12 July 2020: Review Articles
The Role of Imaging Techniques in Management of COVID-19 in China: From Diagnosis to Monitoring and Follow-Up
Zhen-zhen Jiang1ABE, Cong He2BDE, De-qing Wang3BCD, Hua-liang Shen1BF, Jia-li Sun1BDF, Wan-ni Gan1DF, Jia-ying Lu1DF, Xia-tian Liu1ADE*DOI: 10.12659/MSM.924582
Med Sci Monit 2020; 26:e924582
Abstract
ABSTRACT: In December 2019, an outbreak of coronavirus infection emerged in Wuhan, Hubei Province of China, which is now named Coronavirus Disease 2019 (COVID-19). The outbreak spread rapidly within mainland China and globally. This paper reviews the different imaging modalities used in the diagnosis and treatment process of COVID-19, such as chest radiography, computerized tomography (CT) scan, ultrasound examination, and positron emission tomography (PET/CT) scan. A chest radiograph is not recommended as a first-line imaging modality for COVID-19 infection due to its lack of sensitivity, especially in the early stages of infection. Chest CT imaging is reported to be a more reliable, rapid, and practical method for diagnosis of COVID-19, and it can assess the severity of the disease and follow up the disease time course. Ultrasound, on the other hand, is portable and involves no radiation, and thus can be used in critically ill patients to assess cardiorespiratory function, guide mechanical ventilation, and identify the presence of deep venous thrombosis and secondary pulmonary thromboembolism. Supplementary information can be provided by PET/CT. In the absence of vaccines and treatments for COVID-19, prompt diagnosis and appropriate treatment are essential. Therefore, it is important to exploit the advantages of different imaging modalities in the fight against COVID-19.
Keywords: COVID-19, Diagnostic Imaging, Therapeutics, Betacoronavirus, COVID-19, COVID-19 Testing, Clinical Laboratory Techniques, Coronavirus Infections, Diagnosis, Differential, Follow-Up Studies, Lung Diseases, Interstitial, Pandemics, Pneumonia, Viral, Positron Emission Tomography Computed Tomography, Radiography, Thoracic, Reverse Transcriptase Polymerase Chain Reaction, SARS-CoV-2, Sensitivity and Specificity, Tomography, X-Ray Computed, Ultrasonography
Background
On 29 December 2019, a cluster of severe acute respiratory infections of unknown etiology was first reported in Wuhan, Hubei province, China [1]. Later, the infection rapidly spread to other regions of China and several other countries [2,3]. Scientists in China were able to quickly identify that the new coronavirus, which was later named severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) by the International Committee on Taxonomy of Viruses (ICTV), was responsible for the outbreak of novel coronavirus pneumonia (NCP) [4]. On 11 January 2020, the World Health Organization (WHO) officially named the disease Coronavirus Disease 2019 (COVID-19) [5]. By 18 March 2020, COVID-19 had spread to many countries around the world, resulting in 191 127 confirmed cases and 7807 deaths [6]. However, after numerous efforts by the Chinese government, public health agencies, and clinicians, the epidemic curve of the new cases in China peaked on February 12–13, after which it began to decline, suggesting that the number of new cases was falling [7]. Now, the number of new daily cases is lower than the number of daily discharged cases in China. Imaging plays an important role in the management of COVID-19. This paper aims to provide a timely review of various imaging modalities in use in the diagnosis and treatment process of COVID-19, including chest radiographs, computerized tomography (CT) scan, ultrasound examination, and positron emission tomography (PET/CT) scan.
Diagnosis of COVID-19
The National Health Commission of the People’s Republic of China recommends a set of clinical criteria requiring that suspected patients meet at least 1 of the 4 epidemiological histories and 2 clinical manifestations. However, if there is no clear epidemiological history, the case must meet at least 3 of the following clinical manifestations [8]: (1) Epidemiological history of travel or residence in Wuhan City, Hubei Province, China within 14 days before the onset of signs and symptoms; (2) History of exposure to confirmed cases within 14 days before the onset of symptoms; (3) History of contact with people who have fever/respiratory symptoms from Wuhan or surrounding districts or clustered onsets; (4) Clinical manifestations of fever and/or respiratory symptoms; (5) Typical imaging characteristics of COVID-19 pneumonia; and (6) Normal or reduced white blood cell counts and reduced lymphocyte counts in the early stages of onset. Suspected cases are confirmed based on the presence of coronavirus nucleic acid with positive real-time fluorescent RT-PCR detection or viral gene sequencing that is highly homologous to the new coronaviruses.
RT-PCR is recognized as the criterion standard for the molecular diagnosis of COVID-19, but it produces many false-negative results. In the detection of COVID-19 infection, lower-respiratory tract samples have higher diagnostic value than upper-respiratory tract samples [9], but lower-respiratory tract sampling (e.g., using alveolar lavage fluid) is difficult. Sampling errors and low viral load limit the accuracy of RT-PCR [10]. In addition, it is time-consuming and a shortage of viral testing kits due to the epidemic also limit the application of RT-PCR [11]. Some patients may be unable to get timely diagnosis and treatment in the early stage, which may increase the spread of the epidemic. Therefore, some Chinese experts recommend use of imaging in the diagnosis of COVID-19 [12], which allows early identification, isolation, and intervention for infected patients, which could help control the sources of infection and reduce the infection rate.
Pathological Findings
Pathological changes form the basis of imaging in diagnosis. Biopsy samples taken from the lungs of patients with COVID-19 infection show diffuse pulmonary alveolar damage. The inflammatory lesions revealed alveolar edema and hyaline membrane formation, which are associated with acute respiratory distress syndrome (ARDS) [13]. The pathological findings of COVID-19 are similar to those previously reported in severe acute respiratory syndrome (SARS) and Middle Eastern respiratory syndrome (MERS) coronavirus infections [14,15]. However, gross anatomical observations showed that pulmonary fibrosis and consolidation in COVID-19 patients were not as severe as those reported in SARS patients, but the exudation response in COVID-19 is more obvious [16]. The pathological findings are consistent with the image changes. At the early stage of COVID-19 infection, a wide range of pulmonary interstitial inflammation with numerous infiltrating plasma cells and macrophages may be the pathological basis for ground-glass opacities (GGOs) [17]. With the progression of the lesions, a large amount of inflammatory exudate accumulates in the alveolar cavity, which increases the alveoli and interstitial edema. Cellulose-like exudate connects the alveolar and form consolidation. Type II pneumocyte hyperplasia and inflammatory cell infiltration of the alveolar wall lead to reticular interlobular septal thickening in CT examination [18]. Pathological findings provide new insights into the pathogenesis of COVID-19 infection, which can be useful in developing novel therapeutic strategies aimed at reducing the mortality rate.
