27 December 2022: Clinical Research
Effect of Physiotherapy to Correct Rounded Shoulder Posture in 30 Patients During the COVID-19 Pandemic in South Korea Using a Telerehabilitation Exercise Program to Improve Posture, Physical Function, and Reduced Pain, with Evaluation of Patient Satisfaction
Yongwoo Lee1ACDEG*, Ki Bum Jung1ABCDEFDOI: 10.12659/MSM.938926
Med Sci Monit 2022; 28:e938926
Abstract
BACKGROUND: This study aimed to evaluate the effect of physiotherapy to correct rounded shoulder posture (RSP) in 30 patients during the COVID-19 pandemic in South Korea using telerehabilitation exercise programs to improve posture and physical function and reduce pain, with evaluation of patient satisfaction.
MATERIAL AND METHODS: Thirty participants with RSP participated in this study for 4 weeks from May to June 2021. Participants were randomly divided into an experimental group (EG, n=15) or control group (CG, n=15). Both groups performed shrug exercise 3 days a week for 4 weeks, while the EG performed self-upper-extremity neural mobilization (SUENM) for 7 more minutes. The pectoralis minor length index for posture, neck range of motion (ROM) and scapular muscle activity for physical function, pressure pain threshold (PPT) for pain, and questionnaires for telerehabilitation satisfaction were assessed. All exercises were conducted at home using videoconferencing.
RESULTS: The EG significantly improved PPT and ROM of extension and right-side bending of the neck compared to the CG (P<0.05) and it significantly reduced the muscle activity of the upper trapezius at 60°, 90°, and 120° shoulder flexion compared to the CG (P<0.05). In the satisfaction survey, participants cited the freedom of time and space as an advantage of telerehabilitation (100%) and reported difficulty in performing correct action as a disadvantage (69.2%).
CONCLUSIONS: These findings support those from recent studies on real-time telerehabilitation physiotherapy exercise programs. However, long-term controlled studies are required to develop evidence-based protocols for implementing and evaluating clinical outcomes of remote physiotherapy programs.
Keywords: COVID-19, Electromyography, Physical Distancing, Posture, telerehabilitation, Humans, Shoulder, Patient Satisfaction, Pandemics, COVID-19, Physical Therapy Modalities, Exercise Therapy, Pain
Background
After the World Health Organization (WHO) officially declared COVID-19 a global pandemic, the need for social distancing to prevent the spread of the virus necessitated the provision of remote services across all fields, including society, the economy, education, and medical care [1]. In particular, because COVID-19 is transmitted by droplets and contact in a short period of time, physical therapists who treat patients in close contact are more likely to be contagious. For this reason, the need for telerehabilitation instead of general physical therapy methods has emerged during the pandemic [2,3].
According to previous studies on telerehabilitation, active participation in appropriate telerehabilitation exercise program reportedly facilitated obesity prevention and provided back pain relief in women after childbirth [4], and improved the range of motion and balance in knee arthritis patients [5]. In addition, when telerehabilitation was applied to people with COVID-19 and post-COVID-19 conditions, the effect of improving physical function and reducing dyspnea was confirmed [6].
Although social distancing is effective for preventing infectious diseases, the frequency of complaints of musculoskeletal problems is increasing due to a decrease in physical activity resulting from the increase in remote work and limited use of indoor sports facilities [7,8]. In particular, prolonged computer use causes the head to assume a posture in which it is maintained in a relatively more frontal plane than the body centerline, leading to an increase in cervical lordosis and kyphosis in the thoracic spine, resulting in rounded shoulder posture (RSP), leading to neck and shoulder diseases [9].
Existing treatment methods for RSP include shrug exercise, push-up plus exercise, and THEREBANDTM exercise. These existing treatment methods tend to focus on the muscular problem, especially strengthening the upward rotation muscles of the scapula [10–12]. According to Sheikhhoseini et al [13], exercise therapy to improve forward-head posture significantly improved craniovertebral angle and moderately improved neck pain in forward-head posture participants. However, a recent study reported a limit to the recovery of upper-extremity function by only performing exercises that strengthen a single muscle as a treatment method for rounded shoulder posture [14]. When upper-extremity movement occurs, the nerve tissue undergoes changes, such as bending, rotation, elongation, and shortening, enabling natural motion with the muscles [15]. However, forms of body misalignment, such as a rounded shoulder, compress the nerve tissue, lower the physiological response of the nerves, and cause abnormal movement of the upper extremities, which can lead to neck and shoulder pain, limited range of motion, and decreased muscle strength [16]. Therefore, a neurological approach is needed to restore upper-extremity function in RSP [14].
Upper-extremity neural mobilization is a therapeutic technique that directly tenses and glides nerve tissue through arm movement, thereby reducing the pressure on the nerve tissue from the surrounding tissue and promoting the physiological response of the nerves [17,18]. A previous study reported that upper-extremity nerve mobilization was effective in alleviating neck and shoulder pain by reducing the mechano-sensitivity of nerves when applied to patients with chronic neck and shoulder pain [17,19,20]. Although upper-extremity nerve mobilization effectively alleviates neck and shoulder pain and movement of the upper extremities, most studies to date have been conducted on the neck, lower back, and carpal tunnel syndrome [17], and studies on RSP are scarce.
The World Confederation of Physical Therapy has emphasized the importance of telerehabilitation to improve safety and access to rehabilitation in the context of COVID-19 [21]. Therefore, this study aimed to evaluate the effect of physiotherapy to correct RSP in 30 patients during the COVID-19 pandemic in South Korea using telerehabilitation exercise programs to improve posture, physical function, and reduce pain, with evaluation of patient satisfaction. Self-upper-extremity neural mobilization (SUENM) was implemented as a telerehabilitation exercise program in this study.
Material and Methods
SUBJECTS:
The research was conducted with the approval of the Research Ethics Committee of SahmYook University (approval number: 2-1040781-A-N-012021016HR). It was conducted in accordance with the Declaration of Helsinki and its later amendments. Before the experiment, the subjects who participated in the study were fully informed about the purpose, process, and expected effects of the investigation, and written consent was obtained from all participants.
In this study, subjects with rounded shoulders were selected through a pre-screening test among adult men and women in their 20s and 30s attending SahmYook University in Seoul. The criteria for RSP were a vertical distance of 2.5 cm or more between the back of the acromion and the table in the supine position [22].
The inclusion criteria for the study were subjects with rounded shoulders, who had not received any treatment for neck and shoulder pain within the previous 6 weeks, had access to equipment and Internet connection for performing telerehabilitation exercise programs, and had physical and cognitive abilities to exercise independently through the provided remote program.
The exclusion criteria for the study subjects were as follows: radiating pain in the arm or neurological symptoms in the past, neck rotation less than 20 degrees [23], fractures and dislocations of the shoulder joint [24], and history of shoulder surgery [25].
To calculate the sample size needed for this study, an effect size of 1.07 was determined through the average difference in the ROM of lateral flexion of the neck between the EG and the CG in the study on the effect of upper-extremity nerve mobilization on the neck ROM [26]. To satisfy this effect, after setting the significance level to 0.05 and the power to 0.80, the G*Power 3.1 [27] program resulted in 24 results, and a dropout rate of 20% was considered. Therefore, 30 people were selected as the number of subjects.
PROCEDURE:
This study used online promotional posts to recruit participants. Thirty subjects who satisfied the inclusion criteria and completed the baseline assessments were randomly selected using a lottery method and classified into one of the 2 groups: an EG (n=15), or a CG (n=15). All assessments were conducted by 2 physiotherapists who were blinded. Before the experiment, the researcher directly educated both groups on the telerehabilitation exercise program. Each group was allowed to participate in the exercise program by up to 6 people at a set time. During the experiment, 1 subject in the EG and 3 subjects in the CG dropped out because they did not complete the exercise session, so 14 people in the EG and 12 people in the CG were analyzed in the post-test.
During the exercise, the researcher performed the exercise in real time with the participants, and a supplementary video was produced to inform the participants of the exact motion and exercise time and number. This video was divided into training and educational videos. The educational video was produced by composing the correct exercise method and the wrong exercise method to ensure that the participants perform the correct exercise (Figure 1A, 1B). The training video was produced to inform the participants not only of the exact movements but also of the time and number of times (Figure 2A, 2B).
