08 July 2022: Clinical Research
A Single-Center Study Comparing the Effects of Thoracic Spine Manipulation vs Mobility Exercises in 26 Office Workers with Chronic Neck Pain: A Randomized Controlled Clinical Study
Jongmin Seo1BCDF, Changho Song2CDF, Doochul Shin3ADEG*DOI: 10.12659/MSM.937316
Med Sci Monit 2022; 28:e937316
Abstract
BACKGROUND: Neck pain is associated with computer work, poor posture, imbalanced neck muscles, and fatigue, particularly in office workers. This study from a single center aimed to compare the effects of thoracic spine mobility exercise and thoracic spine manipulation to improve cervical spine range of motion in 26 office workers who had chronic neck pain for more than 12 weeks.
MATERIAL AND METHODS: The participants were 26 office workers with neck pain lasting >12 weeks. These participants were randomly assigned to undergo TSME (n=13) or TSM (n=13). Both groups underwent cervical joint mobilization and deep cervical flexor muscle exercises for 25 min a day, twice weekly, for 6 weeks. The TSME group additionally performed TSME 15 min a day, twice a week, for 6 weeks, while the TSM group received TSM 2 times a day, twice a week, for 6 weeks. Cervical and thoracic spine ROM, numeric pain rating scale (NPRS), and neck disability index (NDI) were measured before and after interventions. The ROM of cervical and thoracic spine was measured using a dual inclinometer.
RESULTS: Both groups showed significant changes in cervical spine ROM, thoracic spine ROM, NPRS, and NDI after intervention compared to before intervention (P<0.05). Cervical spine right lateral flexion and right rotation differed significantly between the groups (P<0.05), while thoracic spine ROM, NPRS, and NDI did not.
CONCLUSIONS: TSME and TSM have similar effects in improving pain and disability in office workers with non-specific chronic neck pain.
Keywords: Exercise Therapy, Musculoskeletal Manipulations, Neck Pain, Thoracic Vertebrae, Cervical Vertebrae, chronic pain, Humans, Manipulation, Spinal, Pain Measurement, Range of Motion, Articular
Background
Neck pain is a common symptom experienced by approximately 67% of the population at least once in their lifetime [1] and is associated with computer work, poor posture, imbalanced neck muscles, and fatigue [2–5]. In particular, office workers maintain their necks and upper bodies in a static posture while using computers; the simultaneous use of a keyboard and mouse, which require dynamic movements, leads to incorrect postures for prolonged periods [6]. Among incorrect postures that cause neck pain, forward head posture, which is mainly observed in office workers, is characterized by excessive extension of the upper cervical spine, excessive flexion of the lower cervical spine, increased thoracic kyphosis, and increased load on the cervical spine muscles and joints from the limited movement of the cervical and thoracic spine [7,8].
The cervical and thoracic spine have a biomechanical relationship. The thoracic spine supports and affects the kinematics of the cervical spine through the cervical-thoracic junction [9]. Impairment of thoracic and cervical spine mobility is a key characteristic of neck pain, and movement of the cervical spine is related to thoracic spine mobility and posture [9]. Somatic dysfunctions such as limited mobility and postural imbalance of the thoracic spine can cause chronic neck pain [10]. Chronic neck pain is pain that usually lasts more than 12 weeks. Falla et al investigated the range of motion (ROM) of thoracic spine rotation during walking in subjects with and without neck pain. Subjects with neck pain showed lower ROM of rotational motion of the thoracic spine compared to subjects without neck pain [11]. Moreover, in their study on the correlation between sagittal thoracic mobility and neck pain, Kaya and Celenay reported that thoracic spine mobility was negatively correlated with neck pain severity [12].
Restricted thoracic spine mobility is one cause of neck pain [9]. Manual therapy such as thoracic spine manipulation (TSM) or mobilization to increase thoracic spine mobility significantly improves cervical spine ROM, pain, and dysfunction in individuals with neck pain [13,14]. Recent studies on active thoracic spine mobility exercise (TSME) for neck pain relief showed that active exercise therapy programs such as TSME and self-exercise effectively improved cervical spine ROM, thoracic spine ROM, pain, thoracic spine dysfunction, and psychological and social characteristics in patients with neck pain [15].
Active therapeutic interventions are more effective than passive therapeutic interventions for the treatment of patients with neck pain [16]. In addition, among the various interventions for chronic neck pain, therapeutic exercises and muscular reeducation are known to be effective [17]. Despite various studies on the effects of therapeutic exercise for neck pain, high-quality evidence on exercise therapy for neck pain is still lacking [18].
Most studies comparing interventions for neck pain only compared passive therapies such as TSM and mobilization or additionally conducted TSME to treat neck pain. Few studies have compared the effects of passive thoracic spine correction and active TSME in office workers with neck pain. Therefore, this study from a single center aimed to compare the effects of TSME and TSM to improve cervical and thoracic spine ROM, pain, and neck dysfunction in 26 office workers who had chronic neck pain for more than 12 weeks. The hypothesis of this study is that the effects of TSME and TSM on the pain intensity and neck disability level of office workers with non-specific chronic neck pain will be different.
Material and Methods
SUBJECTS:
The participants of this study were 28 adult men and women who worked in offices at Company S in Seoul and had had chronic neck pain for >12 weeks, and all subjects were diagnosed with non-specific neck pain by a physician. The specific selection criteria of the participants were as follows: office workers engaged in program development and design, general affairs, human resources, accounting, sales, and planning; with neck pain lasting >12 weeks; and with a NPRS of ≥3. The exclusion criteria were office workers with spine diseases such as congenital deformities, spinal disc herniation, and stenosis, orthopedic diseases of the shoulder, neurological symptoms, and traffic accidents within the last 12 weeks, pregnancy, and increased neck pain during the study.