Chest Radiography
Chest radiography showed no abnormalities in early-stage COVID-19 infection (Figure 1A). Therefore, radiography was not recommended as the first-line modality in screening suspected COVID-19 patients [19]. However, chest radiography in mild COVID-19 infections showed local patchy shadows in the outer band and subpleural area of the lungs (Figure 1B). Multiple consolidations were found in severe cases, where some fused into large patches, with small amounts of pleural effusion detected. In critically ill patients, diffuse consolidation shadows present as “white lung” [20]. For critically ill patients (especially those who had endotracheal intubation), a bedside digital radiography can be used as an important review tool to determine the severity of infection [12].
Chest CT Images
IMAGING FEATURES:
Chest CT examination, especially chest CT volume scanning with thin-layer reconstruction, is currently being used as the first-line imaging modality in the diagnosis of COVID-19 in China [12,20]. The most commonly reported CT findings in COVID-19 include: (1) GGOs, consolidation, or both, with a peripheral and basal distribution in the bilateral lungs and often with reticular interlobular septal thickening (known as crazy-paving pattern) (Figure 2); (2) Bronchial wall thickening and air bronchogram signs occur in a proportion of patients (Figure 3); and (3) Signs of pleural effusion, pericardial effusion, and lymphadenopathy are relatively rare [19,21–23]. There were notable differences in CT findings between COVID-19-infected children and adults. Most pediatric lesions were relatively limited and GGOs were smaller [24]. A paving pattern is rarely seen in children, but there may be bronchopneumonia-like changes in the lungs. Epidemiological history and clinical manifestations were more helpful in the diagnosis of COVID-19 infection in children versus chest CT [25].
DIFFERENTIATING BETWEEN COVID-19 PNEUMONIA AND OTHER KINDS OF PNEUMONIA:
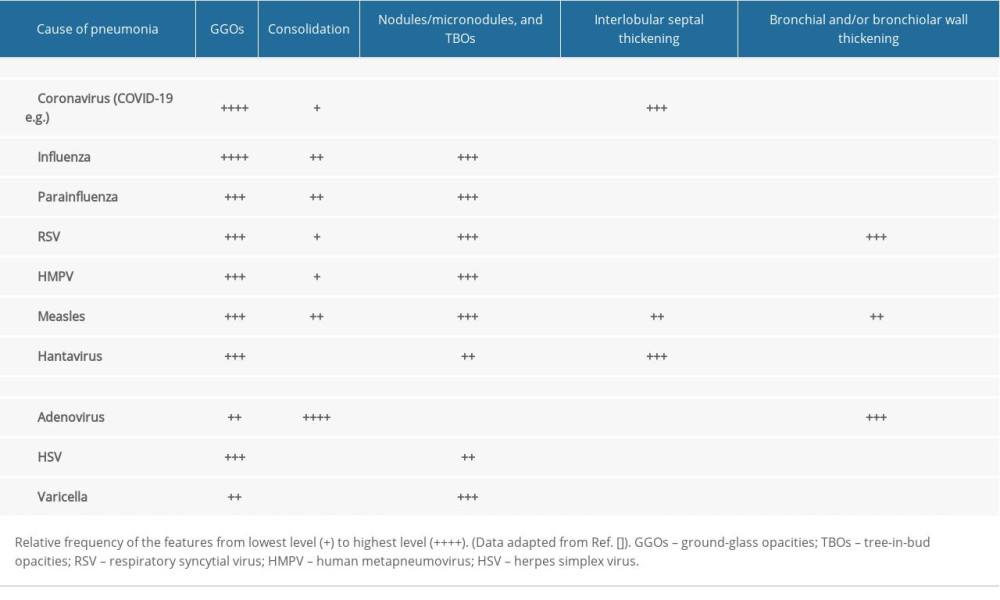
It is important to distinguish COVID-19 pneumonia from other viral pneumonia (such as influenza pneumonia, parainfluenza pneumonia, SARS and adenovirus pneumonia), mycoplasma pneumonia, and bacterial pneumonia. CT manifestations of bacterial pneumonia are patchy shadows distributed along the bronchi, which can be merged into a large-lobe lesion or consolidation. Coupled with the increase in white blood cells, laboratory tests can be used to distinguish COVID-19 pneumonia [19]. Pneumonias caused by different viruses share similar CT features, so differential diagnosis by CT images is difficult. Table 1 summarizes CT findings in different viral pneumonias [26]. Compared with non-COVID-19 pneumonia, COVID-19 pneumonia was more likely to have a peripheral distribution GGOs and reticular interlobular septal thickening, but less likely to have central distributions, pleural effusion, and lymphadenopathy [27]. Travel or residence in Wuhan or close contact with confirmed/suspected patients can provide an essential clue for the diagnosis of COVID-19 pneumonia. The diagnosis must be confirmed by nucleic acid testing or viral gene sequencing.
CLINICAL APPLICATION VALUES:
RT-PCR testing was reported to have high specificity but its sensitivity was low, at only 59–70% [11,28]. This means that excluding a suspected case of COVID-19 infection requires multiple negative results. RT-PCR testing is time-consuming and this increases the risk of spread in the population due to the highly contagious nature of COVID-19. CT examination is relatively easy to perform and can thus provide a quick diagnosis. In most COVID-19 confirmed cases, typical CT imaging findings were reported [11]. Typical CT imaging findings were observed in symptomatic patients with negative RT-PCR results [29,30]. Even asymptomatic patients could have positive CT images and these could be the basis for imaging assist in early diagnosis [31]. Jiang et al. reported the CT imaging features of 17 asymptomatic health care workers diagnosed with COVID-19 infection by RT-PCR. The study revealed that all the health care workers had a history of close contact with COVID-19 patients and their CT images were positive for COVID-19 [32]. The lesions in patients receiving treatment reduced in size while those in patients not receiving treatment were enlarged. In a study of 1014 patients, the results showed that 59% had positive RT-PCR results and 88% had positive CT results. The sensitivity of CT in identifying COVID-19 was 97% [28], which indicates that CT examination is a reliable, practical, and rapid method in the diagnosis of COVID-19, especially in epidemic areas where the focus is rapid detection with high sensitivity.
