24 January 2023: Clinical Research
Effects of Caregiver’s Gender or Distance Between Caregiver and Patient’s Home on Home Discharge from Hospital in 285 Patients Aged ≥75 Years in Japan
Yoshimasa Oda12ABCDEF, Naoko E. KatsukiDOI: 10.12659/MSM.939202
Med Sci Monit 2023; 29:e939202
Abstract
BACKGROUND: Many hospitalized aged patients in Japan, the most super-aged society, are unable to be discharged home. This study was performed to clarify the factors associated with home discharge, not to a long-term care (LTC) facility or another hospital, among inpatients aged ≥75 years.
MATERIAL AND METHODS: A single-center prospective cohort study was performed for inpatients aged ≥75 years in a rural acute-care hospital in Japan, from November 2017 to October 2019. We divided the patients into 2 groups: those who resided at home or had died at home by 30 days after discharge, and others. We obtained data from medical charts and questionnaires given to patients and their caregivers. For each factor shown to be statistically significant by the univariable analysis, a multivariable analysis with adjustment was conducted.
RESULTS: In all, 285 patients agreed to participate. With adjustment by where the patient was admitted from, residing with other family members, cognitive function scores, and Barthel index, multivariable analysis using each factor identified as relevant by univariable analysis identified the following as associated with home discharge: being less informed about LTC insurance; cost of home-visit medical, nursing, or LTC services; shorter hospital stays; close proximity between patient and caregiver; main caregiver being female; and life expectancy of over 6 months (P<0.05).
CONCLUSIONS: Male gender and a long distance between the caregiver and patient’s home significantly hindered home discharge in patients aged ≥75 years, suggesting the need to provide information regarding home-visit services under Japan’s LTC insurance system for such caregivers.
Keywords: Aged, Caregivers, Long-Term Care, Patient Discharge, home environment, Humans, Male, Female, Japan, Prospective Studies, Hospitals
Background
Japan is the world’s most super-aged country: in 2020, it had a record-breaking 29% of its population aged ≥65 years [1]; the rate is even higher in rural areas [2]. Accordingly, the cost of the national pension system, medical health insurance, and long-term care (LTC) insurance for the aged exceeds 723 billion United States dollars (USD) annually, which is 10% of gross domestic product [3,4]. To reduce this expenditure, Japan’s government has undertaken reform of the national health-care system (implemented at the prefectural level), which has reduced the number of inpatient beds nationwide [5]. However, owing to limited facilities, the number of people aged ≥65 years on waiting lists for LTC was almost 292 000 in 2019; 34 000 of those needed immediate institutionalization [6]. Thus, it is necessary for home medical or nursing care of aged patients to compensate for the lack of inpatient beds [7], which shows the increasing importance of LTC at home.
Contrary to the increasing importance of home care, however, a considerable proportion of aged individuals worldwide (about 9–11%) was discharged to facilities other than the home after undergoing inpatient treatment [8,9]. Currently, 68% of people in Japan and 58–70% in other countries die in hospitals – even though worldwide the proportion who wish to die at home is 25–97% [10,11]. Evidently, it is becoming increasingly difficult for aged patients to be discharged home after having undergone repeated hospitalization.
Investigating how Japan copes with various problems that have emerged owing to its aging society – especially in rural areas – may be helpful for other countries: they could address their own problems based on the efforts made in rural Japan. Some research has examined the characteristics of patients discharged home [12–19]; however, no studies have investigated home discharge after acute-care hospitalization, and few studies have reported the characteristics of caregivers for patients discharged home – even in Japan. We conducted the present study to clarify the factors promoting home discharge without being transferred to an LTC facility or another hospital among inpatients aged ≥75 years in Japan. These findings will help to identify appropriate and effective interventions.
Material and Methods
ETHICS STATEMENT:
The present study conforms to the ethics guidelines for medical and health research involving human subjects issued by Japan’s Ministry of Health, Labour, and Welfare and Ministry of Education, Culture, Sports, Science, and Technology. This study was approved by the Research Ethics Committee of the Yuai-Kai Foundation and Oda Hospital (no. 20170725). We obtained written informed consent from each patient, and patient anonymity was protected.
STUDY DESIGN AND POPULATION:
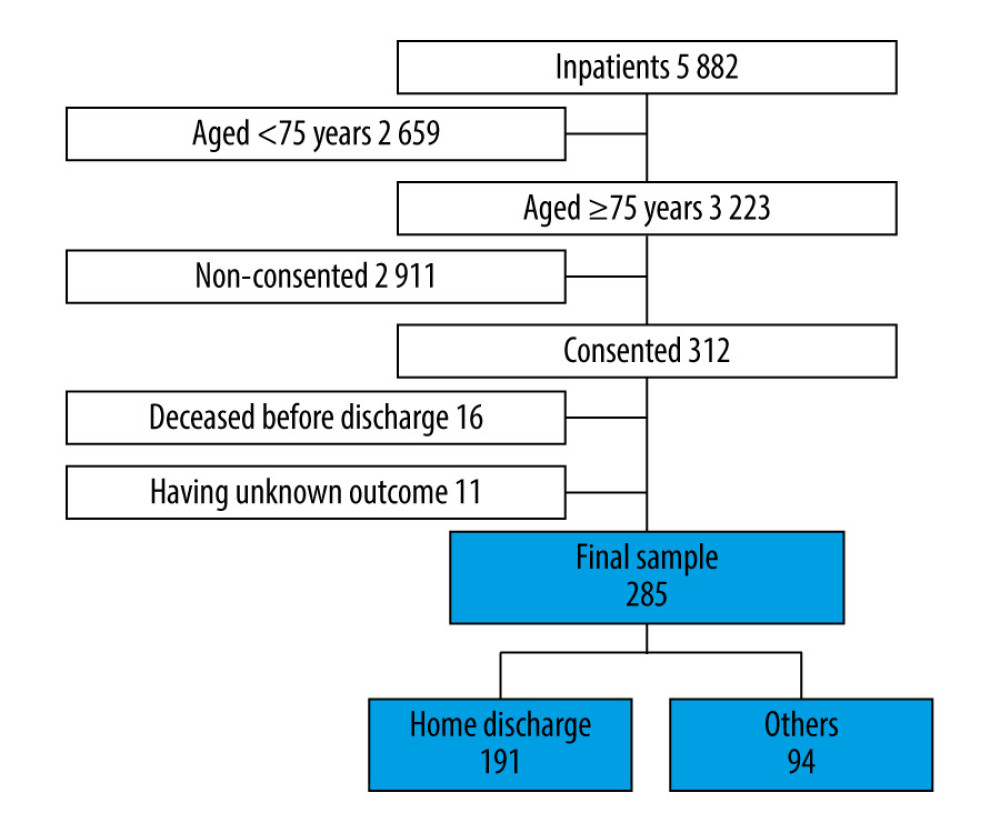
This was a single-center-based prospective cohort study using medical charts, questionnaires, and telephone inquiries. We enrolled all patients aged ≥75 years admitted to an acute-care hospital in a rural city in Japan from November 2017 to October 2019. We divided the patients into 2 groups according to the results of telephone inquiries performed over 30 days after discharge: those who had remained at home longer than they did elsewhere or had died at home by 30 days after discharge (the Home group); and others (the Other group). We compared the data derived from medical charts and questionnaire responses between the groups.