An announcement was made in the company to recruit 28 office workers with chronic neck pain. Two participants with orthopedic shoulder disease were excluded; thus, the final analyses included 26 participants.
PROCEDURE:
This study featured a randomized controlled clinical study design. A total of 26 non-specific chronic neck pain patients were recruited for this study. After assessment of general characteristics such as age, height, weight, and pain intensity, the baseline assessment was conducted. The cervical and thoracic spine ROMs and neck disability index (NDI) were evaluated.
Thoracic and cervical spine ROMs were measured using a digital inclinometer and goniometer. The NDI was assessed using a questionnaire. After baseline assessment, 26 participants were randomly assigned to TSME or TSM group with 13 participants in a 1: 1 ratio. For random group assignment of participants, the envelope-opening method was used.
The TSME group performed TSME for 10 min a day, twice weekly, for 6 weeks. The TSM group performed TSM up to twice a day, twice a week, for 6 weeks. Both groups underwent cervical joint mobilization and cervical spine deep flexor muscle exercises for 25 min a day, twice weekly, for 6 weeks. Additionally, both groups conducted the same home exercise program consisting of cervical spine isometric exercise for 15 min a day, twice weekly, for 6 weeks. No participant dropped out during the study. After 6 weeks of intervention, post-intervention evaluations were conducted in the same way as the baseline assessment (Figure 1).
THORACIC SPINE MOBILITY EXERCISES:
The TSME was developed based on the exercise described by Henegahn et al [19]. The exercise consisted of movements in all directions of thoracic spine flexion, extension, lateral flexion, and rotation. In the thoracic spine extension exercise, both hands were locked behind the wrists and the back was placed on a foam roller with the feet positioned flat on the floor. The knee was maintained at 90° to perform the extension exercise on the foam roller (Figure 2A). Additionally, the hands were locked with the elbow on a chair. After kneeling, the hip was moved toward the heels to extend the thoracic spine (Figure 2B) [19]. In the thoracic spine flexion exercise, the thoracic spine was flexed by moving backward until the hip touched the heels in a quadruped position (Figure 2C).
This rotation exercise was conducted with participants lying on their sides. The elbows were straight and the palms were held together. The leg facing the ceiling was bent to the level of the stomach. Then, the arm facing the ceiling was moved backward in a large arc to rotate the thoracic spine (Figure 2D). Another thoracic spine rotation exercise was conducted as follows in a kneeling position, the hip touched the heels; the hand in the direction of rotation was placed behind the neck and the elbow of the opposite arm was placed on the floor; then, the torso was slowly rotated toward the ceiling (Figure 2E); for lateral flexion of the thoracic spine, both hands were locked behind the neck with the participant seated on a chair and the torso was then flexed laterally (Figure 2F).
THORACIC SPINE MANIPULATION:
The TSM included the distraction technique and upper mid-thoracic spine manipulation in the supine position, as described by Cleland et al [20].
First, in the distraction treatment, the hands were locked and placed around the neck. The mediator behind the participant held the wrists and fixed the sternum below the target area of the participant. Then, the wrists were pulled by the mediator to distract the thoracic spine. At the end of the participant’s thoracic spine, distraction was conducted at high speed in the upper rotation direction.
Second, the upper thoracic spine (T1–T4) was manipulated in the supine position. The participants locked their hands behind their necks in the supine position. The mediator then fixed the main hand on the segment (T4) below the corrected segment (T3); the other hand was used to grab and fix the elbow of the participant. Then, the weight of the mediator’s body was moved in the direction of the participant’s arm. At the end of the thoracic spine, high-speed, low-amplitude movements were performed in the direction of the participant’s arm for correction.
Third, the mid-thoracic spine (T5–8) was manipulated as follows. In the supine position, the participant’s hands were locked behind their neck. The mediator fixed the main hand on the segment (T6) below the corrected segment (T5); the other hand was used to grab and fix the participant’s elbow. Then, the weight of the mediator’s body was moved in the direction of the participant’s arm. At the end of the thoracic spine, high-speed, low-amplitude movements were performed in the direction of the participant’s arm for correction. If a popping sound was not heard immediately after correction, the procedures were repeated up to 2 times.
CERVICAL JOINT MOBILIZATION:
Cervical joint mobilization was performed using anterior and lateral glide of the cervical spinous processes, as described by Edmond [21]. For anterior glide using the cervical spinous processes, the participant was placed in supine position. The mediator was positioned near the participant’s head and placed the thumb of the main hand on top of the thumb of the supporting hand, which was placed over the painful and low-mobility spinous process to glide the spinous process in an anterior direction. The lateral glide using the cervical spinous processes was conducted in the same manner but in a different direction and hand position. The thumb of the supporting hand was fixed at the lateral spinous process in the direction of glide, while the thumb of the main hand was placed on the lateral spinous process in the opposite direction for gliding. Cervical joint mobilization was applied to the segments with the most severe pain and limited movement. Joint mobilization of levels 1–3 was applied according to the pain pattern and movement restriction of the participants.
