09 December 2022: Clinical Research
Neuropsychological Features in Patients with General Paresis of the Insane at an Early Stage
Jun-Hua Gao12345ABE, Du-Yu Ding5BC, Yan-Yun Qi5AB, Yu-Ming Huang5AE, Jing-Lin Zhang5ADF, Wei Zhang1234ACEG*DOI: 10.12659/MSM.938316
Med Sci Monit 2022; 28:e938316
Abstract
BACKGROUND: This study aimed to explore the features of cognitive impairment in patients with neurosyphilis at the early stage of mild cognitive impairment (MCI).
MATERIAL AND METHODS: A total of 18 patients with asymptomatic neurosyphilis (ANS), 19 patients with neurosyphilis at the MCI stage (neurosyphilis-MCI), and 15 patients with neurosyphilis at the dementia stage (neurosyphilis-dementia) were enrolled. Cognitive function was evaluated using comprehensive rating scales. Tests of syphilis in blood and cerebrospinal fluid (CSF) were conducted, and white blood cell (WBC) counts and protein levels in CSF were measured.
RESULTS: Overall cognitive function and individual cognitive domains, including memory, language, visuospatial skill, and attention/executive function, were all significantly impaired in the neurosyphilis-MCI group compared with the ANS group, and were further impaired in the neurosyphilis-dementia group. Although there was no difference in serum rapid plasma regain (RPR) titer among the 3 groups, the number of patients with serum RPR titer ≥1: 32 in the neurosyphilis-MCI group was much higher than that in the ANS group. CSF RPR positive rate in the neurosyphilis-MCI group was significantly higher than that in the ANS group. The WBC count, protein level, and the rate of elevated protein level or increased WBC count in CSF did not differ among the 3 groups.
CONCLUSIONS: The feature of cognitive impairment of neurosyphilis-MCI patients displayed multiple-domain amnestic MCI. Perhaps there were extensive brain areas involved at the early stage, and a continuous neuroinflammatory process was through the different stages of neurosyphilis. Early diagnosis and treatment are very important for preventing the progression of general paresis of the insane.
Keywords: Neuropsychological Tests, Neurosyphilis, Humans, Dementia
Background
Neurosyphilis results from the invasion of
GPI occurs within 10 to 20 years after syphilis infection, and patients present cognitive decline and neuropsychiatric symptoms. Previous studies showed that patients with GPI accounted for about 38.9% to 49.0% of total neurosyphilis cases [1–4]. A retrospective study focusing on 187 patients with rapid progressive dementia showed that the most common causes were infectious diseases, among which neurosyphilis was second in frequency [5]. However, clinicians, including neurologists and psychiatrists, are rarely aware of this. Thus, the misdiagnosis rate of GPI is very high, ranging from 36.1% to 84.6% [6–8]. GPI is largely reversible if early diagnosis and standard treatment are given. Therefore, it is possible for patients to go back to work and life [9].
Until now, most studies focused on the neuropsychiatric symptoms and neurological signs of GPI [7,10,11]. However, one study investigating cognition indicated that multiple cognitive domains were impaired in 8 patients with mild GPI, with Mini-Mental State Examination (MMSE) score of 19 to 25 points [12]. A case report showed that a GPI patient with an MMSE score of 21 points had impaired executive function and attention [13]. However, there have been no studies on the cognitive features in patients with neurosyphilis tested by using a comprehensive rating scale at the different stages of disease, including asymptomatic, mild cognitive impairment (MCI), and dementia stages.
According to the number of impaired cognitive domains and whether memory is compromised, MCI is divided into 4 types: single-domain amnestic MCI, multiple-domain amnestic MCI, single-domain non-amnestic MCI, and multiple-domain non-amnestic MCI. Different classifications can be due to different etiologies. For example, until now, possible causes of single-domain amnestic MCI included Alzheimer’s disease (AD) and depression, and possible causes of multiple-domain non-amnestic MCI included frontotemporal degeneration and vascular cognitive impairment. The features of cognitive impairment in patients with neurosyphilis at the stage of MCI have not been investigated, and the pattern of cognitive impairment has not been confirmed yet.
Atrophy of the anterior brain, including the frontal and temporal lobes, is a common neuroimaging finding in patients with GPI [9]. Severe medial temporal lobe atrophy was found to be a predictor of poor cognitive outcome [14]. A report on the postmortem histopathologic analysis of a GPI patient with an MMSE score of 25 points and Montreal Cognitive Assessment score of 22 points showed that the frontal lobe was severely damaged but the temporal lobe was relatively preserved [15]. It was suspected that the atrophy of the medial temporal lobe was secondary to the dysfunction of the other cerebral areas due to its connections with most of these brain areas [16]. Accordingly, we assumed that impairments of cognitive domains, such as executive function, and neuropsychiatric symptoms associated with the frontal lobe might occur, but other cognitive domains might not be compromised at the MCI stage.