STUDY HOSPITAL CHARACTERISTICS:
The hospital is located in a rural city, Kashima, in Saga Prefecture, southern Japan, and the city’s population is approximately 27 000 [20]. That hospital treats over 3 100 inpatients annually, with a mean length of stay of 12.1 days. The institution has 111 beds and has 10 departments, including internal medicine, general surgery, and cardiovascular surgery, without orthopedic surgery. The hospital provides home services, such as medical and nursing care and rehabilitation with home visits. The institution also focuses on key areas such as special treatment for patients suffering from dementia by means of a specific ward (Dementia Care Unit) and providing support for patients, caregivers, or family members about life after hospital discharge.
DATA SOURCE:
Written responses to the questionnaires were made within 24–72 hours after admission by the patients themselves and their main caregivers. If patients had difficulty writing their answers, hospital medical staff assisted them. The telephone inquiries were made by research assistants within 3 days after 30 days of discharge to determine where the patients resided or where they had died after discharge.
We selected all the variables listed below from factors reportedly relevant to home discharge [12–19]; relevant to home death [21–23]; or that doctors, nurses, or certified care managers at the hospital involved in this study believed relevant.
VARIABLES EXTRACTED FROM THE HEALTH RECORDS:
The variables extracted from the health records were the following: patient’s age (years); gender (man or woman); Barthel index (0–100) [24]; official Japanese activity of daily living (ADL) scale for aged people (bedriddenness rank – normal, J1, J2, A1, A2, B1, B2, C1, C2) [25,26]; official Japanese cognitive function scores for aged people (cognitive function scores – normal, 1, 2a, 2b, 3a, 3b, 4, M) [25,26]; requiring continuous medical treatment after discharge (present or absent); requiring continuous sputum aspiration after discharge (present or absent); necessity of home remodeling to stay home after discharge (necessary or unnecessary); facility to which the certified care manager belonged (hospital where the present study was conducted or other); main diagnosis on discharge; life expectancy (up to 6 months or longer); and date of admission and discharge (date). A certified care manager is a person who plans, conducts, or monitors a patient’s nursing care under Japan’s LTC insurance system [5,27–30]. The name of the in-hospital attending physician, main diagnosis, and life expectancy were determined and recorded by a physician based on medical charts. Attending nurses determined and recorded the basic ADLs for calculating the Barthel index and assessing whether or not medical treatment was required after discharge. Care managers at the study hospital determined and recorded the facility to which the certified care manager responsible for the patient belonged. Necessary medical treatment after discharge was defined as follows: presence of pressure ulcer, skin wound, or gastric, colonic, or urinary stoma; necessity for applying ointment, self-injection, sputum aspiration, or respirator, urethral catheter, intravenous infusion, or administration of oxygen; or self-monitoring of blood glucose.
VARIABLES IN THE QUESTIONNAIRE FOR PATIENTS:
The variables on the questionnaire for patients included the following: other resident family members; place the patient was admitted from (home, LTC facility, another hospital); whether the patient had talked with other family members about where and how to live at the end of their lives (had talked, had never talked); how much the patient preferred to stay at the 3 kinds of places (home, LTC facility, another hospital) immediately after discharge, during LTC life, or at the end stage of life (visual analog scale [VAS] ranging from 0 to 100); whether the patient owned or rented their place of residence; how long the patient lived at the residence (years); patient’s knowledge of home-visit medical care, home-visit nursing care, home-visit rehabilitation, home-visit LTC, care managers [29,30], and Japan’s LTC insurance system [5,27,28] (had never heard about the service, had heard the term, was well informed or had experience of use); and patient’s knowledge of the cost of home-visit medical care, home-visit nursing care, home-visit rehabilitation, and home-visit LTC (had never heard the cost, had heard the cost, had experience of using the service).
VARIABLES IN THE QUESTIONNAIRE FOR MAIN CAREGIVERS:
The variables on the questionnaire for main caregivers included the following: caregiver’s age; gender (man or woman); family relationship to the patient; how often the patient’s behavioral and psychiatric symptoms of dementia (BPSD) appeared (none, once a month, once a week, 2 or 3 days/week, almost daily); distance between where the patient and caregiver lived (same house, different house but within 5-minute walk, more distant but same city, more distant but same prefecture, outside the prefecture); weekly time available for caregiving (hours); monthly financial expense for the patient (under 7.2 USD, 7.2–71 USD, 72–216 USD, 217–360 USD, 361 USD or more, did not wish to answer); previous experience of caregiving (experience or no experience); whether a second caregiver was present (present or absent); how much the caregiver preferred to let the patient stay at the 3 kinds of places (home, LTC facility, another hospital) at 3 time points (immediately after discharge, during LTC life, or at the end stage of life; VAS, 0–100); caregiver’s knowledge of home-visit medical care, home-visit nursing care, home-visit rehabilitation, home-visit LTC, care managers [29,30], and Japan’s LTC insurance system [5,27,28] (had never heard about the service, had heard the term, was well informed, had experience of use); caregiver’s knowledge of cost of home-visit medical care, home-visit nursing care under medical insurance, home-visit nursing care under LTC insurance, home-visit rehabilitation, and home-visit LTC (had never heard the cost, had heard the cost, had experience of using the service); 12-item short-form health survey (SF-12) v2, which is a measure of physical and mental health related to quality of life [31]; and burden index of caregivers (BIC)-11, which is a measure of the caregiver’s burden from 5 domains (time-dependent, emotional, existential, physical, and service-related) [32]. The score 50 of SF-12 signifies a standard deviation for each of the 8 categories: a higher score indicates higher quality. The total BIC-11 score ranges from 0 to 44: a higher score indicates greater caregiver burden.
SAMPLE SIZE:
Owing to the exploratory nature of this study, we did not calculate a formal sample size. A convenience sample size could not be determined because no previous study had indicated a significant relationship among caregivers’ gender and home discharge or home death, which would have been required for calculation.