DEEP CERVICAL FLEXOR MUSCLE EXERCISES:
The cervical stabilization exercises included the deep cervical flexor muscle activation exercise described by Chiu and the cervical isometric exercise described by Chung and Jeong [22,23]. The deep cervical muscle activation exercise was conducted by placing a stabilizer pressure biofeedback device (Chattanooga, USA) on the occiput to create a neutral position of the cervical spine in the supine position. Each participant was then instructed to touch the roof of the mouth with their tongue. The stabilizer pressure biofeedback device was then placed behind the neck at 20 mm Hg. The mediator asked the participant to slowly nod their head to gradually increase and maintain the pressure at 30 mmHg for 10 s. After practicing, a 15-s break was provided, followed by 15 min of cervical deep muscle activation exercise. The exercise was paused when muscle fatigue was felt or the muscle did not contract.
The cervical isometric exercises were performed at home and comprised 6 movements: cervical spine flexion, extension, right lateral flexion, left lateral flexion, right rotation, and left rotation. The movement of the neck was resisted with the hand at 30% of the maximum neck strength. The hand was pushed to contract the neck muscles. A hand was used to prevent changes in the joint angle of the cervical spine. The cervical spine muscle was contracted for 10 s. A total of 10 sets of contraction for 10 s and rest for 15 s was conducted for each of the 6 exercises.
CERVICAL SPINE ROM:
A digital dual inclinometer (J-TECH Medical Dualer IQ Pro Manual; J-TECH Medical, USA) and a goniometer (Shindongbang Medical, Korea) were used to measure the cervical spine ROM. With the participant in a neutral standing position, the digital dual inclinometer was placed on the first thoracic spine and skull to set to zero. Then, the participant was asked to flex the neck to measure the cervical flexion ROM. To measure the cervical extension ROM, the digital dual inclinometer was placed on the first thoracic spine and skull of the participant to set to zero in a neutral standing position. The neck was then extended for measurements. In a neutral standing position, the digital dual inclinometer was placed on the first thoracic spine and skull of the participant to set to zero. After lateral flexion of the neck, the cervical lateral flexion ROM was measured with the participant in a neutral sitting position. The goniometer was placed on the skull and the cervical spine was rotated to measure the ROM of the nose. The measurements were made twice, with the average value used for the final analysis.
THORACIC SPINE ROM:
A digital dual inclinometer (J-TECH Medical Dualer IQ Pro Manual; Jech Medical, USA) was used to measure the thoracic spine ROM. With the participant in a neutral standing position, the digital dual inclinometer was placed on the 12th and 1st thoracic spine, and the zero was set. The thoracic spine was flexed to measure the ROM. Similarly, to measure the thoracic spine extension ROM, the digital dual inclinometer was placed on the 12th and 1st thoracic spine in a neutral standing position, and the zero was set. The thoracic spine was extended to measure the ROM. The measurements were made twice, with the average value used for the final analysis.
NUMERIC PAIN RATING SCALE:
The NPRS was used to measure pain intensity. The NPRS has sufficient discrimination power to explain the intensity of pain [24]. The scale evaluates the intensity of pain using numbers or words through several types of scales listed from 0 to 10. The pain rating ranges from 0 (no pain), 1–3 (mild pain, slight irritation or discomfort, slight impairment in daily life activities), 4–6 (moderate pain, ample impairment in daily life activities), and 7–10 (severe pain, inability to perform daily life activities).
NECK DISABILITY INDEX:
The NDI questionnaire was applied to determine the severity of the neck disability according to the pain. The NDI evaluates 10 domains: pain intensity, personal care (eg, washing, dressing), lifting objects, reading, headache, concentration, working, driving, sleeping, and leisure activities. Each item is scored from 0 points for no pain or no dysfunction to 5 points for intolerable pain or complete dysfunction. The questionnaire is self-reported, with the total score ranging from 0 to 50 points. A higher score indicated a more severe disability. The Cronbach’s alpha, indicating the reliability of the tool, was 0.82.
STATISTICAL ANALYSIS:
IBM SPSS Statistics for Windows, version 21.0 was used to perform the statistical analyses in this study. Means and standard deviations were calculated. Shapiro-Wilk normality tests were used to confirm the normal distribution of the participant data. Descriptive statistics were used to calculate the means and standard deviations of the general participant characteristics. Independent-sample
Results
The general characteristics of the TSME and TSM groups were homogeneous. The mean ages of these groups were 35.15±5.60 and 36.39±5.17 years, respectively, and did not differ significantly between the 2 groups. The mean height was 168.69±7.34 cm in the TSME group and 169.45±6.91 cm in the TSM group. The mean weights were 64.53±7.99 kg and 66.46±8.69 kg in the TSME and TSM groups, respectively. The mean heights and weights did not differ significantly between the 2 groups. The NPRS scores were 4.54±1.35 points in the TSME group and 4.92±1.5 points in the TSM group, with no significant difference between the 2 groups (Table 1).
In both groups, all cervical spine ROM, including flexion, extension, right lateral flexion, left lateral flexion, right rotation, and left rotation, differed significantly after the intervention compared to before the intervention (
Both TSME and TSM groups showed significant changes in thoracic flexion and extension ROM post-intervention compared to before the intervention (
The NPRS score was significantly reduced after the intervention compared to before the intervention in both the TSME and TSM groups (
Discussion
This study assessed and compared the effects of TSME and TSM on cervical and thoracic spine ROM, pain, and neck dysfunction. In this study, both TSME and TSM significantly improved all cervical spine ROM. Right lateral flexion and right rotation post-intervention also changed significantly between the groups. Although extension and flexion of the thoracic spine improved significantly post-intervention in both TSME and TSM groups, no other significant differences were observed between the groups.
