, Dabbous OH, Feldman LJ, Determinants and prognostic impact of heart failure complicating acute coronary syndromes: Observations from the Global Registry of Acute Coronary Events (GRACE): Circulation, 2004; 109(4); 494-99
29. Fuentes QE, Fuentes QF, Andres V, Role of platelets as mediators that link inflammation and thrombosis in atherosclerosis: Platelets, 2013; 24(4); 255-62
30. Hudzik B, Szkodzinski J, Gorol J, Platelet-to-lymphocyte ratio is a marker of poor prognosis in patients with diabetes mellitus and ST-elevation myocardial infarction: Biomark Med, 2015; 9(3); 199-207
31. Temiz A, Gazi E, Güngör Ö, Platelet/lymphocyte ratio and risk of in-hospital mortality in patients with ST-elevated myocardial infarction: Med Sci Monit, 2014; 20; 660-65
32. Acet H, Ertaş F, Akıl MA, Relationship between hematologic indices and global registry of acute coronary events risk score in patients with ST-segment elevation myocardial infarction: Clin Appl Thromb Hemost, 2014; 22(1); 60-68
33. Fest J, Ruiter R, Ikram MA, Reference values for white blood-cell-based inflammatory markers in the Rotterdam Study: A population-based prospective cohort study: Sci Rep, 2018; 8(1); 10566
34. Zhou X, Du Y, Huang Z, Prognostic value of PLR in various cancers: A meta-analysis: PLoS One, 2014; 9(6); e101119
35. Lindemann S, Kramer B, Seizer P, Gawaz M, Platelets, inflammation and atherosclerosis: J Thromb Haemost, 2007; 5(Suppl 1); 203-11
36. Kurtul A, Murat SN, Yarlioglues M, Association of platelet-to-lymphocyte ratio with severity and complexity of coronary artery disease in patients with acute coronary syndromes: Am J Cardiol, 2014; 114(7); 972-78
37. Fioranelli M, Bottaccioli AG, Bottaccioli F, Stress and inflammation in coronary artery disease: A review psychoneuroendocrineimmunology-based: Front Immunol, 2018; 9; 2031
38. Ridker PM, Rifai N, Stampfer MJ, Hennekens CH, Plasma concentration of interleukin-6 and the risk of future myocardial infarction among apparently healthy men: Circulation, 2000; 101(15); 1767-72
39. Turkmen K, Erdur FM, Ozcicek F, Platelet-to-lymphocyte ratio better predicts inflammation than neutrophil-to-lymphocyte ratio in end-stage renal disease patients: Hemodial Int, 2013; 17(3); 391-96
40. Durmus E, Kivrak T, Gerin F, Neutrophil-to-lymphocyte ratio and platelet-to-lymphocyte ratio are predictors of heart failure: Arq Bras Cardiol, 2015; 105(6); 606-13
41. Prabhu SD, Cytokine-induced modulation of cardiac function: Circ Res, 2004; 95(12); 1140-53
Figures
 Figure 1. Platelet-to-lymphocyte ratio (PLR) difference based on heart failure (HF) onset. Acute-onset=HF occurred during the hospitalization and/or <7 days after acute coronary syndrome (ACS); Late-onset=HF occurred later after ACS hospitalization (≥7 days-6 months). P value <0.05 (*) was considered statistically significant, and P value >0.05 (NS) was considered not statistically significant.
Figure 1. Platelet-to-lymphocyte ratio (PLR) difference based on heart failure (HF) onset. Acute-onset=HF occurred during the hospitalization and/or <7 days after acute coronary syndrome (ACS); Late-onset=HF occurred later after ACS hospitalization (≥7 days-6 months). P value <0.05 (*) was considered statistically significant, and P value >0.05 (NS) was considered not statistically significant. Figure 2. Receiver operating characteristic curve of the final model consist of left ventricular ejection fraction and platelet-to-lymphocyte ratio to predict heart failure incidence at 6 months after acute coronary syndrome. AUC – area under curve.
Figure 2. Receiver operating characteristic curve of the final model consist of left ventricular ejection fraction and platelet-to-lymphocyte ratio to predict heart failure incidence at 6 months after acute coronary syndrome. AUC – area under curve. Figure 3. Receiver operating characteristic curve of platelet-to-lymphocyte ratio (PLR) as a predictor of heart failure (HF) incidence at 6 months. The best cut-off for PLR to discriminate 6-month HF is 87 (Sensitivity=89%, Specificity=63%, Odds ratio=2.92, 95% confidence interval 1.55–5.50, P<0.001). AUC – area under curve.
Figure 3. Receiver operating characteristic curve of platelet-to-lymphocyte ratio (PLR) as a predictor of heart failure (HF) incidence at 6 months. The best cut-off for PLR to discriminate 6-month HF is 87 (Sensitivity=89%, Specificity=63%, Odds ratio=2.92, 95% confidence interval 1.55–5.50, P<0.001). AUC – area under curve. Figure 4. Multivariate Cox regression hazard function analysis showing differences between patients with high and low platelet-to-lymphocyte ratio (PLR) associated with the outcome of HF occurring within 6 months after hospital admission for acute coronary syndrome. The hazard ratio for high PLR (PLR ≥87) is 4.5 (95% confidence interval=1.8–11, P=0.001).
Figure 4. Multivariate Cox regression hazard function analysis showing differences between patients with high and low platelet-to-lymphocyte ratio (PLR) associated with the outcome of HF occurring within 6 months after hospital admission for acute coronary syndrome. The hazard ratio for high PLR (PLR ≥87) is 4.5 (95% confidence interval=1.8–11, P=0.001). Figure 5. Scatter plots showing the association between (A) platelet-to-lymphocyte ratio (PLR) and Global Registry of Acute Coronary Events score (GRACE) risk score, (B) PLR and left ventricular ejection fraction (LVEF).
Figure 5. Scatter plots showing the association between (A) platelet-to-lymphocyte ratio (PLR) and Global Registry of Acute Coronary Events score (GRACE) risk score, (B) PLR and left ventricular ejection fraction (LVEF). Tables
 Table 1. Baseline characteristics of study population.
Table 1. Baseline characteristics of study population. Table 2. In-hospital and long-term outcomes of patients with acute coronary syndrome.
Table 2. In-hospital and long-term outcomes of patients with acute coronary syndrome. Table 3. Comparison of characteristics between acute coronary syndrome patients who develop heart failure during vs after hospitalization.
Table 3. Comparison of characteristics between acute coronary syndrome patients who develop heart failure during vs after hospitalization. Table 4. Risk factors for developing heart failure at 6 months after acute coronary syndrome.
Table 4. Risk factors for developing heart failure at 6 months after acute coronary syndrome. Table 1. Baseline characteristics of study population.
Table 1. Baseline characteristics of study population. Table 2. In-hospital and long-term outcomes of patients with acute coronary syndrome.
Table 2. In-hospital and long-term outcomes of patients with acute coronary syndrome. Table 3. Comparison of characteristics between acute coronary syndrome patients who develop heart failure during vs after hospitalization.
Table 3. Comparison of characteristics between acute coronary syndrome patients who develop heart failure during vs after hospitalization. Table 4. Risk factors for developing heart failure at 6 months after acute coronary syndrome.
Table 4. Risk factors for developing heart failure at 6 months after acute coronary syndrome. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