STATISTICAL ANALYSIS:
We present the categorical and continuous variables as absolute numbers (percentage) and medians (interquartile range). We compared each variable between the Home and the Other groups by univariable analysis using the chi-square test for categorical variables and Mann-Whitney U test for continuous variables. To validate the independent factors for home discharge, we conducted multivariable analysis using binary logistic regression with the forced-entry method. First, only 4 factors are reportedly related to home discharge – place where the patient was admitted from, living alone, Barthel index, and cognitive function scores – which we used as covariables [13,15,16,19]. Second, for each factor that showed significant difference between the 2 groups by univariable analysis, we conducted multivariable analysis using binary logistic regression with the forced-entry method to identify the factors related to home discharge. We adjusted the above 4 covariables in the analysis. We set the statistical significance level at P<0.05.
Results
UNIVARIABLE ANALYSIS:
Univariable analysis for each factor showed that the Home group had a significantly higher proportion of patients with the following factors: men (47% versus 33%; P=0.038); living with other family members (93% versus 74%; P=0.001); living with spouse (46% versus 24%: P=0.009); living with child’s spouse (22% versus 6.5%; P=0.025); owning the home (97% versus 92%; P=0.003); no need for ongoing medical treatment after discharge (71% versus 40%; P=0.001); no need for ongoing sputum aspiration after discharge (96% versus 81%; P=0.010); life expectancy greater than 6 months (96% versus 85%; P=0.001); and caregivers being women (69% versus 57%; P=0.044). The Home group showed the following: significantly younger patients (85 versus 88 years; P<0.001); higher Barthel index (85 versus 30; P<0.001); fewer of episodes of patient’s BPSD (P<0.001); shorter hospital stays (10 versus 20 days; P<0.001); stronger preference for staying home after discharge (100 versus 100; P<0.001); poorer understanding of the LTC insurance system (P=0.002), cost of home-visit medical care (P=0.050), cost of home-visit nursing care under medical insurance system (P=0.050), and cost of home-visit LTC (P=0.048); caregiver being older (P=0.044); closer distance between patient’s and main caregiver’s residence (P<0.001); more time for caregiving (70 versus 7 hours/week; P<0.001); stronger preference for caregiver to let patient stay home after discharge (100 versus 50; P<0.001); and poorer understanding by caregiver about care manager in hospital (P=0.034). There were significant differences between the Home and the Other group for the following: bedriddenness rank (P<0.001); cognitive function scores (P<0.001); place where the patient was admitted from (P<0.001); and family relationship of patient with primary caregiver (P<0.001). The Home group showed higher proportions for the following: normal bedriddenness rank on admission (34% versus 4.4%); normal cognitive function scores (47% versus 14%); admission from home (97% versus 50%); and spouse as primary caregiver (30% versus 5.5%; Tables 1, 3).
MULTIVARIABLE ANALYSIS WITH 4 COVARIABLES:
We conducted multivariable analysis with 4 covariables: where the patient was admitted from; living alone; Barthel index; and cognitive function scores. We found that apart from cognitive function scores, the covariables had a significant relationship with home discharge: admission from home (admission from LTC facility, regression coefficient [B] −3.11, 95% confidence interval [CI] of odds ratio [OR] 0.01–0.23, P<0.001; admission from hospital, B −3.29, 95% CI of OR 0.01–0.27, P=0.001); living alone (B −1.65, 95% CI of OR 0.05–0.69, P=0.012); and Barthel index (B 0.03, 95% CI of OR 1.01–1.05, P=0.003) (Table 4).
MULTIVARIABLE ANALYSIS USING EACH FACTOR ADJUSTED BY 4 COVARIABLES:
Table 5 shows the results of the multivariable analysis for each factor in which a significant difference existed between the 2 groups in the univariable analysis adjusted by the 4 covariables (from where the patient was admitted, living alone, Barthel index, and cognitive function scores). Some factors showed a significant relationship with home discharge: life expectancy under 6 months (B −2.13, 95% CI of OR 0.02–0.65, P=0.014); length of hospital stay (B −0.06, 95% CI of OR 0.90–0.98, P=0.002); understanding LTC insurance system (B −0.70, 95% CI of OR 0.30–0.82, P=0.006); understanding cost of home-visit medical care (B −1.00, 95% CI of OR 0.14–0.97, P=0.042); understanding cost of home-visit nursing care under medical insurance system (B −0.99, 95% CI of OR 0.14–0.99, P=0.047); understanding cost of home-visit LTC (B −1.08, 95% CI of OR 0.15–0.78, P=0.010); distance between patient and caregiver (B −0.62, 95% CI of OR 0.34–0.84, P=0.006); and caregiver being a woman (B 1.08, 95% CI of OR 1.06–8.23, P=0.038) (Tables 5, 6).
Discussion
The following factors are reportedly characteristic of patients discharged home after hospitalization: living with other family members [14,16]; being admitted from home [13]; having independent ADLs before admission [12]; higher Barthel index or Functional Independence Measure [14,19]; able to stand within 5 days after admission [12]; lower Acute Physiology and Chronic Health Evaluation (APACHE) II score [12]; cardiovascular disease as a main pathophysiological condition on day 3 of admission [14]; lower Charlson comorbidity index [13]; and normal or only slight cognitive impairment [14]. Similar to previously reported factors, we identified admission from home, not living alone, and higher Barthel index as factors associated with home discharge. We conducted our study in Kashima city, which has one of the highest age levels in Japan: 33% of the population is aged ≥65 years. In Japan, medical and welfare budgets are limited, and the need for home-visit LTC services has increased more than in other countries. We also found the following 5 characteristics to be associated with home discharge: being poorly informed about home-visit LTC services; life expectancy longer than 6 months; shorter hospital stay; closer distance between the patient and caregiver; and primary caregiver being a woman.
A key finding of the present study is that the patients who were discharged home were less informed about both home-visit medical care and home-visit LTC services. The relationship between death at home and knowledge or experience of home death has been examined [23]; however, the relationship between home discharge and knowledge of home-visit services has hitherto been unreported. Our findings were contrary to our expectations about well-informed patients tending to be discharged home: knowledge of services was not a facilitator of home discharge in the present study. Patients discharged to LTC facilities or transferred to another hospital would have been familiar with home-visit services; thus, patients should be provided with knowledge about such services before using LTC facilities. Patients discharged home tended to have poorer knowledge about home-visit services, which could indicate that achieving home discharge was possibly due to work overload among informal caregivers. Despite the high need for professional LTC upon discharge [33], the patients in our study had poor knowledge of home-visit services. Generally, patients are less familiar with home-visit services than with LTC facilities [34]. Admission to some hospitals could be a good opportunity to acquire knowledge about home-visit services under Japan’s medical or LTC insurance system, which would improve both patients’ and caregivers’ quality of life with LTC.