The cervical and thoracic spine have a biomechanical relationship and structural interdependence. Changes in the thoracic spine affect cervical spine function, and thoracic spine dysfunction is commonly observed in individuals with neck pain [25]. Thoracic spine dysfunction, such as decreased mobility of the upper thoracic spine, causes pain in the muscles around the cervical spine and leads to cervical dysfunction [9]. Erdem et al reported that correction of Cyriax’s thoracic extension improved spinal alignment in patients with mechanical neck pain and increased the cervical flexion and rotation range through relaxation and pain reduction of the muscles around the spine [25]. Heggannavar and Battula compared the immediate effects of cross-upper TSM and thoracic spine distraction in adults with mechanical neck pain, reporting significantly increased cervical spine ROM after both interventions [26].
TSM changes the biomechanical movement of the cervical-thoracic junction to reduce tension of the muscles around the cervical spine, thereby improving cervical spine pain and ROM [27,28] in their study on the immediate effects of thoracic spine self-mobility exercise in patients with neck pain. In the present study, all joint ROMs of the cervical and thoracic spine were significantly increased in both groups post-intervention, consistent with previous findings. Therefore, the cervical mobilization and stabilization exercises applied in this study, as well as additional TSME and TSM, improved thoracic spine mobility in patients with chronic neck pain.
In the present study, we observed significant differences in the right lateral flexion and right rotation ROM of the cervical spine between the 2 groups. However, the right lateral flexion and rotation in both groups recovered to the normal angles of 40° and 80°, respectively. Although there were significant differences in the right lateral flexion and rotation of the cervical spine between the 2 groups, the restoration of normal ROM in both groups suggested no significant difference in the effects of the 2 treatment interventions. The experimental and control groups for cervical spine ROM and cervical flexion and extension showed small effect sizes of 0.1 and 0.35, respectively. However, the effect sizes of right lateral flexion, left lateral flexion, right rotation, and left rotation were 2.5, 0.5, 1.1, and 0.61, respectively, showing medium or greater effect sizes. Moreover, thoracic flexion showed a small effect size of 0.1 while thoracic extension showed a medium effect size of 0.6. These findings suggested that TSME combined with cervical spine mobilization and stabilization exercises may be more effective for cervical lateral flexion and rotation and thoracic extension ROM than TSM combined with cervical spine mobilization and stabilization exercises.
This study compared the effects of TSME and TSM on NPRS. Both groups showed significantly improved NPRS scores post-intervention, with no significant difference between the 2 groups. Park et al reported that sling thoracic active exercise relieved the pressure between the neck joints in women with neck pain and improved muscle fiber tension caused by chronic pain, thereby reducing activity and pain in the muscles around the cervical spine [29]. Although the effect of thoracic spine manipulation on neck pain has not been elucidated in detail, a systematic study found that thoracic spine manipulation can also be effective in improving pain and function [30]. Yang et al reported that upper TSM stimulated mechanoreceptors in the muscles, joints, and joint capsules of patients with neck pain to improve the transmitter response of the central nervous system and restore proprioception [31]. Thoracic manipulation improved information transmission of the central nervous system by mechanically stimulating the joint capsule, which resulted in increased ROM and reduced pain in the spine. In the present study, the NPRS scores were significantly decreased in both groups post-intervention compared to pre-intervention. These findings are consistent with those of previous studies in which TSME and TSM had positive effects on pain in patients with neck pain. However, the NPRS scores did not differ significantly between the 2 groups. This may be because the TSME and TSM had similar effects on thoracic spine ROM, which subsequently had comparable effects on neck pain. The effect size on neck pain improvement was 0.23, suggesting similar effects between TSME and TSM.
A score of 4 points on the NPRS determines the need for additional treatment, medication, or intervention for pain relief [32]. In the present study, both groups showed decreases to NPRS scores of 3 points or less after the intervention, indicating that neither group required additional treatment, medication, or interventions. These results suggested the beneficial effects of TSME and TSM on neck pain relief in office workers.
Although neck dysfunction changed significantly post-intervention in both groups in this study, we observed no significant difference between the groups. Thoracic spine mobility plays an important role in cervical spine dysfunction. In patients with chronic neck pain, dysfunctions such as decreased mobility of the thoracic spine and cage lead to increased pain of the cervical spine and altered movement [10]. Perveen et al reported that TSM and mobilization reduced muscle spasm around the spine and locking of facet joints in patients with neck pain, improving cervical spine pain and ROM and, subsequently, cervical dysfunction [33]. In the present study, consistent with previous findings, NDI was significantly improved post-intervention in both groups. TSME and TSM may have improved facet joint function and the biomechanical relationship between the cervical and thoracic spine in office workers with neck pain, thus increasing ROM and reducing pain and, consequently improving the NDI. However, the NDI did not differ significantly between the 2 groups. TSME and TSM actively and passively, respectively, led to changes in the joints and muscles. Although the 2 treatments showed different methods (passive versus active), the effects were similar, leading to no significant difference in NDI. The effect size for cervical dysfunction was.03, suggesting little to no difference between the experimental and control groups.
Several limitations must be considered in the interpretation of this study’s findings. First, too few participants were included in this study to generalize the findings to all individuals with neck pain. Second, although this study intended to investigate the effects of TSME and TSM, the independent effects on the thoracic spine could not be assessed as both cervical spine mobility and stabilization exercises were simultaneously applied. Third, this study was not blinded, so there may be bias in the study results. Lastly, the limited mobility of the thoracic spine of the participants could not be measured and quantified. Follow-up studies are needed to assess the effects of independent interventions of only TSME or TSM in patients with neck pain and limited thoracic spine mobility.