After undergoing the 4-week telerehabilitation exercise program, evaluation parameters of the subject, such as PPT for pain, ROM of the neck and muscle activity for physical function, and pectoralis minor muscle length index for posture were measured, and satisfaction with the telerehabilitation exercise program was assessed with the questionnaires.
All groups performed the telerehabilitation exercise program 3 times a week for 4 weeks. While the EG performed the shrug exercise and SUENM for 14 min, the CG performed the shrug exercise for 7 min. The period of participation in the experiment was from May to June 2021, when South Korea’s social distancing was in the second stage (Figure 3).
SELF-UPPER-EXTREMITY NERVE MOBILIZATION (SUENM):
After subjects spread their legs shoulder-width apart and the arm designated as a rounded shoulder was rotated 90° externally and abducted by 60° along the coronal plane. After that, the elbow was straightened, and the wrist extended while depressing the shoulder and bending the neck to the opposite side until nerve tension was felt [28]. Subjects performed 3 sets of 6 repetitions of 10 s each, resting for 10 s between each exercise and 30 s between each set, for a total of 7 min [29,30].
SHRUG EXERCISE:
The subject spread their legs shoulder-width apart and then externally rotated both arms at 90° and 30° abduction along the coronal plane. Then, they would shrug their shoulders as close as possible to their ears. The subjects performed 3 sets of 12 repetitions lasting 5 s each, resting for 5 s between each exercise and 30 s between each set, for a total of 7 min [11].
PECTORALIS MINOR LENGTH INDEX: Digital calipers (Winwin Industrial Co., Fuzhou, China) were used to measure the length of the pectoralis minor muscle, which causes RSP. The subjects laid both arms in a neutral position and neatly next to the torso in a supine position during the measurement. Then, the vertical distance between the back side of the subject’s acromion and the table was measured 3 times and the higher average value for both shoulders was used for analysis [12]. If the value was 2.5 cm or more, rounded shoulder was diagnosed [22]. The arm with the higher index among the left and right arms was defined as the rounded shoulder arm, and SUENM was performed on the arm.
RANGE OF MOTION OF THE NECK: To measure the neck’s ROM, a cervical range of motion instrument (Performance Attainment Associates, Inc., St. Paul, MN, USA) was used. The subject sat in a chair with the pelvis in a neutral position during the measurement, and the hip and knee joints flexed by 90°. After wearing the cervical ROM instrument on the head, the measurer asked the subject to perform active movements comprising neck flexion, extension, right rotation, left rotation, right lateral flexion, and left lateral flexion in sequence [31]. The measurements were performed 3 times in each direction, and the average value was used for analysis.
PRESSURE PAIN THRESHOLD: A digital pressure algometer (JTECH Medical Industries, Inc., Midvale, UT, USA) with a catheter diameter of 1 cm2 was used to measure the PPT of the upper trapezius. The measurer placed the tip of the algometer vertically in the middle of the upper trapezius between the 7th cervical vertebra and the acromion and increased the pressure at a constant rate of 1 N/cm2. Subjects were instructed to say ‘it hurts’ when they felt the pressure as pain and then were measured. Measurement was performed 3 times on the arm designated to be with a rounded shoulder, resting for 30 s between each measurement, and the average value was used [32].
MUSCLE ACTIVITY: Surface electromyography (EMG) (Noraxon, Inc., Scottsdale, Arizona, USA) was used to measure the muscle activity. As the muscles to be measured, we selected the levator scapula, which is a downward rotator of the scapula, and upper trapezius, serratus anterior, and lower trapezius muscles, which are upward rotator muscles [11].
For normalization of EMG data, each muscle’s maximal voluntary isometric contraction (MVIC) was measured using a manual muscle test. When measuring MVIC, the subject was encouraged to contract the maximum isometric contraction for 5 s, and the measurement was repeated 3 times. There was a break of 30 s between each measurement, and 1 min between measurements of each muscle. For each measurement, the average value for 3 s, excluding the first and last seconds, was used. The measurement procedure was as follows [33]:
The activity of the scapula muscle selected as a rounded shoulder was measured when the shoulder was flexed at 60°, 90°, and 120° in the scapular plane. To reduce measurement error, the examiner used a goniometer to check the subject’s scapular plane and induced shoulder flexion angles of 60°, 90°, and 120° using a horizontal bar. During measurement, the subjects spread their legs shoulder-width apart, flexed their shoulders along the scapula until their second finger touched the horizontal bar, and held it for 5 s. Measurements were performed 3 times at each angle, and the average value for 3 s excluding the first and last seconds was used [23].
The collected data were analyzed using electromyography software (MyoResearch Master 1.08 XP). The sampling rate of the measured data was set to 2000 Hz, and the frequency bandwidth was set to 80–250 Hz [34]. After the measured EMG signal of the muscle was rectified, a value close to the actual output value of the EMG signal was processed using the root-mean-square method. The signal collected from each muscle was normalized as a percentage of the MVIC value.
SATISFACTION WITH THE TELEREHABILITATION EXERCISE PROGRAM: A visual analog scale and multiple-choice narrative questions were used to survey the satisfaction of the telerehabilitation exercise program. Satisfaction with the telerehabilitation exercise program, image clarity, and sound quality was measured using the visual analog scale, and the equipment used when using the remote program was investigated using multiple-choice items. The pros and cons of the telerehabilitation exercise program were analyzed using descriptive questions [35].
STATISTICAL ANALYSIS:
This study was performed using SPSS version 25.0 statistical software (IBM, Chicago, IL, USA). Except for the electromyography data, all data were tested for normality using the Shapiro-Wilk test, and it was confirmed that they were normally distributed. The EMG data used for the analysis satisfied the assumption of a normal distribution, with skewness −0.524 to 1.851 and kurtosis −1.815 to 4.597 [36]. The chi-square test and independent sample t test were performed to confirm the homogeneity between the groups. A paired-sample t test was used to compare the difference between the before and after effects according to the intervention method within each group, and an independent sample t test was performed to compare the differences between groups. The statistical significance level for all data was set at P<0.05.
Results
PECTORALIS MINOR LENGTH INDEX:
In the pectoralis minor muscle length index, the EG significantly decreased from 48.89 mm before the intervention to 38.13 mm after the intervention (P<0.05), and the CG also significantly decreased from 51.20 mm before the intervention to 44.00 mm after the intervention (P<0.05) (Table 2).
RANGE OF MOTION OF NECK:
Changes in flexion, bilateral rotation, and left lateral flexion of the neck were not significant in the before and after changes in the ROM of the neck according to the intervention method. However, the CG did not show any significant changes in extension and right lateral flexion, whereas the EG showed a significant increase after the intervention compared with before the intervention (P<0.05). Also, there was a significant difference in the amount of change before and after the intervention between the groups (P<0.05) (Table 3).
PRESSURE PAIN THRESHOLD:
In the pressure pain threshold, the EG significantly increased from 24.75 before the intervention to 29.35 after the intervention, and there was no significant difference in the CG. There was a significant difference in the amount of change before and after the intervention (P<0.05), and the EG had a significantly increased PPT compared to the CG (P<0.05) (Table 4).
CHANGES OF MUSCLE ACTIVITY:
The change in muscle activity according to the angle of the serratus anterior and lower trapezius muscles did not differ between the EG and the CG before and after the experiment according to the intervention method. The changes in muscle activity of the levator scapula and upper trapezius in the EG showed significant differences before and after the experiment at 60°, 90°, and 120° (P<0.05), and there was no significant difference in the CG. A significant difference was also shown in the comparison between groups before and after the experiment (P<0.05) (Table 5).
SURVEY ON SATISFACTION OF TELEREHABILITATION EXERCISE PROGRAM:
The satisfaction of the telerehabilitation exercise program is shown in Table 6. The items of time-saving, audio clarity of the video, and communication with supervisor showed the highest grade (>9/10), the image clarity of the video, exercise content, intention to re-engage, exercise recommendation, and exercise effect items showed high ratings (>7/10) and showed the lowest grade (>6/10) in the self-exercise category.
