14 February 2023: Database Analysis
Association Between Neutrophil-Lymphocyte Ratio and All-Cause Mortality in Critically Ill Patients with Chronic Obstructive Pulmonary Disease: A Retrospective Cohort Study
Shujie Hao1ABCDEF, Yamei Yuan1BDEG, Weidong Ye2BCD, Xiangming Fang2AEFG*DOI: 10.12659/MSM.938554
Med Sci Monit 2023; 29:e938554
Abstract
BACKGROUND: Neutrophil-lymphocyte ratio (NLR) is related to increased mortality risk in many diseases. However, there is limited research on critically ill patients with chronic obstructive pulmonary disease (COPD). A retrospective cohort study was performed to investigate whether NLR can be used as a biomarker to predict the mortality of critically ill COPD patients.
MATERIAL AND METHODS: In the research, the data were gathered from the database of the Medical Information Mart for Intensive Care-IV. The 28-day mortality was defined as the primary outcome, while the secondary outcomes were in-hospital and 90-day mortality. Through the application of the Kaplan-Meier curves and the multivariate Cox regression analysis, the potential association between NLR and mortality for critically ill patients with COPD was evaluated. For subgroup analysis, age, sex, ethnicity, mean blood pressure, and comorbidities were considered.
RESULTS: We extracted data on 2650 patients, of which 53.7% were male. A higher level of NLR was correlated with higher 28-day mortality risk. Compared to the lower quartile (NLR<4.56), HR (95% CI) of the upper quartile (NLR>16.86) was 1.75 (1.21-2.52) in the multivariate Cox regression model when adjusted for confounders (P=0.003). A similar tendency was found in the 90-day mortality (HR=1.59, 95% CI=1.16-2.19, P=0.004) and the in-hospital mortality (HR=1.71, 95% CI=1.22-2.42, P=0.002). Subgroup analyses showed that the correlation between NLR and 28-day mortality was stable.
CONCLUSIONS: The higher level of NLR is likely to be correlated with the increase of the all-cause mortality risk in critically ill patients with COPD, but this needs to be validated in future prospective research.
Keywords: COPD, Severe Early-Onset, Mortality, Humans, Male, Female, Neutrophils, Leukocyte Count, Critical Illness, Lymphocytes, Pulmonary Disease, Chronic Obstructive, Prognosis
Background
Chronic obstructive pulmonary disease (COPD) is a lung disease with persistent respiratory symptoms and airflow restriction; it is preventable, common, and treatable [1]. Many epidemiological studies and the Burden of Obstructive Lung Diseases show that a total of 391.9 million cases of COPD were found among individuals aged 30–79 years in 2019, with a worldwide prevalence of 10.3% (95% CI=8.2–12.8) [2]. The World Health Organization has reported that COPD is currently among the 3 major causes of death globally, causing around 3 million deaths each year, and also has substantial social and economic costs worldwide [3]. In the United States, it is estimated that the 20-year (2019–2038) direct medical cost for COPD is $800.9 billion [4]. In the coming decades, the COPD burden is expected to rise greatly all over the world due to the aging population in wealthy countries and the rising prevalence of smoking in developing countries [5].
It is well-known that inflammation plays an important role in the progression of COPD [6,7], and several biomarkers, including Interleukin-6 (IL-6) [8,9], C-reactive protein (CRP) [10,11], and Procalcitonin (PCT) [12], have been reported to be related to increased mortality in patients with COPD. However, high costs and technical issues prevent the clinical use of these inflammation biomarkers [13]. Neutrophil-lymphocyte ratio (NLR) is a cost-effective and rapid index that is easily obtained in clinical practice from routine laboratory tests [14]. Over the last 10 years, more studies have reported that NLR may be a new marker of systemic inflammation to assess the prognosis of many diseases, including acute coronary syndrome [15], stroke [16], inflammatory bowel disease [17], sepsis [18], and neoplastic disease [19]. Furthermore, a meta-analysis found that NLR levels had a good predictive value for disease severity and mortality among COVID-19 patients [20]. Recently, it was shown that NLR has is associated with COPD exacerbation and severity [21–24]. However, the sample size used in earlier research was limited, and most studies focused on the association between NLR and prognosis in the acute exacerbation of patients with COPD, and few studies that have focused on critically ill COPD patients.
In view of this, the present research aimed to analyze the relationship between NLR and mortality in critically ill COPD patients using the MIMIC-IV database. Our research hypothesis was that higher NLR is associated with higher mortality risk of critically ill COPD patients.
Material and Methods
DATA SOURCE:
All data were extracted from the Medical Information Mart for Intensive Care Database IV, which is considered the largest open-source and freely accessible clinical database in critical care. Based on the electronic medical records of patients hospitalized in the intensive care units (ICUs) of Beth Israel Deaconess Medical Center, the MIMIC database involves data on basic demographics, laboratory results, ICU monitoring records, and therapy prescriptions. The latest version of MIMIC-IV was available on the official website of Physionet (https://physionet.org/content/mimiciv/2.2/) [25,26], which contains approximately 250 000 electronic hospitalization records from 2008 to 2019. Shujie Hao completed the data research training program of the Collaborative Institutional Training Initiative (record ID 50152135) and gained access to the database. This database use was approved by the Institutional Review Boards of the Massachusetts Institute of Technology (Cambridge, MA) and the Beth Israel Deaconess Medical Center (Boston, MA). All patient identification data were recorded, and all personally identifiable information was concealed.