In addition to aiding in diagnosis at an early stage, CT examination can also be used to assess the severity of the disease. Patients with RT-PCR-confirmed COVID-19 and normal chest CT were usually mild cases rather than severe cases, suggesting that CT images can predict the outcome of patients. Wu et al. performed a semi-quantitative analysis of the pulmonary lesions in patients with COVID-19 and found that the pulmonary lesion index values were significantly correlated with the values of the main clinical symptoms and inflammatory markers [23]. There was a significantly higher incidence rate of consolidations, crazy-paving pattern, and bronchial wall thickening in severe and critical patients than in mild patients [33].
Also, during the treatment process, CT can be used to follow the disease time course and quickly detect lung complications. The number, range, and density of GGOs are reported to increase as the disease progresses [29,34], while smaller size, range, and absorption of GGOs or consolidation indicated improved disease condition [35, 36]. CT manifestations can be divided into early stage, advanced stage, critical stage, and involuted stage based on lesion extension and severity [12]. Pan et al. revealed that in early-stage disease, CT images in approximately 50% of patients had peripheral lung opacities. The GGOs developed rapidly, demonstrating crazy-paving and/or consolidation involving multiple lobes (Figure 4). In patients without ARDS, chest CT showed that lesions were most severe about 10 days after the onset, which then began to improve [37]. A subset of patients whose CT imaging showed multiple lobular lesions or progression of lesion focus within 48 h ≥50% indicated critical stage and the need for Intensive Care Unit (ICU) monitoring and treatment [38].
CT imaging has specific limitations. Because COVID-19 patients with RT-PCR-confirmed infection can also have normal CT findings, constant vigilance is needed to identify COVID-19 patients who may be asymptomatic with normal chest CT findings and/or even negative initial PR-PCT results [39]. Considering the financial cost and repeated exposure to ionizing radiation involved in CT examination, a more thorough analysis is needed. A dedicated CT scanner room, examination waiting area, and a special pathway for COVID-19-infected patients is essential to avoid cross-infection [40].
Ultrasound Examination
FOUNDATION FOR CLINICAL APPLICATIONS:
Ultrasound is one of the most commonly used imaging modalities in clinical practice, providing systematic and rapid examinations of multiple organs at the bedside without use of radiation. Initially, ultrasound was thought to be incapable of detecting lung lesions. However, since the 1990s, lung ultrasound has been applied in a wide range of clinically critical conditions [41]. Basic signs of lung ultrasound can be described as A-lines, B-lines, subpleural consolidation, and lung sliding sign [42]. For COVID-19-infected cases, pulmonary lesions predominantly appeared in peripheral areas of the lung and subpleural regions of both lungs [30]. This makes it possible for an ultrasound to detect subpleural abnormalities [43]. However, deeply located lung lesions cannot be detected by ultrasound, and it is difficult for ultrasound to be used in the differential diagnosis of pneumonia. Ultrasound is not recommended in the diagnosis of mild cases. It can be used as a supplementary method in pulmonary and cardiac evaluation, especially in critically ill patients who should not be moved and for whom CT examination is impossible [44].
APPLICATIONS OF CRITICAL ULTRASONOGRAPHY:
Some COVID-19-infected patients progress to severe or critical condition [45]. Ultrasonography is particularly important in examining critically ill patients and in determining the direction of treatments, especially hemodynamic therapy [46,47]. It focuses on functional imaging rather than anatomical imaging and its applications can be summarized as follows.
Firstly, an ultrasound examination can be used as an imaging modality in the rapid assessment of illness. A critical consultation ultrasonic examination (CCUE) is recommended in COVID-19-infected patients with symptoms of dyspnea or circulation fluctuation, for prompt analysis of possible complications. An increase in the number of B-lines and the area of the consolidation may suggest progression of the lung disease. Otherwise, changes in the heart size and ventricular wall thickness, segmental wall motion abnormalities, and decreased ventricular contractile function could indicate heart injury [48].
Secondly, respiratory support is essential in severe and critical cases, but the time point to switch from noninvasive ventilation to invasive mechanical ventilation is a major issue among clinicians [49]. Lung ultrasound showing progressive diffuse fusion B-line and the presence of significantly enhanced diaphragm activity can be an indication of severe lung damage. Combined with the oxygenation index, shifting from noninvasive ventilation to invasive mechanical ventilation is likely to occur earlier [50]. After invasive ventilation, ultrasound can help monitor the process of lung recruitment maneuver while preventing lung injuries caused by mechanical ventilation [51]. Weaning is a critical part of mechanical ventilation for COVID-19-infected patients. Systematic ultrasound evaluation of lung, heart, and diaphragm function before and after weaning can help to avoid weaning failure or even re-injury caused by failed extubation, which can reduce the mortality rate and the risk of medical staff infection [52]. When mechanical ventilation cannot improve oxygenation, extracorporeal membrane oxygenation (ECMO) can be a treatment option [53]. Ultrasound enables visual management in the process of ECMO.
Thirdly, echocardiography can be used to assess circulation functions. The most commonly reported complication of COVID-19 critical patients is ARDS, followed by acute heart injury and secondary infection [38]. Elevated troponin levels occur in COVID-19 patients at the early stages of onset, suggesting viral myocardial damage [50], but this needs to be confirmed by additional study, such as monitoring hemodynamic changes. The use of floating catheters and central venous pressure monitoring is limited by the environment of epidemic areas. The 7th Diagnosis & Treatment Scheme published in China has recommended Doppler ultrasound and echocardiography as noninvasive means for the evaluation of hemodynamics [8]. Echocardiography can quickly evaluate hemodynamics and identify whether there are segmental wall motion abnormalities [54], stress-induced cardiomyopathy, or acute right heart dysfunction [55], which could guide treatment.
Finally, coagulation abnormalities have been reported in approximately 20% of severe and critically ill COVID-19 patients [35,38]. Sudden deterioration in condition, often accompanied by a dramatic elevation in D-dimer, suggests a hypercoagulable state [56]. For patients who stay in bed for more than 3 days, the symptom of asymmetrical pain, swelling, or discomfort of unilateral/bilateral lower limbs can indicate the risk of lower-limb deep vein thrombosis (DVT). For patients with central venous catheters, local swelling of the catheterized limbs can indicate the risk of upper-limb DVT. Secondary pulmonary thromboembolism should also be watched for [57]. It is proposed that all hospitalized patients undergo ultrasound examinations of the circulation (including intermuscular veins) to detect a thrombus and define its scope and nature [44]. This way, effective and timely interventions can be provided for patients who are at high risk for embolism.