This study is the first to examine the relationship between home discharge and caregiver factors. We found that home discharge was associated with the following: primary caregiver being a woman; closer distance to the patient; caregiver strongly preferring home discharge; and caregiver less preferring discharge to another hospital. Concerning the primary caregiver being a woman, several reasons could explain why male caregivers hinder home discharge: younger male caregivers’ tendency to be under financial strain [35]; tendency of caregivers spending over 10 hours/week on caregiving to leave employment [36]; socially accepted gender role consciousness of the man being the breadwinner [37]; and longer paid working hours for men than women [38]. Patients using home-visit services tend to die at home [23]; thus, using those services would help male caregivers accept home discharge by reducing the caregiving time or alleviating the patients’ financial burden. It is essential to provide knowledge about home-visit services through the LTC insurance system to caregivers who live far from the patient and to male caregivers: home-visit services reportedly reduce the caregivers’ burden [39]. Information about subsidy programs, which could help caregivers live closer to patients or rebuild patients’ house to accommodate caregivers, must also be provided.
In light of reports about the relationship between caregivers’ preferences for patients’ home death and achieving it [21,22,40], their preferences for home discharge appear crucial toward bringing it about. Caregiver preferences having greater weight than those of the patient for home discharge is similar to the situation with home death [21,40]. We found that caregiver preferences for home discharge were independent of the patient living alone, physical and cognitive functions, and where the patient resided before admission; however, further research needs to elucidate the influence of those preferences.
We observed that admission from home was associated with home discharge. This finding is consistent with previous reports: patients aged ≥20 years admitted from another acute- or chronic-care hospitals or chronic nursing care facilities could not be discharged home [18]; admitted patients aged ≥20 years who had changed hospitals had longer hospital stays with a higher probability of discharge to post-acute-care medical facilities [17]. Our multivariable analysis showed that admission from another hospital and longer hospital stays were independent of home discharge (Table 4). Therefore, to help patients undergo LTC at home and achieve home death, it is necessary for medical staff to make efforts to shorten their hospital stays and avoid transfer to another facility after completing acute-care treatment. Conversely, it may be that home discharge itself helps reduce the length of hospital stays. Organizing patient transfers through negotiations with other hospitals is reportedly a reason for longer stays in the emergency department [41]: such transfers are unnecessary in the case of home discharge. Providing home-visit services to complement home discharge would help patients or caregivers achieve earlier discharge [42]; that would avoid some of the disadvantages caused by shorter hospital stays [43].
In this study, we observed that not having other resident family members was a factor against home discharge, which is consistent with previous results [15,17]. It is almost impossible for health-care providers to address the problems of not residing with other family members or patients’ short life expectancy; however, it would be useful to give such providers appropriate information on various support systems for helping aged patients living alone or at home at their end stage of life. The following factors reportedly help achieve home death: 24-hour-availablity of home-visit nursing care services [44]; clinics that provide end-of-life home treatment to patients [45]; having plentiful local care workers [45]; and physicians or nurses with positive attitudes toward home death [44]. Providing aged patients with positive information could promote home discharge.
The present study has some limitations. It was conducted at only 1 facility: it was a middle-scale hospital in a rural city in Japan with 111 beds and low numbers of patients undergoing advanced surgical operation or chronic rehabilitation. That could limit the generalizability of this study. We did not obtain details of the following: the environment of medical or LTC for individual patients, such as the number of nursing facilities providing 24-hour home-visit nursing care service, clinics providing home treatment for end-of-life patients, number of local care workers in the area, and physicians or nurses having positive attitudes for the home death of aged patients. In addition, the relatively low number of subjects (Figure 1) may have caused selection bias. Because we performed multiple comparisons for each factor by both univariable analysis and multivariable analysis, the risk of type I error may have increased. Additionally, because we adjusted for only 4 factors in the multivariable analysis, a further study with a larger sample size is desirable to determine whether the factors that were found to be significant in the present study are in fact independently associated with home discharge.
Conclusions
Caregivers living far from the patient or being male had a negative effect on home discharge of inpatients aged ≥75 years; providing appropriate support, including information about the LTC insurance system and home-visit support to such caregivers, could facilitate home discharge. It is also necessary to provide appropriate information about various kinds of support for the following: home discharge to patients admitted from home; those having a higher Barthel index or having other resident family members; closer distance between the patient and caregiver; the main caregiver being female; caregivers’ stronger preference for home discharge; and life expectancy of over 6 months. That would help improve both patients’ and caregivers’ quality of life at home with LTC.
Tables
Table 1. Comparison between the Home group and the Other group concerning the factors on the side of the patient.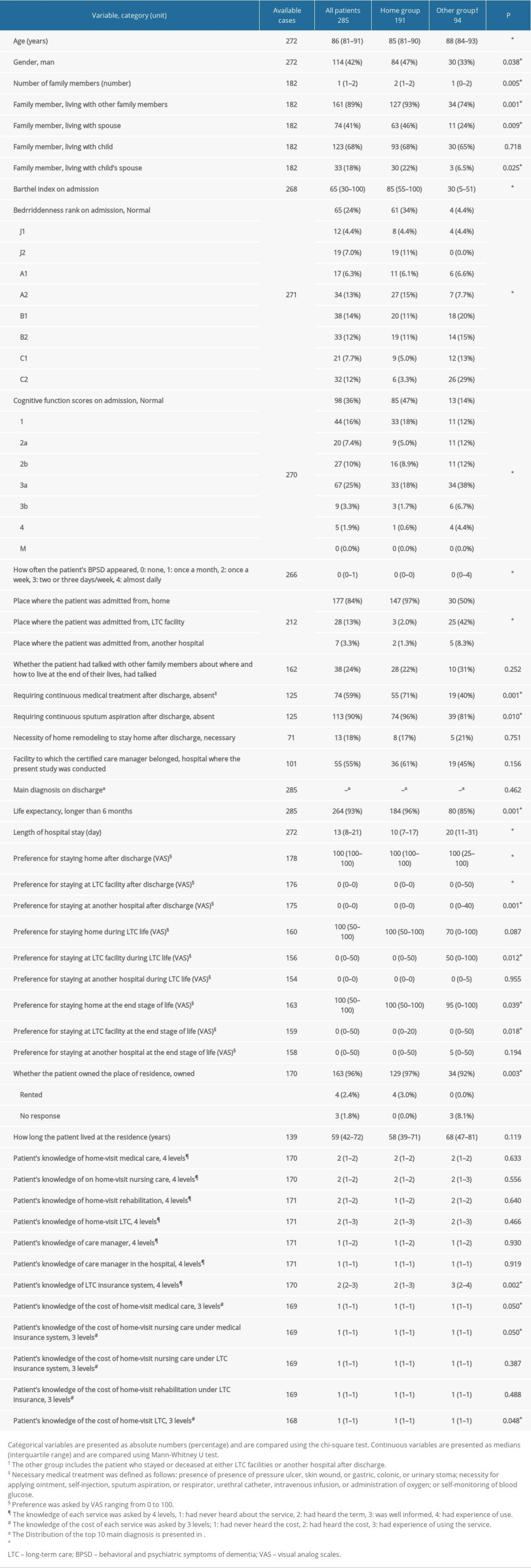 Table 2. Top 10 main diagnoses.