POPULATION SELECTION CRITERIA:
All critically ill patients with COPD as the primary diagnosis were enrolled using the Tenth Revision of International Classification of Diseases (ICD-10) in the MIMIC-IV database. Only the first ICU admission was taken into account when a patient had multiple ICU admissions. Patients were excluded if: (1) their ICU stay was less than 24 h, (2) their NLR data were incomplete or unavailable within 24 h after ICU admission, or (3) their record had more than 20% missing individual data.
DATA EXTRACTION:
PostgreSQL and a structured query language were used to extract data [27]. The baseline characteristics, including clinical severity scales, laboratory parameters, clinical parameters, and demographic parameters, were all collected 1 day after admission to the ICU. Demographic parameters were race, sex, and age. Clinical parameters were respiratory rate, heart rate, temperature, mean blood pressure (MBP), diastolic blood pressure (DBP), systolic blood pressure (SBP), percutaneous oxygen saturation (SPO2), and multiple comorbidities. Laboratory parameters were blood urea nitrogen (BUN), white blood cell (WBC) count, serum lactate, platelet count, hemoglobin, anion gap, hematocrit, serum bicarbonate, serum sodium, serum chloride, serum glucose, serum creatinine, serum potassium, neutrophil count, and lymphocyte count. The scoring systems included the Simplified Acute Physiology Score II (SAPS II) [28] and the Sequential Organ Failure Assessment (SOFA) [29].
The primary outcome in this study was 28-day mortality, with 90-day mortality and in-hospital mortality as secondary outcomes. NLR referred to the ratio of neutrophil count to lymphocyte count.
STATISTICAL ANALYSIS:
Patients were classified into quartiles according to NLR levels. Categorical variables were expressed as frequency (percentage), and continuous variables as mean±standard deviation. Different NLR quartile groups were compared by the Kruskal-Wallis test (non-normal distribution), one-way variance analysis (normal distribution), and chi-square test (categorical variables). The Kaplan-Meier (KM) survival analysis and the Cox proportional hazard regression model were used to determine the relationship between different categories of NLR and mortality. Three models were created: Model I, which was unadjusted; Model II, where covariates were adjusted for race, age, and sex; and Model III, which was further adjusted for model II plus some additional variables (
In this study, multiple multivariate imputations were used to impute missing values for continuous variables. The statistical software packages R 3.3.2 and free statistical software version 1.6 were used for statistical analysis. All of the tests were two-sided, and the statistical significance was set at
Results
BASELINE CHARACTERISTICS OF THE INCLUDED PARTICIPANTS:
A total of 2650 subjects were selected who fulfilled the inclusion criteria from the MIMIC-IV database in this study (Figure 1). Table 1 shows the detailed characteristics across NLR quartiles. Most patients (71.3%) were White. The patients had an average age of 71.8±11.4 years, and 53.7% were male. The overall mean NLR was 14.6±19.6. Participants in the highest NLR quartile group tended to be old and White, and to have a history of malignant cancer, congestive heart failure, or renal disease. As the NLR increased, heart rate, respiratory rate, platelet count, WBC count, anion gap, creatinine, glucose, and BUN levels increased, whereas SPO2, chloride, and sodium levels decreased. Additionally, patients with higher NLR had higher SAPS and SOFA scores.
RELATIONSHIP BETWEEN NLR AND MORTALITY:
Of the 2650 critically ill COPD patients enrolled, 28-day mortality was 14.1%, while 90-day mortality and in-hospital mortality were 17.1% and 15.2%, respectively. Kaplan-Meier survival curves showed significant differences in survival probability between groups. In addition, the survival probability was consistently observed to be markedly lower in the highest NLR quartile group (P<0.0001) (Figure 2). The independent effect of NLR on all-cause mortality in critically ill patients with COPD was decided through a further construction of the 3 different Cox regression models, as shown in Table 2. With the increase of NLR, HR value showed an upward trend in all 3 models. After controlling for potential confounders in Cox regression analysis, patients in the upper quartile group (NLR>16.86) saw a significantly higher risk of 28-day (HR=1.75, 95% CI=1.21–2.52, P=0.003), in-hospital (HR=1.71, 95% CI=1.22–2.42, P=0.002), and 90-day (HR=1.59, 95% CI=1.16–2.19, P=0.004) mortality than patients in the lower quartile group (NLR<4.56).
RESULTS OF SUBGROUP ANALYSIS:
The potential clinical heterogeneity was analyzed using interaction and stratified analyses. The NLR and all-cause mortality correlation was evaluated in different subgroups (Table 3). In the subgroup analysis of 28-day mortality, stratified and interaction analyses were not found in sex, age (<75 and ≥75), race, MBP (<75 and ≥75 mmHg), malignant cancer, liver disease, renal disease, congestive heart failure, diabetes, and hypertension.
In the subgroup analysis of in-hospital mortality, women with COPD (second quartile: HR=2.32, 95% CI=1.28, 4.22; third quartile: HR=2.07, 95% CI=1.15, 3.73; upper quartile: HR=2.78, 95% CI=1.57, 4.91;
Similar findings were found in patients with 90-day mortality of MBP ≥75 mmHg (second quartile: HR=2.07, 95% CI=1.2, 3.58; third quartile: HR=3.17, 95% CI=1.86, 5.41; upper quartile: HR=3.12, 95% CI=1.79, 5.42;
Discussion
This research explored the NLR and mortality correlation in COPD patients admitted to the ICU. The main finding is that higher NLR values have an independent relationship with an increased risk of 28-day, in-hospital, and 90-day mortality after controlling for important covariates.