PET/CT Examination
18F-FDG PET/CT is not recommended for routine diagnosis in emergency settings, but in early-stage COVID-19, PET/CT has potential clinical utility in the differential diagnosis of complex cases. A case series illustrated the PET/CT findings of patients with ARDS caused by COVID-19 infection [58]. The study reported that all patients had peripheral GGOs and/or lung consolidations in multiple pulmonary lobes. Pulmonary lesions were characterized by high 18F-FDG uptake, which reflected the inflammatory burden. It is similar to PET/CT images of respiratory syndrome and MERS coronaviruses infections [59,60]. 18F-FDG uptakes were higher in involved lymph nodes, which was not revealed by other imaging modalities [20,61]. There were no disseminated lesions in other body parts, indicating that this coronavirus exhibited pulmonary tropism. It was also reported that PET/CT lung ventilation and perfusion scanning can provide accurate imaging of regional lung function [62]. Radioisotope scanning could possibly be used in the evaluation of lung function in COVID-19 pneumonia. However, it is worth noting that a long PET/CT procedure might increase the risk of virus spreading [63].
Diagnostic Performance of Various Imaging Modalities in Detecting COVID-19 Pneumonia
The reported sensitivities and specificities of CT in detecting COVID-19 pneumonia varied from 67–98% and 24–94%, respectively [11,28,64–66]. As reported by Raptis et al., the sensitivities may be overestimated by patient selection bias and the lack of detailed definition of positive CT findings [67]. The specificities may also be overestimated due to the lack of singular image features unique to COVID-19 and lack of objective criteria for the definition of positive CT results [64]. There is little research on the diagnostic performance of detecting various stages of COVID-19 infection. However, a recent study showed the sensitivity and specificity of CT visual quantitative analysis in diagnosing severe-critical cases were 82.6% and 100%, respectively, indicating its potential to reflect the clinical classification of COVID-19 [68].
Regarding the diagnostic performance of lung ultrasonography, the ultrasound scores in diagnosis of mild, moderate, and severe lung lesions exhibited a sensitivity of 68.8%, 77.8%, and 100.0%, a specificity of 85.7%, 76.2%, and 92.9%, and diagnostic accuracy of 76.7%, 76.7%, and 93.3%, respectively [69]. These results indicate that ultrasound diagnostic efficacy is relatively low for mild to moderate cases but high for severe cases. There is no relevant research reported on the diagnostic performance of chest radiography and PET/CT examination.
Conclusions
In summary, this paper compares various imaging modalities being used in the management of COVID-19 in China. The advantage and disadvantage of each imaging modality in detecting lesions can be summarized as below: (1) Chest radiography shows no abnormalities in early-stage COVID-19 but could be used as a screening tool in patients who are not allowed to be transferred for CT examination; (2) Chest CT is a reliable, fast, and practical imaging modality for management of COVID-19 in China, although the financial cost and repeated exposure to ionizing radiation should be considered; (3) Deeply located lung lesions cannot be detected by ultrasound, but it could be used in critically ill patients to assess cardiorespiratory function, help in respiratory support, and identify the presence of deep venous thrombosis; and (4) PET/CT provides supplementary information beyond that provided by other imaging modalities. It is important to exploit the advantages of various imaging modalities in the fight against COVID-19.
Figures
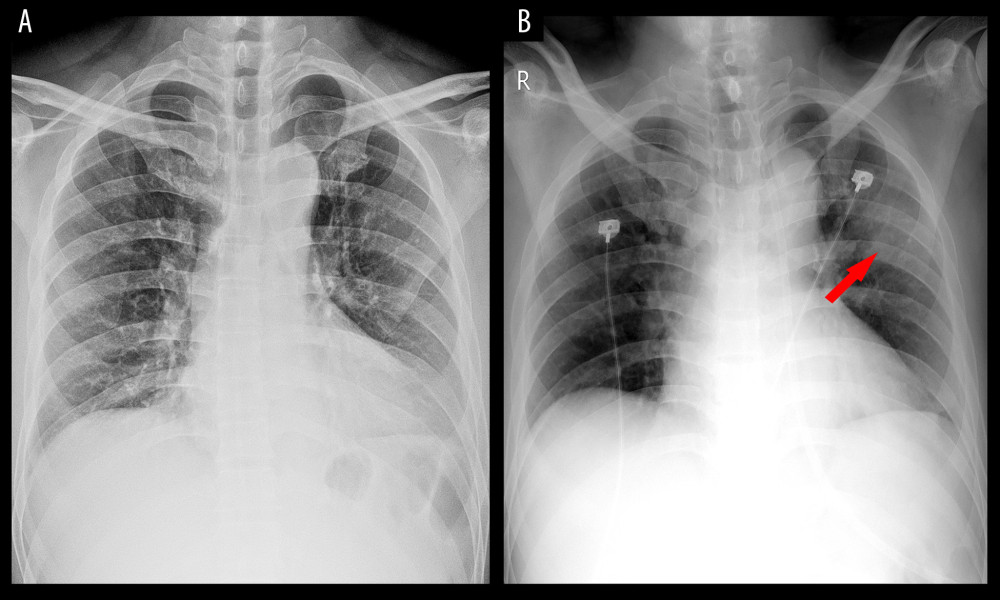 Figure 1. Chest radiography image of a COVID-19-infected patient. A 50-year-old man with a 2-day history of fever and cough. At first, there was no abnormality in the chest radiography image except for a mild enlarged cardiac shadow (A). Two days later, a local patchy shadow was found in the outer band of the left lung (arrow) (B).