Table 2. Top 10 main diagnoses.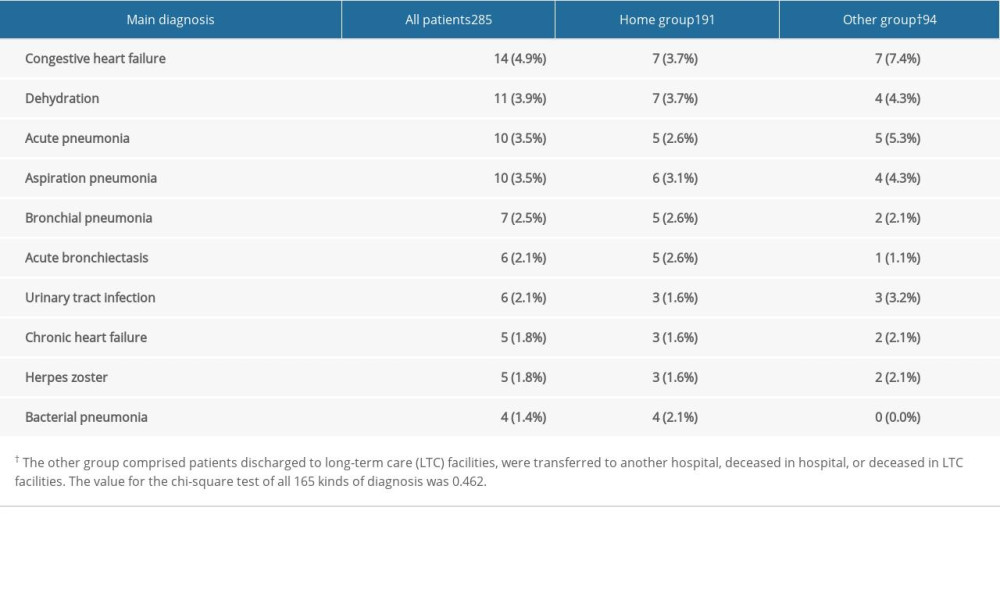 Table 3. Comparison between the Home group and the Other group concerning the factors on the side of patient’s caregiver.
Table 3. Comparison between the Home group and the Other group concerning the factors on the side of patient’s caregiver.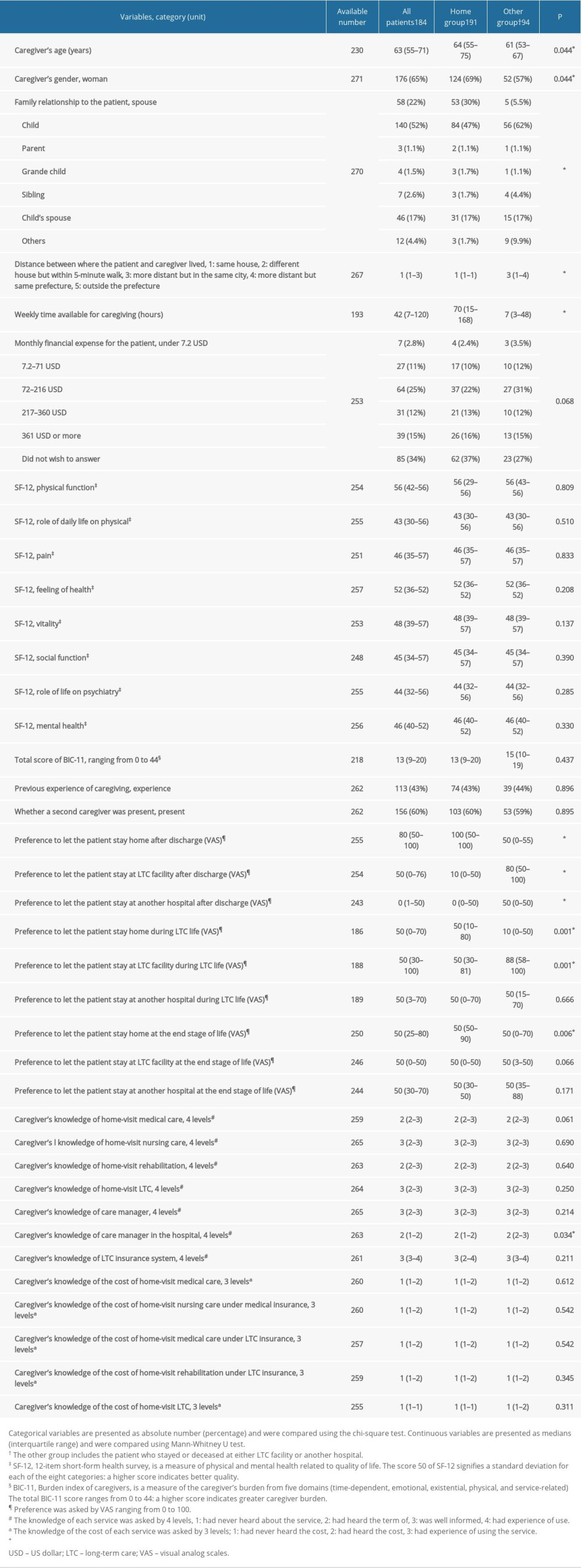 Table 4. Multivariable analysis with 4 covariables reportedly related to home discharge.
Table 4. Multivariable analysis with 4 covariables reportedly related to home discharge.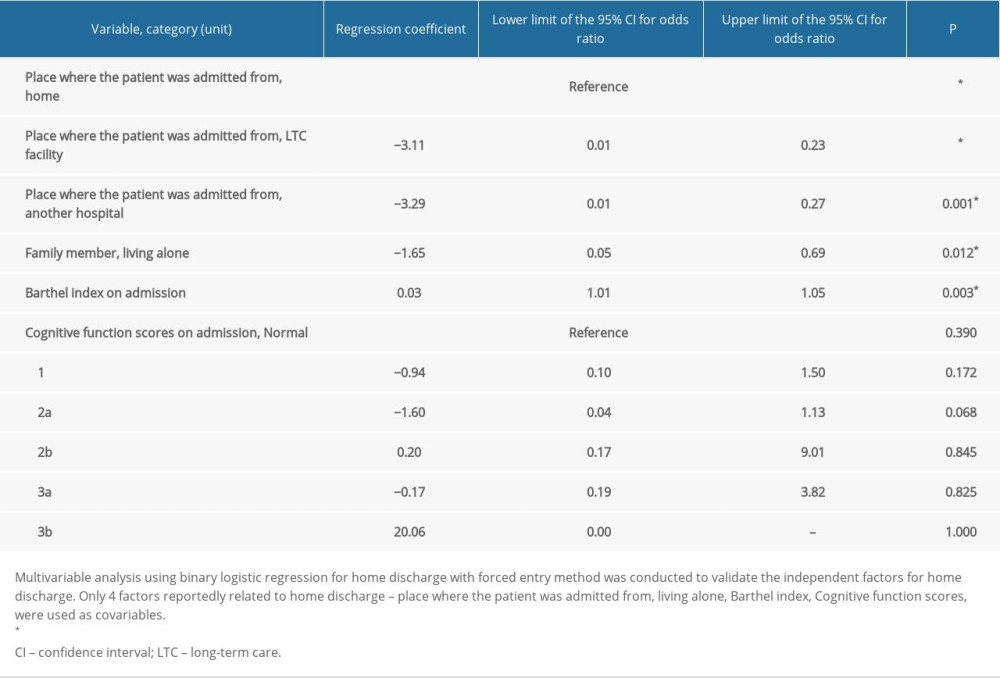 Table 5. Multivariable analysis using each factor adjusted by 4 covariables (on the side of patients).
