24 November 2022: Clinical Research
Single-Center Study in Lithuania to Evaluate the Role of Transthoracic Impedance Cardiography in the Diagnosis and Outcome Evaluation of 301 Patients with Chronic Heart Failure Exacerbation
Andrius Ališauskas1ABCDEFG*, Albinas Naudžiūnas1ACDEFG, Saulius SadauskasDOI: 10.12659/MSM.938389
Med Sci Monit 2022; 28:e938389
Abstract
BACKGROUND: Scientific data regarding transthoracic impedance cardiography (ICG) parameters and its utility in patients with heart failure (HF) remains controversial. This study from a single center in Lithuania aimed to evaluate the role of ICG in the diagnosis and outcome evaluation of patients who were admitted to the hospital due to HF exacerbation.
MATERIAL AND METHODS: The sample consisted of 301 consecutive patients with a previous chronic HF diagnosis (166 men, 135 women) hospitalized for HF flare-ups. ICG data were compared to other noninvasive HF diagnostic tests. Data about patient outcomes were gathered from the Lithuanian Medical Record Database.
RESULTS: A weak correlation of amino-terminal pro-brain natriuretic peptide (NT-proBNP) with thoracic fluid content (TFC) and thoracic fluid content index (TFCI) was found (r=0.204, P<0.001 and r=0.207, P<0.001, respectively). There was weak to moderate correlation of 6-min walk distance with main ICG data. There was weak correlation between left ventricular ejection fraction (LVEF) with TFCI (r=-0.163, P=0.005), systolic index (r=-0.137, P=0.017), and systolic time ratio (r=0.236, P<0.001). By multivariate Cox proportional analysis, the following parameters were independently associated with cardiac death (P<0.001): NT-proBNP ≥425.5 pmoL/L (hazard ratio (HR), 5.104, 95% confidence interval (CI) 3.326-7.832), TFC ≥36.9 1/kOhm (HR, 4.604, 95% CI 2.701-7.849), LVEF ≤40% (HR, 4.942, 95% CI 2.8256-8.647).
CONCLUSIONS: The combination of non-invasively measured TFC, LVEF, and NT-proBNP showed great prognostic value for predicting readmissions and cardiac death in patients with HF.
Keywords: Cardiography, Impedance, Echocardiography, Heart Failure, Pro-Brain Natriuretic Peptide (1-76), Walk Test, Male, Humans, Female, Stroke Volume, Lithuania, Ventricular Function, Left, Natriuretic Peptide, Brain, Prognosis, Chronic Disease, Peptide Fragments
Background
Heart failure (HF) is a complex clinical syndrome with the main symptoms of breathlessness, peripheral edema, and fatigue. During clinical stages of the disease, this syndrome can be accompanied by main clinical signs such as elevated jugular venous pressure, pulmonary crackles, fluid accumulation in peripheral tissues, and serous cavities [1]. Signs and symptoms are due to a structural or functional abnormality of the heart that results in elevated pressure inside the heart chambers or inadequate cardiac output at rest or during exercise [1]. Traditionally, HF is divided into distinct phenotypes based on the measurement of left ventricular ejection fraction (LVEF) [2]: HF with reduced LVEF (≤40%) is designated as heart failure with reduced ejection fraction, HF with mid-range LVEF (41–49%) is designated as heart failure with mildly reduced ejection fraction, and HF with normal LVEF (≥50%) is designated as heart failure with preserved ejection fraction. According to clinical presentation, HF is usually divided into 2 subgroups: chronic HF (CHF) and acute HF [1]. CHF describes patients who already have an established diagnosis of HF or who have a more gradual onset of symptoms. If CHF deteriorates, either suddenly or slowly, the episode can be described as decompensated HF. This can result in a hospital admission or treatment with intravenous diuretic therapy in the outpatient setting [1]. Currently, the prevalence of HF appears to be 1% to 2% in the adult population [3,4]. The prevalence increases with age, from around 1% in individuals younger than 55 years to >10% in those aged 70 years or older [1]. As researchers usually only include confirmed HF cases, the true prevalence is likely to be higher. The overall survival rate of patients with confirmed HF is slightly more than 56.7% at the 5-year margin and only 34.9% at the 10-year margin [5]. Patients with advanced HF (symptoms persist even with maximal therapy) have even worse prognosis, with a 5-year survival rate as low as 20% [6]. In 2021, the prevalence of HF in Lithuania was 30.15 of 1000 in the general population (84 682 total cases), proportion of patients admitted to hospitals was 3.59 of 1000 (10 076 total cases), mortality rate was 221.41 of 1000 inpatients, and average length of hospital stay was 28 days [7]. The current guidelines recommend the following tests in patients with suspected CHF [1]: a resting 12-lead electrocardiography (ECG), measurement of natriuretic peptides, including amino-terminal pro-brain natriuretic peptide (NT-proBNP), routine blood tests for comorbidities, transthoracic echocardiography (TTE), and chest radiography. If a patient is suspected to have acute HF, additional tests, such as lung ultrasound, mid-regional pro-atrial natriuretic peptide, serum troponin, D-dimer, procalcitonin, lactate, pulse oximetry, and arterial blood gas analysis, are recommended [1]. For the evaluation of patient outcomes and prognostication, the current guidelines [1] recommend the following tests: natriuretic peptides, serum creatinine, serum electrolytes, and iron status (transferrin, ferritin).
To improve the diagnosis of HF, it is important to search for new diagnostic methods or revive the old ones that are inexpensive, widely available, effective, preferably noninvasive, and have reliable prognostic significance. Transthoracic impedance cardiography (ICG) is one such test. It is a safe, noninvasive, and inexpensive diagnostic method based on the detection of changes in thoracic bio-impedance during the cycle of the heart. The cost of a commercially available ICG system is comparable to that of an electrocardiograph, and the technical skill needed to perform an ICG test is equivalent to that needed for recording ECG [8]. The recording procedure of ICG does not require any specially trained technicians (eg, ultrasonographers), it takes up to 10 min, the results are available immediately, and it can register many useful parameters relevant in diagnosis, real time monitoring, prognosis, and decision making in the treatment of patients with HF.
Numerous studies have been carried out in recent years that examine the possibilities of ICG in HF patients in various aspects: diagnosis, monitoring, treatment, and prognosis. Moderately strong to strong correlations between main ICG parameters and natriuretic peptides, cardiac ultrasound, and invasive diagnostic methods were observed in most studies. For example, Galas et al [9] showed that thoracic fluid content (TFC), the marker of chest congestion, had a moderately strong positive correlation with NT-proBNP (r=0.46,
Scientific data regarding ICG parameters and its applicability in patients with HF remain controversial. Our previous research has focused only on severe CHF flare-ups and involved only relatively small samples (60 patients [10] and 120 patients [11]), and patient outcomes were evaluated during short periods of time (6 months) [11]. Therefore, this present study from a single center in Lithuania aimed to evaluate the role of transthoracic impedance cardiography in the diagnosis and outcome evaluation of 301 patients with exacerbation of CHF.
Material and Methods
STUDIED SAMPLE:
All patients provided written informed consent for their participation in this study, the protocol of the study was approved by the local Kaunas Regional Biomedical Research Ethics Committee (approval no. BE-2–17), and all procedures were conducted in accordance with the principles of the Declaration of Helsinki. This prospective study was conducted between 2019 and 2022 in the Hospital of the Lithuanian University of Health Sciences (Lithuania). It was registered in the ClinicalTrials.gov registry, identifier: NCT05480345. The sample consisted of 301 consecutive patients (166 men, 135 women) admitted to the hospital due to CHF flare-ups. All patients at enrollment had a previously confirmed diagnosis of CHF, according to the current guidelines [1]. The following conditions were exclusion criteria: acute HF, acute myocardial infarction, QRS ≥120 ms, mean arterial pressure >130 mmHg, severe aortic regurgitation, severe aortic stenosis, HR >200 beats per min, implantable device measuring intrathoracic impedance, and patients with minute ventilation pacemakers [10,11,20].