Conclusions
The purpose of this study was to investigate the effects of TSME and TSM on cervical spine ROM, thoracic spine ROM, pain, and neck dysfunction in office workers with chronic neck pain. As a result of the study, the effects of TSME and TSM on the improvement of cervical and thoracic ROM, NPRS, and NDI of patient with neck pain were confirmed. However, the effects of TSME and TSM on patients with neck pain was similar.
Figures
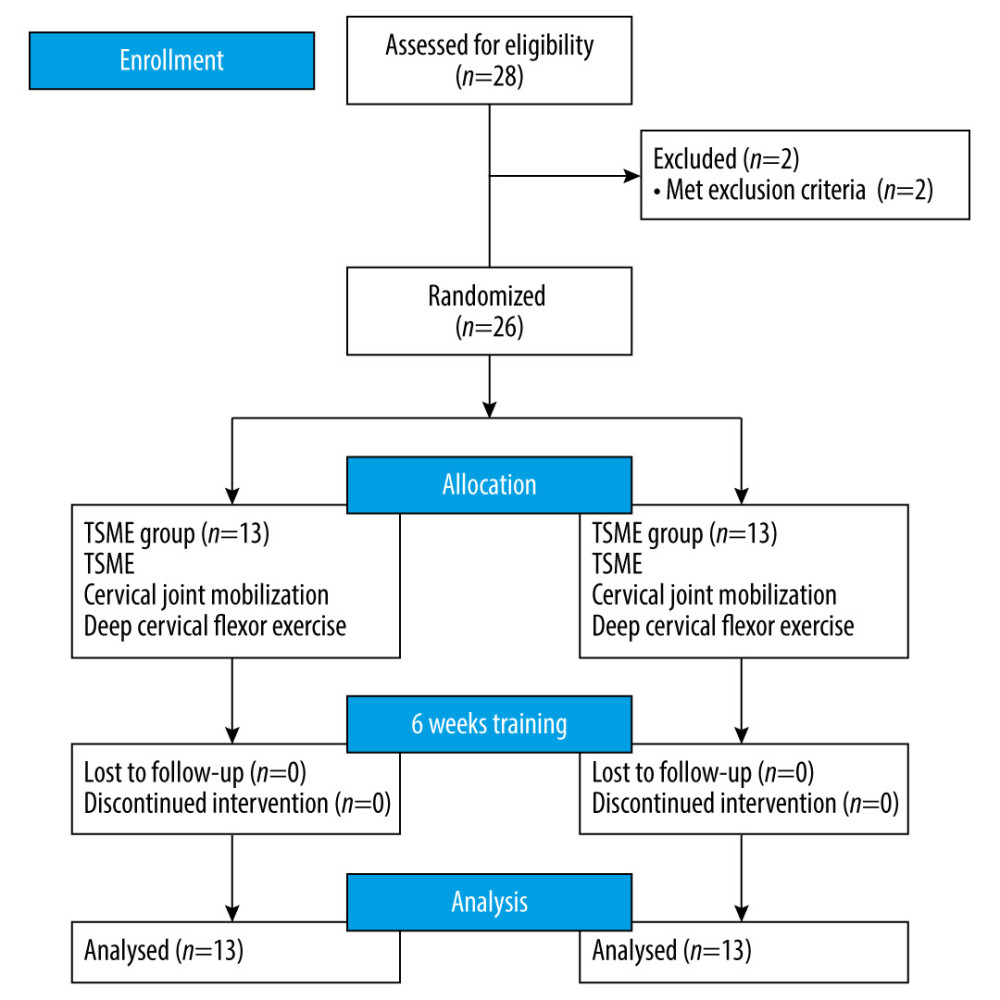 Figure 1. Research procedure.
Figure 1. Research procedure.  Figure 2. (A) Thoracic extension with foam roller. (B) Thoracic extension with chair. (C) Thoracic flexion in quadruped position. (D) Thoracic rotation in side lying. (E) Thoracic rotation in a kneeling position. (F) Thoracic lateral flexion in sitting position.
