06 February 2023: Database Analysis
Comparison of Neonatal Morbidity and Mortality Following Spontaneous and Medically Indicated Preterm Births: A Retrospective Population-Based Study Using Data from the Slovenian National Perinatal Information System 2013–2018
Katja Čehovin1DEF, Ajda Gortnar2DEF, Ivan Verdenik3ABCD, Miha Lučovnik34ACDE, Lilijana Kornhauser-Cerar3ACDE, Štefan Grosek356ACDEFG*DOI: 10.12659/MSM.938941
Med Sci Monit 2023; 29:e938941
Abstract
BACKGROUND: This retrospective population-based study analyzed data from the Slovenian National Perinatal Information System (NPIS) between 2013 and 2018 to compare neonatal morbidity and mortality following spontaneous and medically indicated preterm births.
MATERIAL AND METHODS: Retrospective population-based cohort. Entries to the NPIS database were searched by gestational age (GA) <37 weeks in Slovenia between 2013 and 2018. Of 9200 (6252 following spontaneous birth, 2948 following medically indicated) neonates included, 1358 were born at extremely to very preterm GA (998 following spontaneous birth, 360 following medically indicated). Logistic regression analysis was used to examine the association between neonatal mortality and composite severe neonatal morbidity and preterm birth type (spontaneous vs medically indicated) controlling for potential confounding variables. Analysis was first performed for all preterm births (GA 22 0/7 to 36 6/7) and later only for extremely to very preterm births (GA 22 0/7 to 31 6/7).
RESULTS: Neonatal mortality was significantly lower following spontaneous preterm birth at extremely to very preterm GA (odds ratio [OR] 0.34; 95% confidence interval [CI] [0.14, 0.81]), while there was no association in all preterm births group (OR 0.56; 95% CI [0.26, 1.20]). No significant correlation between preterm birth type and neonatal morbidity was found (OR 0.76; 95% CI [0.54, 1.09] for all preterm births and OR 0.71; 95% CI [0.47, 1.07] for extremely to very preterm births).
CONCLUSIONS: In this population study from Slovenia between 2013 and 2018, medically indicated preterm births at <32 weeks of GA were associated with significantly increased neonatal mortality but not neonatal morbidity.
Keywords: Infant, Infant Mortality, Morbidity, Premature Birth, Preterm Premature Rupture of the Membranes, Pregnancy, Female, Infant, Newborn, Humans, Gestational Age
Background
Preterm births, defined as birth before 37 weeks of pregnancy, are completed. Based on GA at birth, preterm births are further divided into moderate to late preterm birth (32 to 37 weeks GA), very preterm (28 to 32 weeks GA), and extremely preterm (less than 28 weeks GA) [1]. Preterm neonates can either be born after spontaneous preterm labor, preterm premature rupture of the membranes (PPROM) (ie, spontaneous preterm birth), or after medically indicated preterm delivery for maternal and/or fetal indications, which includes induction of labor or cesarean delivery [2]. The incidence of medically indicated preterm birth has been increasing globally as well as in Slovenia [3–7]. However, recent temporal trends have shown either a decline or stabilization of the rate of preterm births in recent years in some high-income countries [8–11].
Analyses of temporal trends in the incidence of medically indicated preterm birth suggested a decline in neonatal mortality in these type of preterm deliveries over time [2,12,13]. Nonetheless, newer temporal analyses have shown conflicting results, varying by GA groups [8,10]. However, studies focusing on mortality within groups of preterm neonates born after either spontaneous or medically indicated preterm labor did not find such an association [14,15]. Some studies have even concluded that mortality seems to be higher in certain groups of neonates born after medically indicated preterm birth [16,17]. The discrepancy in previously reported findings is even greater when analyzing correlations between types of preterm birth and severe neonatal morbidity, such as severe intraventricular hemorrhage (IVH) (Papile grade 3 and 4), cystic periventricular leukomalacia (cPVL) followed by long-term neurological impairment [15,18], bronchopulmonary dysplasia (BPD) [19], necrotizing enterocolitis (NEC) [20,21], retinopathy of prematurity (ROP) [22,23], and late-onset neonatal sepsis (LOS) [15]. Furthermore, recent larger studies have shown the neonatal outcomes are affected by underlying disorders necessitating preterm termination of pregnancy by induction of labor or cause spontaneous preterm birth [24–27].