STATUS OF DEVICES USED WHEN USING REMOTE PROGRAMS:
The devices used when using the remote program are as follows: As equipment for watching video, smartphones were the most commonly used (11 people, 42.3%), followed by laptops (8 people, 30.8%), tablets (4 people, 15.4%), and personal computers (3 people, 11.5%). Regarding the equipment for listening to sound, built-in speakers were the most common (16 people, 61.5%), followed by earphones (9 people, 34.6%), and headsets (1 person, 3.8%). Regarding the equipment for using a microphone, the built-in microphone was most commonly used (16 people, 61.5%), followed by earphones (9 people, 4.6%) and headset (1 person, 3.8%) (Table 7).
ADVANTAGES AND DISADVANTAGES OF TELEREHABILITATION EXERCISE PROGRAM:
The answers to the question of being free to describe the advantages and disadvantages of telerehabilitation are as follows: As an advantage of the telerehabilitation exercise program, ‘Irrespective of time and place’ was cited by 26 people (100%), and as a disadvantage, ‘it is difficult to know whether I am taking the correct action’ was cited by 18 people (69.2%), ‘motivation of exercise is low’ was reported by 3 people (11.5%), ‘I am reluctant to expose my privacy’ was reported by 1 person (3.8%), ‘I have difficulty in bringing communication equipmen’ was reported by 1 person (3.8%), ‘No’ was reported by 3 people (11.5%) (Table 8).
Discussion
Our study was conducted to assess the effect of the SUENM telerehabilitation exercise program on patients with RSP in 2021, during the COVID-19 pandemic restrictions in South Korea. Results of this study showed that telerehabilitation exercise program effectively increased the PPT of the upper trapezius and neck ROM and reduced the muscle activity of the levator scapula and upper trapezius during shoulder flexion in subjects with RSP. In the satisfaction survey, participants indicated space-time freedom as an advantage of the telerehabilitation exercise program and reported difficulty in correctly performing the exercises as a disadvantage.
According to the World Confederation of Physical Therapy, the importance of telerehabilitation to improve safety and access to rehabilitation in the context of COVID-19 should be emphasized [21]. Pehlivan et al [2] reported that the telerehabilitation exercise program for COVID-19 patients had a significant effect on improving respiratory function, quality of life, and physical function, and that it is an exercise program that can be applied in real life only when it is carried out without special equipment. Hyun and Cho [4] reported that non-face-to-face home Pilates exercise had a significant effect on relieving pain and improving physical strength for postpartum women. They showed a significant effect on neck pain relief and physical function improvement when telerehabilitation exercise programs were applied to RSP subjects, which is consistent with the mediating effect of existing face-to-face neural mobility [26,37]. In addition, telerehabilitation program exercise is possible without special equipment, so it can be easily applied in real life. We found that the transition from existing face-to-face treatment to telerehabilitation exercise programs was successful.
The EG experienced significantly improved ROM of extension and right-side bending of the neck compared to the CG. According to previous studies, shortening of the scalene muscle due to RSP compresses the brachial plexus, thereby lowering the physiological flow of nerves and aggravating the limitation of the ROM of the neck [9,38]. It has been reported that upper-extremity neural mobilization improves the neck’s ROM by inducing maximum tension in the brachial plexus and nerve roots of the 5th, 6th, and 7th cervical vertebrae, thereby increasing nerve conduction and blood flow [29]. Previous studies reported that the application of upper-extremity neural mobilization in patients with cervical pain provided significant neck pain relief and improvement of ROM [26,37]. These results show that SUENM applied to the EG affected the brachial plexus of the cervical and improved the ROM.
In the EG of the present study, the PPT increased significantly compared to the CG. According to a previous study, the mechanical sensitivity of the nerve and the PPT were negatively correlated, and the lower the nerve flexibility, the higher the tender point of the upper trapezius muscle [39]. Another study reported that upper-extremity neural mobilization effectively alleviates neck and shoulder pain by reducing the mechanical sensitivity of nerves in patients with chronic neck and shoulder pain [19,20,40]. Thus, it is demonstrated that SUENM in the present study increased the PPT of the upper trapezius by reducing the mechanical sensitivity of the nerve.
In this study, the muscle activity of the upper trapezius muscle was significantly reduced in the EG at 90° and 120° of shoulder flexion compared to the CG, and in the comparison before and after intervention, EG showed a significant effect on the reduction of muscle activity of the levator scapula. At shoulder flexion 90° and above, the shortening of the levator scapula due to RSP limits the upward rotation of the scapula, resulting in excessive scapular elevation as a compensatory action [22,41]. Excessive activation of the upper trapezius muscle due to scapular elevation creates a tender point in the fascia and affects the scapulohumeral rhythm, which can cause secondary shoulder impingement syndrome [42,43]. Previous studies reported that the application of upper-extremity neural mobilization in breast cancer surgery patients had a significant effect on the recovery of shoulder ROM and upper-limb function [44]. These results indicate that SUENM is effective in reducing the muscle activity of the levator scapula and upper trapezius during shoulder flexion, leading to the recovery of upper-limb function, thereby relieving the tender point of the upper trapezius.
There was no significant difference between the 2 groups in the pectoralis minor length index, but the decrease was greater in the EG. According to previous studies, the pectoralis minor muscle is connected to the biceps brachii muscle by fascia. It has been reported that shortening of the biceps brachii muscle is positively correlated with shortening of the pectoralis minor muscle [45]. Another study reported that when upper-extremity nerve mobilization was applied to the biceps brachii, it increased nerve axon transport and muscle blood flow to improve the flexibility of nerves and muscle tissue and had an effect on movement recovery [46]. It is thought that the SUENM performed in this study increased the flexibility of the biceps brachii and further affected the pectoralis minor muscle connected to the fascia, thereby decreasing the pectoralis minor muscle length index.
The participants in this study mainly used smartphones and laptops to use the remote program ZOOM, and they primarily used built-in speakers, microphones, and earphones to communicate with the supervisor during the telerehabilitation exercise programs. After the intervention, the 2 groups were satisfied with the clarity and sound quality, time-saving, contents of the exercise, and the exercise effect. In addition, although all participants indicated that an advantage of the telerehabilitation exercise program is that it is not limited by time and place, and indicated that the main disadvantages were that it is difficult to know whether the correct exercise movements were being performed, and that they had low motivation to exercise. According to previous studies, factors such as lack of Internet devices, poor Internet connection, age, cognition, and education level are barriers to entry into telerehabilitation exercise programs, and the need for a satisfaction survey was argued to verify the effect of telerehabilitation exercise programs [47]. Another previous study found that participants in a telerehabilitation exercise program were satisfied with the clarity of image and sound quality, exercise effect, and time-saving [35]. This is consistent with the present study results, and supports the effectiveness of telerehabilitation exercise programs. In addition, when using the telerehabilitation exercise program in this study, the device survey item can be used as a study to lower the entry barrier of the telerehabilitation exercise program in the future.
For further development of telerehabilitation exercise programs, the shortcomings of this study should be identified and improved. In this study, a physical therapist guided the exercise in real time and used supplementary video to guide the participants to accurately perform movements. However, it is difficult to get accurate guidance from a physical therapist because most of the participants were not familiar with exercise or the online environment. Previous studies have shown that errors in online environments, such as Internet problems, have a negative effect on telerehabilitation exercise programs [48]. Therefore, in future studies, participants need to be educated in an online environment before the experiment, and consider ways to give feedback on exercise to participants.
The limitations of this study are as follows: First, the study subjects are limited to 20–40 years old, making it difficult to generalize to all age groups. Second, when measuring the length index of the pectoralis minor muscle causing RSP, only the vertical distance between the back of the acromion and the table was classified in the supine position, without considering other variables. Therefore, various types of scapular misalignment other than the length of the pectoralis minor may have influenced the dependent variable. Third, it is difficult to generalize the study results because the number of test subjects was insufficient, and the proportions of the arms selected for rounded shoulders in the 2 groups differed. Forth, it is difficult to know whether the participant was performing the correct motion during the telerehabilitation exercise program. Therefore, a follow-up study is necessary to take these limitations into consideration and use all age groups as the subjects, further subdivide the scapula misalignment when measuring RSP, and equalize the proportion of arms selected. In addition, it is necessary to user a method assuring that participants accurately perform telerehabilitation exercises.