NLR is a combination of lymphocyte and neutrophil counts that can predict the prognosis of patients. In recent years, NLR, as an emerging indicator of systemic inflammation, has been applied in COPD patients. Teng et al [22] discovered that the increased NLR is an independent risk factor for 28-day mortality (OR=1.067; 95% CI=1.039–1.095), ICU occupancy (OR=1.046; 95% CI=1.023–1.068), and invasive mechanical ventilation (OR=1.042; 95% CI=1.019–1.066) in a retrospective study of 698 patients with acute COPD exacerbation. In a 10-year prospective study of 386 patients with moderate to severe COPD, it was found that NLR was associated with long-term mortality in COPD patients (HR=1.090, 95% CI=1.036, 1.148) [30]. Emami et al [31] indicated that the mortality rate of patients with NLR≥6.9 is higher than those with NLR<6.9. There was an independent association between NLR and in-hospital mortality among patients with acute exacerbation of COPD. Our results agree with prior research findings in terms of the relationship between NLR and mortality among COPD patients. However, the sample size of previous studies was limited and potential confounders were not controlled for. Furthermore, they focused on the NLR and mortality correlation within the acute exacerbation of COPD patients.
The inflammatory process of COPD can be used to show the correlation between NLR and mortality. It has long been recognized that airway and systemic inflammation in COPD are related to disease progression, exacerbation, and mortality [32,33]. Neutrophils play a significant role in airway inflammation [34]. Several previous studies [35,36] have discovered that lung inflammation is maintained after smoking cessation and may progressively increase over time, indicating that neutrophil recruitment and activation could be caused by the continuous inflammatory response in the lungs [37]. When activated, human neutrophil lipocalin, myeloperoxidase (MPO), matrix metalloproteinase MMP-8 and MMP-9, cathepsin G, proteinase-3, and neutrophil elastase were released, contributing to the development and progression of COPD and emphysema [38]. Additionally, systemic inflammatory reactions are common in critically ill patients. Previous findings indicated that lymphopenia was related to high mortality rates in individuals with systemic inflammatory response syndrome, and lymphopenia could perpetuate harmful inflammation [39,40]. Lymphocyte count was negatively proportional to inflammation, and neutrophil count increased with the systemic inflammatory response, causing a higher NLR. Taken together, the level of NLR simultaneously provides information about 2 different immune pathways, indicating that the overall inflammatory state of the body has a higher predictive value of risk than alone [41], suggesting that the increase of NLR may be a crucial marker for monitoring the clinical prognosis of COPD.
In our subgroup analyses, taking 28-day mortality as an example, there were consistent findings within different subgroups by age (<75 and ≥75), sex, race, MBP (<75 and ≥75 mmHg), and COPD comorbidities, including malignancy, liver disease, renal disease, congestive heart failure, hypertension, and diabetes. However, critically ill COPD patients with MBP≥75 mmHg had a higher risk of 90-day and in-hospital mortality, and critically ill COPD patients with hypertension had a higher risk of 90-day mortality. The association between NLR and hypertension has been widely studied, and NLR is considered to be a reliable hypertension predictor [42–44]. Sun et al [45] found that a higher quartile of NLR is an independent predictor of all-cause 3-month mortality in patients with hypertension who are more than 80 years old (RR=16.451, 95% CI=2.137, 66.643). Several studies have shown that higher NLR is associated with a worse prognosis of hypertension [46–49], but this needs to be further confirmed. Interestingly, this study showed that COPD patients with a history of liver disease had a lower risk of in-hospital and 90-day mortality, with a higher NLR. However, the sample size of participants in the study was quite limited. A previous systematic review [50] found that NLR was a predictor for prognosis of patients with cirrhosis, but was not significantly associated with liver fibrosis in patients with chronic hepatitis C infection. Therefore, the potential mechanism underlying the association the outcome of COPD and these factors needs further research.
There are several limitations to the present study. Firstly, it was a retrospective and observational study, and causal inferences cannot be made. Secondly, there are still some unmeasured variables influencing results after adjusting for confounders as much as possible. This is because the MIMIC-IV databases do not record all of the variables, such as income, place of residence, insurance status, and educational attainment, which are likely to be relevant to mortality. Thirdly, attention was paid to the NLR value obtained within 24 h after ICU admission, but the impact of NLR changes on outcomes during the ICU stay is unknown. Finally, although this study had a relatively large sample size, multicenter prospective studies are needed to verify these findings in the future.
Conclusions
High NLR is associated with a higher risk of 28-day, in-hospital, and 90-day mortality in COPD patients admitted to the ICU. The level of NLR is likely to reliably predict the mortality risk in critically ill COPD patients, but this needs to be considered and confirmed in future prospective research.