Figure 1. Chest radiography image of a COVID-19-infected patient. A 50-year-old man with a 2-day history of fever and cough. At first, there was no abnormality in the chest radiography image except for a mild enlarged cardiac shadow (A). Two days later, a local patchy shadow was found in the outer band of the left lung (arrow) (B). 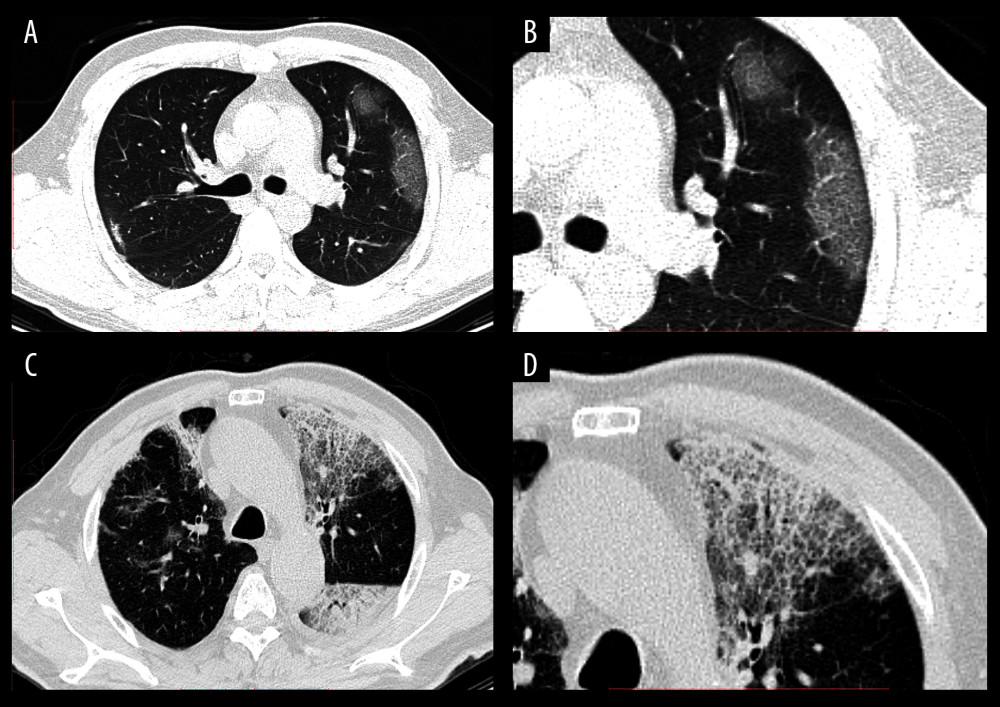 Figure 2. CT images of confirmed COVID-19-infected patients. (A) A 37-year-old man with a 3-day history of fever and cough. The chest CT image showed GGOs with peripheral distribution in the lung. (B) Local amplification of the GGOs. (C) A 70-year-old man with a history of type 2 diabetes mellitus and hypertension. On the seventh day after coming back from Wuhan, he had fever and cough. Reticular interlobular septal thickening and typical crazy-paving pattern were shown by chest CT images. (D) Local amplification of crazy-paving pattern.
Figure 2. CT images of confirmed COVID-19-infected patients. (A) A 37-year-old man with a 3-day history of fever and cough. The chest CT image showed GGOs with peripheral distribution in the lung. (B) Local amplification of the GGOs. (C) A 70-year-old man with a history of type 2 diabetes mellitus and hypertension. On the seventh day after coming back from Wuhan, he had fever and cough. Reticular interlobular septal thickening and typical crazy-paving pattern were shown by chest CT images. (D) Local amplification of crazy-paving pattern. 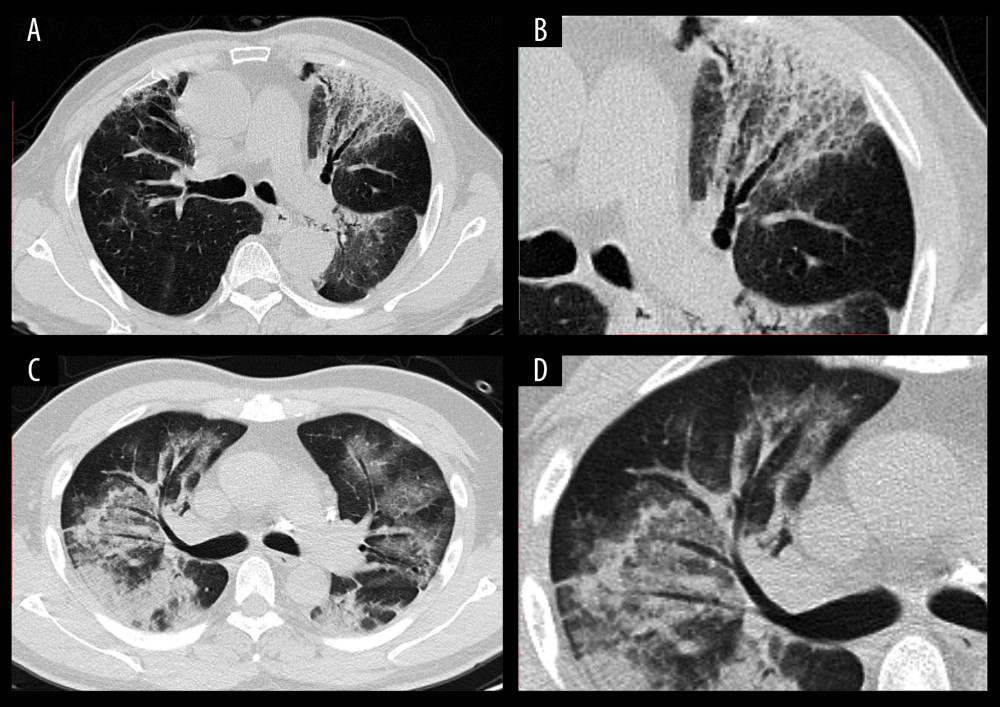 Figure 3. CT images of confirmed COVID-19-infected patients. (A) A 70-year-old man with fever (38.5°C), cough for three days, and had a travel history of Wuhan City. Chest CT displayed patchy GGOs with bronchial wall thickening in the left upper field. (B) Local amplification of the bronchial wall thickening. (C) A 50-year-old male with a residence history of Wuhan City. He had his first visit to our hospital on January 25, 2020, because he had a fever and cough for two days. Chest CT acquired on February 1, 2020, showed multiple subpleural distributed GGOs with consolidation lesions. An air bronchogram sign could be found in the right lung lobe. (D) Local amplification of the air bronchogram sign.