Table 5. Multivariable analysis using each factor adjusted by 4 covariables (on the side of patients).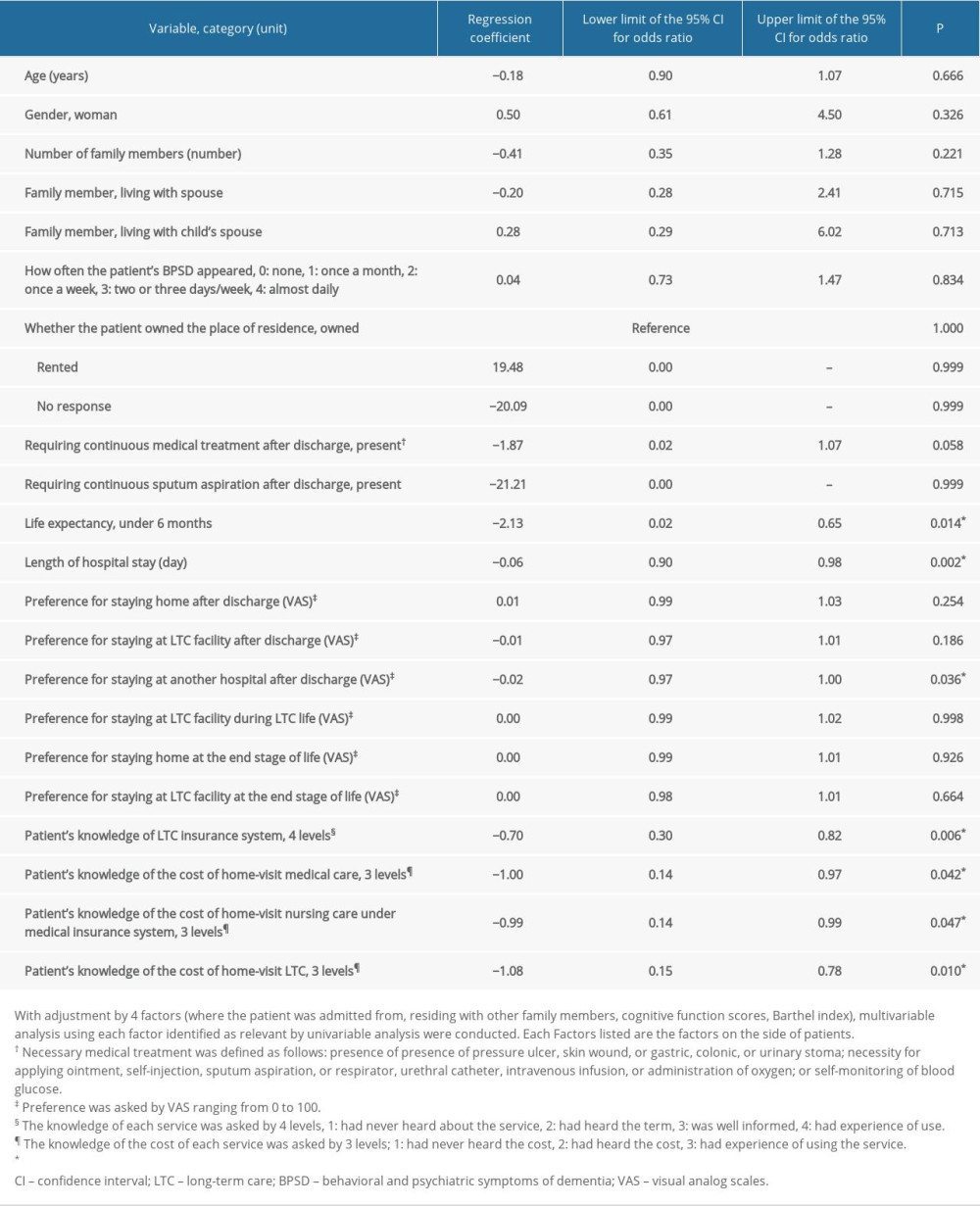 Table 6. Multivariable analysis using each factor adjusted by 4 covariables (on the side of caregivers).