The Slovenian NPIS collects data on newborn and maternal medical care from national birth records. The registration is mandatory by law for all deliveries in Slovenia’s maternity units at ≥22 weeks of pregnancy or when the birthweight is ≥500 g [28].
This retrospective population-based study analyzed data from the Slovenian NPIS between 2013 and 2018 to compare neonatal morbidity and mortality following spontaneous and medically indicated preterm births.
Material and Methods
STUDY DESIGN:
We conducted a retrospective population-based study using data retrieved from the NPIS. We analyzed all preterm births (GA <37 0/7 weeks) in Slovenia from 1/1/2013 to 31/12/2018. The database contains perinatal and neonatal information on more than 140 variables entered by midwives or physicians. Data are periodically audited and comparisons to international databases are made to ensure quality.
DEFINITIONS:
Spontaneous preterm birth was defined as spontaneous onset of preterm labor with intact membranes or preterm premature rupture of membranes (PPROM) resulting in preterm birth. Medically indicated preterm birth was defined as preterm birth following induction of labor or cesarean section for maternal and/or fetal indications. Calculation of GA was based on the last menstrual period and was confirmed or modified by ultrasound imaging within the first trimester.
EXCLUSION CRITERIA:
We excluded neonates with congenital anomalies and those who died within 24 hours after birth, because they died before specific morbidities analyzed in the study could develop.
STRATIFICATION:
We stratified premature neonates in 2 groups: all preterm neonates born at GA 22 0/7 to 36 6/7 weeks and extremely-very preterm neonates born at GA 22 0/7 to 31 6/7 weeks. We analyzed neonatal mortality and morbidity by onset of labor: spontaneous (intact membranes and PPROM) and medically indicated (induction or premature cesarean section for maternal/fetal indications). The association between preterm birth type (spontaneous vs medically indicated) and neonatal mortality, as well as neonatal morbidity, was analyzed for both GA groups separately. Composite neonatal morbidity was defined as at least 1 of the following: severe IVH (Papile grade 3 and 4), cPVL, NEC, BPD, LOS, and ROP. The association between preterm birth type and each of these morbidities was also analyzed separately.
STATISTICAL ANALYSIS:
Univariate comparison of neonatal outcomes following spontaneous vs medically indicated preterm birth was performed with the Pearson chi-square test [29], and P value <0.05 was considered significant. Multivariate logistic regression was used to analyze associations between neonatal outcomes and preterm birth type, accounting for potential confounding variables: small for gestational age (SGA - defined as neonatal birth weight <5th percentile for gestation), mode of delivery (cesarean vs vaginal delivery), breech presentation, administration of glucocorticoids before birth, multiple pregnancies, administration of magnesium sulfate for neuroprotection, maternal age >37 years, maternal body-mass-index (BMI) >30 kg/m2, and in vitro fertilization (IVF). In multivariate analysis of extremely to very preterm births we also accounted for GA groups: 22 0/7 to 27 6/7 and 28 0/7 to 31 6/7 weeks. We used SPSS software, version 25 (SPSS, Chicago, IL, USA).
Results
STUDY SAMPLE:
Over the study period we identified 9258 preterm neonates born in the Republic of Slovenia. First, we excluded 58 neonates who died within 24 hours of birth. The remaining 9200 were analyzed as the all-preterm births group. Analysis was also performed separately for 1358 neonates born at extremely to very preterm GA. These 2 groups were then subdivided by the onset of labor. Most neonates were born after spontaneous onset of labor or PPROM: 6252 out of 9200 (68.0%) in the all-preterm group and 998 out of 1358 (73.5%) in the extremely to very preterm group; 2948 out of 9200 (32.0%) were born after medically indicated induction of labor or cesarean section in the all-preterm group and 360 out of 1358 (26.5%) in the extremely to very preterm group.
