27 July 2022: Meta-Analysis
The Prognostic Value of Periostin Expression in Non-Small Cell Lung Cancer: A Meta-Analysis
Mengjie Li1234ABCDEFG, Guangzhi Ma1ABCDEF, Xuebing Li2ACFG*, Qinghua Zhou12ACFGDOI: 10.12659/MSM.936898
Med Sci Monit 2022; 28:e936898
Abstract
BACKGROUND: Non-small cell lung cancer (NSCLC) is one of the leading causes of cancer-related death in the world and its poor prognosis is a major concern. Periostin was found to be associated with the prognosis of NSCLC. However, the research results were inconsistent. This meta-analysis evaluated the correlation between periostin expression and the prognosis of NSCLC.
MATERIAL AND METHODS: A meta-analysis was performed on data acquired from PubMed, EMBASE, the Cochrane Library, China National Knowledge Infrastructure (CNKI), and Wanfang Database from inception to 18 June 2022. Published and unpublished studies investigating the correlation between periostin expression and the prognosis of NSCLC were included in this meta-analysis. Eligible studies reported at least 1 of the following clinical outcome measures: overall survival, progression-free survival, cancer-specific survival, relapse-free survival, disease-free survival, or other clinical parameters of prognosis. Pooled hazard ratios (HR) with 95% confidence interval (CI) were calculated using the random-effects model. Sensitivity and subgroup analyses and assessment of publication bias were also conducted.
RESULTS: This meta-analysis enrolled 2504 NSCLC cases from 12 eligible studies. The hazard ratio for the overall survival was 1.761 (95% CI: 1.022-3.033, P=0.041). Heterogeneity was significant among the studies, but publication bias was lacking. Subgroup analyses were performed based on different issues, such as districts, antibodies and methods for periostin detection.
CONCLUSIONS: Overexpression of periostin is a negative prognostic factor and is associated with worse overall survival (OS) in NSCLC patients. Periostin may serve as a prognostic biomarker for NSCLC patients.
Keywords: non-small cell lung cancer, Prognosis, Periostin, Meta-Analysis, Carcinoma, Non-Small-Cell Lung, Disease-Free Survival, Humans, Lung Neoplasms, Neoplasm Recurrence, Local
Background
Lung cancer is the leading cause of cancer-associated mortality globally in both men and women [1]. In 2018, over 230 000 new cases of lung cancer (13% of all cancer diagnoses) and over 150 000 deaths (25% of cancer deaths) were reported in the United States [2]. NSCLC is the most common type of lung cancer, and accounts for 80–90% of all the lung cancer cases [3]. Routine treatments for NSCLC include surgery, chemotherapy, and radiotherapy, but the benefits of these treatments are limited for patients in advanced stages [4,5]. Despite the promising development of molecular-targeted therapies, the outcomes of patients with stage III/IV NSCLC remains unsatisfactory, with a 5-year survival rate around 16% [6–8]. Several serum-based tumor biomarkers have been applied to monitor cancer treatment, such as neuron-specific enolase (NSE), cytokeratin 19 fragment (CYFRA21-1), and carcinoembryonic antigen (CEA) [9]. However, due to their low sensitivity and specificity, these biomarkers have limited ability to predict the prognosis of NSCLC [10]. Therefore, new biomarkers for prognosis of NSCLC are needed.
Periostin (POSTN), also referred to as osteoblast-specific factor 2, is a 93.3-kDa extracellular matrix (ECM) protein that was identified in murine osteoblast-like cells in 1993 [11]. Periostin has been detected in a wide variety of normal tissues, and especially in tissues under stress conditions such as heart under pressure or volume overload and skeletal muscle after injury [12,13]. Previous studies have shown that a high level of periostin is strongly associated with malignant behavior in many kinds of malignancies such as esophageal cancer, breast carcinoma, and NSCLC [14–16]. Periostin has been studied and found to be associated with cancer-related death and employed as a useful prognostic indicator in many kinds of solid tumors [17]. A meta-analysis involving 993 patients with cancer demonstrated that periostin overexpression was markedly associated with poor overall survival (OS) (HR=2.35, 95% CI=1.88–2.93) and worse disease-free survival (DFS) (HR=2.70, 95% CI=2.00–3.65) [17]. These data showed that periostin could be a potential cancer prognostic biomarker.
The prognostic role of periostin in NSCLC has been reported in various studies [16,18–25]. Many studies indicated that periostin was associated with a decrease in survival and as a negative prognostic factor, while others did not reach to any conclusive and relevant result indicating that periostin was associated with the prognosis of NSCLC [26–28]. In view of the inconsistent results across these studies, we aimed to perform a systematic review and meta-analysis of published research to assess the prognostic value of periostin in NSCLC patients.
Material and Methods
DATA SOURCES AND SEARCHES:
We searched PubMed, the Cochrane Library, EMBASE, Wanfang Database, and China National Knowledge Infrastructure (CNKI) to find relevant articles up to 18 June 2022 in all languages using the following text word or Medical Subject Heading terms: (“non-small-cell lung cancer”) OR “non-small cell lung cancer” OR “non small-cell lung cancer” OR “non small cell lung cancer” OR “non-small-cell lung carcinoma” OR “non-small cell lung carcinoma” OR “non small-cell lung carcinoma” OR “non small cell lung carcinoma” OR “nsclc”) AND (“osteoblast-specific factor 2” OR “periostin” OR “osteoblast specific factor” OR “OSF-2 protein” OR “periostin protein”) AND (“prognosis” OR “prognostic” OR “survival” OR “recurrence”). We also manually searched the reference lists of relevant reviews and original articles to identify other eligible studies.