Figures
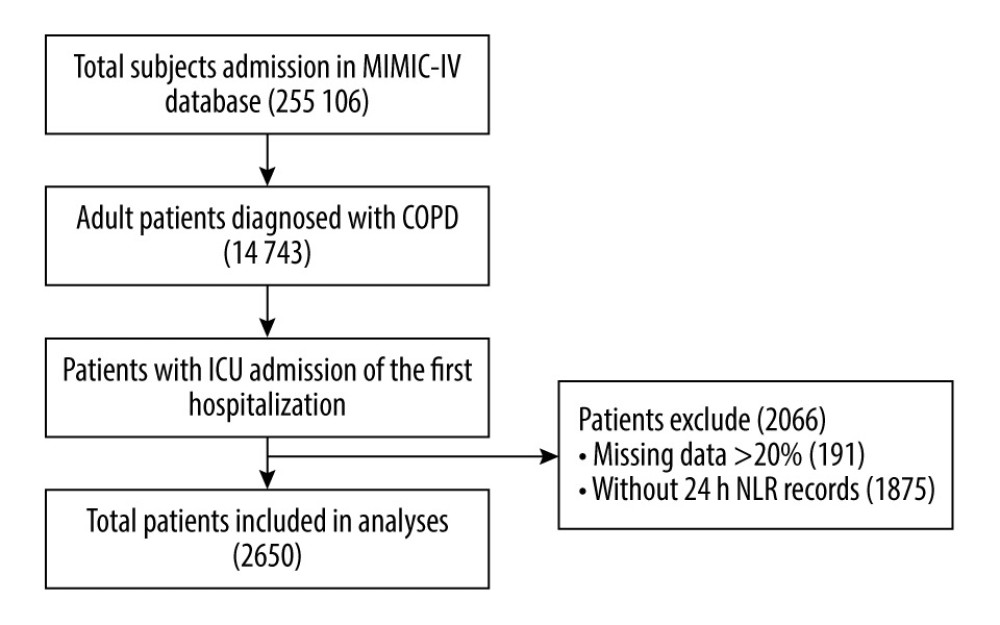 Figure 1. Flow chart of the population included in the study. MIMIC-IV – Medical Information Mart for Intensive Care-IV; COPD – chronic obstructive pulmonary disease; ICU – Intensive Care Unit; NLR – neutrophil-lymphocyte ratio.
Figure 1. Flow chart of the population included in the study. MIMIC-IV – Medical Information Mart for Intensive Care-IV; COPD – chronic obstructive pulmonary disease; ICU – Intensive Care Unit; NLR – neutrophil-lymphocyte ratio. 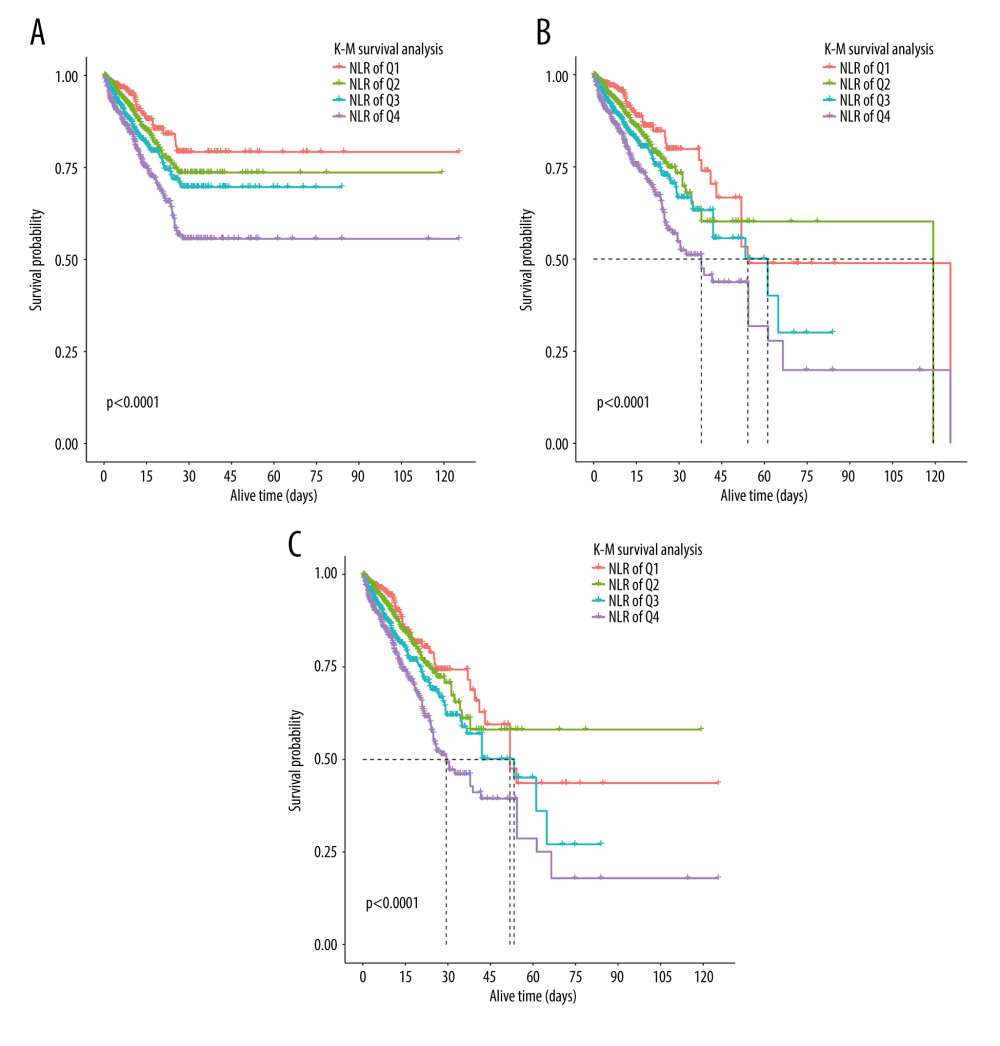 Figure 2. Kaplan-Meier survival curves showing the association between NLR and all-cause mortality. Image software: R 3.3.2, MathSoft. (A) 28-day mortality; (B) In-hospital mortality; (C) 90-day mortality.