Figure 3. CT images of confirmed COVID-19-infected patients. (A) A 70-year-old man with fever (38.5°C), cough for three days, and had a travel history of Wuhan City. Chest CT displayed patchy GGOs with bronchial wall thickening in the left upper field. (B) Local amplification of the bronchial wall thickening. (C) A 50-year-old male with a residence history of Wuhan City. He had his first visit to our hospital on January 25, 2020, because he had a fever and cough for two days. Chest CT acquired on February 1, 2020, showed multiple subpleural distributed GGOs with consolidation lesions. An air bronchogram sign could be found in the right lung lobe. (D) Local amplification of the air bronchogram sign. 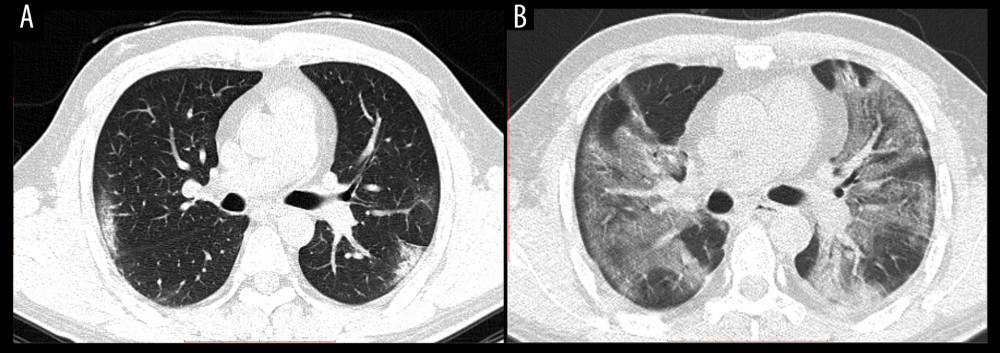 Figure 4. A 37-year-old man with a 3-day history of fever and cough. He had a history of close contact with COVID-19 confirmed cases and later he was confirmed to be COVID-19-infected by RT-PCR. (A) The first chest CT acquired on February 12, 2020, showed small GGOs in the bilateral lungs. (B) Eight days later, follow-up chest CT showed the GGOs developed rapidly. The size and range of the lesions increased, which indicated the deterioration of the disease.
Figure 4. A 37-year-old man with a 3-day history of fever and cough. He had a history of close contact with COVID-19 confirmed cases and later he was confirmed to be COVID-19-infected by RT-PCR. (A) The first chest CT acquired on February 12, 2020, showed small GGOs in the bilateral lungs. (B) Eight days later, follow-up chest CT showed the GGOs developed rapidly. The size and range of the lesions increased, which indicated the deterioration of the disease. References
1. Epidemic Response: Urgent research agenda for the novel coronavirus epidemic: Transmission and non-pharmaceutical mitigation strategies: Zhonghua Liu Xing Bing Xue Za Zhi, 2020; 41(2); 135-38
2. Phan LT, Nguyen TV, Luong QC, Importation and human-to-human transmission of a novel coronavirus in Vietnam: N Engl J Med, 2020; 382(9); 872-74
3. Wong JEL, Leo YS, Tan CC, COVID-19 in Singapore – current experience: Critical global issues that require attention and action: JAMA, 2020 [Online ahead of print]
4. Zhu N, Zhang D, Wang W, A novel coronavirus from patients with pneumonia in China, 2019: N Engl J Med, 2020; 382(8); 727-33
5. WHO: WHO Director-General’s remarks at the media briefing on 2019-nCoV on 2020 https://www.who.int/dg/speeches/detail/who-director-general-s-remarks-at-the-media-briefing-on-2019-ncov-on-11-february-2020
6. WHO, Coronavirus disease (COVID-2019) situation reports: Situation report – 58, 2020 https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200318-sitrep-58-covid-19.pdf?sfvrsn=20876712_2
7. Deng SQ, Peng HJ, Characteristics of and public health responses to the coronavirus disease 2019 outbreak in China: J Clin Med, 2020; 9(2); 575
8. , Medicine: NHCotPsRoCaNAoTC: Diagnosis & treatment scheme for novel coronavirus pneumonia (trial), 2020 http://www.nhc.gov.cn/xcs/zhengcwj/202003/46c9294a7dfe4cef80dc7f5912eb1989/files/ce3e6945832a438eaae415350a8ce964.pdf
9. Charlton CL, Babady E, Ginocchio CC, Practical guidance for clinical microbiology laboratories: Viruses causing acute respiratory tract infections: Clin Microbiol Rev, 2019; 32(1); e00042
10. Mo X, Qin W, Fu Q, Guan MUnderstanding the influence factors in viral nucleic acid test of 2019 novel coronavirus (2019-nCoV): Chinese Journal of Laboratory Medicine, 2020; E002 [in Chinese]
11. Fang Y, Zhang H, Xie J, Sensitivity of chest CT for COVID-19: Comparison to RT-PCR: Radiology, 2020 [Epub ahead of print]
12. Radiology HSo, Association ITPCoHM: Imaging examination, diagnosis, and control and prevention of nosocomial infection for coronavirus disease 2019: Expert consensus of Hunan radiologist, 2020 http://kns.cnki.net/kcms/detail/43.1427.r.20200218.0950.002.html
13. Xu Z, Shi L, Wang Y, Pathological findings of COVID-19 associated with acute respiratory distress syndrome: Lancet Respir Med, 2020; 8(4); 420-22
14. Ding Y, Wang H, Shen H, The clinical pathology of severe acute respiratory syndrome (SARS): A report from China: J Pathol, 2003; 200(3); 282-89
15. Ng DL, Al Hosani F, Keating MK, Clinicopathologic, immunohistochemical, and ultrastructural findings of a fatal case of Middle Wast respiratory syndrome coronavirus infection in the United Arab Emirates, April 2014: Am J Pathol, 2016; 186(3); 652-58
16. Qian L, Rongshuai W, Guoqiang QGross specimen observation report of a new coronavirus pneumonia death: Journal of Forensic Medicine, 2020; 36(1); 1-3 [in Chinese]
17. Cai Y, Hao Z, Gao Y, COVID-19 in the perioperative period of lung resection: A brief report from a single thoracic surgery department in Wuhan, China: J Thorac Oncol, 2020 [Online ahead of print]
18. Tian S, Xiong Y, Liu H, Pathological study of the 2019 novel coronavirus disease (COVID-19) through postmortem core biopsies: Mod Pathol, 2020 [Online ahead of print]
19. Zu ZY, Jiang MD, Xu PP, Coronavirus disease 2019 (COVID-19): A Perspective from China: Radiology, 2020 [Epub ahead of print]
20. Radiological diagnosis of new coronavirus infected pneumonitis: Expert recommendation from the Chinese Society of Radiology (First edition): Chin J Radiol, 2020; 54; E001 [in Chinese]
21. Lee KS, Pneumonia associated with 2019 novel coronavirus: Can computed tomographic findings help predict the prognosis of the disease?: Korean J Radiol, 2020; 21(3); 257-58
22. Kanne JP, Little BP, Chung JH, Essentials for radiologists on COVID-19: An update-radiology scientific expert panel: Radiology, 2020 [Online ahead of print]
23. Wu J, Wu X, Zeng W, Chest CT findings in patients with coronavirus disease 2019 and its relationship with clinical features: Investig Radiol, 2020; 55(5); 257-61
24. Lu X, Zhang L, Du H, SARS-CoV-2 Infection in Children: N Engl J Med, 2020; 382(17); 1663-65