Table 6. Multivariable analysis using each factor adjusted by 4 covariables (on the side of caregivers).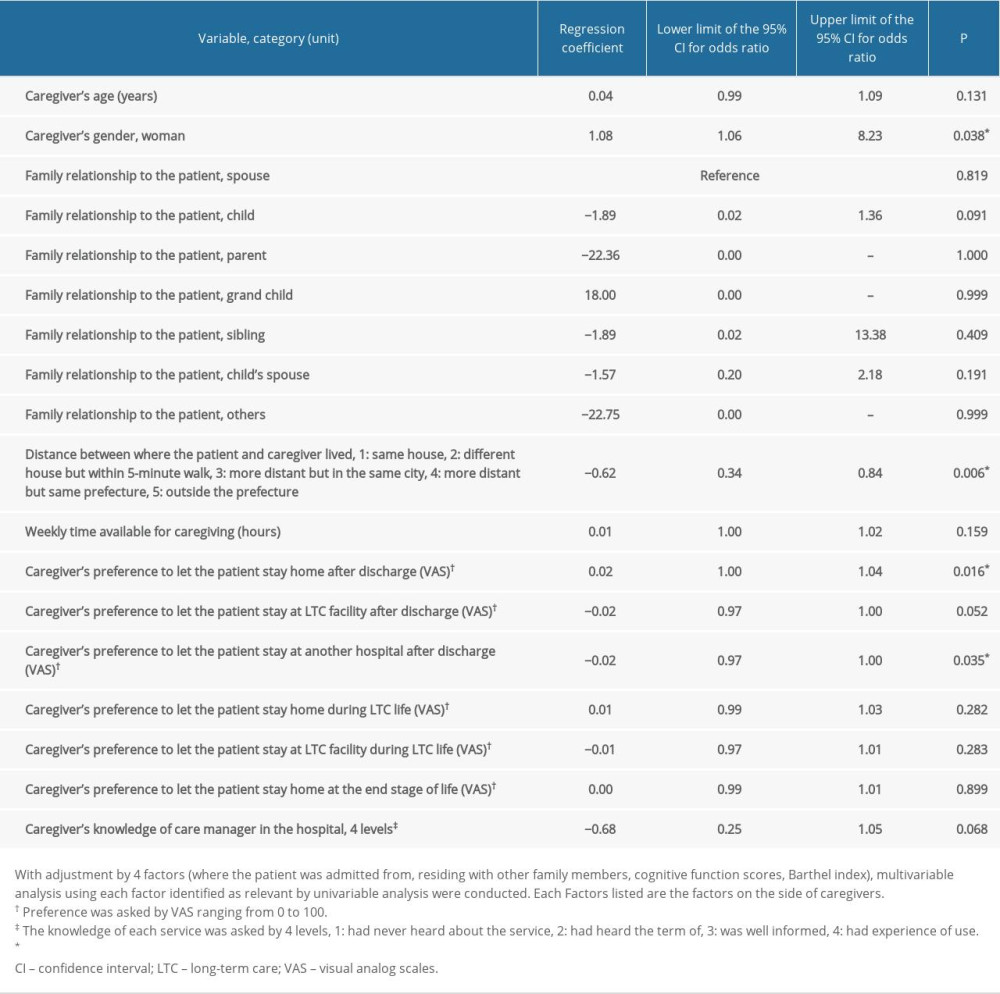
References
1. Organization for Economic Co-operation and Development National Institute (OECD): Elderly population, Demography, Statistics, OECD iLibrary. 1970–2021, 2022 [Cited 2022 Dec 16]. Available from: https://www.oecd-ilibrary.org/social-issues-migration-health/elderly-population/indicator/english_8d805ea1-en
2. : Cabinet office Japan 4 Aging by region, 1 Status of aging society, 1 Status of aging society, Annual report on the aging society FY2022 (in Japanese), 2022, Tokyo, The Institute [Cited 2022 Dec 19]. Available from: https://www8.cao.go.jp/kourei/whitepaper/w-2021/zenbun/pdf/1s1s_04.pdf
3. Organization for Economic Co-operation and Development National Institute (OECD): Insurance spending (Indicators), OECD data 2000–2020, 2022 [Cited 2022 Dec 19]. Available from: https://data.oecd.org/insurance/insurance-spending.htm
4. National institute of population and social security research Tokyo Japan 2021: The Financial statistics of social security in Japan Fiscal Year 2019 Aug, 2021 [Cited 2022 Dec 16]. Available from: https://www.ipss.go.jp/index-e.asp
5. Sakamoto H, Rahman M, Nomura S: Japan health system review, 2018, New Delhi, World Health Organization, Regional Office for South-East Asia Available from: https://apps.who.int/iris/handle/10665/259941
6. Japanese Ministry of Health, Labour and Welfare: Status of applicants for admission to special nursing homes for the elderly [in Japanese], 2019 [Cited 2022 Dec17] Available from: www.mhlw.go.jp/content/12304250/000581323.pdf
7. Japanese Ministry of Health, Labour and Welfare: Guideline for the establishment of regional medical care concept; attached to the notice from the chief of the Medical Policy Bureau, Ministry of Health, Labour and Welfare, Number 0331-57 dated March 31, 2017 [in Japanese] Mar, 2017 [Cited 2022 Dec17] Available from: https://www.mhlw.go.jp/stf/seisakunitsuite/bunya/0000080850.html
8. Tian W: An all-payer view of hospital discharge to postacute care, 2013: Statistical Brief# 205. Healthcare cos and utilization project May, 2016 Available from: https://www.ncbi.nlm.nih.gov/books/NBK373736
9. : The national statistics center (Japan) Table 34 Estimated number of patients discharged from hospital, place before admission × destination after discharge × hospital - clinic and type of bed, Patient survey, Portal site of official statistics of Japan (in Japanese) Mar, 2019 [Cited 2022 Dec 18]. Available from: https://www.e-stat.go.jp/dbview?sid=0003318594
10. The national statistics center (Japan): Table 5-5 Number of deaths by place of death by year, Deaths, Upper volume, Portal site of official statistics of Japan (in Japanese) Dec, 2022 [Cited 2022 Dec 17]. Available from: https://www.e-stat.go.jp/dbview?sid=0003411652
11. International Longevity Center Japan: The International comparison study on death and dying in place, 2012, Tokyo, The institute [Cited 2022 Dec 17]. Available from:https://www.ilcjapan.org/studyE/doc/End-of-life_Care2011.pdf
12. Shimogai T, P Izawa K, Kawada M, Factors affecting discharge to home of medical patients treated in an intensive care unit: Int J Environ Res Public Health, 2019; 16(22); 4324
13. McCann A, Sorensen J, Nally D, Discharge outcomes among elderly patients undergoing emergency abdominal surgery: Registry study of discharge data from Irish public hospitals: BMC Geriatr, 2020; 20(1); 72
14. Campbell SE, Seymour DG, Primrose WR, A multi-centre European study of factors affecting the discharge destination of older people admitted to hospital: Analysis of in-hospital data from the ACME plus project: Age Ageing, 2005; 34(5); 467-75
15. Everink IH, van Haastregt J, van Hoof SJ, Factors influencing home discharge after inpatient rehabilitation of older patients: A systematic review: BMC Geriatr, 2016; 16; 5
16. Agosti P, Tettamanti M, Vella F, Living alone as an independent predictor of prolonged length of hospital stay and non-home discharge in older patients: Eur J Intern Med, 2018; 57; 25-31
17. Sultana I, Erraguntla M, Kum HC, Post-acute care referral in United States of America: A multiregional study of factors associated with referral destination in a cohort of patients with coronary artery bypass graft or valve replacement: BMC Med Inform Decis Mak, 2019; 19(1); 223
18. Singh AB, Bronsert MR, Henderson WG, Accurate preoperative prediction of discharge destination using 8 predictor variables: A NSQIP analysis: J Am Coll Surg, 2020; 230(1); 64-75e2
19. Thornburgh Z, Samuel D, Factors influencing length of stay and discharge destination of patients with hip fracture rehabilitating in a private care setting: Geriatrics (Basel), 2022; 7(2); 44
20. The national statistics center (Japan): Main results by prefecture and municipality, Census, Portal site of official statistics of Japan [in Japanese] Jul, 2022 [Cited 2022 Dec 18]. Available from: https://www.e-stat.go.jp/stat-search/file-download?statInfId=000032143614&fileKind=0
21. Ishikawa Y, Fukui S, Saito T, Family preference for place of death mediates the relationship between patient preference and actual place of death: A nationwide retrospective cross-sectional study: PLoS One, 2013; 8(3); e56848
22. Costa V, Earle CC, Esplen MJ, The determinants of home and nursing home death: A systematic review and meta-analysis: BMC Palliat Care, 2016; 15; 1-15
23. Wahid AS, Sayma M, Jamshaid S, Barriers and facilitators influencing death at home: A meta-ethnography: Palliat Med, 2018; 32(2); 314-28
24. Mahoney FI, Barthel DW, Functional evaluation: The Barthel Index: Md State Med J, 1965; 14; 61-65
25. Yokobayashi K, Matsushima M, Watanabe T, Prospective cohort study of fever incidence and risk in elderly persons living at home: BMJ Open, 2014; 4; e004998
26. Tago M, Katsuki NE, Nakatani E, External validation of a new predictive model for falls among inpatients using the official Japanese ADL scale, Bedriddenness ranks: A double-centered prospective cohort study: BMC Geriatr, 2022; 22(1); 331