In this study, we investigated for the first time the patterns and features of cognitive impairment in patients with neurosyphilis at the early stage of MCI with a set of rating scales. The data from this study may help clinicians make an early diagnosis, reduce the misdiagnosis rate, and understand the pathogenesis and predict the progression of GPI.
Material and Methods
ETHICS STATEMENT:
This study was conducted in accordance with the principles of the Helsinki Declaration. The protocol was approved by the Ethics Review Board of Beijing Ditan Hospital, Capital Medical University in Beijing China (approval no.: Jingdi Lunke Zi [2020] no. [044]-01. All enrolled patients and their family members signed the informed consent.
PATIENTS:
A total of 34 patients with neurosyphilis who were hospitalized in the Department of Neurology, Beijing Ditan Hospital and Beijing Tiantan Hospital of Capital Medical University from January 2020 to July 2021 were enrolled in the study. There were 19 patients in the neurosyphilis-MCI group and 15 patients in the neurosyphilis-dementia group. The control group consisted of 18 patients with ANS hospitalized during the same period.
INCLUSION AND EXCLUSION CRITERIA:
The criteria for the diagnosis of neurosyphilis were as previously described. Syphilis at any stage met 1 of 2 conditions: (1) a positive rapid plasma regain (RPR) titer in the cerebrospinal fluid (CSF); (2) positive T. pallidum particle agglutination or fluorescent treponemal antibody absorption (FTA-ABS) in the CSF, with increased WBC count (>5/μL) or elevated protein level (>45 mg/dL) in the CSF, with no other known causes which could induce these abnormalities [17]. The ANS group met the criteria of neurosyphilis, with no central nervous system (CNS) signs or symptoms. The neurosyphilis-MCI and neurosyphilis-dementia groups met the diagnostic criteria from our previous study [17]. MCI was diagnosed based on the report of the International Working Group on Mild Cognitive Impairment: (1) cognitive impairment reported by patients or informant; (2) objective evidence of cognitive impairment; (3) retention of functional mobility; and (4) failure to meet the criteria for dementia [18]. The dementia group met the criteria of the Diagnostic and Statistical Manual of Mental Disorder, 4th edition (DSM-IV): (1) normal intelligence in the past, and acquired cognitive decline (impairment of memory, execution, language, visuospatial ability) or abnormal mental behavior; (2) daily work ability or daily life was affected; and (3) other mental diseases were excluded.
The exclusion criteria were as follows: (1) treatment with antibiotics within the last 6 months; (2) positive for HIV; and (3) presence of other diseases that might affect cognition, such as AD and cerebral vascular diseases.
DEMOGRAPHIC VARIABLES OF ANS, NEUROSYPHILIS-MCI, AND NEUROSYPHILIS-DEMENTIA GROUPS:
All patients in the ANS group had syphilis detected during preoperative examination or pregnancy, and all patients in the neurosyphilis-MCI and neurosyphilis-dementia groups had syphilis detected after the occurrence of cognitive impairment or neuropsychiatric symptoms. Demographic variables, including age, sex, education level, and time from the symptom onset to diagnosis, were recorded for all patients in the ANS, neurosyphilis-MCI, and neurosyphilis-dementia groups.
ASSESSMENTS OF COGNITIVE FUNCTION:
Cognitive function of each patient, including overall cognitive function and individual cognitive domains, were assessed by a series of neuropsychological rating scales by a trained rater who did not know the diagnosis of the patients. All the rating scales had good validity.
OVERALL COGNITIVE FUNCTION:
The overall cognitive function was assessed by the MMSE scale [19]. There are 30 items in the MMSE scale, including orientation, memory, attention, calculation, language, and visuospatial ability. The lower the score of the MMSE scale, the worse the overall cognitive function.
The Montreal Cognitive Assessment scale was another scale used to assess the overall cognitive function [20]. The Beijing version of this scale covered 8 cognitive domains, including visuospatial/executive function, naming, memory, attention, language, abstraction, delayed recall, and orientation. If the patient’s education level was ≤12 years, 1 point was added to the total score. A lower score of the Montreal Cognitive Assessment scale indicated worse overall cognitive function.
MEMORY: The auditory verbal learning test (AVLT) [21] included 12 words. After reciting all the words once, patients were instructed to recall them immediately, and the number of words recalled were recorded. The same procedure was repeated 3 times, which was defined as immediate recall. After learning the words 3 times, patients were told to remember these words. After 5 min and 20 min, patients were instructed to recall the words and the numbers of correct recalls were recorded, which were defined as short-delayed recall and long-delayed recall, respectively. Finally, the patients were instructed to recall words by memory [12].
The Rey-Osterrich complex figure test (RCFT) and delayed-RCFT are commonly used to assess visuospatial ability and visual memory [22]. Patients were told to copy a picture, with the time limited to 5 min. Patients were then required to draw this picture by recall after 25 min. There was no time limit for the delayed drawing. The picture was divided into 18 units, and the total score was 36 points. Each unit was scored 2 points when the shape and position were correct, 1 point was scored when the shape was correct and position was incorrect, 0.5 points was scored when the element was deformed, incomplete, and incorrectly positioned, and 0 points were scored when the element was missing or unrecognizable. Regarding the scoring of the RCFT, 1 point was also scored when the shape was distorted but placed correctly, as per scoring instructions.
