12 December 2020: Clinical Research
Comparison of Role of Hand and Wrist Ultrasound in Diagnosis of Subclinical Synovitis in Patients with Systemic Lupus Erythematosus and Rheumatoid Arthritis: A Retrospective, Single-Center Study
Honghu Tang1BCDEF, Yi Liu1ABCDEFG*, Yi Liu1BCDF, Hua Zhao1BCDFDOI: 10.12659/MSM.926436
Med Sci Monit 2020; 26:e926436
Abstract
BACKGROUND: This retrospective study aimed to compare the roles of hand and wrist ultrasound in diagnosing subclinical synovitis in patients with systemic lupus erythematosus (SLE) and rheumatoid arthritis (RA) at a single center in Sichuan, China.
MATERIAL AND METHODS: Forty-one patients with SLE and 20 patients with RA were included. SLE was diagnosed using the American rheumatology Society (ACR) classification standard. Severity of SLE was evaluated using the SLE disease activity index (SLEDAI). General and clinical manifestations and laboratory indicators were measured. Spearman correlation analysis was used for analyzing correlations between musculoskeletal ultrasound results and indexes.
RESULTS: Among 41 patients with SLE, 26 (63.4%) had joint pain, and 39 (95.1%) had at least 1 joint abnormality. Thirteen patients with SLE (31.7%) had wrist joint involvement, 7 (17.1%) had metacarpal phalangeal-1 (MCP1) involvement, 8 (19.5%) had MCP2 involvement, 17 (41.5%) had MCP3 involvement, 14 (34.1%) had MCP4 involvement, and 5 (12.2%) had MCP5 involvement. Meanwhile, 2 (4.8%) had proximal interphalangeal-1 (PIP1) involvement, 10 (24.4%) had PIP2 involvement, 17 (41.5%) had PIP3 involvement, 12 (29.3%) had PIP4 involvement, and 3 (7.3%) had PIP4 involvement. Twelve patients demonstrated knee joint involvement. MCP joints had the highest involvement frequency (P=0.003). The most frequently detected disease was synovitis, followed by tenosynovitis, joint effusion, and bone erosion. ESR (P=0.002), CRP (P=0.020), and SLEDAI (P=0.011) of patients with SLE with arthralgia were significantly higher compared to patients without arthralgia. In patients with RA, musculoskeletal ultrasound scores were correlated with erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), disease activity score-28 (DAS28), and interleukin-6 (IL-6). In patients with SLE, musculoskeletal ultrasound scores were correlated with double-stranded DNA (dsDNA), ribonucleoprotein (RNP), DAS28, and IL-6.
CONCLUSIONS: Musculoskeletal ultrasound is highly sensitive in evaluating subclinical synovitis in patients with SLE, and its score is positively correlated with dsDNA, RNP IL-6, and DAS28 in patients with SLE.
Keywords: Arthralgia, rheumatoid arthritis, Lupus Erythematosus, Systemic, Ultrasonography, Adolescent, Arthritis, Rheumatoid, Autoantibodies, data analysis, Hand, Interleukin-6, Joints, synovitis, Wrist, young adult
Background
Systemic lupus erythematosus (SLE) is an autoimmune disease characterized by multiple autoantibodies and multiple organ involvement [1,2]. SLE can involve the skin, mucosa, joint muscles, kidney, neuropsychic system, and digestive system [3]. Among the diseases of the above organs, arthritis is one of the most common clinical manifestations of SLE. The incidence of arthritis in patients with SLE of different races ranges from 69% to 95% [4–6]. A previous study [7] reported that 78.3% patients with lupus have arthritis at the initial diagnosis, and about 58% of patients with SLE relapse have active arthritis. The typical manifestation of SLE arthritis is symmetrical poly-articular inflammation, mainly involving metacarpal phalangeal (MCP), proximal interphalangeal (PIP), distal interphalangeal (DIP), and knee joints [8]. SLE arthritis can also damage the elbow joint, ankle joint, and sacroiliac joint [8,9]. Clinically, symptoms of arthritis can last for several hours, weeks, or even months. Compared with rheumatoid arthritis (RA), the swelling caused by effusion and synovium hyperplasia in SLE arthritis is relatively light.