METHODS OF EXAMINATION:
In accordance with current guidelines [1] the following investigations were performed: interview (anamnesis, symptoms, New York Heart Association [NYHA] class), physical examination (general inspection, lung auscultation), ECG, basic blood tests, NT-proBNP, chest radiography, and TTE. In addition, all patients underwent ICG, and selected patients underwent the 6-min walk test. Patients underwent ICG, blood sample collection for NT-proBNP serum concentration measurement, and 6-min walk test at enrollment and on the day of discharge from the hospital.
ICG parameters were recorded immediately after TTE, using a Niccomo™ transthoracic ICG monitor (Medis Medizinische Messtechnik GmbH, Ilmenau, Germany) [20] and on the last day of patient’s in-hospital treatment, except if there was a death during the hospitalization period. All ICG parameters were recorded, although we only evaluated the main parameters, suitable for the diagnosis and prognosis of HF: systolic index, TFC, cardiac output, TFCI, systolic time ratio, left cardiac work, and left cardiac work index [9–11,17].
The 6-min walk test was performed according to the most recent methodology and guidelines [21]. Only selected patients underwent the test (without severe limiting disabilities, such as advanced osteoarthritis) at enrollment and on the day of discharge from the hospital. The total 6-min walk distance (6MWD), as the main diagnostic and prognostic variable, was used for statistical analysis [21].
The primary endpoint was sudden cardiac death during in-hospital treatment and the secondary endpoint was death due to HF after discharge from the hospital. Data about patient outcomes after discharge from the hospital (readmissions, time to death due to HF) were gathered from an online database, the Lithuanian Medical Record Database (Electronic Information System of Health Services and Cooperation Infrastructure). These data were used to calculate Kaplan-Meier survival curves.
STATISTICAL ANALYSIS:
The analysis of the data was performed using IBM Statistical Package for Social Sciences Statistics for Windows, version 27.0 (SPSS, IBM Corp, Armonk, NY, USA). Descriptive statistics are presented as mean values with 95% CIs. Means between 2 independent groups were compared using the
Results
In this prospective study, we enrolled 301 consecutive patients with previously diagnosed CHF who were admitted to the hospital due to an HF flare-up; 135 were women (44.9%) and 166 were men (55.1%). The mean age of patients was 71.87 years (95% CI 70.4–73.4). The main characteristics of the patients are present in Table 1. The patients’ mean NT-proBNP serum level on admission was 283.9 pmoL/L (95% CI 261.26–306.48) and 192.9 pmoL/L (95% CI 160.94–224.87) on the day of discharge. The patients’ mean LVEF was 36.04% (95% CI 34.28–37.8). On the day of admission to the hospital, the distribution of patients by the NYHA classes was as follows: NYHA II, 33 patients (10.9%), NYHA III, 207 patients (68.8%), and NYHA IV, 61 patients (20.3%). On the day of discharge, the distribution was as follows: NYHA I, 1 patient (0.3%), NYHA II, 235 patients (78.1%), NYHA III, 56 patients (18.6%), and NYHA IV, 3 patients (1%).
We compared the relationships between NT-proBNP serum concentration, 6MWD, and LVEF with the main ICG parameters. The analysis revealed a weak correlation of NT-proBNP with TFC and TFCI, whereas the correlations between NT-proBNP and other ICG parameters were not significant (Table 2). The analysis of relationships between 6MWD and the main ICG parameters showed that there were weak to moderate correlations of 6MWD with systolic index, cardiac output, left cardiac work, left cardiac work index, and TFCI (Table 3); while the comparison of LVEF and ICG data showed only weak correlations of LVEF with systolic index, systolic time ratio, and TFC (Table 4).
We also compared the differences between main HF and ICG parameters between admission and discharge from the hospital by using the Wilcoxon signed ranks test (Table 5). Statistically significant results were obtained when evaluating main ICG parameters, NT-proBNP, and 6MWD.
Throughout a median follow-up period of 17 months, there were 128 deaths due to cardiac death in total (42.5%). We compared the main physical examination, laboratory, and instrumental test data between deceased and survived patient groups (Table 6). As seen in the table, there were significant differences in the main HF parameters, such as NYHA class, 6MWD, TTE parameters, ICG parameters (except cardiac output and left cardiac work index), and NT-proBNP, with patients who died during follow-up period having worse parameters. There were more readmissions in the deceased patient group as well: 1.59±0.789 vs 1.09±0.733 at 6 months (
To analyze the relationship of ICG data and other HF parameters with fatal outcome, we calculated Kaplan-Meier survival curves (Figures 1–3) and used univariate and multivariate Cox proportional-hazards models to calculate HRs for fatal outcome. Table 7 shows that univariate analysis parameters, such as systolic blood pressure, respiratory rate, LVEF, left ventricular end-diastolic dimension, left atrial dimension, serum creatinine, NT-proBNP, 6MWD, systolic index, TFC, and TFCI, showed a significant association with cardiac death. However, multivariate Cox proportional analysis revealed that only the following baseline variables were independently and significantly associated with cardiac death (
For the prediction of cardiac death in patients with HF, TFC ≥36.9 1/kOhm had a sensitivity of 80.5%, specificity of 55.5%, positive predictive value of 57.2%, negative predictive value of 79.3%, and predictive accuracy of 66% (Table 8). Adding predictors such as LVEF ≤40% or NT-proBNP ≥425.5 pmoL/L increased the predictive accuracy to 85.2% and 86.8%, respectively.
Patients with HF with reduced ejection fraction had significantly worse outcomes than patients with HF with mildly reduced and preserved ejection fraction (
Discussion
The major finding of the present study was that parameters such as TFC ≥36.9 1/kOhm, LVEF ≤40%, and NT-proBNP ≥425.5 pmoL/L were powerful and independent prognostic markers of worsening of HF and increased mortality. This study showed that HF patients with TFC ≥36.9 1/kOhm had a 4.6-times higher risk of dying from cardiac death than patients with TFC <36.9 1/kOhm. In patients with HF with reduced ejection fraction, this risk was 4.9-fold higher than that of patients with HF with mildly reduced and preserved ejection fraction. Patients with a baseline NT-proBNP ≥425.5 pmoL/L had a 5.1-fold higher risk of death during the follow-up period. Moreover, these parameters predicted a higher risk of readmission to the hospital due to HF exacerbation. We also found that the main ICG data had a weak to moderate correlation with other noninvasive HF diagnostic tests.
Most previous studies that investigated the value of ICG in the diagnosis and prognosis of patients with HF had small sample sizes [10,12,14,15,17], whereas the data of larger randomized clinical trials are controversial. For instance, Kamath et al [13] found the following: (1) only modest correlation between ICG and invasively measured cardiac output; (2) TFC measured by ICG is not a reliable measure of pulmonary capillary wedge pressure; (3) there is poor agreement between ICG and invasively measured hemodynamic profiles (kappa ≤0.1); and (4) ICG data do not have a good prognostic value. However, Myers et al [18], in their study with more than a thousand participants, found good prognostic value in the main ICG parameters. Some previous studies did not assess the progression of HF, namely readmission to the hospital; the primary endpoint in these studies was cardiac death [11,17], and some previous studies only included stable outpatients [14,17,18]. For this reason, our study included patients with more severe HF, namely those admitted to the hospital due to exacerbation of HF, and the sample size of the study was comparatively large. We also analyzed the prognostic significance of ICG data in predicting further hospitalizations within a period of 12 months from discharge from the hospital. To the best of our knowledge, there have been no other large clinical studies with patients who were hospitalized due to HF exacerbation.