LANGUAGE: The Chinese version of 30-item Boston naming test was used to evaluate language function. Patients were instructed to name 30 items from item 1, and if named correctly, the examiners would proceed to item 2, and so on. If the patients made self-corrections, credits were given [23].
The verbal fluency test was another scale used to test language. Patients were instructed to name as many animals, furniture, and animal with furniture alternation as possible in 1 min. The numbers of unique response were recorded [24].
VISUOSPATIAL ABILITY: The RCFT was used to assess visuospatial ability, as described above [22].
ATTENTION AND EXECUTIVE FUNCTION:
The symbol digit modality test [25] was used to assess attention and executive function. Patients were asked to match the symbols to digits in the 90s, according to an illustration of pairing symbol-digital. Every correctly filled symbol was counted as 1 point, and the inversion of a symbol was counted as 0.5 points. The first 10 samples were not counted, and the total score was 90 points.
The trail making test A (TMT-A) [25] was also used for evaluating attention and executive function. Patients were asked to connect the numbers from 1 to 25 in a proper sequence. The time taken was recoded. The trail making test B (TMT-B) was evaluated as follows: the numbers from 1 to 25 were all surrounded by a square and a circle, patients were asked to connect the digits in a proper sequence but alternating between squares and circles.
The Stroop color-word test (SCWT)-Chinese version [25] was performed as follows: patients were asked to read the words, colors, or color-words on the test board one by one at the fastest speed. The correct numbers and the total time were recorded.
COLLECTION OF CSF AND BLOOD SAMPLES:
Before penicillin therapy was administered, each patient underwent lumbar puncture and had CSF collected; a blood sample was collected immediately after lumbar puncture. Tests for RPR (Shanghai Rongsheng Biological Pharmaceutical Co., Ltd, China) and
STATISTICAL ANALYSIS:
Data were analyzed using IBM SPSS version 25.5. Continuous variables were presented as mean±standard deviations (with normal distribution) and interquartile range (with abnormal distribution). Categorical variables were described by numbers and percentages. Multiple groups were compared using the Kruskal-Wallis H test, and 2 groups were compared using the 2-sample
Results
DEMOGRAPHIC VARIABLES:
The demographic variables of the ANS, neurosyphilis-MCI, and neurosyphilis-dementia groups are shown in Table 1.
We found that patients in the ANS group were significantly younger than those in the neurosyphilis-MCI group (
COGNITIVE FUNCTION:
The overall cognitive function and individual cognitive domains were evaluated by a series of rating scales (Table 2).
There were significant differences in all the scales except for TMT-A time, TMT-A accuracy, TMT-B accuracy, SCWT-A time, SCWT-A accuracy, SCWT-B time, SCWT-B accuracy, and SCWT-C time between the ANS and neurosyphilis-MCI groups. There were significant differences except for AVLT4R, AVLT5R, AVLT6R, RCFT delay recall, Boston naming test, RCFT-figure copying, symbol digit modality test, SCWT-A accuracy, and SCWT-C accuracy between the neurosyphilis-MCI and neurosyphilis-dementia groups.
In summary, overall cognitive function and individual cognitive domains, including memory, language, visuospatial skill, and attention/executive function, were all significantly impaired in the neurosyphilis-MCI group compared with the ANS group, and further impairments were found in the neurosyphilis-dementia group (Table 2).
LABORATORY RESULTS:
Although there was no significant difference in the serum RPR titer among the 3 groups, more patients in the neurosyphilis-MCI group had serum RPR ≥1: 32 than in the ANS group (P<0.01). The CSF RPR positive rate in the neurosyphilis-MCI group was significantly higher than that in the ANS group (P=0.02), and the number of patients with a CSF RPR titer ≥1: 8 in the neurosyphilis-MCI group was significantly higher than that in the ANS group (P<0.01), and lower than that in the neurosyphilis-dementia group (P<0.01). There were no significant differences in protein level, WBC count, rate of abnormal protein level, or WBC count in the CSF among the 3 groups (Table 3).
Discussion
It was reported that GPI was more prevalent in male patients [8,28], which was similar to the findings in our study. However, in the present study, there were more female patients in the ANS group. In the era of penicillin, the primary-stage manifestations of syphilis, such as eruption, are no longer typical, so it is difficult to detect syphilis at the early stage. However, female patients have more opportunities, such as pregnancy or abortion, to be screened for syphilis-related variables, and early treatment can prevent the development of GPI. The average time from symptom onset to confirmed GPI diagnosis was found to be 10.87 months [29]. Further analysis in the present study indicated that this duration in the neurosyphilis-MCI group was much shorter than that in the neurosyphilis-dementia group. Hence, the different duration between the neurosyphilis-MCI and neurosyphilis-dementia groups revealed the potential time window of intervention, implying that early diagnosis and timely treatment might prevent disease progression from MCI to dementia. It is urgently recommended that all members of society should increase their knowledge of syphilis, establish a healthy lifestyle, and achieve early detection and standardized treatment of syphilis.