Figure 2. Kaplan-Meier survival curves showing the association between NLR and all-cause mortality. Image software: R 3.3.2, MathSoft. (A) 28-day mortality; (B) In-hospital mortality; (C) 90-day mortality. References
1. Agusti A, Beasley R, Celli BR: 2022 Global strategy for prevention, diagnosis and management of COPD Available from: https://goldcopd.org/2022-gold-reports/
2. Adeloye D, Song P, Zhu Y, Global, regional, and national prevalence of, and risk factors for, chronic obstructive pulmonary disease (COPD) in 2019: A systematic review and modelling analysis: Lancet Respir Med, 2022; 10(5); 447-58
3. World Health Organization: The Global Health Observatory, Global Health Estimates: Life expectancy and leading causes of death and disability Available from: https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates
4. Zafari Z, Li S, Eakin MN, Projecting long-term health and economic burden of COPD in the United States: Chest, 2021; 159(4); 1400-10
5. Mathers CD, Loncar D, Projections of global mortality and burden of disease from 2002 to 2030: PLoS Med, 2006; 3(11); e442
6. Barnes PJ, Inflammatory mechanisms in patients with chronic obstructive pulmonary disease: J Allergy Clin Immunol, 2016; 138(1); 16-27
7. Brightling C, Greening N, Airway inflammation in COPD: Progress to precision medicine: Eur Respir J, 2019; 54(2); 1900651
8. Fermont JM, Masconi KL, Jensen MT, Biomarkers and clinical outcomes in COPD: A systematic review and meta-analysis: Thorax, 2019; 74(5); 439-46
9. Song W, Wang Y, Tian F, Clinical significance of procalcitonin, C-reactive protein, and interleukin-6 in helping guide the antibiotic use for patients with acute exacerbations of chronic obstructive pulmonary disease: Dis Markers, 2021; 2021; 8879401
10. Thomsen M, Ingebrigtsen TS, Marott JL, Inflammatory biomarkers and exacerbations in chronic obstructive pulmonary disease: JAMA, 2013; 309(22); 2353-61
11. Hoult G, Gillespie D, Wilkinson TMA, Biomarkers to guide the use of antibiotics for acute exacerbations of COPD (AECOPD): A systematic review and meta-analysis: BMC Pulm Med, 2022; 22(1); 194
12. Ni W, Bao J, Yang D, Potential of serum procalcitonin in predicting bacterial exacerbation and guiding antibiotic administration in severe COPD exacerbations: A systematic review and meta-analysis: Infect Dis (Lond), 2019; 51(9); 639-50
13. Sakurai K, Chubachi S, Irie H, Clinical utility of blood neutrophil-lymphocyte ratio in Japanese COPD patients: BMC Pulm Med, 2018; 18(1); 65
14. Günay E, Sarınç Ulaşlı S, Akar O, Neutrophil-to-lymphocyte ratio in chronic obstructive pulmonary disease: A retrospective study: Inflammation, 2014; 37(2); 374-80
15. Dong CH, Wang ZM, Chen SY, Neutrophil to lymphocyte ratio predict mortality and major adverse cardiac events in acute coronary syndrome: A systematic review and meta-analysis: Clin Biochem, 2018; 52; 131-36
16. Li W, Hou M, Ding Z, Prognostic value of neutrophil-to-lymphocyte ratio in stroke: A systematic review and meta-analysis: Front Neurol, 2021; 12; 686983
17. Fu W, Fu H, Ye W, Peripheral blood neutrophil-to-lymphocyte ratio in inflammatory bowel disease and disease activity: A meta-analysis: Int Immunopharmacol, 2021; 101(Pt B); 108235
18. Huang Z, Fu Z, Huang W, Huang K, Prognostic value of neutrophil-to-lymphocyte ratio in sepsis: A meta-analysis: Am J Emerg Med, 2020; 38(3); 641-47
19. Cupp MA, Cariolou M, Tzoulaki I, Neutrophil to lymphocyte ratio and cancer prognosis: An umbrella review of systematic reviews and meta-analyses of observational studies: BMC Med, 2020; 18(1); 360
20. Li X, Liu C, Mao Z, Predictive values of neutrophil-to-lymphocyte ratio on disease severity and mortality in COVID-19 patients: A systematic review and meta-analysis: Crit Care, 2020; 24(1); 647
21. Farah R, Ibrahim R, Nassar M, The neutrophil/lymphocyte ratio is a better addition to C-reactive protein than CD64 index as a marker for infection in COPD: Panminerva Med, 2017; 59(3); 203-9
22. Teng F, Ye H, Xue T, Predictive value of neutrophil to lymphocyte ratio in patients with acute exacerbation of chronic obstructive pulmonary disease: PLoS One, 2018; 13(9); e0204377
23. El-Gazzar AG, Kamel MH, Elbahnasy OKM, El-Naggar ME, Prognostic value of platelet and neutrophil to lymphocyte ratio in COPD patients: Expert Rev Respir Med, 2020; 14(1); 111-16
24. Lu FY, Chen R, Li N, Neutrophil-to-lymphocyte ratio predicts clinical outcome of severe acute exacerbation of COPD in frequent exacerbators: Int J Chron Obstruct Pulmon Dis, 2021; 16; 341-49
25. Johnson A, Bulgarelli L, Pollard T, MIMIC-IV (version 2.2): PhysioNet, 2023 Available from: https://doi.org/10.13026/6mm1-ek67