Presently, how to evaluate, treat, and predict SLE arthritis accurately is the main problem faced by rheumatologists. In recent years, most studies have focused on the clinical aspects of rheumatoid arthritis. From the traditional point of view, arthritis of patients with SLE is non-erosive and recoverable; however, this view has now been challenged by use of new imaging technology [10]. According to the description of a previous study [11], the concept of bone erosion should be refined. A previous study called this kind of erosive joint disease “rhupus” to specifically refer to the combination of the characteristics of rheumatoid arthritis and systemic lupus erythematosus [12]. According to clinical characteristics and manifestations, SLE joint involvement could be divided into arthralgia/synovitis, Jaccoud arthropathy, mild deformable arthropathy, erosive arthropathy, and involvement of periarticular tissue [13,14].
In the diffuse connective tissue disease, joint involvement of patients with SLE is generally considered as non-aggressive. Rheumatologists may neglect the detailed assessment of lupus joint, which can lead to aggravation of arthritis or even deformity. Therefore, in the present study we developed a joint assessment system suitable for use in SLE arthritis. Clinically, the SLE disease activity index 2000 (SLEDAI) scoring system is widely used in patients with SLE; however, this system also focuses on multiple systems and organs of the whole body, and is not limited to joints [15]. In the past few years, the disease activity score-28 (DAS28) score has been verified in many ways and widely used in routine clinical practice in patients with RA. The DAS28 score is accepted because of its advantages of easy operation, high standard, high correlation with doctors’ and patients’ evaluation, and full differentiation of disease activity and disease remission rate. It has been found that DAS28 can be used to evaluate the joint involvement of patients with SLE [16].
Nowadays, in the classification and recognition of SLE arthritis, there are some new technical weapons, such as magnetic resonance imaging (MRI), musculoskeletal ultrasound and molecular methods [17]. However, there is not a well-defined classification system for SLE arthritis. Use of new imaging techniques, including MRI and musculoskeletal ultrasound, is improving understanding of the erosion process and joint pathology in rheumatic diseases. There remain many problems to be explored and solved in SLE arthritis research. Therefore, it is of long-term significance to study subclinical synovitis, bone erosion, and joint dysfunction in SLE arthritis [18]. At the same time, we can recognize SLE as a complex disease from another perspective.
This retrospective study aimed to compare the role of hand and wrist ultrasound in diagnosis of subclinical synovitis in patients with SLE and RA at a single center in Sichuan, China.
Material and Methods
PATIENTS:
We enrolled 41 patients with SLE hospitalized in the Rheumatology and Immunology Ward of West China Hospital of Sichuan University, from February 2014 to February 2015. Among all patients with SLE, there were 5 male patients and 36 female patients, with an average age of 34.73±12.298 years (range, 15–65 years). The average course of disease was 48.17±48.297 months (range, 1–180 months). A total of 20 patients with RA (5 males and 15 females) were also included in this study. The average age of patients with RA was 41.10±11.548 years (range, 18–65 years old), and an average course of disease of 21.750±20.8879 months (range, 3–72 months). Patients with confirmed diagnosis of SLE or AR and complete history were included in this study. We excluded patients with severe infection, combined SLE and RA, and other types of arthritis (such as spinal arthritis and gout).
This study was approved by the Ethics Committee of West China Hospital, Sichuan University, Chengdu, China. All of the patients with SLE and patients with RA provided written formed consent.
CLASSIFICATION CRITERIA AND DISEASE ASSESSMENT OF SLE:
For the classification standard of SLE, we used the SLE classification standard revised by the American rheumatology Society (ACR) [19]. The ACR SLE classification includes 11 items, and SLE is diagnosed when the patient has 4 or more items, excluding infection, tumor, and other connective tissue diseases. For the assessment of SLE, we used the SLE disease activity index 2000 (SLEDAI) scoring standard [20]. Inactive SLE was defined as SLEDAI ≤4 and active SLE was defined as SLEDAI ≥5.
CLASSIFICATION OF RA AND EVALUATION OF MUSCULOSKELETAL ULTRASOUND:
RA was classified according to the 1987 American rheumatic Association (ACR) classification of RA [21]. Evaluation of musculoskeletal ultrasound was carried out according to EULAR guidelines for musculoskeletal US in rheumatology [22] and Outcome Measures in RA Clinical Trials (OMERACT) [23]. The Esaote MyLab 20 ultrasound instrument (with probe frequency of 8–12 MHZ and 12–18 MHZ, respectively) was used. The bilateral wrist joints, bilateral MCP joints, bilateral PIP joints, and bilateral knee joints of all patients with SLE and RA were examined by a single rheumatologist. The semi-quantitative ultrasound evaluation system was used to evaluate each joint in 4 aspects: joint effusion, synovitis, tenosynovitis/peritendinitis, and bone erosion.