Within a median follow-up period of 17 months (maximum follow-up 36 months), there were 128 fatal outcomes due to cardiac death in total (42.5%), which may be explained by the severity of hospitalized patients: 89.1% were NYHA class III and IV. This finding agrees with previous studies, in which survival at 5 years was only 20% in decompensated HF patients [6]. In the present study, there were more readmissions to the hospital due to HF exacerbation in patients who had worse ICG parameters at baseline, which is confirmed by most of previous studies; although, Gilewski et al and Kamath et al did not find such a connection [13,19].
In agreement with our previous research [10,11], we found only a modest to moderate correlation between ICG data and other noninvasive HF diagnostic methods. Also, as mentioned above, the data of the previous studies were controversial, with some finding a strong correlation [22], while others only a modest correlation [13]. We hypothesized that the best correlation would be observed between LVEF, NT-proBNP, and the main ICG parameters, but, to our surprise, the best correlation was observed between 6MWD and ICG data, which is in agreement with research of other investigators [23,24].
To predict outcomes in patients with HF, researchers have used ICG data in conjunction with other tools, such as TTE, natriuretic peptides, cardiopulmonary exercise, and invasive tests. In our present study, we employed TTE and NT-proBNP. The sensitivity, specificity, positive predictive value, negative predictive value, and a predictive accuracy of TFC alone were not perfect, but in combination with other tests, the predictive performance slightly increased. The data in other studies, again, are conflicting. For example, Malfatto et al found that for prediction of cardiac death at the 1-year follow-up, a combination of BNP ≥450 pg/mL and TFC ≥40/kOhm had a sensitivity of 89%, specificity of 86%, positive predictive value of 88%, and negative predictive value of 92%; the combination retained its powerful predictive value of mortality at the 4-year follow-up as well. Kamath et al, however, did not find any predictive use of ICG data [13]. In agreement with most of the small-scale studies, we found a great prognostic value in the combination of TFC with LVEF or TFC with NT-proBNP. With univariate analysis, systolic blood pressure, respiratory rate, LVEF, left ventricular end-diastolic dimension, left atrial dimension, serum creatinine, serum NT-proBNP, 6MWD, systolic index, TFC, and TFCI showed increased HRs for cardiac death, but this association was not clinically significant (the HRs were approximately equal to 1). In the present study, we used ICG and other noninvasive, widely available, and inexpensive diagnostic tests and found that these simple diagnostic tests had great prognostic power in the prediction of HF worsening and fatal outcomes.
There were 4 main limitations in our study. First, we enrolled all patients with HF regardless of their LVEF. Second, it was a single-center observational study, so data can be biased. Third, we included only hospitalized patients with moderate to severe HF, and patients with stable HF were not enrolled. Therefore, our results should not be generalized to the outpatient population, especially to those who have mild HF. Finally, as multiple studies suggest, ICG produces controversial data in both diagnostic and prognostic fields; therefore, clinicians cannot rely solely on ICG data.
Conclusions
The combination of noninvasively measured TFC, LVEF, and NT-proBNP is of great prognostic value for predicting readmissions and cardiac death in patients with CHF. However, the predictive value of these parameters in patients with CHF needs further evaluation.
Figures
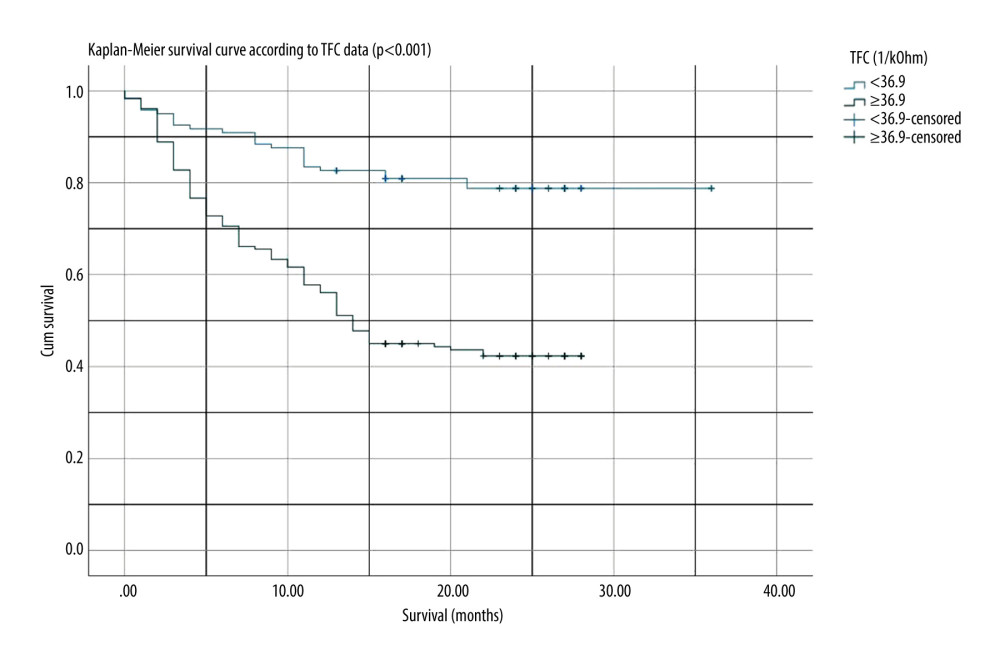 Figure 1. Kaplan-Meier survival curve according to thoracic fluid content (TFC) throughout a maximum follow-up of 36 months. Figure generated by SPSS version 27.0 (IBM Corp, Armonk, USA).