26. Peng CK, Stanley HE, PhysioBank, PhysioToolkit, and PhysioNet: Components of a new research resource for complex physiologic signals: Circulation, 2000; 101(23); E215-E20
27. : Patrick Structured Query Language (SQL) fundamentals, 2008, Upper Saddle River (NJ), Prentice Hall
28. Le Gall JR, Lemeshow S, Saulnier F, A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study: JAMA, 1993; 270(24); 2957-63
29. Vincent JL, Moreno R, Takala J, The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine: Intensive Care Med, 1996; 22(7); 707-10
30. Sorensen AK, Holmgaard DB, Mygind LH, Neutrophil-to-lymphocyte ratio, calprotectin and YKL-40 in patients with chronic obstructive pulmonary disease: Correlations and 5-year mortality – a cohort study: J Inflamm (Lond), 2015; 12; 20
31. Emami Ardestani M, Alavi-Naeini N, Evaluation of the relationship of neutrophil to lymphocyte ratio and platelet-to-lymphocyte ratio with in-hospital mortality in patients with acute exacerbation of chronic obstructive pulmonary disease: Clin Respir J, 2021; 15(4); 382-88
32. Angelis N, Porpodis K, Zarogoulidis P, Airway inflammation in chronic obstructive pulmonary disease: J Thorac Dis, 2014; 6(Suppl 1); S167-72
33. Celli BR, Locantore N, Yates J, Inflammatory biomarkers improve clinical prediction of mortality in chronic obstructive pulmonary disease: Am J Respir Crit Care Med, 2012; 185(10); 1065-72
34. Barnes PJ, Inflammatory endotypes in COPD: Allergy, 2019; 74(7); 1249-56
35. Rutgers SR, Postma DS, ten Hacken NH, Ongoing airway inflammation in patients with COPD who do not currently smoke: Thorax, 2000; 55(1); 12-18
36. King PT, Inflammation in chronic obstructive pulmonary disease and its role in cardiovascular disease and lung cancer: Clin Transl Med, 2015; 4(1); 68
37. Kido T, Tamagawa E, Bai N, Particulate matter induces translocation of IL-6 from the lung to the systemic circulation: Am J Respir Cell Mol Biol, 2011; 44(2); 197-204
38. Paliogiannis P, Fois AG, Sotgia S, Neutrophil to lymphocyte ratio and clinical outcomes in COPD: Recent evidence and future perspectives: Eur Respir Rev, 2018; 27(147); 170113
39. Riff R, Cohen Y, Eini-Rider H, Systemic inflammatory response syndrome-related lymphopenia is associated with adenosine A1 receptor dysfunction: J Leukoc Biol, 2017; 102(1); 95-103
40. Li W, Ai X, Ni Y, The association between the neutrophil-to-lymphocyte ratio and mortality in patients with acute respiratory distress syndrome: A retrospective cohort study: Shock, 2019; 51(2); 161-67
41. Celikbilek M, Dogan S, Akyol L, Neutrophil-lymphocyte ratio in patients with familial Mediterranean fever: J Clin Lab Anal, 2015; 29(1); 80-83
42. Srinivasagopalane B, Andrew Rajarathinam S, Balasubramaiyan T, Clinical pertinence of neutrophil-to-lymphocyte ratio among hypertensives with different grades and duration of hypertension – an insight: Clin Exp Hypertens, 2019; 41(4); 394-99
43. Bozduman F, Yildirim E, Cicek G, Biomarkers of nondipper hypertension in prehypertensive and hypertensive patients: Biomark Med, 2019; 13(5); 371-78
44. Liu X, Zhang Q, Wu H, Blood neutrophil to lymphocyte ratio as a predictor of hypertension: Am J Hypertens, 2015; 28(11); 1339-46
45. Sun X, Luo L, Zhao X, Ye P, Du R, The neutrophil-to-lymphocyte ratio on admission is a good predictor for all-cause mortality in hypertensive patients over 80 years of age: BMC Cardiovasc Disord, 2017; 17(1); 167
46. Balta S, Ozturk C, Yildirim AO, The relation between neutrophil-lymphocyte ratio and hypertension: Am J Hypertens, 2015; 28(11); 1386
47. Wang H, Hu Y, Geng Y, The relationship between neutrophil to lymphocyte ratio and artery stiffness in subtypes of hypertension: J Clin Hypertens (Greenwich), 2017; 19(8); 780-85
48. Derya MA, Demir V, Ede H, Relationship between neutrophil/lymphocyte ratio and epicardial fat tissue thickness in patients with newly diagnosed hypertension: J Int Med Res, 2018; 46(3); 940-50
49. Chen ZN, Huang YR, Chen X, Value of neutrophil-to-lymphocyte ratio as a marker of renal damage in patients with H-type hypertension: Biomark Med, 2021; 15(9); 637-46
50. Peng Y, Li Y, He Y, The role of neutrophil to lymphocyte ratio for the assessment of liver fibrosis and cirrhosis: A systematic review: Expert Rev Gastroenterol Hepatol, 2018; 12(5); 503-13
Figures
 Figure 1. Flow chart of the population included in the study. MIMIC-IV – Medical Information Mart for Intensive Care-IV; COPD – chronic obstructive pulmonary disease; ICU – Intensive Care Unit; NLR – neutrophil-lymphocyte ratio.