27. Ikegami N, Yamauchi K, Yamada Y, The long term care insurance law in Japan: Impact on institutional care facilities: Int J Geriatr Psychiatry, 2003; 18(3); 217-21
28. Shimizutani S: The future of long-term care in Japan, Discussion paper series 13-E-064, 2013, Tokyo, The research institute of economy, trade and industry (RIETI) [Cited 2022 Dec 17]. Available from: https://www.rieti.go.jp/jp/publications/dp/13e064.pdf
29. Hirakawa Y, Care manager as a medical information source for elderly people: Med Res Arch, 2016; 4(5); 12 [Cited 2022 Dec 17]
30. Itoh S, Mori T, Jeon B, Comparison of progression of care-need levels among long-term care recipients with and without advanced care management in a rural municipality of Japan: A population-based observational study: Int J Nurs Stud, 2021; 113; 103804
31. Ware J, Kosinski M, Keller SD, A 12-Item Short-Form Health Survey: Construction of scales and preliminary tests of reliability and validity: Med Care, 1996; 34(3); 220-33
32. Miyashita M, Yamaguchi A, Kayama M, Validation of the Burden Index of Caregivers (BIC), a multidimensional short care burden scale from Japan: Health Qual Life Outcomes, 2006; 4; 52
33. Huang ST, Chen CM, Su YY, Retrospective evaluation of discharge planning linked to a long-term care 2.0 project in a medical center: Int J Environ Res Public Health, 2022; 19(16); 10139
34. Tang F, Pickard JG, Aging in place or relocation: Perceived awareness of community-based long-term care and services: J Hous Elderly, 2008; 22(4); 404-22
35. Willert B, Minnotte KL, Informal caregiving and strains: Exploring the impacts of gender, race, and income: Appl Res Qual Life, 2021; 16; 943-64
36. King D, Pickard L, When is a carer’s employment at risk? Longitudinal analysis of unpaid care and employment in midlife in England: Health Soc Care Community, 2013; 21(3); 303-14
37. Ministry of foreign affairs of Japan: 39 Public opinion survey on a gender-equal society (regarding the concept of “men at work and women at home”), Statistical annex, Fifth periodic report on implementation of convention on the elimination of all forms of discrimination against women (Japan) Sep, 2002 [Cited by 2022 Dec 17]. Available from: https://www.mofa.go.jp/policy/human/women_rep5/039.html
38. Organization for Economic Co-operation and Development National Institute (OECD) 2022: Time spent in paid and unpaid work, by sex, Employment, Gender, Social protection and well-being Dec, 2022 [Cited 2022 Dec 19]. Available from: https://stats.oecd.org/index.aspx?queryid=54757
39. Falzarano FB, Cimarolli V, Boerner K, Use of home care services reduces care-related strain in long-distance caregivers: Gerontologist, 2022; 62(2); 252-61
40. Alonso-Babarro A, Bruera E, Varela-Cerdeira M, Can this patient be discharged home? Factors associated with at-home death among patients with cancer: J Clin Oncol, 2011; 29(9); 1159-67
41. Driesen BEJM, Van Riet BHG, Verkerk L, Long length of stay at the emergency department is mostly caused by organisational factors outside the influence of the emergency department: A root cause analysis: PLoS One, 2018; 13(9); e0202751
42. Langhorne P, Taylor G, Murray G, Early supported discharge services for stroke patients: A meta-analysis of individual patients’ data: Lancet, 2005; 365(9458); 501-6
43. Tung YJ, Huang CT, Lin WC, Longer length of post-acute care stay causes greater functional improvements in poststroke patients: Medicine (Baltimore), 2021; 100(26); e26564
44. Takeu RA review of articles about factors association with death at home and death at hospital since1990 in Japan: Journal of Japan Academy of Community Health Nursing, 2008; 11(1); 87-92 [in Japanese]
45. Ishikawa MThe ratio of home deaths and related factors in national municipalities, ecological study: Journal of Japanese Association for Health Care Administrators, 2018; 12(1); 15-19 [in Japanese]
Tables
 Table 1. Comparison between the Home group and the Other group concerning the factors on the side of the patient.
Table 1. Comparison between the Home group and the Other group concerning the factors on the side of the patient. Table 2. Top 10 main diagnoses.
Table 2. Top 10 main diagnoses. Table 3. Comparison between the Home group and the Other group concerning the factors on the side of patient’s caregiver.
Table 3. Comparison between the Home group and the Other group concerning the factors on the side of patient’s caregiver. Table 4. Multivariable analysis with 4 covariables reportedly related to home discharge.
Table 4. Multivariable analysis with 4 covariables reportedly related to home discharge. Table 5. Multivariable analysis using each factor adjusted by 4 covariables (on the side of patients).
Table 5. Multivariable analysis using each factor adjusted by 4 covariables (on the side of patients). Table 6. Multivariable analysis using each factor adjusted by 4 covariables (on the side of caregivers).
Table 6. Multivariable analysis using each factor adjusted by 4 covariables (on the side of caregivers). Table 1. Comparison between the Home group and the Other group concerning the factors on the side of the patient.
Table 1. Comparison between the Home group and the Other group concerning the factors on the side of the patient. Table 2. Top 10 main diagnoses.
Table 2. Top 10 main diagnoses. Table 3. Comparison between the Home group and the Other group concerning the factors on the side of patient’s caregiver.
Table 3. Comparison between the Home group and the Other group concerning the factors on the side of patient’s caregiver. Table 4. Multivariable analysis with 4 covariables reportedly related to home discharge.
Table 4. Multivariable analysis with 4 covariables reportedly related to home discharge. Table 5. Multivariable analysis using each factor adjusted by 4 covariables (on the side of patients).
Table 5. Multivariable analysis using each factor adjusted by 4 covariables (on the side of patients). Table 6. Multivariable analysis using each factor adjusted by 4 covariables (on the side of caregivers).
Table 6. Multivariable analysis using each factor adjusted by 4 covariables (on the side of caregivers). In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387