25. Liu H, Liu F, Li J, Clinical and CT imaging features of the COVID-19 pneumonia: Focus on pregnant women and children: J Infect, 2020; 80(5); e7-13
26. Franquet T, Imaging of pulmonary viral pneumonia: Radiology, 2011; 260(1); 18-39
27. Rodriguez-Morales AJ, Cardona-Ospina JA, Gutierrez-Ocampo E, Clinical, laboratory and imaging features of COVID-19: A systematic review and meta-analysis: Travel Med Infect Dis, 2020; 34; 101623
28. Ai T, Yang Z, Hou H, Correlation of chest CT and RT-PCR testing in coronavirus disease 2019 (COVID-19) in China: A report of 1014 cases: Radiology, 2020 [Online ahead of print]
29. Chung M, Bernheim A, Mei X, CT imaging features of 2019 novel coronavirus (2019-nCoV): Radiology, 2020; 295(1); 202-7
30. Xie X, Zhong Z, Zhao W, Chest CT for typical 2019-nCoV pneumonia: Relationship to negative RT-PCR testing: Radiology, 2020 [Online ahead of print]
31. Shi H, Han X, Jiang N, Radiological findings from 81 patients with COVID-19 pneumonia in Wuhan, China: A descriptive study: Lancet Infect Dis, 2020; 20(4); 425-34
32. Jiang N, Zheng C, Fan YCT appearance of new coronavirus pneumonia in subclinical period and short-term changes: Chinese Journal of Radiology, 2020; E008 [in Chinese]
33. Li K, Wu J, Wu F, The clinical and chest CT features associated with severe and critical COVID-19 pneumonia: Invest Radiol, 2020; 55(6); 327-31
34. Bernheim A, Mei X, Huang M, Chest CT findings in coronavirus disease-19 (COVID-19): Relationship to duration of infection: Radiology, 2020 [Online ahead of print]
35. Chen N, Zhou M, Dong X, Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: A descriptive study: Lancet (London, England), 2020; 395(10223); 507-13
36. Shi H, Han X, Zheng C, Evolution of CT manifestations in a patient recovered from 2019 novel coronavirus (2019-nCoV) pneumonia in Wuhan, China: Radiology, 2020; 295(1); 20
37. Pan F, Ye T, Sun P, Time course of lung changes on chest CT during recovery from 2019 novel coronavirus (COVID-19) pneumonia: Radiology, 2020 [Online ahead of print]
38. Huang C, Wang Y, Li X, Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China: Lancet (London, England), 2020; 395(10223); 497-506
39. Yang W, Yan F, Patients with RT-PCR confirmed COVID-19 and normal chest CT: Radiology, 2020; 295(2); E3
40. Xiao Y, Guo Y, Liu SThe role of medical imaging in the diagnosis and treatment of new coronavirus pneumonia: Chinese Journal of Radiology, 2020; E005 [in Chinese]
41. Lichtenstein D, Meziere G, Biderman P, The comet-tail artifact. An ultrasound sign of alveolar-interstitial syndrome: Am J Respir Crit Care Med, 1997; 156(5); 1640-46
42. Mojoli F, Bouhemad B, Mongodi S, Lichtenstein D, Lung ultrasound for critically ill patients: Am J Respir Crit Care Med, 2019; 199(6); 701-14
43. Pulmonary ultrasonography and remote diagnosis for new coronavirus pneumonia (First Edition): Chinese Journal of Ultrasonography, 2020; E001 [in Chinese]
44. Changyang X, Qiaoyin L, Jianqi LEmphasis on the application of ultrasound monitoring in comprehensive assessment of new coronavirus pneumonia: Chinese Journal of Medical Ultrasound, 2020; E005 [in Chinese]
45. Guan WJ, Ni ZY, Hu Y, Clinical characteristics of coronavirus disease 2019 in China: N Engl J Med, 2020 [Epub ahead of print]
46. Zhang LN, Zhang HM, Cao YG, Ten basic principles about critical ultrasonography: Critical care practitioners need to know: Chin Med J, 2017; 130(13); 1610-14
47. Solomon SD, Saldana F, Point-of-care ultrasound in medical education – stop listening and look: N Engl J Med, 2014; 370(12); 1083-85
48. Wanhong Y, Xiaoting W, Dawei LTechnical specification for clinical application of critical ultrasonography: Zhonghua Nei Ke Za Zhi, 2018; 57(6); 397-417
49. Qiu H, Li X, Du BThe keypoints in treatment of the critical novel coronavirus pneumonia patient: Chinese Journal of Tuberculosis and Respiratory Diseases, 2020; E022 [in Chinese]
50. Lina ZTreatment of severe new coronavirus pneumonia: use of critical ultrasonography: Chinese Journal of Critical Care & Intensive Care Medicine, 2020; E022 [in Chinese]
51. Mayo P, Volpicelli G, Lerolle N, Ultrasonography evaluation during the weaning process: The heart, the diaphragm, the pleura and the lung: Intensive Care Med, 2016; 42(7); 1107-17
52. Tuinman PR, Jonkman AH, Dres M, Respiratory muscle ultrasonography: methodology, basic and advanced principles and clinical applications in ICU and ED patients – a narrative review: Intensive Care Med, 2020; 46(4); 594-605
53. Wang D, Hu B, Hu C, Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China: JAMA, 2020 [Epub ahead of print]
54. Bedside echocardiography of patients with new coronavirus pneumonia and recommendations for the implementation of remote ultrasound consultation (first edition): Chinese Journal of Ultrasonography, 2020; 3(29); 192-205 [in Chinese]
55. Rudski LG, Lai WW, Afilalo J, Guidelines for the echocardiographic assessment of the right heart in adults: A report from the American Society of Echocardiography endorsed by the European Association of Echocardiography, a registered branch of the European Society of Cardiology, and the Canadian Society of Echocardiography: J Am Soc Echocardiogr, 2010; 23(7); 685-713
56. Li X, Du B, Wang YThe keypoints in treatment of the critical coronavirus disease 2019 patient: Zhonghua Jie He He Hu Xi Za Zhi, 2020; 43(4); 277-81 [in Chinese]
57. Recommendations for prevention and treatment of venous thromboembolism associated with new coronavirus pneumonia (trial): National Medical Journal of China, 2020; E007 [in Chinese]
58. Qin C, Liu F, Yen TC, Lan X, (18)F-FDG PET/CT findings of COVID-19: A series of four highly suspected cases: Eur J Nucl Med Mol Imaging, 2020; 47(5); 1281-86