Conclusions
The findings support those from recent studies on real-time telerehabilitation physiotherapy exercise programs. However, long-term controlled studies are required to develop evidence-based protocols for implementing and evaluating clinical outcomes of remote physiotherapy programs.
Figures
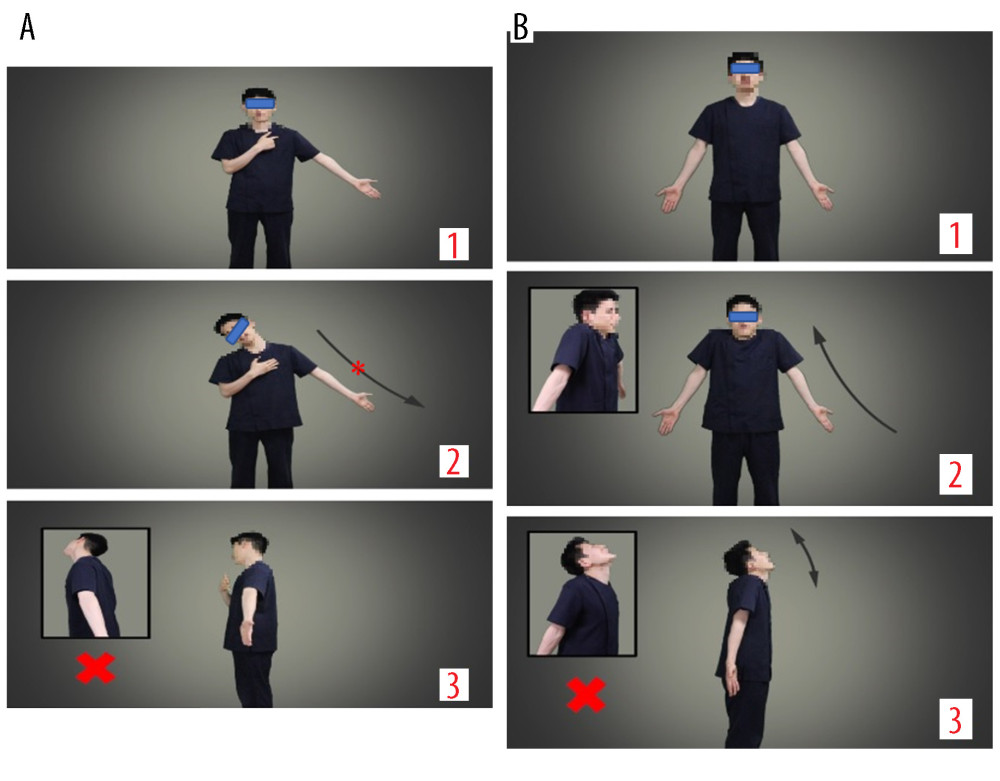 Figure 1. (A) Screenshot of educational video for self-upper-extremity neural mobilization. 1. Starting position; 2. End positton; 3. Wrong position. * Black arrows indicate the stretching direction of arm. (B) Screenshot of educational video for shrug exercise. 1. Starting position; 2. End positton; 3. Wrong position.
Figure 1. (A) Screenshot of educational video for self-upper-extremity neural mobilization. 1. Starting position; 2. End positton; 3. Wrong position. * Black arrows indicate the stretching direction of arm. (B) Screenshot of educational video for shrug exercise. 1. Starting position; 2. End positton; 3. Wrong position. 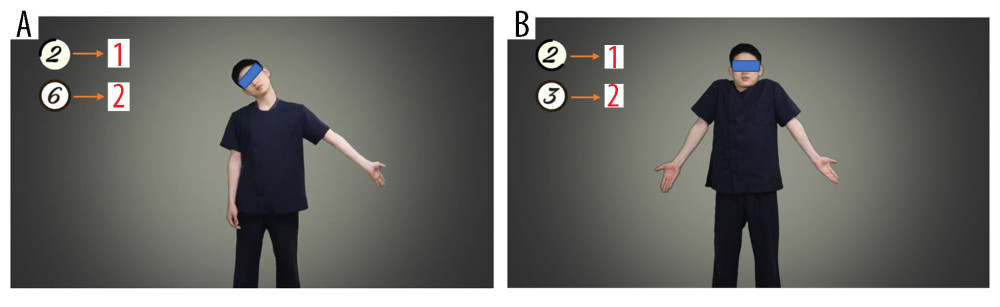 Figure 2. (A) Screenshot of training video for self-upper-extremity neural mobilization. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions. (B) Screenshot of educational video for shrug exercise. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions.
Figure 2. (A) Screenshot of training video for self-upper-extremity neural mobilization. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions. (B) Screenshot of educational video for shrug exercise. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions. 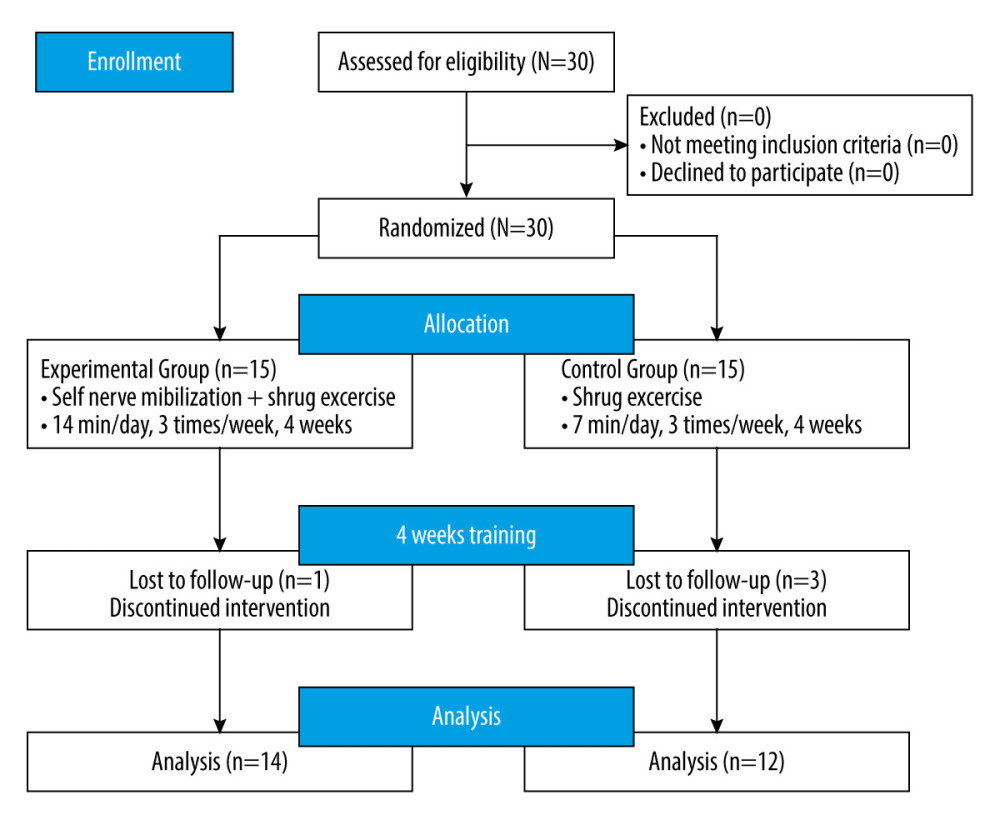 Figure 3. Research procedure.