Figure 2. (A) Thoracic extension with foam roller. (B) Thoracic extension with chair. (C) Thoracic flexion in quadruped position. (D) Thoracic rotation in side lying. (E) Thoracic rotation in a kneeling position. (F) Thoracic lateral flexion in sitting position. References
1. Wang WT, Olson SL, Campbell AH, Effectiveness of physical therapy for patients with neck pain: an individualized approach using a clinical decision-making algorithm: Am J Phys Med Rehabil, 2003; 82(3); 203-18
2. Falla DL, Jull GA, Hodges PW, Patients with neck pain demonstrate reduced electromyographic activity of the deep cervical flexor muscles during performance of the craniocervical flexion test: Spine (Phila Pa 1976), 2004; 29(19); 2108-14
3. Hush JM, Maher CG, Refshauge KM, Risk factors for neck pain in office workers: A prospective study: BMC Musculoskelet Disord, 2006; 7; 81
4. Owen N, Healy GN, Matthews CE, Dunstan DW, Too much sitting: The population health science of sedentary behavior: Exerc Sport Sci Rev, 2010; 38(3); 105-13
5. Hoe VC, Urquhart DM, Kelsall HL, Ergonomic interventions for preventing work-related musculoskeletal disorders of the upper limb and neck among office workers: Cochrane Database Syst Rev, 2018; 10; CD008570
6. Paksaichol A, Janwantanakul P, Purepong N, Office workers’ risk factors for the development of non-specific neck pain: A systematic review of prospective cohort studies: Occup Environ Med, 2012; 69(9); 610-18
7. Szeto GP, Straker L, Raine S, A field comparison of neck and shoulder postures in symptomatic and asymptomatic office workers: Appl Ergon, 2002; 33(1); 75-84
8. Weon JH, Oh JS, Cynn HS, Influence of forward head posture on scapular upward rotators during isometric shoulder flexion: J Bodyw Mov Ther, 2010; 14(4); 367-74
9. Lau KT, Cheung KY, Chan KB, Relationships between sagittal postures of thoracic and cervical spine, presence of neck pain, neck pain severity and disability: Man Ther, 2010; 15(5); 457-62
10. Brindise JP, Nelson KE, Kappler RE, Association between cervical and thoracic somatic dysfunction among second-year osteopathic medical students: J Am Osteopath Assoc, 2014; 114(7); 540-48
11. Falla D, Gizzi L, Parsa H, People with chronic neck pain walk with a stiffer spine: J Orthop Sports Phys Ther, 2017; 47(4); 268-77
12. Ozer Kaya D, Toprak Celenay S, An investigation of sagittal thoracic spinal curvature and mobility in subjects with and without chronic neck pain: Cut-off points and pain relationship: Turk J Med Sci, 2017; 47(3); 891-96
13. Dunning JR, Cleland JA, Waldrop MA, Upper cervical and upper thoracic thrust manipulation versus nonthrust mobilization in patients with mechanical neck pain: A multicenter randomized clinical trial: J Orthop Sports Phys Ther, 2012; 42(1); 5-18
14. Galindez-Ibarbengoetxea X, Setuain I, Ramirez-Velez R, Short-term effects of manipulative treatment versus a therapeutic home exercise protocol for chronic cervical pain: A randomized clinical trial: J Back Musculoskelet Rehabil, 2018; 31(1); 133-45
15. Nakamaru K, Aizawa J, Kawarada K, Immediate effects of thoracic spine self-mobilization in patients with mechanical neck pain: A randomized controlled trial: J Bodyw Mov Ther, 2019; 23(2); 417-24
16. Miller J, Gross A, D’Sylva J, Manual therapy and exercise for neck pain: A systematic review: Man Ther, 2010 [Online ahead of print]
17. Harris GR, Susman JL, Managing musculoskeletal complaints with rehabilitation therapy: summary of the Philadelphia Panel evidence-based clinical practice guidelines on musculoskeletal rehabilitation interventions: J Fam Pract, 2002; 51(12); 1042-46