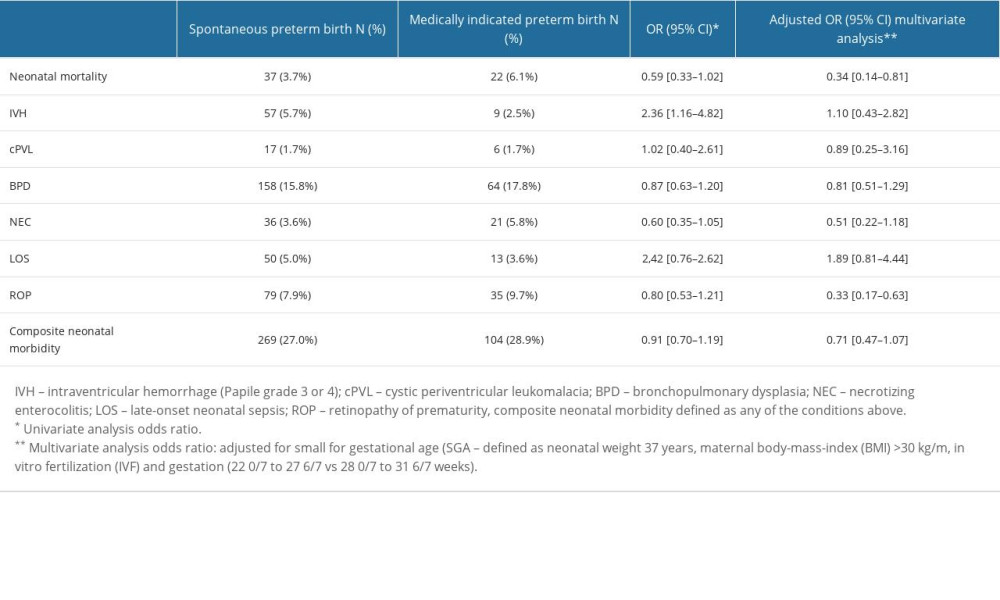
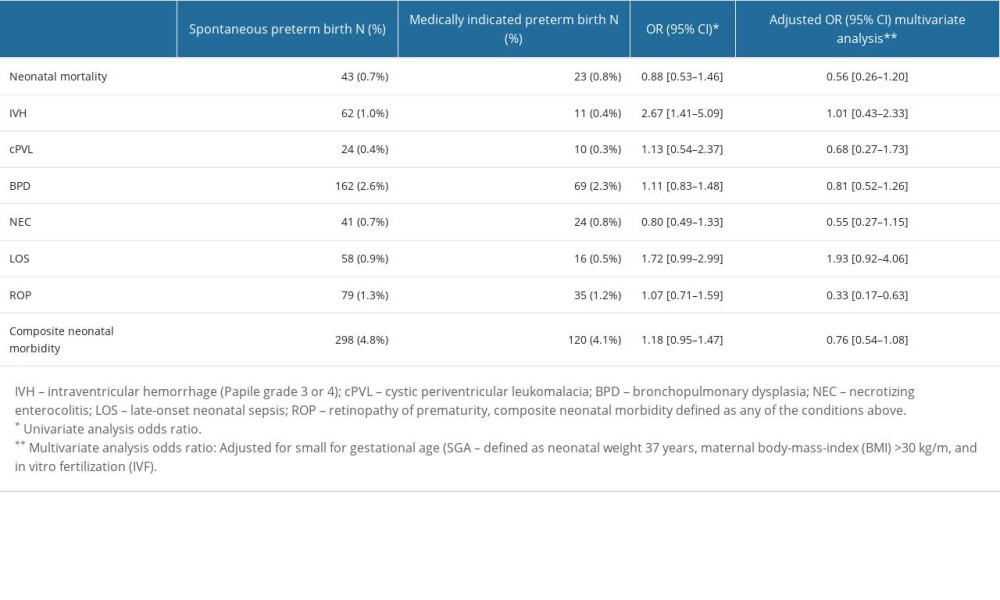
Tables 1 and 2 present neonatal outcomes according to type of preterm birth at extremely to very preterm GA (Table 1) and all preterm GA (Table 2).
NEONATAL MORTALITY:
In univariate analysis, we did not find a statistically significant correlation between type of onset of labor and mortality in the group of all preterm neonates (OR 0.88; 95% CI [0.53,1.46], or in the extremely to very premature neonate group (OR 0.59; 95% CI [0.34,1.02]). Multivariate analysis showed significantly lower mortality after spontaneous preterm birth (OR 0.34; 95% CI [0.14, 0.81]) compared to medically indicated preterm birth in extremely to very preterm births group, but not in the group of all preterm neonates (Table 1).