Figure 3. Research procedure. Tables
Table 1. General characteristic of subjects.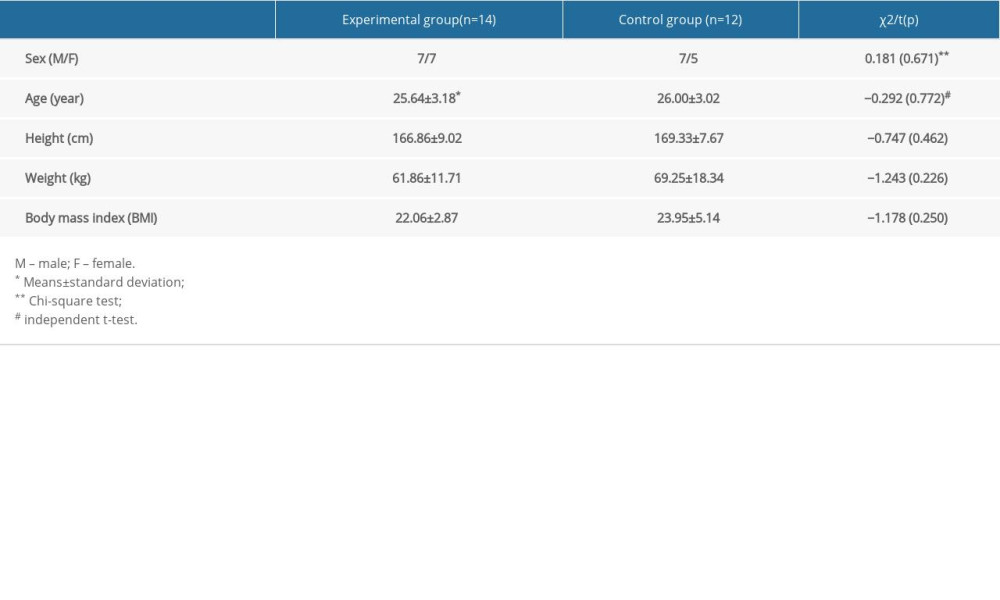 Table 2. Changes of pectoralis minor length index according to intervention.
Table 2. Changes of pectoralis minor length index according to intervention.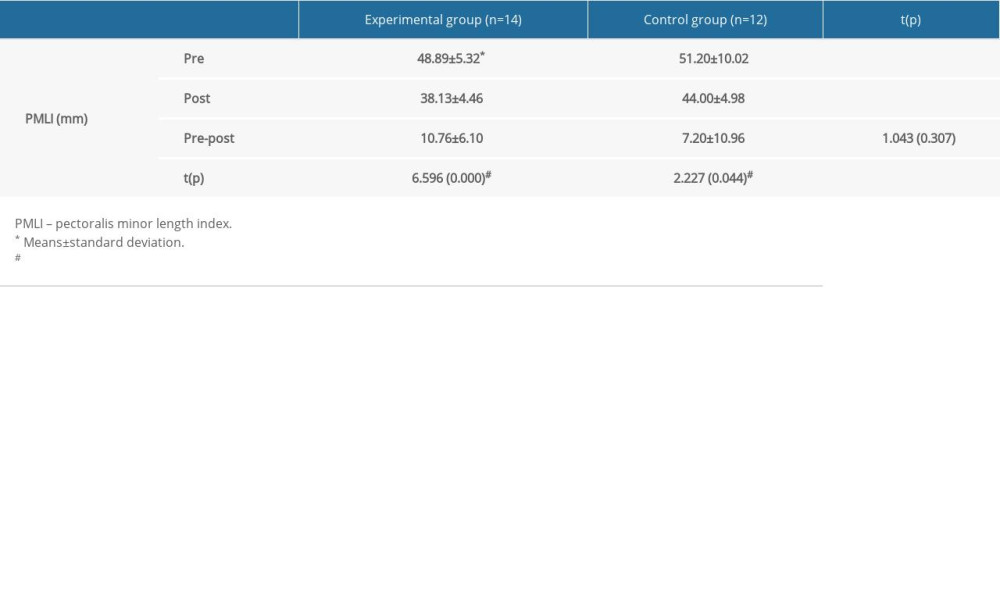 Table 3. Changes of neck range of motion according to intervention.
Table 3. Changes of neck range of motion according to intervention.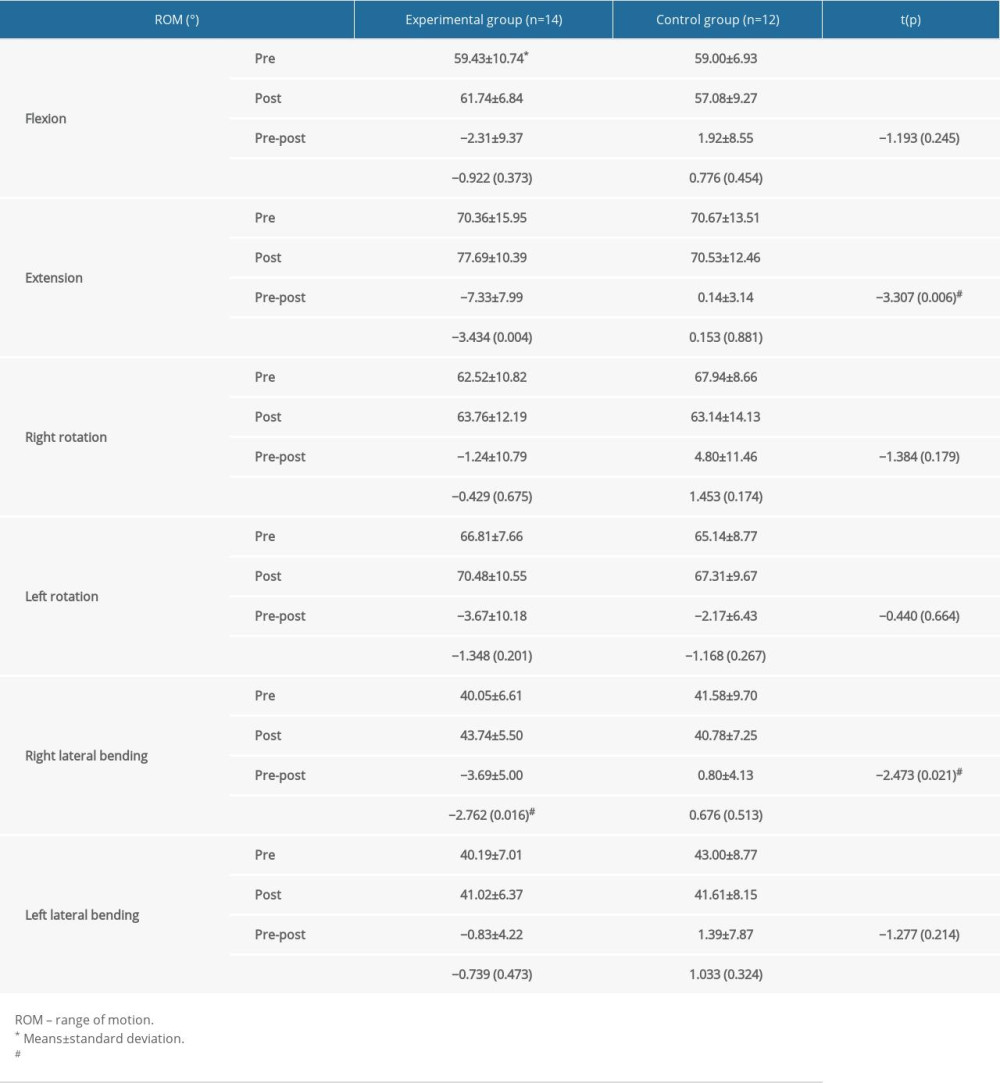 Table 4. Change of pressure pain threshold according to intervention.
Table 4. Change of pressure pain threshold according to intervention.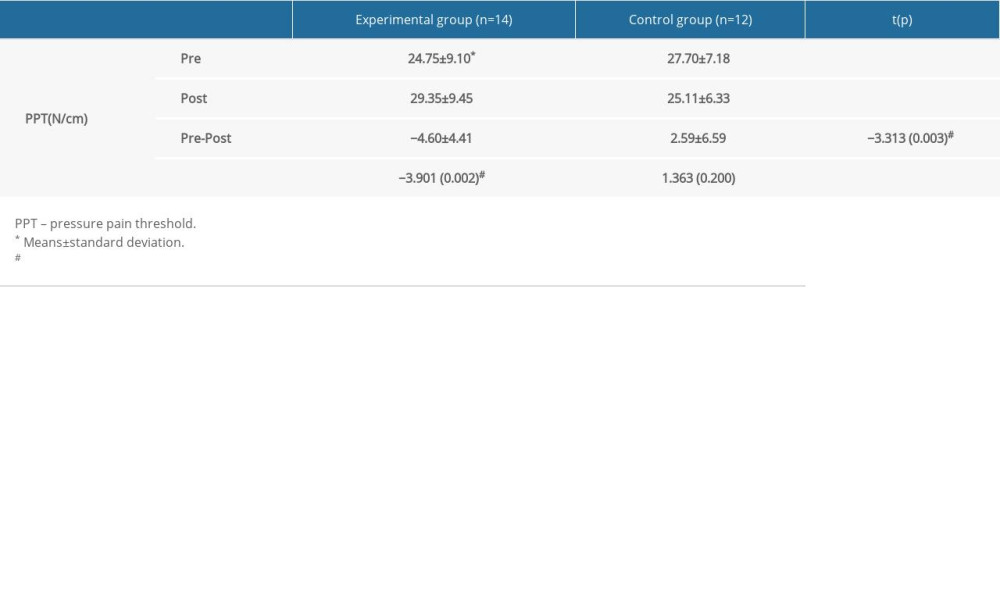 Table 5. Change in muscle activity.