This is the first study exploring the cognitive features of neurosyphilis at the MCI stage by using a set of rating scales. We found that the overall cognitive function was declined in the neurosyphilis-MCI group, which was similar to the results of the neurosyphilis-dementia groups. Of note, compared with the ANS groups, the neurosyphilis-MCI group presented significantly compromised multiple cognitive domains, including memory, language, visuospatial ability, attention and executive function, displaying the multiple-domain amnestic type of MCI.
Memory impairment is easy to recognize by patients and their families due to its severe influence on patients’ daily lives. Our study supported that short-term and long-term memories were all significantly impaired in patients with GPI, as in patients with AD [12]. Golby et al verified that the right hippocampus is involved in visual memory [30]. Hippocampal body volume is associated with delayed verbal memory in healthy individuals [31] and in patients with mild AD [32]. Therefore, it was speculated that memory-related brain regions, for example, the hippocampus, might be firstly damaged, whereas the temporal cortex was relatively preserved, according to the previously reported pathological findings in patients with GPI [15]. The Papez circuit, including the vault and entorhinal cortex, is an important brain structure that is closely related to memory. Any damage in the Papez circuit can lead to memory impairment. It was previously shown that the structure of the caudate nucleus and thalamus were related to the recognition score of the AVLT [33]. It was suggested that there was a significant correlation between the delayed recall score and metabolism in the posterior cingulate gyrus of both hemispheres and in the left precuneus in patients with mild AD [34]. Thus, the brain regions involved in memory are very complex and may be involved in the memory impairment in patients with neurosyphilis-MCI.
Visuospatial disability is a cognitive impairment of the properties of objects in space. It is commonly ignored by patients in daily life. The RCFT was used to evaluate visuospatial ability [35]. It was reported that the parietal lobe is closely related to visuospatial ability in healthy people and that of the right hemisphere is lateralized [36]. In the present study, it was surprising to find that visuospatial ability was impaired in the neurosyphilis-MCI group, because varying degrees of atrophy were found in the anterior parts of the brain but seldomly in the parietal and occipital lobes by magnetic resonance imaging (MRI) in patients with GPI [8]. In a functional MRI (fMRI) study of patients with MCI, reductions in the activation of the neural network, such as the bilateral visual association cortex, temporo-occipital junction area, left prefrontal lobe, and cingulate gyrus, in addition to the reduction of the parietal lobe, were found in patients with impaired visuospatial ability. The left para-hippocampal gyrus is vital in visuospatial ability [37]. One study showed that patients with neurosyphilis-MCI had different degrees of atrophy of the frontotemporal lobe [6]. Thus, it is not difficult to notice that the patients in the present study, including those with neurosyphilis-MCI, had impaired visuospatial ability.
Language disturbance usually occurs when the damage is located in the dominant hemisphere. However, the hemisphere that is prone to be affected in patients with neurosyphilis-MCI has not been reported. It is known that temporal neocortical [38] and hippocampus [39] volumes were all correlated with the scores of language tests, such as the Boston naming test. Moreover, with the development of new imaging technologies, such as fMRI, brain networks and specific brain regions were found to be related to language function [40]. Therefore, although the autopsy pathological results showed no temporal lobe atrophy, we believe that there might be damage to the brain network relating to language in patients with GPI, including patients with neurosyphilis-MCI.
Impairment of executive function and attention can lead to decreased learning ability and working memory, which are related to the disruption of the integrity of the frontal-striatal circuit. Frontal lobe atrophy is a common neuroimaging change found in brain MRI. In this investigation, executive function and attention were significantly impaired, indicating that the frontal lobe might have been involved. Meanwhile, it was reported that frontal-parietal areas, including the right precuneus, right angular gyrus, left paracentral lobule, and right dorsolateral prefrontal cortex, are the underlying brains areas involved in executive function [41]. In addition to the above areas, white matter hyperintensities were also found to be associated with attention impairment [14]. Therefore, correlation analysis between cognitive evaluation and MRI of the brain would be helpful to further understand the impaired cognitive domains and corresponding lesions in the brain.
In summary, according to the consensus of the International Working Group on MCI, patients with neurosyphilis-MCI present with multi-domain amnestic MCI, which is perhaps related to the widespread brain involvement at the MCI stage of neurosyphilis. Thus, neurosyphilis may be an important etiology of multi-domain amnestic MCI, and widespread involvement of brain regions may account for the protean manifestations.