NEONATAL MORBIDITY:
When searching for possible associations between composite morbidity and type of onset of labor, we did not find any significant correlation in univariate and multivariate analysis in the all-preterm group (OR 0.76; 95% CI [0.54,1.08]) (Table 2) or in the extremely to very preterm group (OR 0.71; 95% CI [0.47, 1.07]) (Table 1).
For individual diagnoses, we found statistically significant correlations between severe IVH (Papile grade 3 and 4) and spontaneous preterm birth in both groups divided by GA (OR 2.67; 95% CI [1.41, 5.09] for the all-preterm group and OR 2.36; 95% CI [1.16,4.82] for extremely to very preterm group). After adjustment for other confounding factors in multivariate analysis, those correlations did not appear to be statistically significant (OR 1.01; 95% CI [0.43, 2.33] for the all-preterm group and OR 1.10; 95% CI [0.43, 2.82] for the extremely to very preterm group).
Other diagnoses (cPVL, BPD, NEC, ROP, and LOS) were not significantly correlated with preterm birth type in any of the groups according to GA at birth in univariate or in multivariate analysis.
Discussion
In the all-preterm births group, we found no association between neonatal mortality or morbidity and type of preterm birth (spontaneous vs medically indicated). In the extremely to very preterm births group, however, medically indicated preterm delivery was associated with higher risk of neonatal mortality. Mortality was significantly lower in neonates after spontaneous preterm birth compared to medically indicated premature birth. Composite morbidity, which included all 5 severe disabilities of prematurity (IVH, cPVL, ROP, NEC, and LOS), was not associated with type of preterm birth.
Our findings regarding neonatal mortality were in line with several previous studies. Similar to our results, Grill et al
For neonatal morbidity, studies have suggested links between type of preterm birth and morbidity in various subgroups divided by GA. Morken et al have suggested a correlation between medically indicated preterm birth and higher incidence of respiratory and gastrointestinal diagnoses, as well as a correlation between spontaneous preterm birth and cerebral palsy and sepsis [15]. Similarly, Stout et al have shown that medically indicated preterm birth are correlated with higher early and late respiratory morbidity [19]. Other conflicting results were found when comparing our results of ROP not being correlated to type of preterm birth to previous studies
Two large retrospective studies of temporal trends in neonatal mortality and incidence of medically indicated preterm birth found that the rising incidence of medically indicated preterm labor coincides with a lower incidence of neonatal mortality over time, suggesting that medically indicated preterm birth could be a successful intervention to decrease preterm neonatal mortality [12,13]. Furthermore, a more recent temporal analysis of Canadian preterm births observed higher rates of medically indicated preterm birth during 2009–2016, but lower mortality and morbidity in the preterm groups. Furthermore, their data showed a decrease in neonatal sepsis and respiratory distress, but higher IVH, during that period [10]. Interestingly, recent research of temporal trends in Washington state between 2004 and 2013 has shown a rise in incidence of medically indicated preterm birth, associated with increased mortality and increased morbidity in the group of medically indicated late preterm births, suggesting that neonatal sepsis mostly affects neonatal morbidity outcomes [8].
We combined several neonatal morbidities into a composite morbidity outcome to be able to analyze larger groups of neonates. Despite this, the type of preterm birth did not appear to be correlated with morbidity in any of the GA groups. It may be that medically indicated preterm birth results in better neonatal outcomes, considering that medical interventions can be planned ahead and executed with proper (optimal) timing. On the other hand, pregnancy disorders necessitating intervention resulting in medically indicated preterm delivery play a strong role in underlying pathological mechanisms of neonatal disorders. Our results suggest that other prenatal factors, rather than type of onset of birth alone, are correlated with neonatal morbidity. This is in line with various recent studies confirming that the underlying disorder in pregnancy is correlated with morbidity of preterm neonates [24–27].