Figure 1. Kaplan-Meier survival curve according to thoracic fluid content (TFC) throughout a maximum follow-up of 36 months. Figure generated by SPSS version 27.0 (IBM Corp, Armonk, USA). 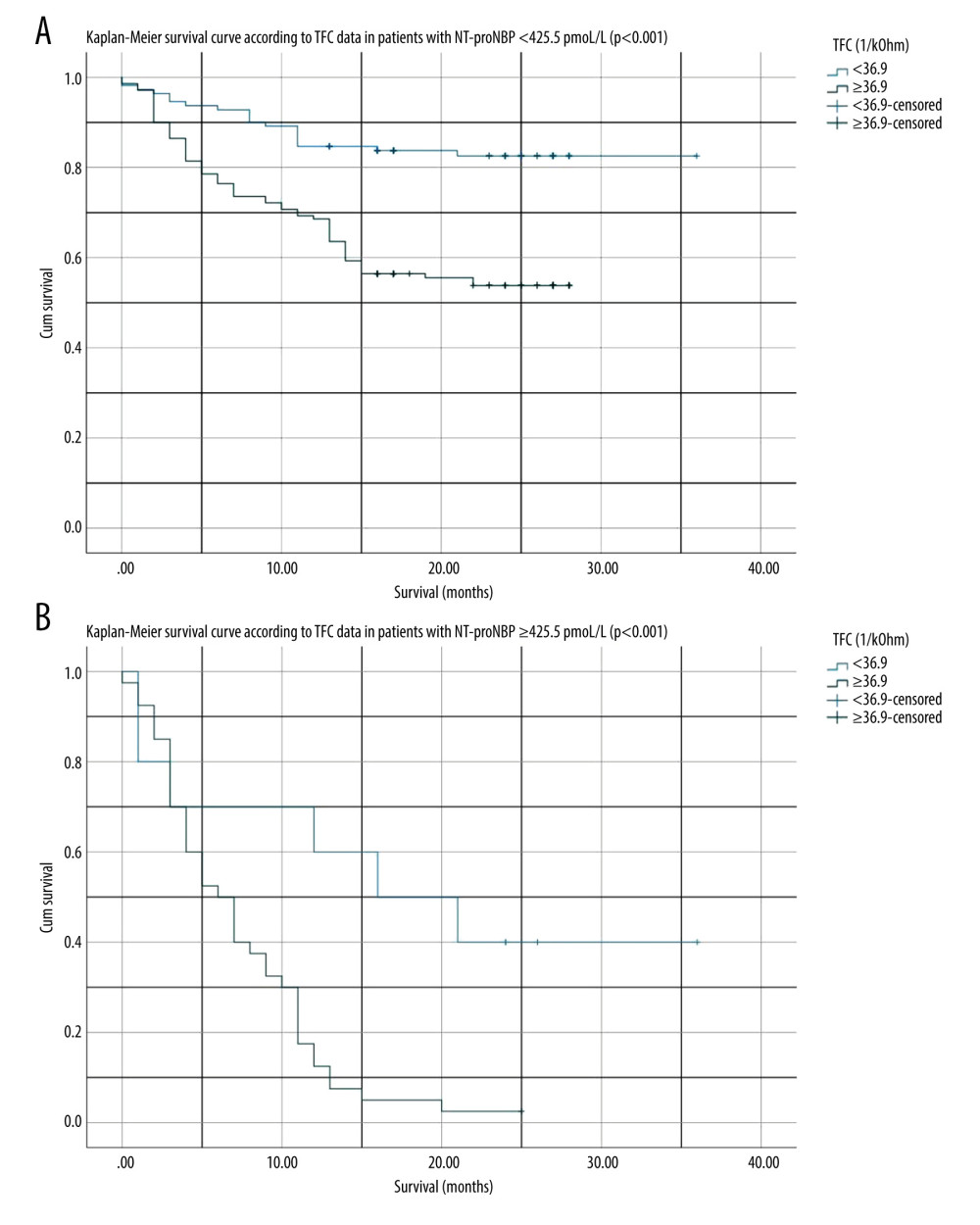 Figure 2. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with amino-terminal pro-brain natriuretic peptide (NT-proBNP) <425.5 pmoL/L throughout a maximal follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with NT-proBNP ≥425.5 pmoL/L throughout a maximum follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA).
Figure 2. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with amino-terminal pro-brain natriuretic peptide (NT-proBNP) <425.5 pmoL/L throughout a maximal follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with NT-proBNP ≥425.5 pmoL/L throughout a maximum follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA). 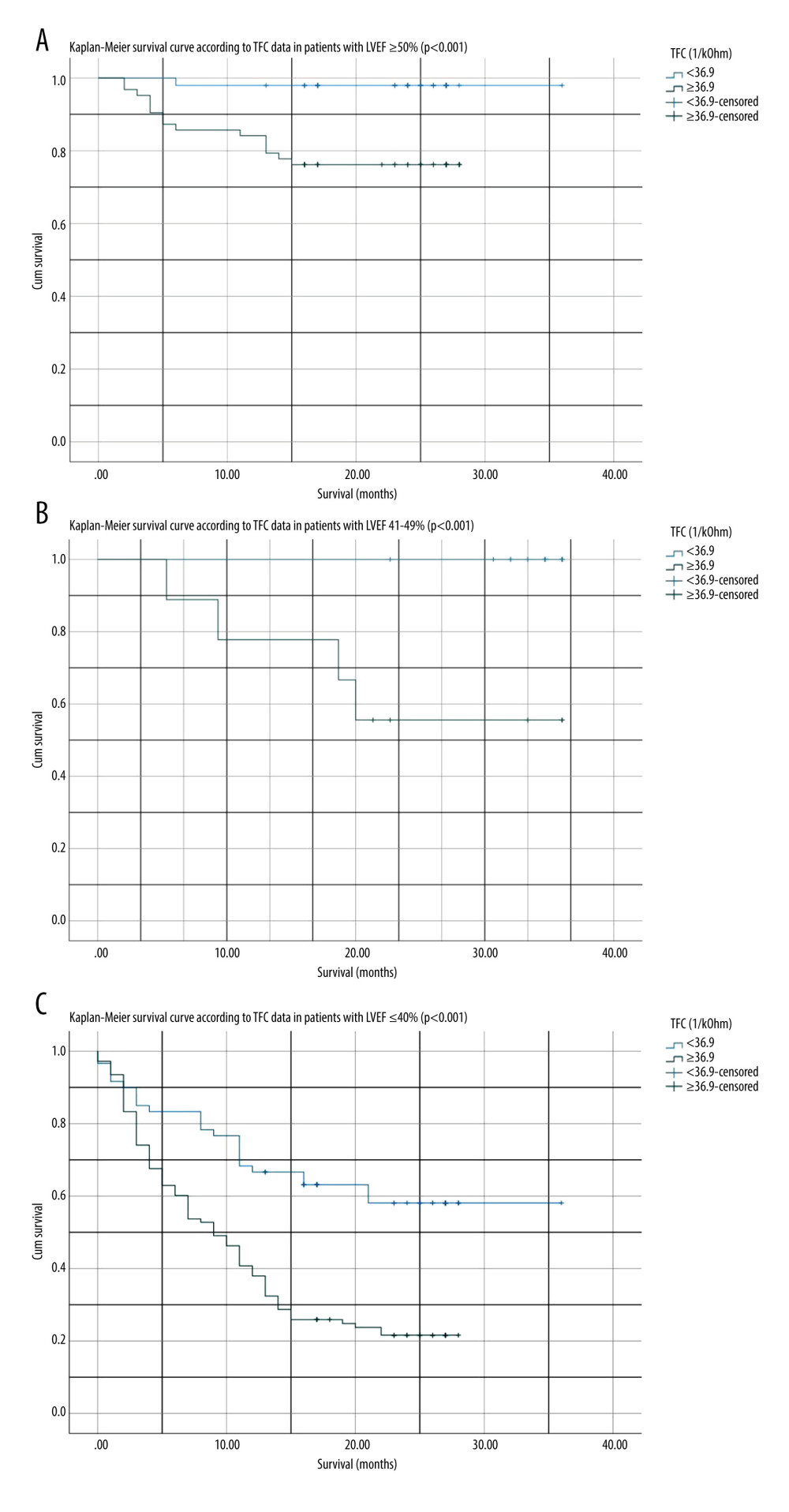 Figure 3. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with left ventricular ejection fraction (LVEF) ≥50% throughout a maximum follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with LVEF 41–49% throughout a maximum follow-up of 27 months. (C) Kaplan-Meier survival curve according to TFC in patients with LVEF ≤40% throughout a maximal follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA).