The differential diagnosis of bilateral temporal lobe lesions includes infectious diseases, such as herpes encephalitis, human herpes virus 6 encephalopathy, fungal infection, and syphilis [42]. A pathological study showed that the olfactory bulbs were involved in patients with GPI [15]. The olfactory organ might be the pathway to the pathogenesis of GPI. It is possible that the frontotemporal lobe is easily affected. It was verified that
RPR, as a nontreponemal test, is 100% sensitive for early neurosyphilis. It was reported that a serum RPR titer ≥1: 32 was predictive of neurosyphilis [45]. However, RPR was only 50% to 75% sensitive for late symptomatic neurosyphilis, with a specificity of 90% [46], and even was negative in late-stage neurosyphilis. In our study, there were no differences in the serum RPR titers among the 3 groups. However, there were many more patients with a serum RPR titer ≥1: 32 in the neurosyphilis-MCI group than in the ANS group, just as in a previous study showing that a higher current serum RPR titer was the independent risk predictor for symptomatic neurosyphilis, including GPI [3]. The CSF RPR is a sensitive index for the diagnosis of neurosyphilis. Similar to the results of a previous study, in which CSF RPR was an independent risk predictor for symptomatic neurosyphilis [3], in the present study, CSF RPR positive rate in the neurosyphilis-MCI group was much higher than that in the ANS group. The CSF WBC count reflected the activity of neurosyphilis and was prone to decrease following therapy [47]. Meanwhile, approximately 10% of patients with GPI were shown to have a WBC count less than 5 cells/mL [47]. In the present study, there were no differences in the WBC count and the rate of increased WBC count in the CSF among the 3 groups, suggesting a continuous neuroinflammatory process through all stages of neurosyphilis. There was also no difference in the protein level and the rate of elevated protein level in the CSF among the 3 groups. Whereas in another study, CSF protein level was an independent risk factor for symptomatic neurosyphilis [3], which might be due to patients with different types of neurosyphilis being enrolled in that study.
This study has the following limitations. First, the sample size was relatively small, and more patients with GPI will be enrolled in the future. Second, this study lacked the investigation of neuroimaging changes and their correlations with cognitive impairment because some patients could not cooperate with neuroimaging scanning owing to their neuropsychiatric symptoms.
Conclusions
This study is the first one to investigate the cognitive features of neurosyphilis at the MCI stage by using a series of rating scales. The pattern of cognitive impairment in the neurosyphilis-MCI stage is multiple-domain amnestic MCI, and cognitive function is further deteriorated with disease progression at the dementia stage. The results imply extensive brain areas are involved in the MCI stage of neurosyphilis. CSF results suggest a continuous inflammatory process through the different stages of neurosyphilis. Accordingly, early diagnosis and treatment are very important for preventing the progression of neurosyphilis from the stage of MCI to dementia.
Tables
Table 1. Demographic variables and clinical signs of the asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.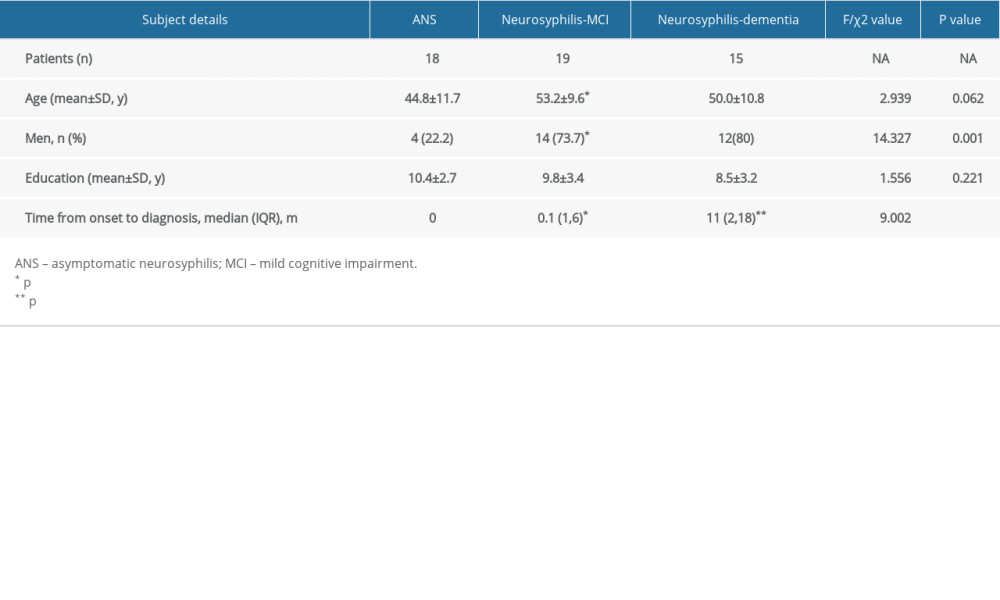 Table 2. Neuropsychological assessments of asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.