The strengths of our study are its large population size, nation-wide nature, and access to high-quality data in the NPIS. These data are consistently collected and coded, and registration of each birth to NPIS is mandatory by law. Data on pregnancy and maternal factors that could possibly affect the results were included in the research. In order for the research to have higher relevance for public health, we decided not to exclude multiple pregnancies, which more often result in preterm birth than singletons and have become more common due to infertility treatments [30].
Our study has several limitations. First, the data in the NPIS are based on forms, filled out by midwives, doctors, and nurses, thus errors in initial data collection, coding and classification may have occurred. Second, the classification of preterm birth subtype could not be strictly separated due to active surveillance of pregnancies, especially those considered high-risk. The PPROM group was included in the spontaneous preterm group, although some researchers suggest that this group should be at higher risk for adverse neonatal outcomes [16]. Third, we have not analyzed specific indications for medically indicated preterm births such as hypertensive disorders of pregnancy, fetal growth restriction, and chorioamnionitis. Each of these can have different effects on outcomes of preterm birth. Fourth, due to the observational nature of the study, we could not account for all potential confounding factors such as admission to the intensive care unit and post-natal interventions such as mechanical ventilation. These may profoundly affect outcomes such as ROP, BPD, and LOS, as well as composite neonatal morbidity, and these need to be addressed in future studies. Last, we recognize the limitations of the main statistical analysis used and the ability to interpret data based on small sample sizes and testing for several independent variables. Hence, the analysis of each preterm group divided by GA – late preterm birth, very preterm, and extremely preterm – would have smaller sample sizes and less statistically significant relevant results, especially when analyzing for each of the diagnoses separately.
Conclusions
Among preterm neonates born in Slovenia between 2013 and 2018, most of the premature births occurred after spontaneous labor or PPROM. Medically indicated preterm birth was associated with higher risks of neonatal mortality at very to extremely preterm GA.
References
1. Vogel JP, Chawanpaiboon S, Moller AB, The global epidemiology of preterm birth: Best Pract Res Clin Obstet Gynaecol, 2018; 52; 3-12
2. Ananth CV, Vintzileos AM, Epidemiology of preterm birth and its clinical subtypes: J Matern Fetal Neonatal Med, 2006; 19(12); 773-82
3. Martin JA, Kirmeyer S, Osterman M, Shepherd RA, Born a bit too early: Recent trends in late preterm births: NCHS Data Brief, 2009(24); 1-8
4. Lucovnik M, Bregar AT, Steblovnik L, Changes in incidence of iatrogenic and spontaneous preterm births over time: A population-based study: J Perinat Med, 2016; 44(5); 505-9
5. Gyamfi-Bannerman C, Ananth CV, Trends in spontaneous and indicated preterm delivery among singleton gestations in the United States, 2005-2012 [published correction appears in Obstet Gynecol. 2016;127(3):605]: Obstet Gynecol, 2014; 124(6); 1069-74
6. Martin JA, Hamilton BE, Sutton PD, Births: Final data for 2004: Natl Vital Stat Rep, 2006; 55(1); 1-101
7. Zeitlin J, Szamotulska K, Drewniak N, Preterm birth time trends in Europe: A study of 19 countries: BJOG, 2013; 120(11); 1356-65
8. Richter LL, Ting J, Muraca GM, Temporal trends in neonatal mortality and morbidity following spontaneous and clinician-initiated preterm birth in Washington State, USA: A population-based study: BMJ Open, 2019; 9(1); e023004
9. Martin JA, Hamilton BE, Osterman MJ, Births: Final data for 2015: Natl Vital Stat Rep, 2017; 66(1); 1
10. Richter LL, Ting J, Muraca GM, Temporal trends in preterm birth, neonatal mortality, and neonatal morbidity following spontaneous and clinician-initiated delivery in Canada, 2009–2016: J Obstet Gynaecol Can, 2019; 41(12); 1742-1751e6