Table 5. Change in muscle activity.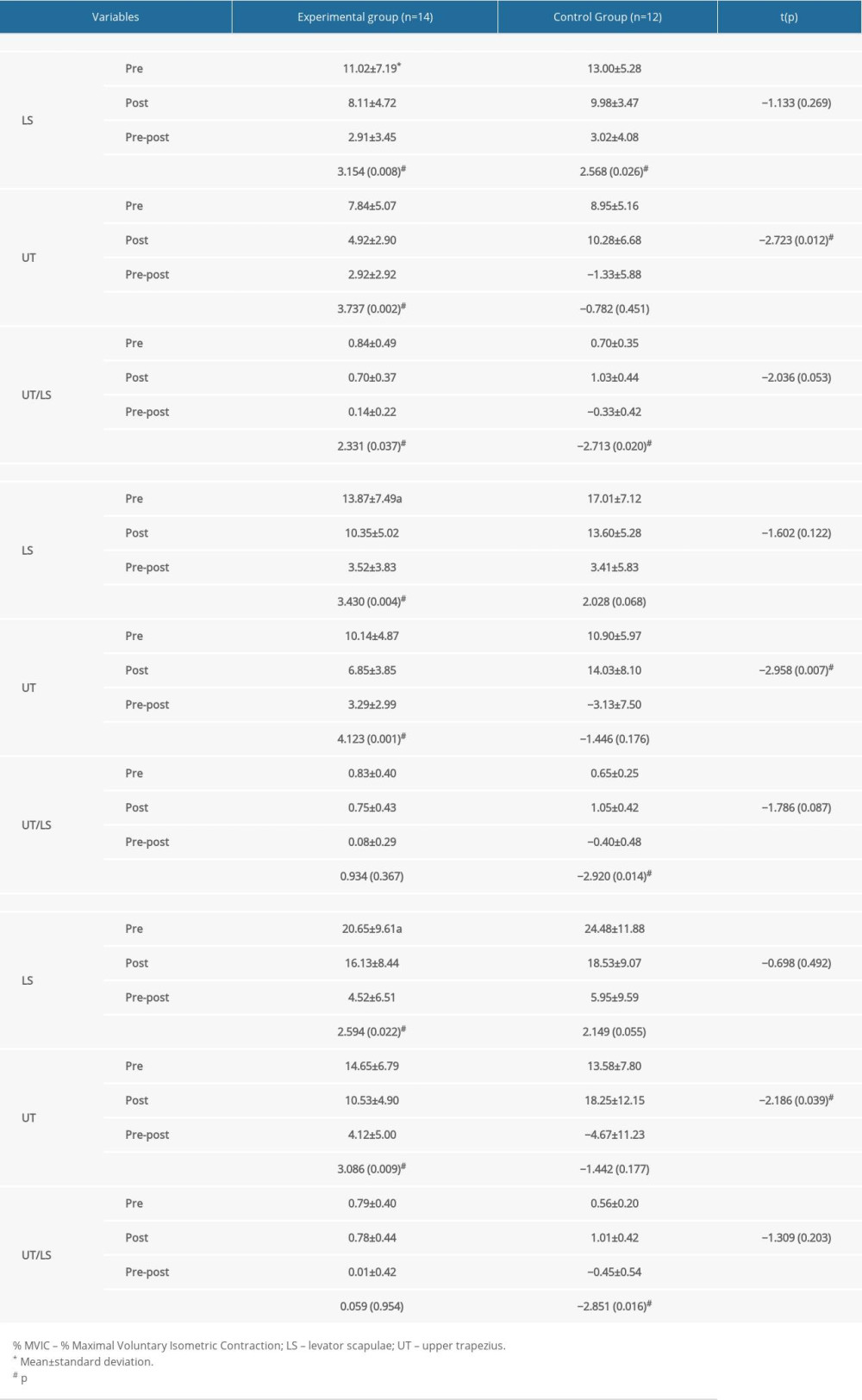 Table 6. Satisfaction with telerehabilitation program.
Table 6. Satisfaction with telerehabilitation program.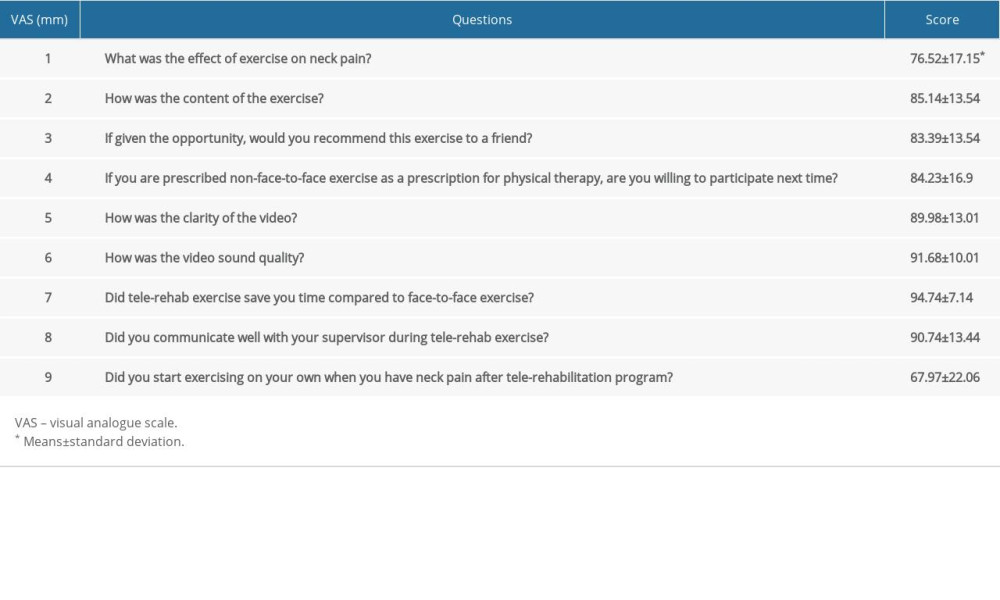 Table 7. Status of devices used when participating in telerehabilitation program.
Table 7. Status of devices used when participating in telerehabilitation program.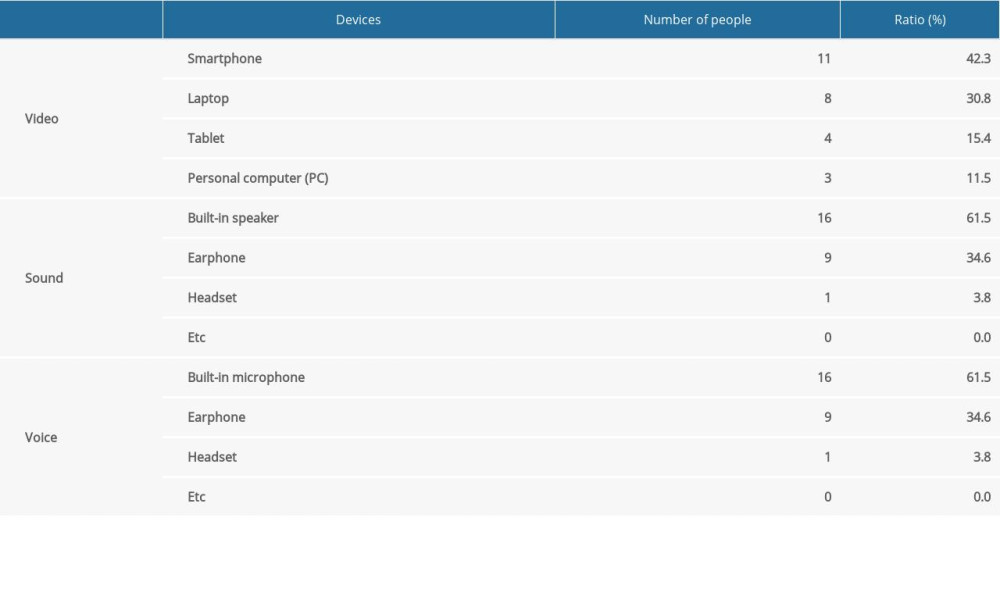 Table 8. Advantages and disadvantages of telerehabilitation.