Table 2. Neuropsychological assessments of asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.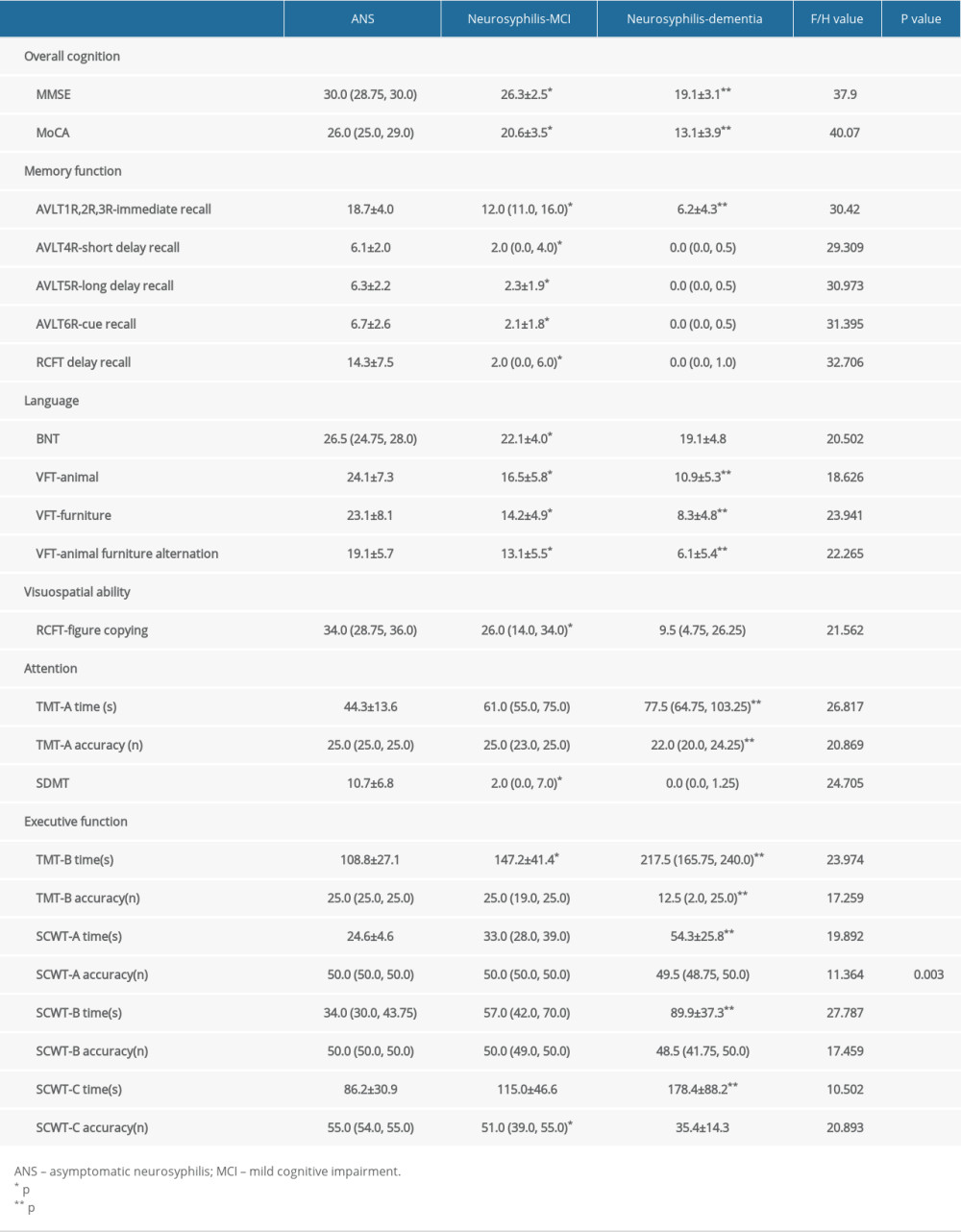 Table 3. Laboratory results in serum and cerebrospinal fluid from asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.
Table 3. Laboratory results in serum and cerebrospinal fluid from asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.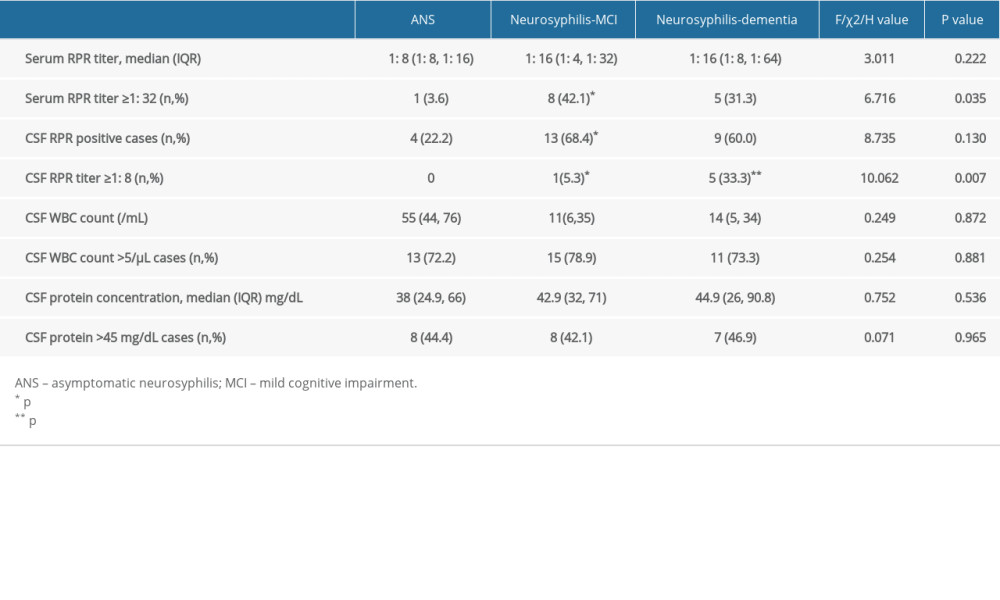
References
1. Conde-Sendín MA, Amela-Peris R, Aladro-Benito Y, Current clinical spectrum of neurosyphilis in immunocompetent patients: Eur Neurol, 2004; 52(1); 29-35
2. Drago F, Merlo G, Ciccarese G, Changes in neurosyphilis presentation: A survey on 286 patients: J Eur Acad Dermatol Venereol, 2016; 30(11); 1886-900
3. Li W, Jiang M, Xu D, Clinical and laboratory characteristics of symptomatic and asymptomatic neurosyphilis in HIV-negative patients: A retrospective study of 264 cases: Biomed Res Int, 2019; 2019; 2426313
4. Zhang HL, Lin LR, Liu GL, Clinical spectrum of neurosyphilis among HIV-negative patients in the modern era: Dermatology, 2013; 226(2); 148-56
5. Anuja P, Venugopalan V, Darakhshan N, Rapidly progressive dementia: An eight year (2008–2016) retrospective study: PLoS One, 2018; 13(1); e0189832
6. Chen YY, Zhang YF, Qiu XH, Clinical and laboratory characteristics in patients suffering from general paresis in the modern era: J Neurol Sci, 2015; 350(1–2); 79-83
7. Kararizou E, Mitsonis C, Dimopoulos N, Psychosis or simply a new manifestation of neurosyphilis: J Int Med Res, 2006; 34(3); 335-37
8. Zheng D, Zhou D, Zhao Z, The clinical presentation and imaging manifestation of psychosis and dementia in general paresis: A retrospective study of 116 cases: J Neuropsychiatry Clin Neurosci, 2011; 23(3); 300-7
9. Kodama K, Okada S, Komatsu N, Relationship between MRI findings and prognosis for patients with general paresis: J Neuropsychiatry Clin Neurosci, 2000; 12(2); 246-50
10. Friedrich F, Aigner M, Fearns N, Psychosis in neurosyphilis – clinical aspects and implications: Psychopathology, 2014; 47(1); 3-9
11. Friedrich F, Geusau A, Greisenegger S, Manifest psychosis in neurosyphilis: Gen Hosp Psychiatry, 2009; 31(4); 379-81
12. Wang J, Guo Q, Zhou P, Cognitive impairment in mild general paresis of the insane: AD-like pattern: Dement Geriatr Cogn Disord, 2011; 31(4); 284-90
13. Thiebaud PC, Banini O, Lambolez T, Neurosyphilis is a treatable cause of dementia not systematically searched for, but still worth to be considered: Rev Neurol (Paris), 2012; 168(2); 195-96
14. Chen B, Shi H, Hou L, Medial temporal lobe atrophy as a predictor of poor cognitive outcomes in general paresis: Early Interv Psychiatry, 2019; 13(1); 30-38
15. Mao C, Gao J, Jin L, Postmortem histopathologic analysis of neurosyphilis: A report of 3 cases with clinicopathologic correlations: J Neuropathol Exp Neurol, 2018 [Online ahead of print]