STUDY SELECTION:
Two reviewers independently screened the titles and abstracts of the retrieved articles, then the relevant studies were reviewed as full-text articles.
Studies that met the following inclusion criteria were considered eligible and taken into consideration: (1) All articles were written and published in English with the availability of the full text of the article; (2) Patients were pathologically diagnosed with NSCLC; (3) Periostin was detected by conventional methods, and its association with survival or other clinical parameters of prognosis was demonstrated; (4) The necessary data can be acquired, including overall survival (OS), progression-free survival (PFS), cancer-specific survival (CSS), relapse-free survival (RFS), disease-free survival (DFS) or other clinical parameters of prognosis; (5) The presence of statistical analysis including hazard ratios (HRs) and the 95% confidence interval (CI), or data that could be utilized to estimate the HRs and 95% CIs such as Kaplan-Meier survival curves.
Studies not meeting the inclusion criteria were excluded. Other exclusion criteria were: (1) Articles which were a review or systematic review, conference paper, commentary, case report, letter, or expert opinion; (2) Laboratory studies, such as studies on animals or
DATA EXTRACTION AND RISK OF BIAS ASSESSMENT:
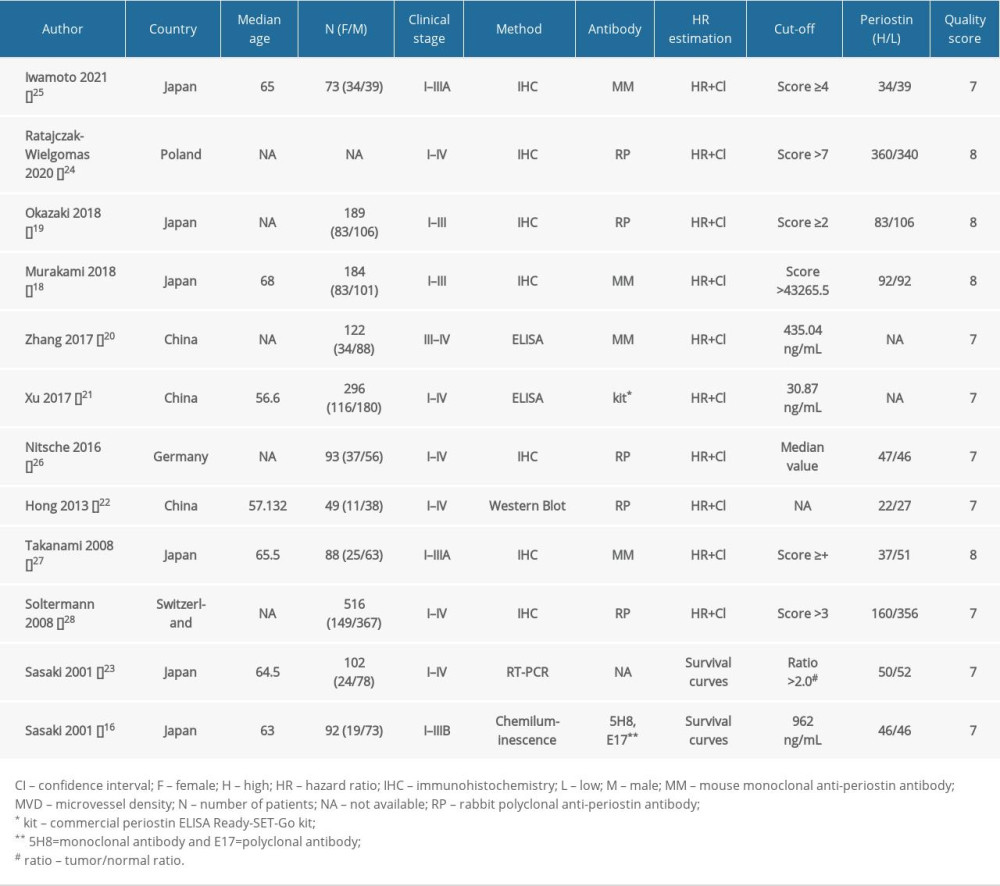
Basic information was extracted using a collection form: publication year, country, name of first author, number of patients involved, median age, sex, clinical stage, method used to detect periostin, antibodies used for detection, cut-off value to define high periostin expression, and number of patients with high and low periostin expression.
The prognostic endpoints were PFS, OS, RFS, CSS, or DFS. We extracted HRs and 95% CIs from either univariate/multivariate analysis or Kaplan-Meier survival curves by use of Engauge Digitizer 4.1 [30].
We assessed risk of bias of individual studies using the Newcastle-Ottawa Scale (NOS) criteria [31]. The NOS was used to assess 3 aspects: subject selection, comparability of the subject, and clinical outcome. The scores of NOS ranged from 0 to 9 stars. Studies with NOS score values ≥6 stars were considered to be high quality.
All investigators independently conducted study selection and data extraction. Two investigators (ML and GM) independently assessed risk of bias of individual studies. Any discrepancies were resolved by consensus and arbitration by a panel of adjudicators (ML, GM, XL, and QZ).