Table 8. Advantages and disadvantages of telerehabilitation.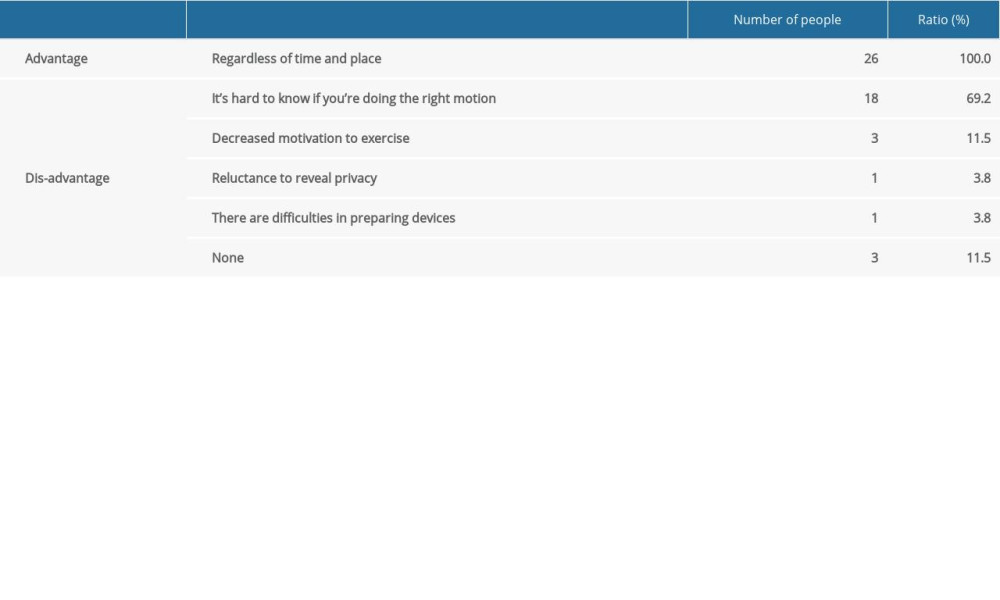
References
1. Kim YUntact and exercise science accelerated by coronavirus infection-19 (COVID-19): Exercise Science, 2021; 129-30 Available at: [in Korean].https://www.ksep-es.org/upload/pdf/es-30-2-129.pdf
2. Pehlivan E, Palali I, Atan SG, The effectiveness of POST-DISCHARGE telerehabilitation practices in COVID-19 patients: Tele-COVID study-randomized controlled trial: Ann Thorac Med, 2022; 17(2); 110-17
3. Ghram A, Briki W, Mansoor H, Al-Mohannadi AS, Home-based exercise can be beneficial for counteracting sedentary behavior and physical inactivity during the COVID-19 pandemic in older adults: Postgrad Med, 2021; 133(5); 469-80
4. Hyun A, Cho JEffect of 8 weeks un-tact pilates home training on body composition, abdominal obesity, pelvic tilt and strength, back pain in overweight women after childbirth: Exercise Science, 2021; 61-69 Available at: [in Korean].https://ksep-es.org/upload/pdf/es-30-1-61.pdf
5. Kim J-Y, Lee D-W, Jeong M-BEffect of a telerehabilitation exercise program on the gait, knee function and quality of life in patients with knee osteoarthritis: Journal of the Korean Society of Physical Medicine, 2020; 15(1); 143-52 [in Korean]
6. Vieira A, Pinto A, Garcia B, Telerehabilitation improves physical function and reduces dyspnoea in people with COVID-19 and post-COVID-19 conditions: A systematic review: J Physiother, 2022; 68(2); 90-98
7. Kim T-H, Jee H-J, Bae C-W, Choi S-ASocial distancing in COVID-19: What are the implications for musculoskeletal problems and the quality of life?: The Journal of Korean Physical Therapy, 2021; 33(2); 84-90 [in Korean]
8. Mutz M, Gerke M, Sport and exercise in times of self-quarantine: How Germans changed their behaviour at the beginning of the COVID-19 pandemic: Int Rev Sociol Sport, 2021; 56(3); 305-16
9. Yang Y, Hur J-G, Kim H-HA review on VDT syndrome of work-related musculoskeletal disorders: Journal of Korean Physical Therapy Science, 2004; 11(4); 20-28 [in Korean]
10. Kim C-S, Kim SGThe effect of strengthening on scapular stabilizer muscles for the rounded shoulders: PNF and Movement, 2013; 11(2); 49-56 [in Korean]
11. Lee J-H, Cynn H-S, Choi W-J, Various shrug exercises can change scapular kinematics and scapular rotator muscle activities in subjects with scapular downward rotation syndrome: Hum Mov Sci, 2016; 45; 119-29
12. Park S-K, Park J-M, Lee J-HEffects of a push-up plus exercise program on scapular position and muscle activity in individuals with rounded shoulder posture: The Journal of Korean Physical Therapy, 2010; 22(5); 1-8 [in Korean]
13. Sheikhhoseini R, Shahrbanian S, Sayyadi P, O’Sullivan K, Effectiveness of therapeutic exercise on forward head posture: A systematic review and meta-analysis: J Manipulative Physiol Ther, 2018; 41(6); 530-39
14. McQuade KJ, Borstad J, de Oliveira AS, Critical and theoretical perspective on scapular stabilization: What does it really mean, and are we on the right track?: Phys Ther, 2016; 96(8); 1162-69
15. Kostopoulos D, Treatment of carpal tunnel syndrome: A review of the non-surgical approaches with emphasis in neural mobilization: J Bodyw Mov Ther, 2004; 8(1); 2-8
16. Seok J-h, Kim T-h, The effects of scapular alignment exercise and nerve mobilization on pain and muscle activity in subjects with scapular depression alignment: Journal of Musculoskeletal Science and Technology, 2020; 4(2); 58-65
17. Basson A, Olivier B, Ellis R, The effectiveness of neural mobilization for neuromusculoskeletal conditions: A systematic review and meta-analysis: J Orthop Sports Phys Ther, 2017; 47(9); 593-615
18. Ellis RF, Hing WA, Neural mobilization: A systematic review of randomized controlled trials with an analysis of therapeutic efficacy: J Man Manip Ther, 2008; 16(1); 8-22
19. Beltran-Alacreu H, Jiménez-Sanz L, Carnero JF, La Touche R, Comparison of hypoalgesic effects of neural stretching vs neural gliding: A randomized controlled trial: J Manipulative Physiol Ther, 2015; 38(9); 644-52
20. Calvo-Lobo C, Unda-Solano F, López-López D, Is pharmacologic treatment better than neural mobilization for cervicobrachial pain? A randomized clinical trial: Int J Med Sci, 2018; 15(5); 456
21. Turolla A, Rossettini G, Viceconti A, Musculoskeletal physical therapy during the COVID-19 pandemic: Is telerehabilitation the answer?: Phys Ther, 2020; 100(8); 1260-64
22. Sahrmann S: Diagnosis and treatment of movement impairment syndromes, 2001, Mosby
23. Kang M-H, Choi J-Y, Oh J-s, Effects of crossed brassiere straps on pain, range of motion, and electromyographic activity of scapular upward rotators in women with scapular downward rotation syndrome: PM R, 2015; 7(12); 1261-68
24. Asheghan M, Aghda AK, Hashemi E, Hollisaz M, Investigation of the effectiveness of acupuncture in the treatment of frozen shoulder: Mater Sociomed, 2016; 28(4); 253
25. Wang SS, Normile SO, Lawshe BT, Reliability and smallest detectable change determination for serratus anterior muscle strength and endurance tests: Physiother Theory Pract, 2006; 22(1); 33-42
26. Kim D-G, Chung SH, Jung HB, The effects of neural mobilization on cervical radiculopathy patients’ pain, disability, ROM, and deep flexor endurance: J Back Musculoskelet Rehabil, 2017; 30(5); 951-59
27. Faul F, Erdfelder E, Buchner A, Lang A-G, Statistical power analyses using G* Power 3.1: Tests for correlation and regression analyses: Behav Res Methods, 2009; 41(4); 1149-60
28. Santana H, Fernandes de Oliveira I, Medrado A, Nunes S, Neurodynamic mobilization and peripheral nerve regeneration: A narrative review: Int J Neurorehabil, 2015; 2(2); 1-7
29. Butler DS: The sensitive nervous system, 2000; 432, Noigroup publications
30. Paquette P, Higgins J, Gagnon DH, Peripheral and central adaptations after a median nerve neuromobilization program completed by individuals with carpal tunnel syndrome: An exploratory mechanistic study using musculoskeletal ultrasound imaging and transcranial magnetic stimulation: J Manipulative Physiol Ther, 2020; 43(6); 566-78
31. Audette I, Dumas J-P, Côté JN, De Serres SJ, Validity and between-day reliability of the cervical range of motion (CROM) device: J Orthop Sports Phys Ther, 2010; 40(5); 318-23
32. Celenay ST, Kaya DO, Akbayrak T, Cervical and scapulothoracic stabilization exercises with and without connective tissue massage for chronic mechanical neck pain: A prospective, randomised controlled trial: Man Ther, 2016; 21; 144-50