16. Mehrabian S, Raycheva M, Traykova M, Neurosyphilis with dementia and bilateral hippocampal atrophy on brain magnetic resonance imaging: BMC Neurol, 2012; 12; 96
17. Gao JH, Li WR, Xu DM, Clinical manifestations, fluid changes and neuroimaging alterations in patients with general paresis of the insane: Neuropsychiatr Dis Treat, 2021; 17; 69-78
18. Winblad B, Palmer K, Kivipelto M, Mild cognitive impairment – beyond controversies, towards a consensus: Report of the International Working Group on Mild Cognitive Impairment: J Intern Med, 2004; 256(3); 240-46
19. Cockrell JR, Folstein MF, Mini-Mental State Examination (MMSE): Psychopharmacol Bull, 1988; 24(4); 689-92
20. Yu J, Li J, Huang X, The Beijing version of the Montreal Cognitive Assessment as a brief screening tool for mild cognitive impairment: A community-based study: BMC Psychiatry, 2012; 12; 156-62
21. Guo Q, Zhao Q, Chen M, A comparison study of mild cognitive impairment with 3 memory tests among Chinese individuals: Alzheimer Dis Assoc Disord, 2009; 23(3); 253-59
22. Siri S, Benaglio I, Frigerio A, A brief neuropsychological assessment for the differential diagnosis between frontotemporal dementia and Alzheimer’s disease: Eur J Neurol, 2001; 8(2); 125-32
23. Cheung RW, Cheung MC, Chan AS, Confrontation naming in Chinese patients with left, right or bilateral brain damage: J Int Neuropsychol Soc, 2004; 10(1); 46-53
24. Guo QH, Cao XY, Zhou Y, Application study of quick cognitive screening test in identifying mild cognitive impairment: Neurosci Bull, 2010; 26(1); 47-54
25. Shi C, Kang L, Yao S, Co-norming and standardization in China: Schizophr Res, 2015; 169(1–3); 109-15
26. Collart P, Franceschini P, Durel P, Experimental rabbit syphilis: Br J Vener Dis, 1971; 47(6); 389-400
27. Lukehart RELA, Biological basis for syphilis: Clin Microbiol Rev, 2006; 19(1); 29-49
28. Yanhua W, Haishan S, Le H, Clinical and neuropsychological characteristics of general paresis misdiagnosed as primary psychiatric disease: BMC Psychiatry, 2016; 16; 230-36
29. Wang X, Yang Y, Wang X, MRI findings and early diagnosis of general paresis of the insane: Neurol Res, 2014; 36(2); 137-42
30. Golby AJ, Poldrack RA, Brewer JB, Material-specific lateralization in the medial temporal lobe and prefrontal cortex during memory encoding: Brain, 2001; 124(Pt 9); 1841-54
31. Chen KH, Chuah LY, Sim SK, Hippocampal region-specific contributions to memory performance in normal elderly: Brain Cogn, 2010; 72(3); 400-7
32. Wolk DA, Dickerson BCAlzheimer’s Disease Neuroimaging Initiative, Fractionating verbal episodic memory in Alzheimer’s disease: Neuroimage, 2011; 54(2); 1530-39
33. Balthazar ML, Yasuda CL, Cendes F, Learning, retrieval, and recognition are compromised in aMCI and mild AD: Are distinct episodic memory processes mediated by the same anatomical structures: J Int Neuropsychol Soc, 2010; 16(1); 205-9
34. Brugnolo A, Morbelli S, Arnaldi D, Metabolic correlates of Rey auditory verbal learning test in elderly subjects with memory complaints: J Alzheimers Dis, 2014; 39(1); 103-13