59. Chefer S, Thomasson D, Seidel J, Modeling [(18)F]-FDG lymphoid tissue kinetics to characterize nonhuman primate immune response to Middle East respiratory syndrome-coronavirus aerosol challenge: EJNMMI Res, 2015; 5(1); 65
60. Jonsson CB, Camp JV, Wu A, Molecular imaging reveals a progressive pulmonary inflammation in lower airways in ferrets infected with 2009 H1N1 pandemic influenza virus: PLoS One, 2012; 7(7); e40094
61. Chung M, Bernheim A, Mei X, CT imaging features of 2019 novel coronavirus (2019-nCoV): Radiology, 2020; 295(1); 202-7
62. Le Roux PY, Hicks RJ, Siva S, Hofman MS, PET/CT lung ventilation and perfusion scanning using galligas and Gallium-68-MAA: Semin Nucl Med, 2019; 49(1); 71-81
63. Joob B, Wiwanitkit V, 18F-FDG PET/CT and COVID-19: Eur J Nucl Med Mol Imaging, 2020; 47(6); 1348
64. Bai HX, Hsieh B, Xiong Z, Performance of radiologists in differentiating COVID-19 from viral pneumonia on chest CT: Radiology, 2020 [Epub ahead of print]
65. Caruso D, Zerunian M, Polici M, Chest CT features of COVID-19 in Rome, Italy: Radiology, 2020 [Epub ahead of print]
66. Li L, Qin L, Xu Z, Artificial intelligence distinguishes COVID-19 from community acquired pneumonia on chest CT: Radiology, 2020 [Epub ahead of print]
67. Raptis CA, Hammer MM, Short RG, Chest CT and coronavirus disease (COVID-19): A critical review of the literature to date: Am J Roentgenol, 2020 [Epub ahead of print]
68. Li K, Fang Y, Li W, CT image visual quantitative evaluation and clinical classification of coronavirus disease (COVID-19): Eur Radiol, 2020 [Epub ahead of print]
69. Lu W, Zhang S, Chen B, A clinical study of noninvasive assessment of lung lesions in patients with coronavirus disease-19 (COVID-19) by bedside ultrasound: Ultraschall Med, 2020 [Epub ahead of print]
Figures
 Figure 1. Chest radiography image of a COVID-19-infected patient. A 50-year-old man with a 2-day history of fever and cough. At first, there was no abnormality in the chest radiography image except for a mild enlarged cardiac shadow (A). Two days later, a local patchy shadow was found in the outer band of the left lung (arrow) (B).
Figure 1. Chest radiography image of a COVID-19-infected patient. A 50-year-old man with a 2-day history of fever and cough. At first, there was no abnormality in the chest radiography image except for a mild enlarged cardiac shadow (A). Two days later, a local patchy shadow was found in the outer band of the left lung (arrow) (B). Figure 2. CT images of confirmed COVID-19-infected patients. (A) A 37-year-old man with a 3-day history of fever and cough. The chest CT image showed GGOs with peripheral distribution in the lung. (B) Local amplification of the GGOs. (C) A 70-year-old man with a history of type 2 diabetes mellitus and hypertension. On the seventh day after coming back from Wuhan, he had fever and cough. Reticular interlobular septal thickening and typical crazy-paving pattern were shown by chest CT images. (D) Local amplification of crazy-paving pattern.
Figure 2. CT images of confirmed COVID-19-infected patients. (A) A 37-year-old man with a 3-day history of fever and cough. The chest CT image showed GGOs with peripheral distribution in the lung. (B) Local amplification of the GGOs. (C) A 70-year-old man with a history of type 2 diabetes mellitus and hypertension. On the seventh day after coming back from Wuhan, he had fever and cough. Reticular interlobular septal thickening and typical crazy-paving pattern were shown by chest CT images. (D) Local amplification of crazy-paving pattern. Figure 3. CT images of confirmed COVID-19-infected patients. (A) A 70-year-old man with fever (38.5°C), cough for three days, and had a travel history of Wuhan City. Chest CT displayed patchy GGOs with bronchial wall thickening in the left upper field. (B) Local amplification of the bronchial wall thickening. (C) A 50-year-old male with a residence history of Wuhan City. He had his first visit to our hospital on January 25, 2020, because he had a fever and cough for two days. Chest CT acquired on February 1, 2020, showed multiple subpleural distributed GGOs with consolidation lesions. An air bronchogram sign could be found in the right lung lobe. (D) Local amplification of the air bronchogram sign.
Figure 3. CT images of confirmed COVID-19-infected patients. (A) A 70-year-old man with fever (38.5°C), cough for three days, and had a travel history of Wuhan City. Chest CT displayed patchy GGOs with bronchial wall thickening in the left upper field. (B) Local amplification of the bronchial wall thickening. (C) A 50-year-old male with a residence history of Wuhan City. He had his first visit to our hospital on January 25, 2020, because he had a fever and cough for two days. Chest CT acquired on February 1, 2020, showed multiple subpleural distributed GGOs with consolidation lesions. An air bronchogram sign could be found in the right lung lobe. (D) Local amplification of the air bronchogram sign. Figure 4. A 37-year-old man with a 3-day history of fever and cough. He had a history of close contact with COVID-19 confirmed cases and later he was confirmed to be COVID-19-infected by RT-PCR. (A) The first chest CT acquired on February 12, 2020, showed small GGOs in the bilateral lungs. (B) Eight days later, follow-up chest CT showed the GGOs developed rapidly. The size and range of the lesions increased, which indicated the deterioration of the disease.
Figure 4. A 37-year-old man with a 3-day history of fever and cough. He had a history of close contact with COVID-19 confirmed cases and later he was confirmed to be COVID-19-infected by RT-PCR. (A) The first chest CT acquired on February 12, 2020, showed small GGOs in the bilateral lungs. (B) Eight days later, follow-up chest CT showed the GGOs developed rapidly. The size and range of the lesions increased, which indicated the deterioration of the disease. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387