18. Gross A, Kay TM, Paquin JP, Exercises for mechanical neck disorders: Cochrane Database Syst Rev, 2015; 1; CD004250
19. Heneghan NR, Lokhaug SM, Tyros I, Clinical reasoning framework for thoracic spine exercise prescription in sport: A systematic review and narrative synthesis: BMJ Open Sport Exerc Med, 2020; 6(1); e000713
20. Cleland JA, Glynn P, Whitman JM, Short-term effects of thrust versus nonthrust mobilization/manipulation directed at the thoracic spine in patients with neck pain: A randomized clinical trial: Phys Ther, 2007; 87(4); 431-40
21. Edmond SL, Joint mobilization/manipulation-e-book: Extremity and spinal techniques: Elsevier Health Sciences, 2016
22. Chiu TT, Lam TH, Hedley AJ, A randomized controlled trial on the efficacy of exercise for patients with chronic neck pain: Spine (Phila Pa 1976), 2005; 30(1); E1-7
23. Chung S, Jeong YG, Effects of the craniocervical flexion and isometric neck exercise compared in patients with chronic neck pain: A randomized controlled trial: Physiother Theory Pract, 2018; 34(12); 916-25
24. Hjermstad MJ, Fayers PM, Haugen DF, Studies comparing Numerical Rating Scales, Verbal Rating Scales, and Visual Analogue Scales for assessment of pain intensity in adults: A systematic literature review: J Pain Symptom Manage, 2011; 41(6); 1073-93
25. Cross KM, Kuenze C, Grindstaff TL, Hertel J, Thoracic spine thrust manipulation improves pain, range of motion, and self-reported function in patients with mechanical neck pain: A systematic review: J Orthop Sports Phys Ther, 2011; 41(9); 633-42
26. Heggannavar A, Battula L, Immediate effect of thoracic distraction thrust versus upper thoracic crossed hand manipulation in mechanical neck pain: A randomized clinical trial: Physiotherapy – The Journal of Indian Association of Physiotherapists, 2021; 15(1); 22
27. Gonzalez-Iglesias J, Fernandez-de-las-Penas C, Cleland JA, Inclusion of thoracic spine thrust manipulation into an electro-therapy/thermal program for the management of patients with acute mechanical neck pain: A randomized clinical trial: Man Ther, 2009; 14(3); 306-13
28. Lau HM, Wing Chiu TT, Lam TH, The effectiveness of thoracic manipulation on patients with chronic mechanical neck pain – a randomized controlled trial: Man Ther, 2011; 16(2); 141-47
29. Park GW, An J, Kim SW, Lee BH, Effects of sling-based thoracic active exercise on pain and function and quality of life in female patients with neck pain: A randomized controlled trial: Healthcare (Basel), 2021; 9(11); 1514
30. Gross A, Miller J, D’Sylva J, Manipulation or mobilisation for neck pain: A Cochrane review: Man Ther, 2010; 15(4); 315-33
31. Yang J, Lee B, Kim C, Changes in proprioception and pain in patients with neck pain after upper thoracic manipulation: J Phys Ther Sci, 2015; 27(3); 795-98
32. Hartrick CT, Kovan JP, Shapiro S, The numeric rating scale for clinical pain measurement: A ratio measure?: Pain Pract, 2003; 3(4); 310-16
33. Perveen S, Mahmood T, Haider R, Ayub A, Effects of low amplitude high velocity thurst manipulation as compare to grade III maitland mobilization of thoracic spine on mechanical neck pain and disability: Journal of Liaquat University of Medical & Health Sciences, 2020; 19(04); 252-56
Figures
Tables
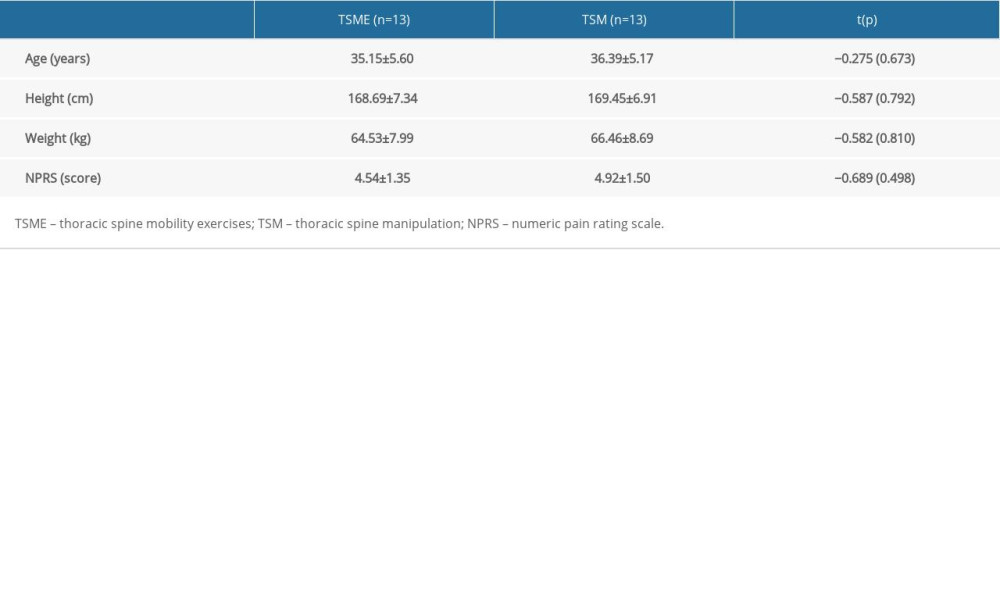 Table 1. General characteristics of study subjects.
Table 1. General characteristics of study subjects.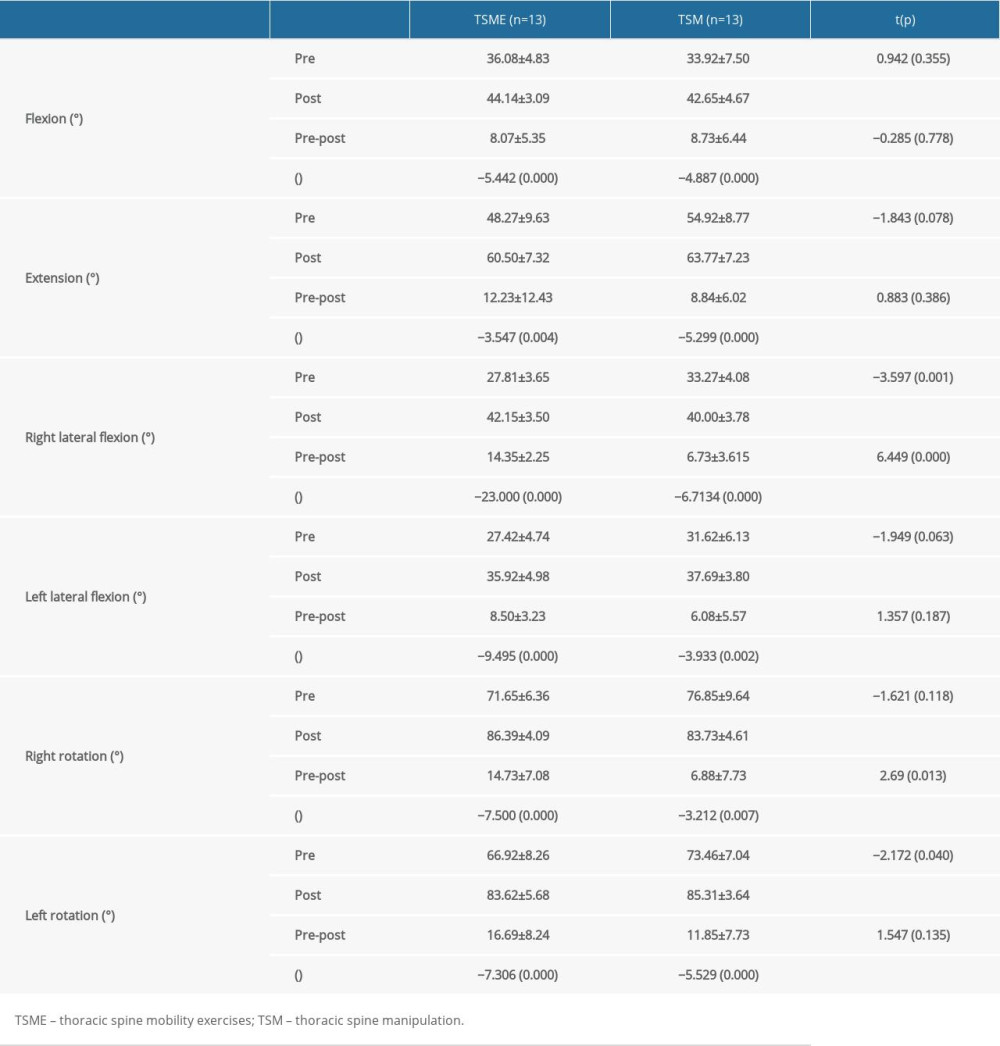 Table 2. Comparison of cervical ROM within groups and between groups.