33. Castelein B, Cagnie B, Parlevliet T, Optimal normalization tests for muscle activation of the levator scapulae, pectoralis minor, and rhomboid major: An electromyography study using maximum voluntary isometric contractions: Arch Phys Med Rehabil, 2015; 96(10); 1820-27
34. Song C, Seo D-kDevelopment of EMG-triggered functional electrical stimulation device for upper extremity bilateral movement training in stroke patients: Feasibility and pilot study: Physical Therapy Rehabilitation Science, 2021; 10(3); 374-78 [in Korean]
35. Russell TG, Buttrum P, Wootton R, Jull GA, Rehabilitation after total knee replacement via low-bandwidth telemedicine: The patient and therapist experience: J Telemed Telecare, 2004(1 Suppl); 85-87
36. West SG, Finch JF, Curran PJ: Structural equation models with nonnormal variables: Problems and remedies, 1995
37. Rodríguez-Sanz D, López-López D, Unda-Solano F, Effects of median nerve neural mobilization in treating cervicobrachial pain: A randomized waiting list-controlled clinical trial: Pain Pract, 2018; 18(4); 431-42
38. Bae S-S, Kim S-H, Kim S-S, Treatment of forward head posture and shoulder instability: PNF and Movement, 2007; 5(2); 1-10 [in Korean]
39. Yılmaz S, Taş S, Yılmaz ÖT, Comparison of median nerve mechanosensitivity and pressure pain threshold in patients with nonspecific neck pain and asymptomatic individuals: J Manipulative Physiol Ther, 2018; 41(3); 227-33
40. Basson A, Olivier B, Ellis R, The effectiveness of neural mobilization for neuromusculoskeletal conditions: A systematic review and meta-analysis: J Orthop Sports Phys Ther, 2017; 47(9); 593-615
41. Neumann DA: Kinesiology of the musculoskeletal system-e-book: Foundations for rehabilitation, 2016, Elsevier Health Sciences
42. Lewis JS, Wright C, Green A, Subacromial impingement syndrome: The effect of changing posture on shoulder range of movement: J Orthop Sports Phys Ther, 2005; 35(2); 72-87
43. Lin J-j, Hanten WP, Olson SL, Functional activity characteristics of individuals with shoulder dysfunctions: J Electromyogr Kinesiol, 2005; 15(6); 576-86
44. de la Rosa Díaz I, Lacomba MT, Téllez EC, del Campo Gómez-Rico CD, Ortega CG, Accessory joint and neural mobilizations for shoulder range of motion restriction after breast cancer surgery: A pilot randomized clinical trial: J Chiropr Med, 2017; 16(1); 31-40
45. Choi S-a, Cynn H-s, Lee J-hRelationships between rounded shoulder posture and biceps brachii muscle length, elbow joint angle, pectoralis muscle length, humeral head anterior translation, and glenohumeral range of motion: Physical Therapy Korea, 2017; 24(2); 48-57 [in Korean]
46. Kim M-K, Cha H-G, Ji SG, The initial effects of an upper extremity neural mobilization technique on muscle fatigue and pressure pain threshold of healthy adults: A randomized control trial: J Phys Ther Sci, 2016; 28(3); 743-46
47. Vieira AGDS, Pinto ACPN, Garcia BMSP, Telerehabilitation improves physical function and reduces dyspnoea in people with COVID-19 and post-COVID-19 conditions: A systematic review: J Physiother, 2022; 68(2); 90-98
48. Tsai LLY, McNamara RJ, Dennis SM, Satisfaction and experience with a supervised home-based real-time videoconferencing telerehabilitation exercise program in people with chronic obstructive pulmonary disease (COPD): Int J Telerehabil, 2016; 8(2); 27
Figures
 Figure 1. (A) Screenshot of educational video for self-upper-extremity neural mobilization. 1. Starting position; 2. End positton; 3. Wrong position. * Black arrows indicate the stretching direction of arm. (B) Screenshot of educational video for shrug exercise. 1. Starting position; 2. End positton; 3. Wrong position.
Figure 1. (A) Screenshot of educational video for self-upper-extremity neural mobilization. 1. Starting position; 2. End positton; 3. Wrong position. * Black arrows indicate the stretching direction of arm. (B) Screenshot of educational video for shrug exercise. 1. Starting position; 2. End positton; 3. Wrong position. Figure 2. (A) Screenshot of training video for self-upper-extremity neural mobilization. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions. (B) Screenshot of educational video for shrug exercise. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions.
Figure 2. (A) Screenshot of training video for self-upper-extremity neural mobilization. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions. (B) Screenshot of educational video for shrug exercise. 1. The number in the circle shows exercise time; 2. The number in the circle shows number of exercise repetitions. Figure 3. Research procedure.
Figure 3. Research procedure. Tables
 Table 1. General characteristic of subjects.
Table 1. General characteristic of subjects. Table 2. Changes of pectoralis minor length index according to intervention.
Table 2. Changes of pectoralis minor length index according to intervention. Table 3. Changes of neck range of motion according to intervention.
Table 3. Changes of neck range of motion according to intervention. Table 4. Change of pressure pain threshold according to intervention.
Table 4. Change of pressure pain threshold according to intervention. Table 5. Change in muscle activity.
Table 5. Change in muscle activity. Table 6. Satisfaction with telerehabilitation program.
Table 6. Satisfaction with telerehabilitation program. Table 7. Status of devices used when participating in telerehabilitation program.
Table 7. Status of devices used when participating in telerehabilitation program. Table 8. Advantages and disadvantages of telerehabilitation.
Table 8. Advantages and disadvantages of telerehabilitation. Table 1. General characteristic of subjects.
Table 1. General characteristic of subjects. Table 2. Changes of pectoralis minor length index according to intervention.
Table 2. Changes of pectoralis minor length index according to intervention. Table 3. Changes of neck range of motion according to intervention.
Table 3. Changes of neck range of motion according to intervention. Table 4. Change of pressure pain threshold according to intervention.
Table 4. Change of pressure pain threshold according to intervention. Table 5. Change in muscle activity.
Table 5. Change in muscle activity. Table 6. Satisfaction with telerehabilitation program.
Table 6. Satisfaction with telerehabilitation program. Table 7. Status of devices used when participating in telerehabilitation program.
Table 7. Status of devices used when participating in telerehabilitation program. Table 8. Advantages and disadvantages of telerehabilitation.
Table 8. Advantages and disadvantages of telerehabilitation. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