Figure 3. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with left ventricular ejection fraction (LVEF) ≥50% throughout a maximum follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with LVEF 41–49% throughout a maximum follow-up of 27 months. (C) Kaplan-Meier survival curve according to TFC in patients with LVEF ≤40% throughout a maximal follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA). Tables
Table 1. Main characteristics of the studied patients.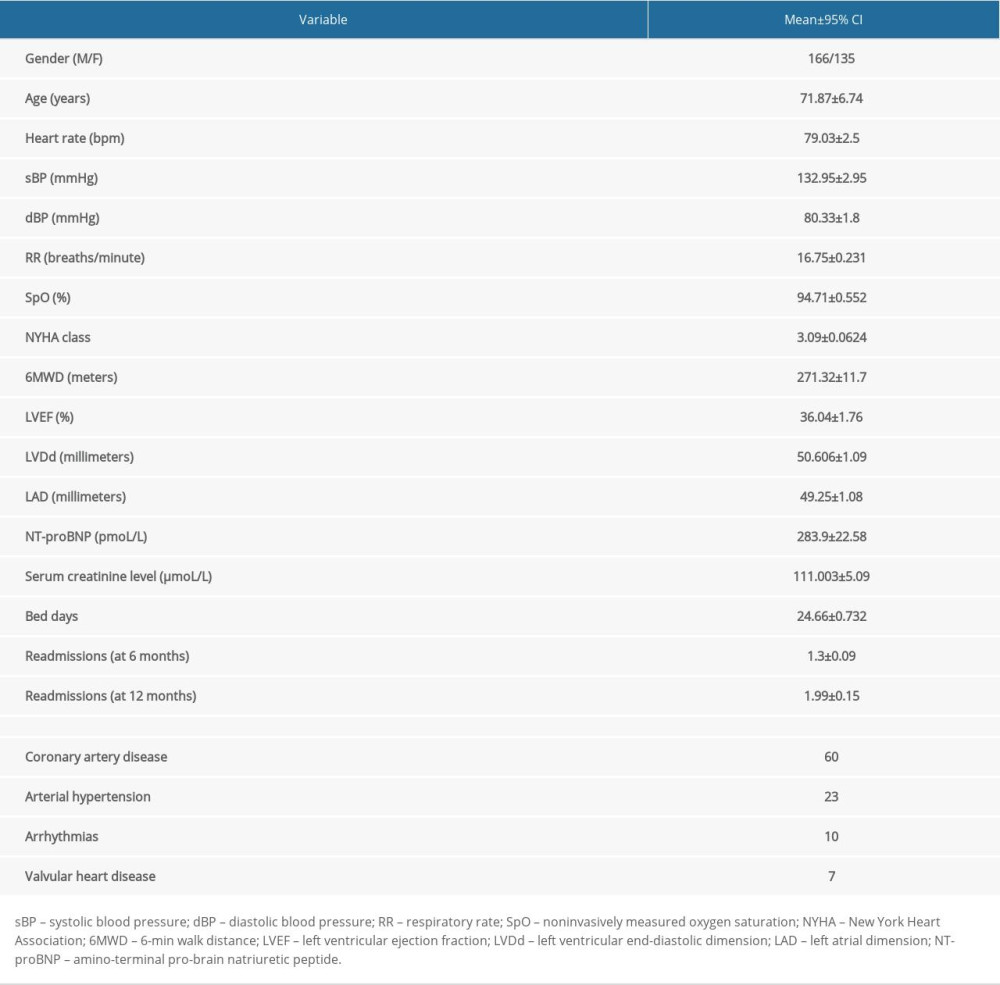 Table 2. Correlation between NT-proBNP and ICG data.
Table 2. Correlation between NT-proBNP and ICG data.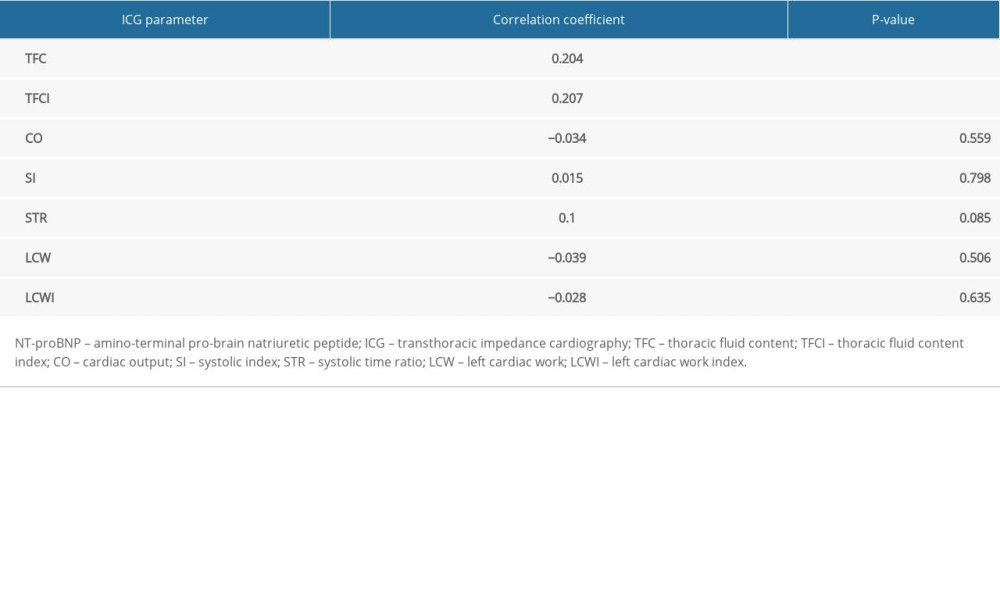 Table 3. Correlation between 6MWD and ICG data.
Table 3. Correlation between 6MWD and ICG data.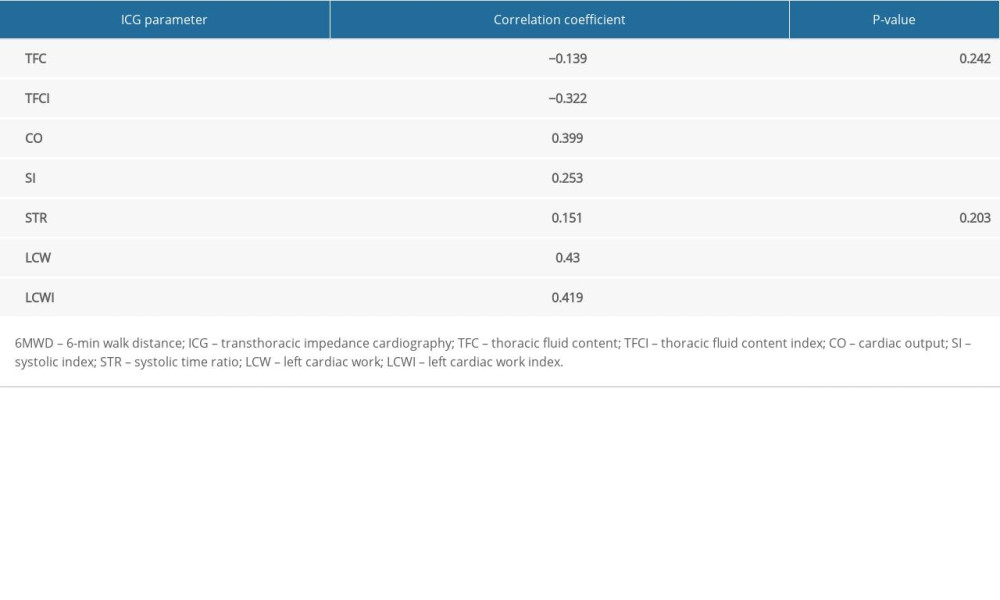 Table 4. Correlation between LVEF and ICG data.