35. Shin MS, Park SY, Park SR, Clinical and empirical applications of the Rey-Osterrieth Complex Figure Test: Nat Protoc, 2006; 1(2); 892-99
36. Bai J, Wang YH, Weng XC, Visuospatial dysfunction in mild cognitive impairment: A functional magnetic resonance imaging study: Chin J Neurosci, 2003(5); 277-81
37. Glass L, Krueger F, Solomon J, Mental paper folding performance following penetrating traumatic brain injury in combat veterans: A lesion mapping study: Cereb Cortex, 2013; 23(7); 1663-72
38. Wilson RS, Sullivan M, Detoledo-Morrell L, Association of memory and cognition in Alzheimer’s disease with volumetric estimates of temporal lobe structures: Neuropsychology, 1996; 10(4); 459-63
39. Davies KG, Bell BD, Bush AJ, Naming decline after left anterior temporal lobectomy correlates with pathological status of resected hippocampus: Epilepsia, 1998; 39(4); 407-19
40. Ardila A, Bernal B, Rosselli M, How localized are language brain areas? A review of Brodmann areas involvement in oral language: Arch Clin Neuropsychol, 2016; 31(1); 112-22
41. Wang P, Zhu XT, Qi Z, Neural basis of enhanced executive function in older video game players: An fMRI study: Front Aging Neurosci, 2017; 9; 382-88
42. Eran A, Hodes A, Izbudak I, Bilateral temporal lobe disease: Looking beyond herpes encephalitis: Insights Imaging, 2016; 7(2); 265-74
43. Kitabayashi Y, Ueda H, Narumoto J, Cerebral blood flow changes in general paresis following penicillin treatment: A longitudinal single photon emission computed tomography study: Psychiatry Clin Neurosci, 2002; 56(1); 65-70
44. Launes J, Sirén J, Valanne L, Unilateral hyperfusion in brain-perfusion SPECT predicts poor prognosis in acute encephalitis: Neurology, 1997; 48(5); 1347-51
45. Marra CM, Maxwell CL, Smith SL, Cerebrospinal fluid abnormalities in patients with syphilis: Association with clinical and laboratory features: J Infect Dis, 2004; 189(3); 369-76
46. Wormser GP, Pavia CS, Neurosyphilis: N Engl J Med, 2019; 381(24); 2376-77
47. Tuddenham S, Ghanem KG, Neurosyphilis: Knowledge gaps and controversies: Sex Transm Dis, 2018; 45(3); 147-51
Tables
 Table 1. Demographic variables and clinical signs of the asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.
Table 1. Demographic variables and clinical signs of the asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups. Table 2. Neuropsychological assessments of asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.
Table 2. Neuropsychological assessments of asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups. Table 3. Laboratory results in serum and cerebrospinal fluid from asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups.
Table 3. Laboratory results in serum and cerebrospinal fluid from asymptomatic neurosyphilis (ANS), neurosyphilis-mild cognitive impairment (MCI), and neurosyphilis-dementia groups. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