DATA SYNTHESIS AND STATISTICAL ANALYSIS:
The STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used for the process of data calculation and analysis. We extracted LogHRs and variances for survival evaluation. If provided indirectly, the HR was extracted from the Cox regression model or Kaplan-Meier curve. If both univariate and multivariate survival analyses existed, we chose multivariate analysis first. If adjusted and unadjusted HRs were both provided, we used the adjusted HR. I2 statistic test and chi-square-based Q test were used to test the heterogeneity among the included studies [32]. If the heterogeneity among the studies was insignificant (P>0.10 or I2<50%), the pooled HR was estimated with the fixed-effect model (Mantel-Haenszel method) [33]. Otherwise, the random-effect model was used to reduce the impact of heterogeneity. Publication bias was evaluated by Begg’s method [34]. P<0.05 was considered to be statistically significant.
Results
STUDY SELECTION:
The initial search retrieved 244 important articles, and the detailed reasons for exclusion are displayed in the flow chart (Figure 1). In total, we identified 12 cohort studies in this analysis.
STUDY CHARACTERISTICS:
The basic information of the 12 eligible studies is listed in Table 1. All the studies that met the inclusion criteria were published between 2001 and 2021, and were conducted in Japan [16,18,19,23,25,27], China [20–22], Poland [24], Germany [26], and Switzerland [28]. A total of 2504 cases were included in this meta-analysis. All the cases were diagnosed with NSCLC based on histology reports, and their clinical stages varied from I to IV. Various methods were used to detect periostin. The most common methods were immunohistochemistry (IHC) [18,19,24–28] staining of tumor tissue specimens, enzyme-linked immunosorbent assay (ELISA) [20,21], and western blot [22] analysis for serum samples. The HRs were acquired directly from most studies [16,18–22,24–28] except for Sasaki’s [23] study, in which they were extracted from the survival curve. All the NOS scores of the included studies were no less than 7.
META-ANALYSIS RESULTS:
OS and PFS evaluated the prognostic value of overexpression of periostin in NSCLC. OS was extracted from most of the included studies, and the pooled HR was 1.761 (95% CI: 1.022–3.033, P=0.041; Figure 2), indicating that high periostin was a negative prognostic factor in NSCLC patients. The heterogeneity was statistically significant (I2=76.0%, P=0.000); therefore, a random-effects model was applied. Only 4 of the included studies provided PFS, and the pooled HR was 1.296 (95% CI: 0.965–1.740, P=0.085; Figure 3). In this procedure, random-effects models were also used because of the statistically significant heterogeneity (I2=80.3%, P=0.002).
SUBGROUP ANALYSIS:
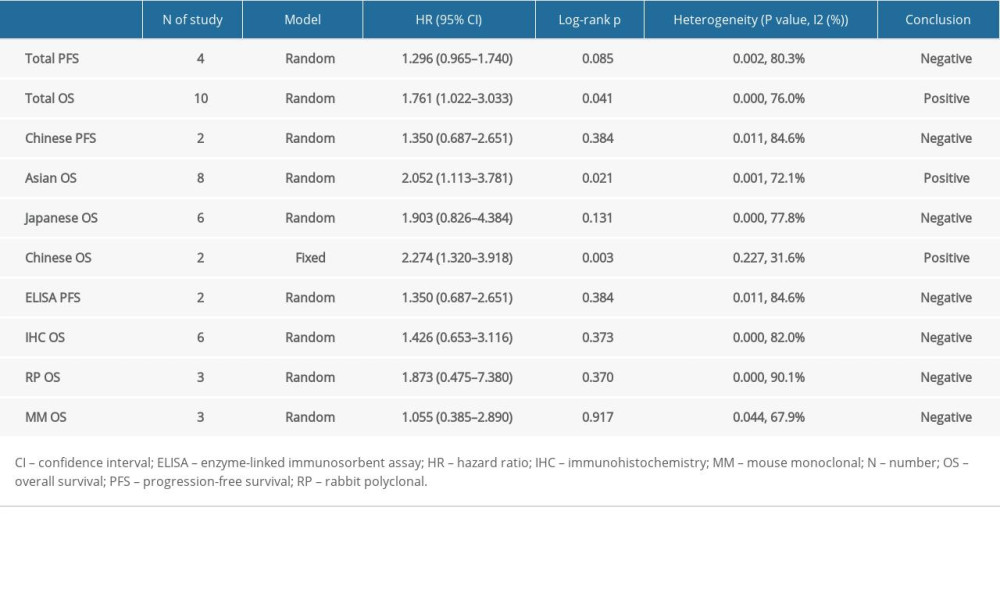
Subgroup analysis was performed based on the extracted information from all the eligible studies. Subgroups were stratified by region (Asian/Chinese/Japanese), detection methods of periostin (IHC/ELISA), and antibodies for periostin detection (rabbit polyclonal/mouse monoclonal), as shown in Table 2.
REGION (ASIAN/CHINESE/JAPANESE):
In total, there were 9 eligible studies from Asia. Among these studies, 6 were from Japan and the others were from China. Considering the Asian studies, the combined HR of OS was 2.052 (95% CI: 1.113–3.781,
DETECTION METHODS FOR PERIOSTIN (IHC/ELISA):
Detection methods for periostin varied among studies, and the most common were IHC and ELISA. IHC was used in 6 studies, and the pooled HR of OS was 1.426 (95% CI: 0.653–3.116,
ANTIBODIES FOR PERIOSTIN DETECTION (RABBIT POLYCLONAL/MOUSE MONOCLONAL):
Three of 12 eligible studies used rabbit polyclonal. For these studies, the pooled HR for OS was 1.873 (95% CI: 0.475–7.380,
All summarized results are listed in Table 2.