Table 4. Correlation between LVEF and ICG data.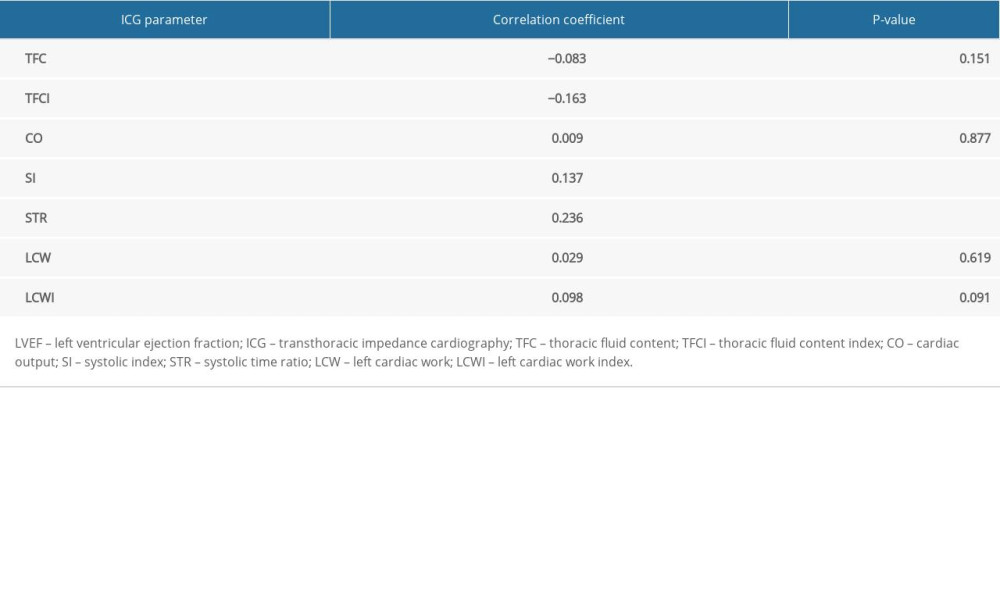 Table 5. Difference between main heart failure parameters on admission and at discharge.
Table 5. Difference between main heart failure parameters on admission and at discharge.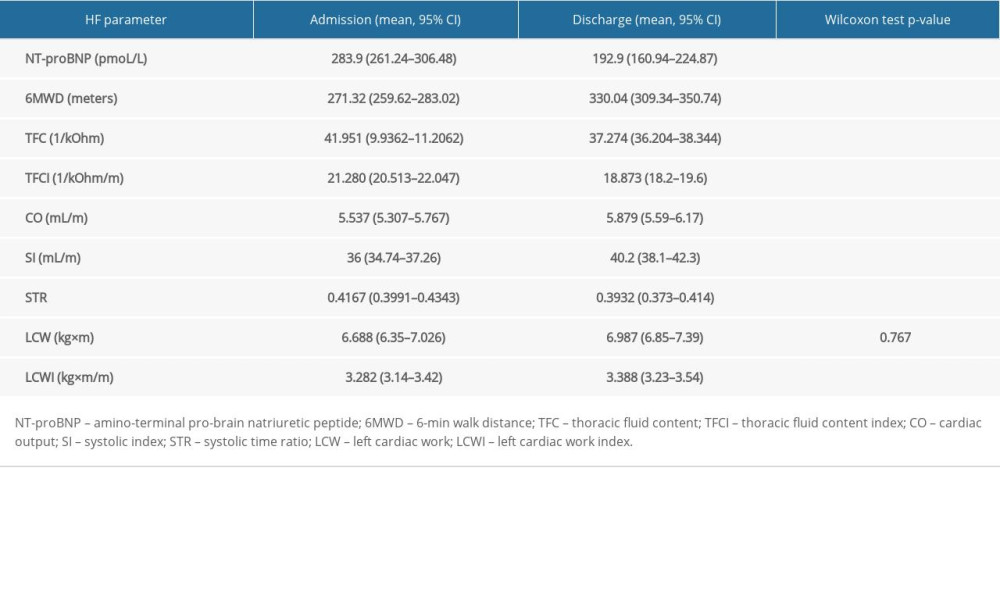 Table 6. The physical examination, laboratory, and instrumental test data comparison between deceased and survived patient groups.
Table 6. The physical examination, laboratory, and instrumental test data comparison between deceased and survived patient groups.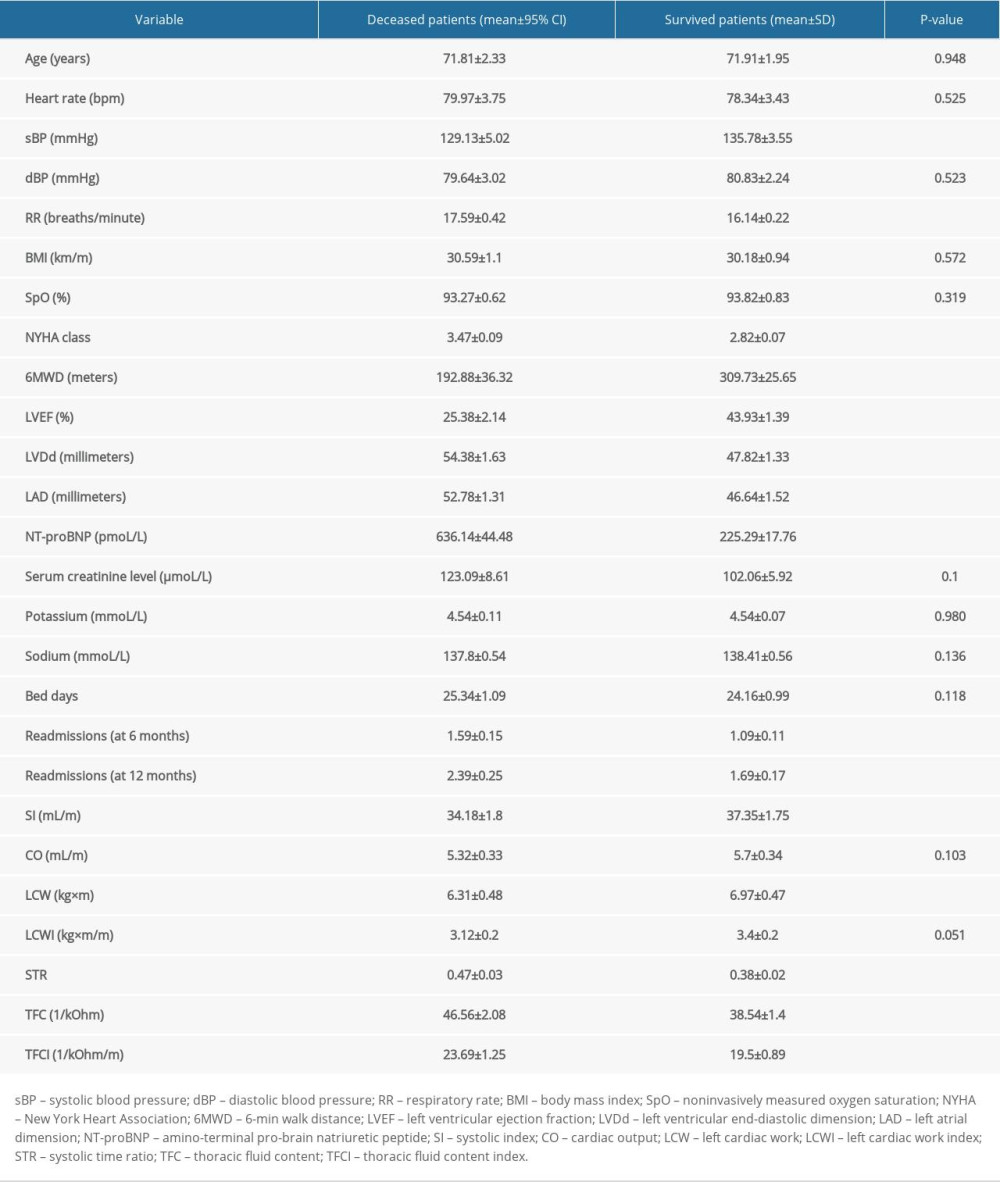 Table 7. Univariate and multivariate Cox proportional hazards analysis to identify heart failure patients at risk of cardiac death.