Figure 1. Flow chart of the population included in the study. MIMIC-IV – Medical Information Mart for Intensive Care-IV; COPD – chronic obstructive pulmonary disease; ICU – Intensive Care Unit; NLR – neutrophil-lymphocyte ratio. Figure 2. Kaplan-Meier survival curves showing the association between NLR and all-cause mortality. Image software: R 3.3.2, MathSoft. (A) 28-day mortality; (B) In-hospital mortality; (C) 90-day mortality.
Figure 2. Kaplan-Meier survival curves showing the association between NLR and all-cause mortality. Image software: R 3.3.2, MathSoft. (A) 28-day mortality; (B) In-hospital mortality; (C) 90-day mortality. Tables
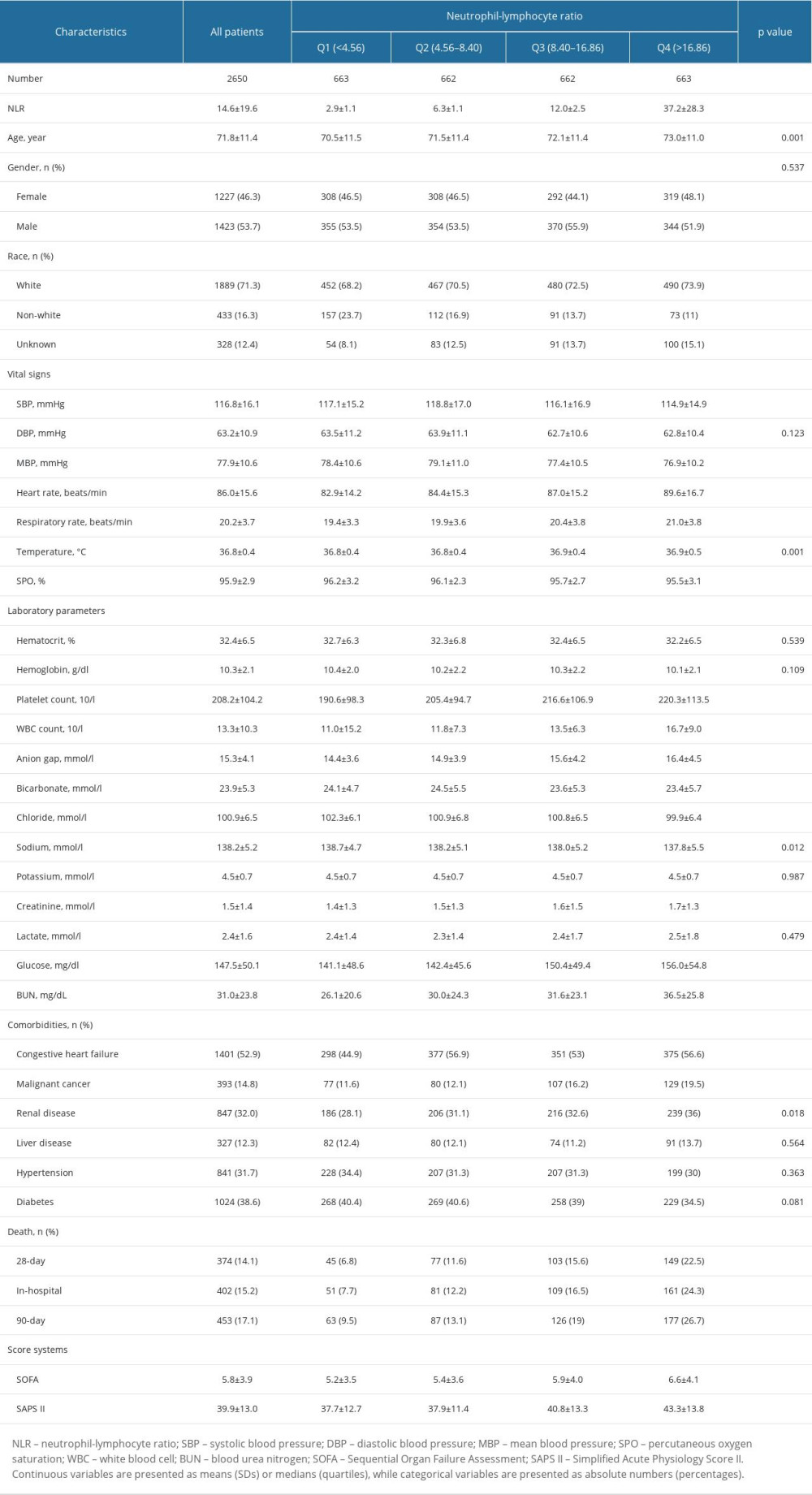 Table 1. Baseline characteristics of the study population.