PUBLICATION BIAS:
To assess publication bias, Begg’s test was performed, but no evidence of publication bias was found (P=0.283) (Figure 4).
Discussion
The aim of this meta-analysis was to integrate the results of the previous studies to arrive at a summary conclusion on the prognostic value of the expression of periostin in NSCLC. The results demonstrated that overexpression of periostin was correlated with poorer OS in NSCLC patients. However, there was an insignificant correlation between PFS and high periostin expression in NSCLC patients. Due to the emergence of various new cancer treatments, including new targeting therapy and immunotherapy, OS and PFS of NSCLC patients have been continuously extended in recent years. Because of the different treatment plans in enrolled studies, the difference in prognosis is large. This may be the main restriction of the results of this meta-analysis.
In the subgroup analysis, high periostin expression in the Asian patients was related to shorter OS. In Japanese patients, the relationship between high periostin with OS was insignificant. Compared with the Chinese patients, high periostin was significantly linked with OS rather than PFS. Concerning the different methods for periostin detection, no relation was found between high periostin and prognosis. And for now, no research has demonstrated which is the most reliable method for periostin detection. Similarly, for different antibodies for periostin detection (rabbit polyclonal or mouse monoclonal), no relation was found between high periostin and prognosis.
Since Takeshita and Kikuno [35] cloned periostin from a murine osteoblast-like cell line in 1993, advancements have been accomplished by in vitro and in vivo studies about periostin. Periostin is not only expressed in tumoral tissues, but also in benign lung diseases such as asthma [36], idiopathic pulmonary fibrosis [37], and tuberculosis [38]. However, Zhang et al [20] demonstrated that the basal serum periostin levels were significantly elevated in NSCLC patients with advanced tumor stage compared with benign lung diseases. As an ECM protein, periostin plays important roles in the formation of a tumor-supportive microenvironment [39]. Recent studies revealed that periostin not only exerts its tumor-promoting effect by binding to integrins to activate cell-signaling pathways, but is also an inductor of epithelial–mesenchymal transition (EMT) [15,39,40]. Overexpressed periostin was found to be correlated with high lymphatic microvessel density (LMVD) and blood microvessel density (MVD), and activated Erk/VEGF pathway, leading to tumor angiogenesis [27,40]. The epithelial–mesenchymal transition (EMT) is an important promoter of tumor invasion and metastasis. Recent studies have found that periostin was involved in the EMT by initiating cross-talks between the integrins and RTK at the plasma membrane, followed by activation of Akt/PKB and FAK pathways [41–45]. Moreover, preclinical studies show that periostin inhibits hypoxia-induced apoptosis via Akt/PKB and TGF-β pathways in A549 NSCLC cells and human periodontal ligament cells, respectively, which can promote tumor cell survival [46,47].
Drug resistance of tumor cells is a major cause of treatment failure, is a negative prognostic factor, and is responsible for unfavorable OS. Studies showed that periostin can induce chemoresistance by activating cell-signaling pathways, such as PI3K/Akt/survivin pathway [48–50]. Park et al [51] also found that periostin regulated tumor resistance to antiangiogenic therapy through activation of signal transducer and activator of transcription 3 (STAT3) in glioma. Thus, inhibition of periostin may sensitize tumor cells to anticancer drugs.
Despite the progress achieved, several issues remain unresolved. For example, it was reported that periostin produced by epithelial cells could inhibit proliferation and invasion in gastric cancer through stabilizing p53 and E-cadherin proteins via the Rb/E2F1/p14ARF/Mdm2 pathway [52], while in another study, periostin derived from stromal myofibroblasts markedly promoted gastric cancer cell growth [53]. These controversial results suggest that periostin derived from distinct types of cells may play different biological functions in tumorigenesis and metastasis [51]. Moreover, Kanno et al [54] demonstrated that periostin has a biphasic function of inducing and repressing pancreatic cancer. The best method to detect periostin and define the elevated periostin level remains uncertain. Thus, more comprehensive and high-quality studies on periostin are still warranted in the future.
To the best of our knowledge, this is the first meta-analysis providing comprehensive insights into the connection between overexpressed periostin and prognosis in NSCLC patients. Due to practical constraints, this study still has limitations. Firstly, all the included studies were observational studies, while no prospective RCT study was found in the literature searching process. Secondly, selection bias was inevitable in all the included studies. Thirdly, all of the included studies were published in English. Hence, it is possible that some eligible studies were omitted due to linguistic limitations. Similarly, eligible studies published in books or journals may have been missed due to the use of online databases. Fourthly, significant heterogeneities were observed in this study. Although subgroup analyses provided some potential sources of heterogeneity, we were not able to identify the source of heterogeneity entirely. There were significant differences in baseline characteristics among studies, such as cut-off value to define periostin overexpression. Because of the lack of available data, we could not evaluate their impacts on heterogeneity. However, in spite of these limitations, our study was performed with detailed protocols and careful statistical analysis with the aim to minimize bias. Therefore, the results of our study are reliable and may be used as a standard reference.