Table 7. Univariate and multivariate Cox proportional hazards analysis to identify heart failure patients at risk of cardiac death.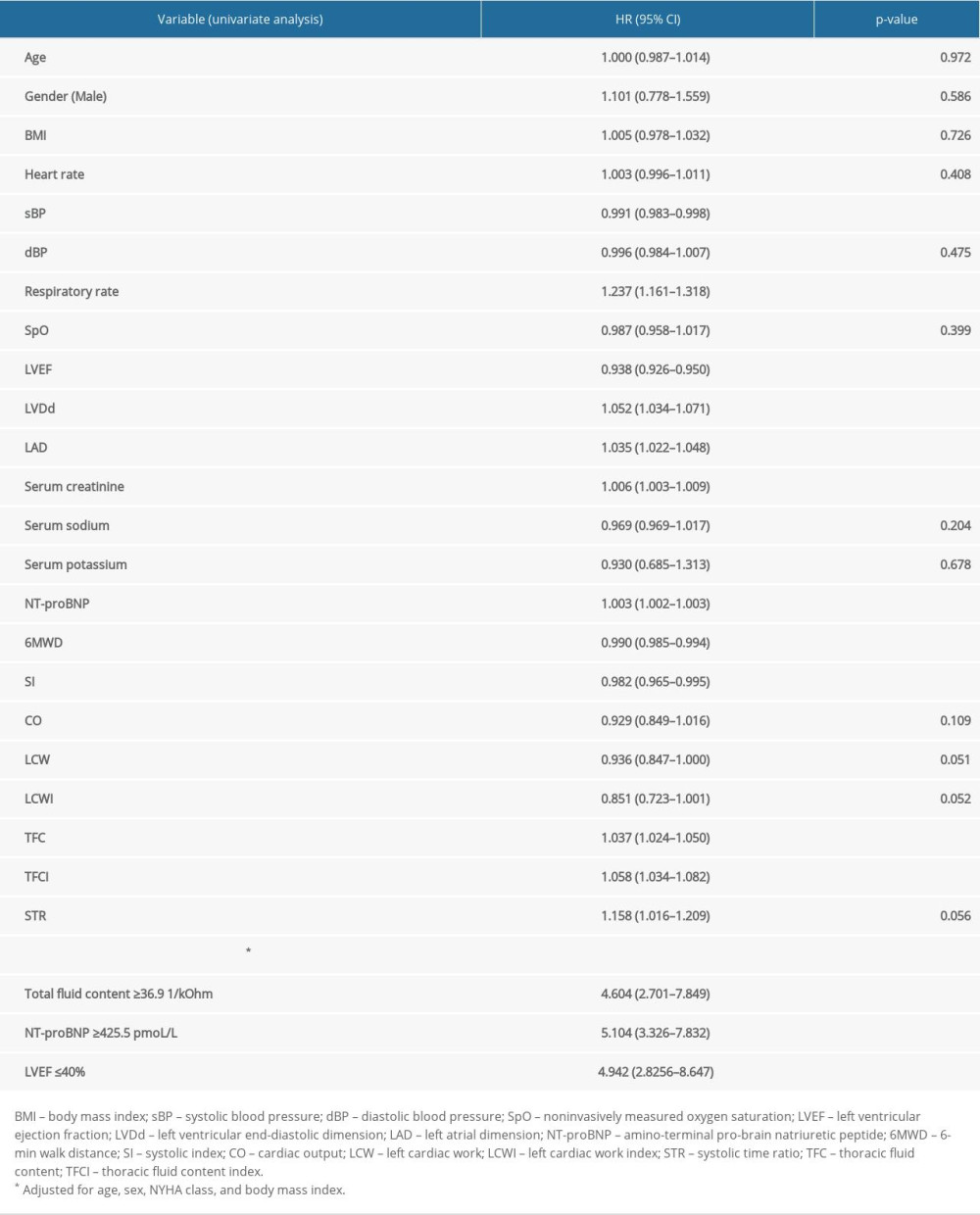 Table 8. Predictive value of the main heart failure parameters.
Table 8. Predictive value of the main heart failure parameters.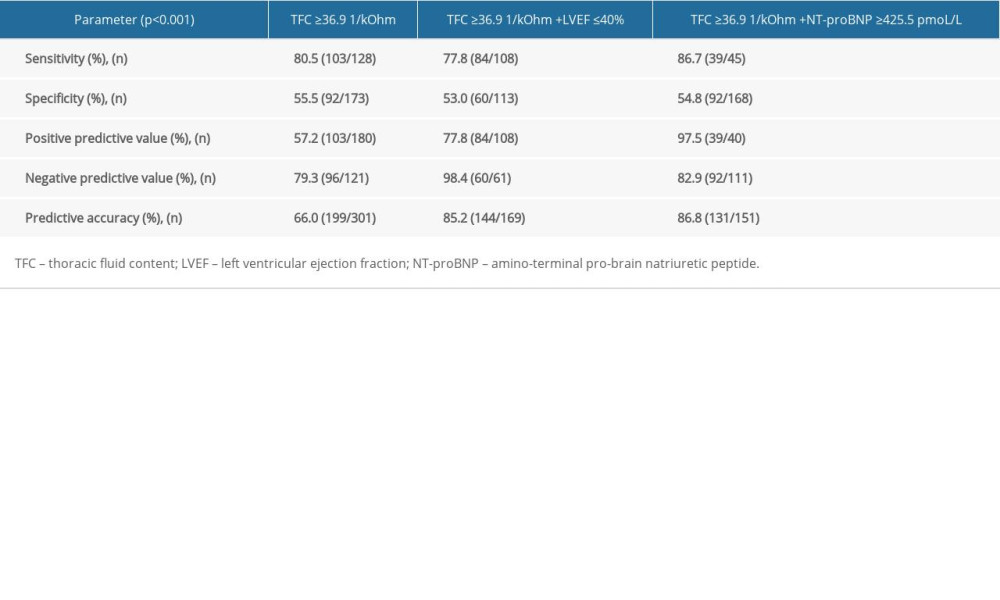
References
1. McDonagh TA, Metra M, Adamo M, 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: Eur Heart J, 2021; 42(36); 3599-26
2. Bozkurt B, Coats AJS, Tsutsui H, Universal definition and classification of heart failure: A report of the Heart Failure Society of America, Heart Failure Association of the European Society of Cardiology, Japanese Heart Failure Society and Writing Committee of the Universal Definition of Heart Failure: Endorsed by the Canadian Heart Failure Society, Heart Failure Association of India, Cardiac Society of Australia and New Zealand, and Chinese Heart Failure Association: Eur J Heart Fail, 2021; 23(3); 352-80
3. Conrad N, Judge A, Tran J, Temporal trends and patterns in heart failure incidence: A population-based study of 4 million individuals: Lancet, 2018; 391(10120); 572-80
4. Virani SS, Alonso A, Benjamin EJ, Heart disease and stroke statistics – 2020 update a report from the American Heart Association: Circulation, 2020; 141(9); E139-596
5. Jones NR, Roalfe AK, Adoki I, Survival of patients with chronic heart failure in the community: A systematic review and meta-analysis: Eur J Heart Fail, 2019; 21(11); 1306-25
6. Ammar KA, Jacobsen SJ, Mahoney DW, Prevalence and prognostic significance of heart failure stages: Application of the American College of Cardiology/American Heart Association heart failure staging criteria in the community: Circulation, 2007; 115(12); 1563-70
7. Health of the Lithuanian Population and the Activity of Healthcare Institutions in 2021: Vilnius, 2022 Available from: [in Lithuanian]https://stat.hi.lt/default.aspx
8. DeMarzo AP, Clinical use of impedance cardiography for hemodynamic assessment of early cardiovascular disease and management of hypertension: High Blood Press Cardiovasc Prev, 2020; 27(3); 203-13
9. Galas A, Krzesiński P, Gielerak G, Complex assessment of patients with decompensated heart failure: The clinical value of impedance cardiography and N-terminal pro-brain natriuretic peptide: Heart Lung, 2019; 48(4); 294-301
10. Sadauskas S, Naudžiūnas A, Unikauskas A, Applicability of impedance cardiography during heart failure flare-ups: Med Sci Monit, 2016; 22; 3614-22
11. Sadauskas S, Naudžiūnas A, Unikauskas A, Diagnostic and outcome prediction value of transthoracic impedance cardiography in heart failure patients during heart failure flare-ups: Med Sci Monit, 2018; 24; 6573-78
12. Facchini C, Malfatto G, Giglio A, Lung ultrasound and transthoracic impedance for noninvasive evaluation of pulmonary congestion in heart failure: J Cardiovas Med, 2016; 17(7); 510-17
13. Kamath SA, Drazner MH, Tasissa G, Correlation of impedance cardiography with invasive hemodynamic measurements in patients with advanced heart failure: The BioImpedance CardioGraphy (BIG) substudy of the Evaluation Study of Congestive Heart Failure and Pulmonary Artery Catheterization Effectiveness (ESCAPE) Trial: Am Heart J, 2009; 158(2); 217-23
14. Malfatto G, Blengino S, Perego GB, Transthoracic impedance accurately estimates pulmonary wedge pressure in patients with decompensated chronic heart failure: Congest Heart Fail, 2012; 18(1); 25-31
15. Malfatto G, Villani A, Rosa FD, Rella V, Correlation between trans and intra-thoracic impedance and conductance in patients with chronic heart failure: J Cardiovasc Med, 2016; 17(4); 276-82
16. Almeida GL, Xavier SS, Garcia MI, Clausell N, Hemodynamic assessment in heart failure: role of physical examination and noninvasive methods: Arq Bras Cardiol, 2012; 98(1); e15-21
17. Malfatto G, Corticelli A, Villani A, Transthoracic bioimpedance and brain natriuretic peptide assessment for prognostic stratification of outpatients with chronic systolic heart failure: Clin Cardiol, 2013; 36(2); 103-9
18. Myers J, Christle JW, Tun A, Cardiopulmonary exercise testing, impedance cardiography, and reclassification of risk in patients referred for heart failure evaluation: J Card Fail, 2019; 25(12); 961-68
19. Gilewski W, Pietrzak J, Banach J, Prognostic value of selected echocardiographic, impedance cardiographic, and hemodynamic parameters determined during right heart catheterization in patients qualified for heart transplantation: Heart Vessels, 2018; 33(2); 180-90
20. , Niccomo – Non-invasive continuous cardiac output monitor: Medizinische Messtechnik GmbH Available from: https://pdf.medicalexpo.com/pdf/medis-medizinische-messtechnik/niccomo/69321-158439.html
21. Holland AE, Spruit MA, Troosters T, An official European Respiratory Society/American Thoracic Society technical standard: Field walking tests in chronic respiratory disease: Eur Respir J, 2014; 44(6); 1428-46