Table 2. Comparison of cervical ROM within groups and between groups.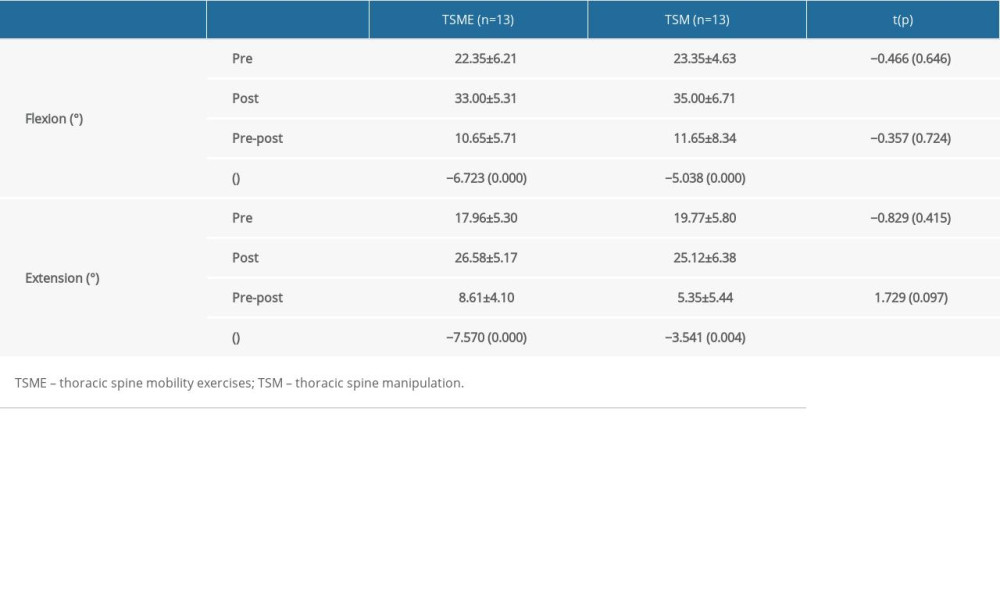 Table 3. Comparison of thoracic ROM within groups and between groups.
Table 3. Comparison of thoracic ROM within groups and between groups.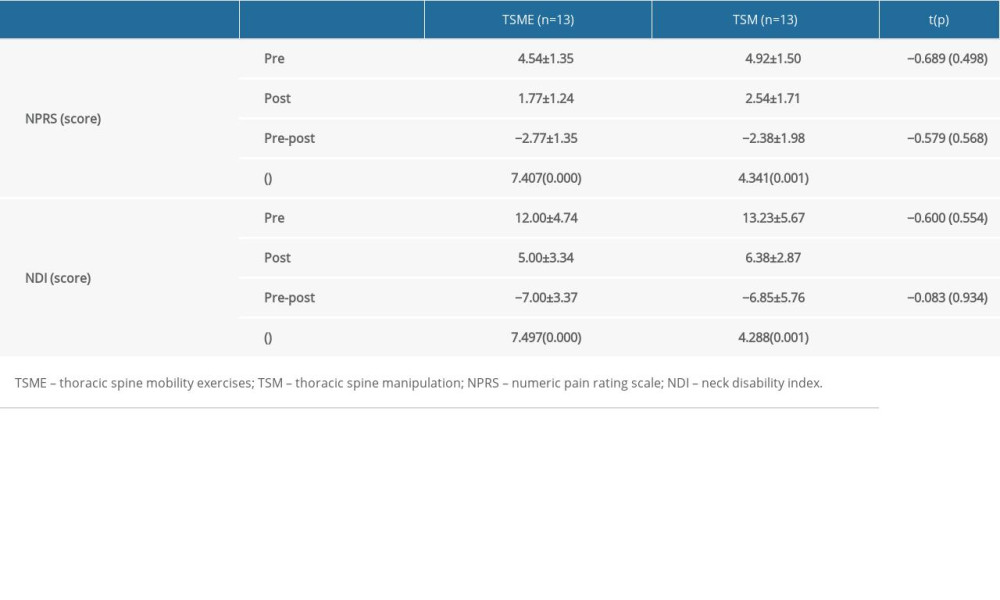 Table 4. Comparison of pain and disability within groups and between groups.
Table 4. Comparison of pain and disability within groups and between groups. Table 1. General characteristics of study subjects.
Table 1. General characteristics of study subjects. Table 2. Comparison of cervical ROM within groups and between groups.
Table 2. Comparison of cervical ROM within groups and between groups. Table 3. Comparison of thoracic ROM within groups and between groups.
Table 3. Comparison of thoracic ROM within groups and between groups. Table 4. Comparison of pain and disability within groups and between groups.
Table 4. Comparison of pain and disability within groups and between groups. In Press
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
06 Mar 2024 : Clinical Research
Prevalence and Variation of Medical Comorbidities in Oral Surgery Patients: A Retrospective Study at Jazan ...Med Sci Monit In Press; DOI: 10.12659/MSM.943884
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