Conclusions
In conclusion, this meta-analysis suggests that overexpressed periostin was a negative prognostic factor in NSCLC patients, especially for OS. However, there was an insignificant correlation between PFS and high periostin. Variations of antibodies used and methods for periostin detection may be major sources of the heterogeneity. Further prospective clinical studies based on large samples are still needed to explore the prognostic value of periostin in NSCLC.
Figures
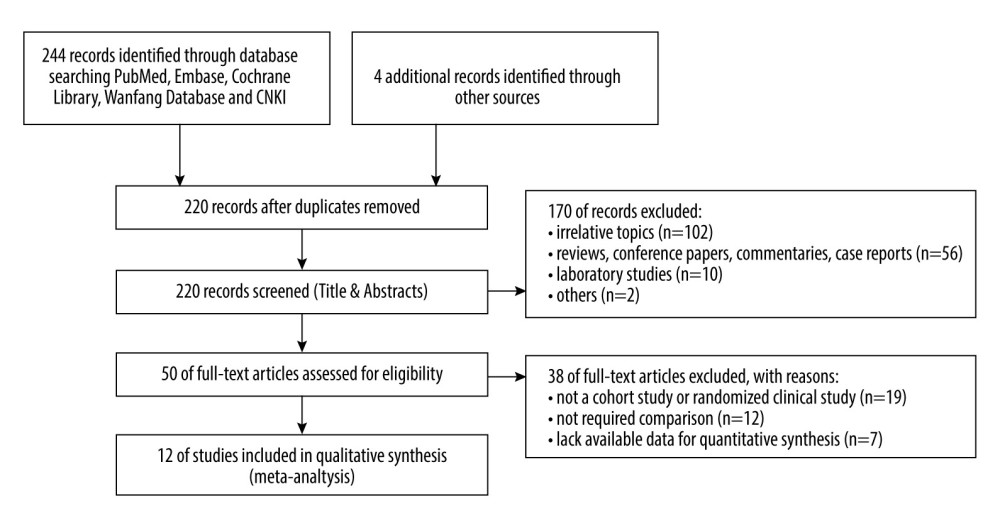 Figure 1. Flow diagram of the study selection process and specific reasons for exclusion in the meta-analysis.
Figure 1. Flow diagram of the study selection process and specific reasons for exclusion in the meta-analysis. 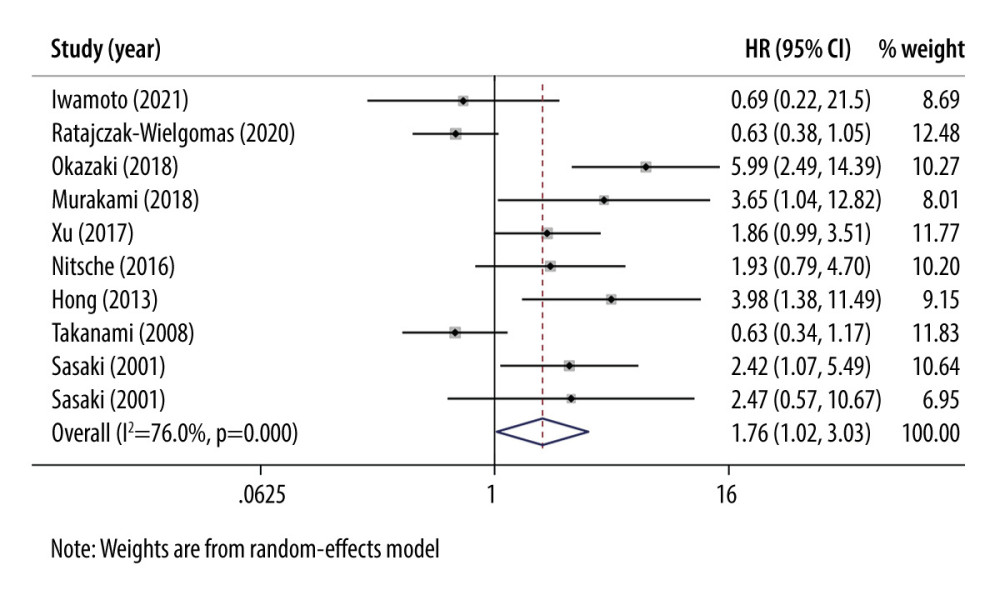 Figure 2. Forest plots of overall outcomes for overall survival (OS). Hazard ratios (HRs) for each trial are represented by squares, and horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for OS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used.
Figure 2. Forest plots of overall outcomes for overall survival (OS). Hazard ratios (HRs) for each trial are represented by squares, and horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for OS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used. 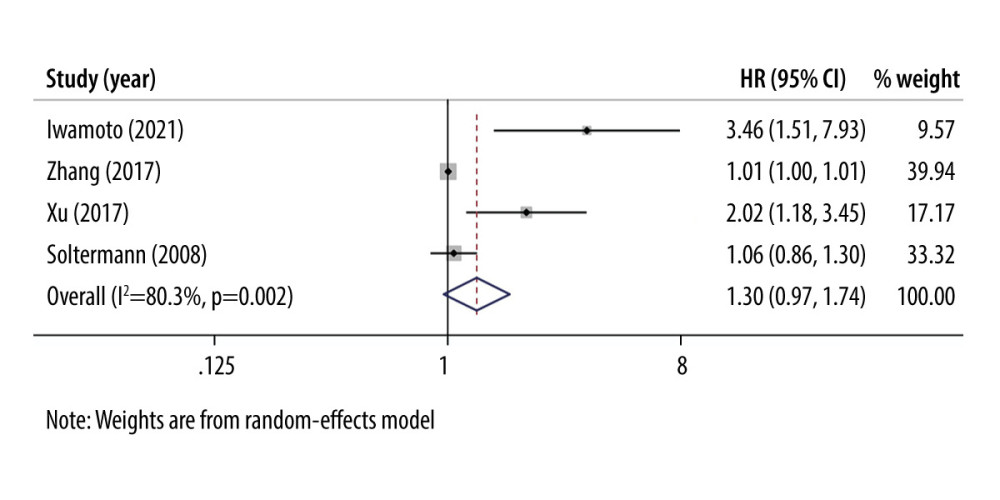 Figure 3. Forest plots of overall outcomes for progression-free survival (PFS). Hazard ratios (HRs) for each trial are represented by the squares, and the horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for PFS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used.