11. Richards JL, Kramer MS, Deb-Rinker P, Temporal trends in late preterm and early term birth rates in 6 high-income countries in North America and Europe and association with clinician-initiated obstetric interventions [published correction appears in JAMA. 2016;316(15):1601]: JAMA, 2016; 316(4); 410-19
12. Ananth CV, Joseph KS, Oyelese Y, Trends in preterm birth and perinatal mortality among singletons: United States, 1989 through 2000: Obstet Gynecol, 2005; 105(5 Pt 1); 1084-91
13. Lisonkova S, Hutcheon JA, Joseph KS, Temporal trends in neonatal outcomes following iatrogenic preterm delivery: BMC Pregnancy Childbirth, 2011; 11; 39
14. Fritz T, Källén K, Maršál K, Jacobsson B, Outcome of extremely preterm infants after iatrogenic or spontaneous birth: Acta Obstet Gynecol Scand, 2018; 97(11); 1388-95
15. Morken NH, Källen K, Jacobsson B, Outcomes of preterm children according to type of delivery onset: A nationwide population-based study: Paediatr Perinat Epidemiol, 2007; 21(5); 458-64
16. Chen A, Feresu SA, Barsoom MJ, Heterogeneity of preterm birth subtypes in relation to neonatal death: Obstet Gynecol, 2009; 114(3); 516-22
17. Grill A, Olischar M, Weber M, Type of delivery onset has a significant impact on post-natal mortality in preterm infants of less than 30 weeks’ gestation: Acta Paediatr, 2014; 103(7); 722-26
18. Chen X, Zhang X, Li W, Iatrogenic vs. spontaneous preterm birth: A retrospective study of neonatal outcome among very preterm infants: Front Neurol, 2021; 12; 649749
19. Stout MJ, Demaree D, Merfeld E, Neonatal outcomes differ after spontaneous and indicated preterm birth: Am J Perinatol, 2018; 35(5); 494-502
20. Patel BK, Shah JS, Necrotizing enterocolitis in very low birth weight infants: A systemic review: ISRN Gastroenterol, 2012; 2012; 562594
21. Wójkowska-Mach J, Różańska A, Borszewska-Kornacka M, Necrotising enterocolitis in preterm infants: Epidemiology and antibiotic consumption in the Polish neonatology network Neonatal Intensive Care Units in 2009: PLoS One, 2014; 9(3); e92865
22. Lee JW, McElrath T, Chen M, Pregnancy disorders appear to modify the risk for retinopathy of prematurity associated with neonatal hyperoxemia and bacteremia: J Matern Fetal Neonatal Med, 2013; 26(8); 811-18
23. Lynch AM, Wagner BD, Hodges JK, The relationship of the subtypes of preterm birth with retinopathy of prematurity: Am J Obstet Gynecol, 2017; 217(3); 354e1-e8
24. Villamor-Martinez E, Álvarez-Fuente M, Ghazi AMT, Association of chorioamnionitis with bronchopulmonary dysplasia among preterm infants: A systematic review, meta-analysis, and metaregression: JAMA Netw Open, 2019; 2(11); e1914611
25. Been JV, Lievense S, Zimmermann LJ, Chorioamnionitis as a risk factor for necrotizing enterocolitis: A systematic review and meta-analysis: J Pediatr, 2013; 162(2); 236-42e2
26. Villamor-Martinez E, Fumagalli M, Mohammed Rahim O, Chorioamnionitis is a risk factor for intraventricular hemorrhage in preterm infants: A systematic review and meta-analysis [published correction appears in Front Physiol. 2019;10:102]: Front Physiol, 2018; 9; 1253
27. Damodaram M, Story L, Kulinskaya E, Early adverse perinatal complications in preterm growth-restricted fetuses: Aust N Z J Obstet Gynaecol, 2011; 51(3); 204-9
28. National Institute of Public Health (Slovenia): Slovenia Perinatal Information System, Comparisons of Data between Regions and Maternity Hospitals for 2001, 2003, Ljubljana, Slovenia, National Institute of Public Health (Slovenia) Available from https://ghdx.healthdata.org/record/slovenia-perinatal-information-system-comparisons-data-between-regions-and-maternity
29. Pearson K, (1900). X. On the criterion that a given system of deviations from the probable in the case of a correlated system of variables is such that it can be reasonably supposed to have arisen from random sampling: The London, Edinburgh, and Dublin Philosophical Magazine and Journal of Science, 2009; 50(302); 157-75
30. Tul N, Lucovnik M, Verdenik I, The contribution of twins conceived by assisted reproduction technology to the very preterm birth rate: A population-based study: Eur J Obstet Gynecol Reprod Biol, 2013; 171(2); 311-13
In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387