Table 1. Baseline characteristics of the study population.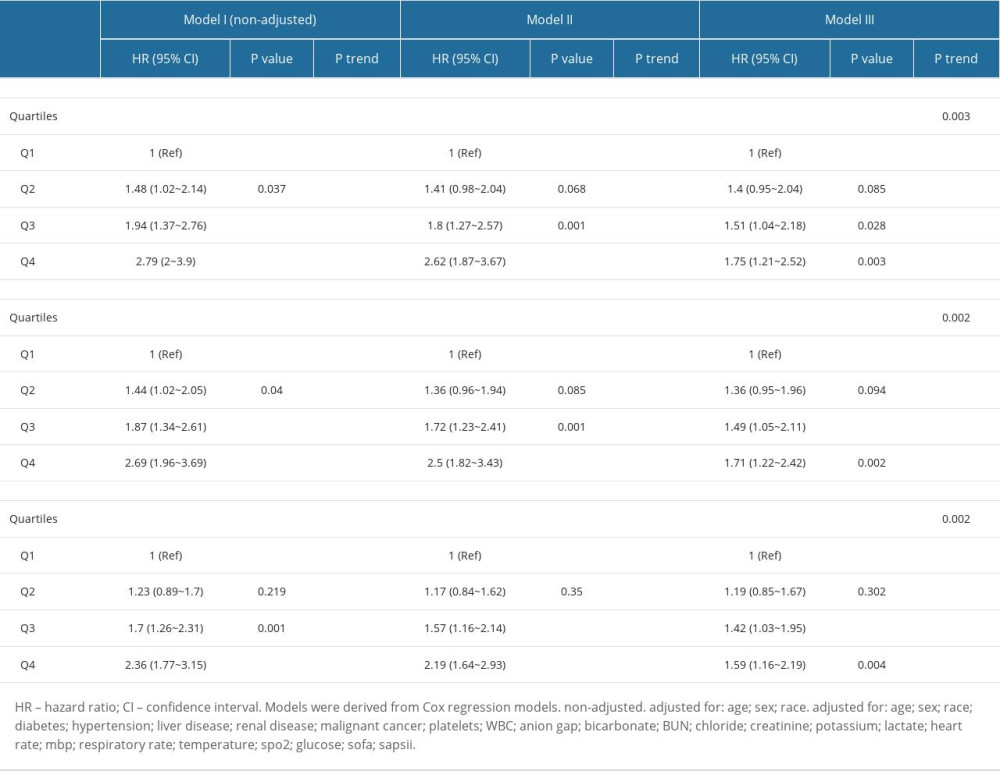 Table 2. HRs (95% CIs) for mortality across groups of neutrophil-lymphocyte ratio.
Table 2. HRs (95% CIs) for mortality across groups of neutrophil-lymphocyte ratio.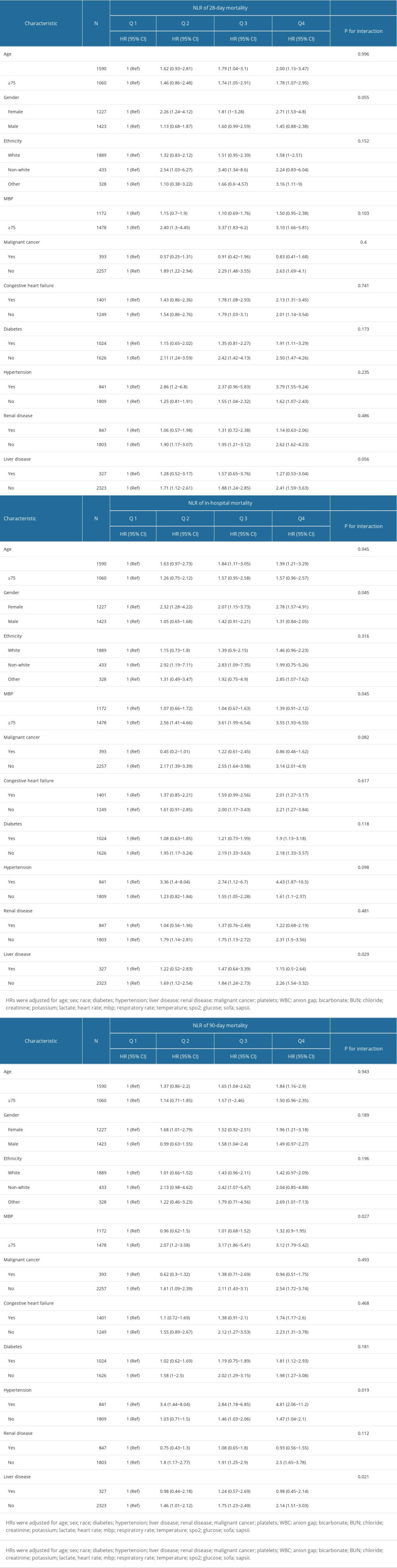 Table 3. Subgroup analysis of the associations between mortality and the neutrophil-lymphocyte ratio.
Table 3. Subgroup analysis of the associations between mortality and the neutrophil-lymphocyte ratio. Table 1. Baseline characteristics of the study population.
Table 1. Baseline characteristics of the study population. Table 2. HRs (95% CIs) for mortality across groups of neutrophil-lymphocyte ratio.
Table 2. HRs (95% CIs) for mortality across groups of neutrophil-lymphocyte ratio. Table 3. Subgroup analysis of the associations between mortality and the neutrophil-lymphocyte ratio.
Table 3. Subgroup analysis of the associations between mortality and the neutrophil-lymphocyte ratio. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