Figure 3. Forest plots of overall outcomes for progression-free survival (PFS). Hazard ratios (HRs) for each trial are represented by the squares, and the horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for PFS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used. 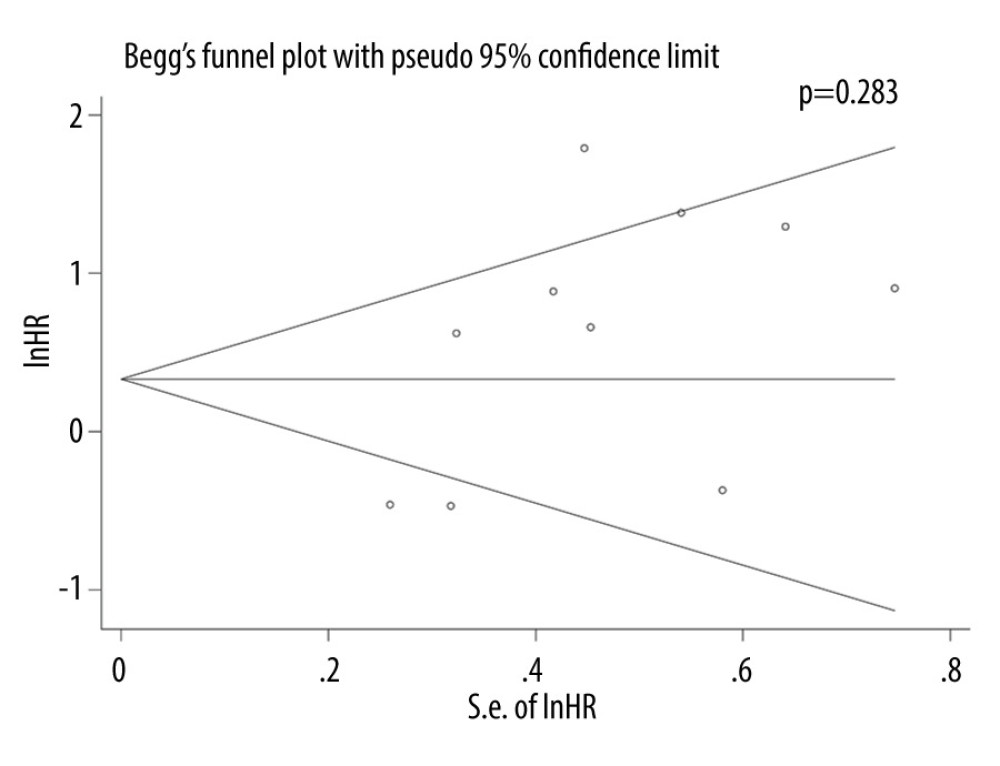 Figure 4. Begg’s publication bias plots of the studies that reported the correlation between periostin expression and NSCLC survival on OS. Each study is represented by 1 circle. The horizontal line represents the pooled effect estimate. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used.
Figure 4. Begg’s publication bias plots of the studies that reported the correlation between periostin expression and NSCLC survival on OS. Each study is represented by 1 circle. The horizontal line represents the pooled effect estimate. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used. References
1. Smith RA, Cokkinides V, Brawley OW, Cancer screening in the United States, 2009: A review of current American Cancer Society guidelines and issues in cancer screening: Cancer J Clin, 2009; 59; 27-41
2. Siegel RL, Miller KD, Jemal A: Cancer statistics, 2018, 2018; 68; 7-30
3. Siegel R, Ma J, Zou Z, Cancer statistics, 2014: Cancer J Clin, 2014; 64; 9-29
4. Ettinger DS, Aisner DL, Wood DE, NCCN Guidelines Insights: Non-small cell lung cancer, Version 5.2018: J Natl Compr Canc Netw, 2018; 16; 807-21
5. Wang J, Ji Z, Wang X, Radical thoracic radiotherapy may provide favorable outcomes for stage IV non-small cell lung cancer: Thorac Cancer, 2016; 7; 182-89
6. Sequist LV, Yang JC, Yamamoto N, Phase III study of afatinib or cisplatin plus pemetrexed in patients with metastatic lung adenocarcinoma with EGFR mutations: J Clin Oncol, 2013; 31; 3327-34
7. Gettinger S, Horn L, Jackman D, Five-year follow-up of nivolumab in previously treated advanced non-small-cell lung cancer: Results from the CA209–003 study: J Clin Oncol, 2018; 36; 1675-84
8. Wang Y, Sun Y, Clinical experiences with molecular targeted therapy in lung cancer in China: Thorac Cancer, 2015; 6; 379-84
9. Li XB, Gu JD, Zhou QH, Review of aerobic glycolysis and its key enzymes – new targets for lung cancer therapy: Thorac Cancer, 2015; 6; 17-24
10. Heukamp LC, Buttner RMolecular diagnostics in lung carcinoma for therapy stratification: Pathologe, 2010; 31; 22-28 [in German]
11. Takeshita S, Kikuno R, Tezuka K, Osteoblast-specific factor 2: Cloning of a putative bone adhesion protein with homology with the insect protein fasciclin I: Biochem J, 1993; 294(Pt 1); 271-78
12. Katsuragi N, Morishita R, Nakamura N, Periostin as a novel factor responsible for ventricular dilation: Circulation, 2004; 110; 1806-13
13. Goetsch SC, Hawke TJ, Gallardo TD, Transcriptional profiling and regulation of the extracellular matrix during muscle regeneration: Physiol Genomics, 2003; 14; 261-71
14. Michaylira CZ, Wong GS, Miller CG, Periostin, a cell adhesion molecule, facilitates invasion in the tumor microenvironment and annotates a novel tumor-invasive signature in esophageal cancer: Cancer Res, 2010; 70; 5281-92
15. Shao R, Bao S, Bai X, Acquired expression of periostin by human breast cancers promotes tumor angiogenesis through up-regulation of vascular endothelial growth factor receptor 2 expression: Mol Cell Biol, 2004; 24; 3992-4003
16. Sasaki H, Dai M, Auclair D, Serum level of the periostin, a homologue of an insect cell adhesion molecule, as a prognostic marker in nonsmall cell lung carcinomas: Cancer, 2001; 92; 843-48
17. Yang T, Deng Z, Prognostic value of periostin in multiple solid cancers: A systematic review with meta-analysis, 2020; 235; 2800-8
18. Murakami D, Takamori S, Kawahara A, Periostin expression in non-small cell lung cancer: Clinical significance: Kurume Med J, 2018; 64; 13-20
19. Okazaki T, Tamai K, Shibuya R, Periostin is a negative prognostic factor and promotes cancer cell proliferation in non-small cell lung cancer: Oncotarget, 2018; 9; 31187-99