22. Parrott CW, Burnham KM, Quale C, Lewis DL, Comparison of changes in ejection fraction to changes in impedance cardiography cardiac index and systolic time ratio: Congest Heart Fail, 2004; 10(2 Suppl 2); 11-13
23. Ding L, Quan XQ, Zhang S, Correlation between impedance cardiography and 6 min walk distance in atrial fibrillation patients: BMC Cardiovasc Disord, 2016; 16; 133
24. Liu F, Jones AYM, Tsang RCC, Noninvasive investigation of the cardiodynamic response to 6MWT in people after stroke using impedance cardiography: PLoS One, 2020; 15(6); e0233000
Figures
 Figure 1. Kaplan-Meier survival curve according to thoracic fluid content (TFC) throughout a maximum follow-up of 36 months. Figure generated by SPSS version 27.0 (IBM Corp, Armonk, USA).
Figure 1. Kaplan-Meier survival curve according to thoracic fluid content (TFC) throughout a maximum follow-up of 36 months. Figure generated by SPSS version 27.0 (IBM Corp, Armonk, USA). Figure 2. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with amino-terminal pro-brain natriuretic peptide (NT-proBNP) <425.5 pmoL/L throughout a maximal follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with NT-proBNP ≥425.5 pmoL/L throughout a maximum follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA).
Figure 2. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with amino-terminal pro-brain natriuretic peptide (NT-proBNP) <425.5 pmoL/L throughout a maximal follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with NT-proBNP ≥425.5 pmoL/L throughout a maximum follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA). Figure 3. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with left ventricular ejection fraction (LVEF) ≥50% throughout a maximum follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with LVEF 41–49% throughout a maximum follow-up of 27 months. (C) Kaplan-Meier survival curve according to TFC in patients with LVEF ≤40% throughout a maximal follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA).
Figure 3. (A) Kaplan-Meier survival curve according to thoracic fluid content (TFC) in patients with left ventricular ejection fraction (LVEF) ≥50% throughout a maximum follow-up of 36 months. (B) Kaplan-Meier survival curve according to TFC in patients with LVEF 41–49% throughout a maximum follow-up of 27 months. (C) Kaplan-Meier survival curve according to TFC in patients with LVEF ≤40% throughout a maximal follow-up of 36 months. Figures generated by SPSS version 27.0 (IBM Corp, Armonk, USA). Tables
 Table 1. Main characteristics of the studied patients.
Table 1. Main characteristics of the studied patients. Table 2. Correlation between NT-proBNP and ICG data.
Table 2. Correlation between NT-proBNP and ICG data. Table 3. Correlation between 6MWD and ICG data.
Table 3. Correlation between 6MWD and ICG data. Table 4. Correlation between LVEF and ICG data.
Table 4. Correlation between LVEF and ICG data. Table 5. Difference between main heart failure parameters on admission and at discharge.
Table 5. Difference between main heart failure parameters on admission and at discharge. Table 6. The physical examination, laboratory, and instrumental test data comparison between deceased and survived patient groups.
Table 6. The physical examination, laboratory, and instrumental test data comparison between deceased and survived patient groups. Table 7. Univariate and multivariate Cox proportional hazards analysis to identify heart failure patients at risk of cardiac death.
Table 7. Univariate and multivariate Cox proportional hazards analysis to identify heart failure patients at risk of cardiac death. Table 8. Predictive value of the main heart failure parameters.
Table 8. Predictive value of the main heart failure parameters. Table 1. Main characteristics of the studied patients.
Table 1. Main characteristics of the studied patients. Table 2. Correlation between NT-proBNP and ICG data.
Table 2. Correlation between NT-proBNP and ICG data. Table 3. Correlation between 6MWD and ICG data.
Table 3. Correlation between 6MWD and ICG data. Table 4. Correlation between LVEF and ICG data.
Table 4. Correlation between LVEF and ICG data. Table 5. Difference between main heart failure parameters on admission and at discharge.
Table 5. Difference between main heart failure parameters on admission and at discharge. Table 6. The physical examination, laboratory, and instrumental test data comparison between deceased and survived patient groups.
Table 6. The physical examination, laboratory, and instrumental test data comparison between deceased and survived patient groups. Table 7. Univariate and multivariate Cox proportional hazards analysis to identify heart failure patients at risk of cardiac death.
Table 7. Univariate and multivariate Cox proportional hazards analysis to identify heart failure patients at risk of cardiac death. Table 8. Predictive value of the main heart failure parameters.
Table 8. Predictive value of the main heart failure parameters. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