20. Zhang Y, Yuan D, Yao Y, Predictive and prognostic value of serum periostin in advanced non-small cell lung cancer patients receiving chemotherapy: Tumour Biol, 2017; 39; 1010428317698367
21. Xu CH, Wang W, Lin Y, Diagnostic and prognostic value of serum periostin in patients with non-small cell lung cancer: Oncotarget, 2017; 8; 18746-53
22. Hong LZ, Wei XW, Chen JF, Overexpression of periostin predicts poor prognosis in non-small cell lung cancer: Oncol Lett, 2013; 6; 1595-603
23. Sasaki H, Lo KM, Chen LB, Expression of Periostin, homologous with an insect cell adhesion molecule, as a prognostic marker in non-small cell lung cancers: Jpn J Cancer Res, 2001; 92; 869-73
24. Ratajczak-Wielgomas K, Kmiecik A, Prognostic significance of stromal periostin expression in non-small cell lung cancer: Int J Mol Sci, 2020; 21; 7025
25. Iwamoto R, Tanoue S, Nagata S, T1 invasive lung adenocarcinoma: Thin-section CT solid score and histological periostin expression predict tumor recurrence: Mol Clin Oncol, 2021; 15; 228
26. Nitsche U, Stangel D, Pan Z, Periostin and tumor-stroma interactions in non-small cell lung cancer: Oncol Lett, 2016; 12; 3804-10
27. Takanami I, Abiko T, Koizumi S, Expression of periostin in patients with non-small cell lung cancer: Correlation with angiogenesis and lymphangiogenesis: Int J Biol Markers, 2008; 23; 182-86
28. Soltermann A, Tischler V, Arbogast S, Prognostic significance of epithelial-mesenchymal and mesenchymal-epithelial transition protein expression in non-small cell lung cancer: Clin Cancer Res, 2008; 14; 7430-37
29. Page MJ, McKenzie JE, Bossuyt PM, The PRISMA 2020 statement: An updated guideline for reporting systematic reviews: Syst Rev, 2021; 10; 89
30. Tierney JF, Stewart LA, Ghersi D, Practical methods for incorporating summary time-to-event data into meta-analysis: Trials, 2007; 8; 16
31. Stang A, Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses: Eur J Epidemiol, 2010; 25; 603-5
32. Higgins JP, Thompson SG, Deeks JJ, Altman DG, Measuring inconsistency in meta-analyses: Bmj, 2003; 327; 557-60
33. Mantel N, Haenszel W, Statistical aspects of the analysis of data from retrospective studies of disease: J Natl Cancer Inst, 1959; 22; 719-48
34. Begg CB, Mazumdar M, Operating characteristics of a rank correlation test for publication bias: Biometrics, 1994; 50; 1088-101
35. Takeshita S, Kikuno R, Tezuka K, Amann E, Osteoblast-specific factor 2: Cloning of a putative bone adhesion protein with homology with the insect protein fasciclin I: Biochem J, 1993; 294(Pt 1); 271-78
36. Li W, Gao P, Zhi Y, Periostin: Its role in asthma and its potential as a diagnostic or therapeutic target: Respir Res, 2015; 16; 57
37. Izuhara K, Conway SJ, Moore BB, Roles of periostin in respiratory disorders: Am J Respir Crit Care Med, 2016; 193; 949-56
38. Yamauchi M, Kinjo T, Diagnostic performance of serum interferon gamma, matrix metalloproteinases, and periostin measurements for pulmonary tuberculosis in Japanese patients with pneumonia, 2020; 15; e0227636
39. Morra L, Moch H, Periostin expression and epithelial-mesenchymal transition in cancer: A review and an update: Virchows Arch, 2011; 459; 465-75
40. Liu Y, Li F, Gao F, Periostin promotes tumor angiogenesis in pancreatic cancer via Erk/VEGF signaling: Oncotarget, 2016; 7; 40148-59, doi: 10.18632/oncotarget.9512
41. Kim CJ, Sakamoto K, Tambe Y, Inoue H, Opposite regulation of epithelial-to-mesenchymal transition and cell invasiveness by periostin between prostate and bladder cancer cells: Int J Oncol, 2011; 38; 1759-66
42. Li G, Jin R, Norris RA, Periostin mediates vascular smooth muscle cell migration through the integrins alphavbeta3 and alphavbeta5 and focal adhesion kinase (FAK) pathway: Atherosclerosis, 2010; 208; 358-65
43. Yan W, Shao R, Transduction of a mesenchyme-specific gene periostin into 293T cells induces cell invasive activity through epithelial-mesenchymal transformation: J Biol Chem, 2006; 281; 19700-8
44. Bao S, Ouyang G, Bai X, Periostin potently promotes metastatic growth of colon cancer by augmenting cell survival via the Akt/PKB pathway: Cancer Cell, 2004; 5; 329-39
45. Morra L, Rechsteiner M, Casagrande S, Characterization of periostin isoform pattern in non-small cell lung cancer: Lung Cancer, 2012; 76; 183-90
46. Aukkarasongsup P, Haruyama N, Matsumoto T, Periostin inhibits hypoxia-induced apoptosis in human periodontal ligament cells via TGF-beta signaling: Biochem Biophys Res Commun, 2013; 441; 126-32
47. Ouyang G, Liu M, Ruan K, Upregulated expression of periostin by hypoxia in non-small-cell lung cancer cells promotes cell survival via the Akt/PKB pathway: Cancer Lett, 2009; 281; 213-19
48. Xiao ZM, Wang XY, Wang AM, Periostin induces chemoresistance in colon cancer cells through activation of the PI3K/Akt/survivin pathway: Biotechnol Appl Biochem, 2015; 62; 401-6
49. Sung PL, Jan YH, Lin SC, Periostin in tumor microenvironment is associated with poor prognosis and platinum resistance in epithelial ovarian carcinoma: Oncotarget, 2016; 7; 4036-47
50. Hu W, Jin P, Liu W, Periostin contributes to cisplatin resistance in human non-small cell lung cancer A549 cells via activation of Stat3 and Akt and upregulation of survivin: Mol Cancer, 2016; 38; 1199-208
51. Park SY, Piao Y, Jeong KJ, Periostin (POSTN) regulates tumor resistance to antiangiogenic therapy in glioma models: Mol Cancer Ther, 2016; 15; 2187-97
52. Lv HJ, Liu R, Fu J, Epithelial cell-derived periostin functions as a tumor suppressor in gastric cancer through stabilizing p53 and E-cadherin proteins via the Rb/E2F1/p14ARF/Mdm2 signaling pathway: Cell Cycle, 2014; 13; 2962-74
53. Kikuchi Y, Kunita A, Iwata C, The niche component periostin is produced by cancer-associated fibroblasts, supporting growth of gastric cancer through ERK activation: Am J Pathol, 2014; 184; 859-70
54. Kanno A, Satoh K, Masamune A, Periostin, secreted from stromal cells, has biphasic effect on cell migration and correlates with the epithelial to mesenchymal transition of human pancreatic cancer cells: Int J Cancer, 2008; 122; 2707-18
Figures
 Figure 1. Flow diagram of the study selection process and specific reasons for exclusion in the meta-analysis.
Figure 1. Flow diagram of the study selection process and specific reasons for exclusion in the meta-analysis. Figure 2. Forest plots of overall outcomes for overall survival (OS). Hazard ratios (HRs) for each trial are represented by squares, and horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for OS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used.
Figure 2. Forest plots of overall outcomes for overall survival (OS). Hazard ratios (HRs) for each trial are represented by squares, and horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for OS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used. Figure 3. Forest plots of overall outcomes for progression-free survival (PFS). Hazard ratios (HRs) for each trial are represented by the squares, and the horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for PFS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used.
Figure 3. Forest plots of overall outcomes for progression-free survival (PFS). Hazard ratios (HRs) for each trial are represented by the squares, and the horizontal lines crossing the square show the 95% confidence intervals (CIs). The diamonds represent the estimated pooled effect of the overall outcome for PFS in NSCLC. All P values are two-sided. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used. Figure 4. Begg’s publication bias plots of the studies that reported the correlation between periostin expression and NSCLC survival on OS. Each study is represented by 1 circle. The horizontal line represents the pooled effect estimate. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used.
Figure 4. Begg’s publication bias plots of the studies that reported the correlation between periostin expression and NSCLC survival on OS. Each study is represented by 1 circle. The horizontal line represents the pooled effect estimate. STATA (version 13.1; Stata Corporation, College Station, TX, USA) was used. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387