DATA COLLECTION:
We collected data on general patient characteristics (age, sex, onset time, onset age), detailed history of disease, clinical manifestations, physical examination, laboratory indicators, imaging data, and treatment plans of the patients with SLE and patients with RA. The main clinical manifestations included arthralgia, new rash, mucosal ulcer, neuropsychological symptoms, alopecia, fever, and myositis. Patient histories mainly included severe infection and course of the disease. Laboratory indexes mainly included antinuclear antibody (ANA) titer, extractable nuclear antibody (ENA) spectrum (including Sjögren syndrome A (SSA), Sjögren syndrome B (SSB), ribonucleoprotein (RNP), Smith (SM), ribosomal (RIB)), complement 3 (C3), complement 4 (C4), rheumatoid factor (RF), cyclic citrullinated peptide (CCP), keratin antibody (AKA), blood routine, urination routine, 24-hour urine protein levels, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), and serum interleukin-6 (IL-6), and these were examined as described by previous published studies [24–26]. All examinations of the above laboratory indexes were completed within 24 h before or after ultrasound examination.
STATISTICAL ANALYSIS:
SPSS20.0 statistical software was used for data analyses. The measurement data were represented as mean±standard deviation (SD), and the counting data were represented as percentage or frequency. Tukey’s post hoc test was used to validate the analysis of variance (ANOVA) for comparing measurement data between groups. Spearman correlation analysis was carried out for analyzing the correlations. Statistical significance was defined as
Results
BASIC DATA OF 41 PATIENTS WITH SLE AND 20 PATIENTS WITH RA:
This study involved 41 patients with SLE and 20 patients with RA, whose clinical manifestations (disease course, joint involvement), laboratory indexes (ANA titer, ENA spectrum, ESR, CRP and serum IL-6, C3, C4, RF, CCP), and scoring data (DAS28 score, SLEDAI score, and ultrasonic score) are illustrated in Table 1.
JOINT INVOLVEMENT FREQUENCY ASSESSMENT IN PATIENTS WITH SLE USING MUSCULOSKELETAL ULTRASOUND:
Musculoskeletal ultrasound was used to scan and evaluate 984 joints of hands, wrists, and knees in 41 patients with SLE from 4 aspects: joint effusion, synovial hyperplasia, tenosynovitis, and bone erosion. Among these 41 patients, 26 patients (63.4%) had joint pain and 39 patients (95.1%) had at least 1 joint abnormality (Figure 1). Among all 41 patients, 13 patients (31.7%) had wrist joint involvement and 7 patients (17.1%) had first metacarpal phalangeal-1 (MCP1) involvement, 8 patients (19.5%) had MCP2 involvement, 17 patients (41.5%) had MCP3 involvement, 14 patients (34.1%) had MCP4 involvement, and 5 patients (12.2%) had MCP5 involvement (Figure 1). Meanwhile, 2 patients (4.8%) had first proximal interphalangeal-1 (PIP1) involvement, 10 patients (24.4%) had PIP2 involvement, 17 patients (41.5%) had PIP3 involvement, 12 patients (29.3%) had PIP4 involvement, and 3 patients (7.3%) had PIP4 involvement (Figure 1). Moreover, there were 12 patients (29.3%) demonstrated knee joint involvement (Figure 1). We found that metacarpal phalangeal joints were the joint groups with the highest frequency of involvement (P=0.003). Among 410 MCP joints, the frequency of involvement from high to low was MCP3 >MCP4 >MCP2 >MCP1 >MCP5 (Figure 1).
EVALUATION FOR DIFFERENT JOINT DISEASES IN JOINTS OF PATIENTS WITH SLE USING MUSCULOSKELETAL ULTRASOUND:
The OMERACT scoring system of musculoskeletal ultrasound can be used for semi-quantitative evaluation of joint effusion, synovitis, tendinitis/peritendinitis, and bone erosion. Our results indicated that among 82 wrist joints, 53 joints demonstrated synovial hyperplasia (27 had CDFI signal), 12 joints demonstrated tenosynovitis, and 3 joints demonstrated bone erosion (Figure 2). Out of 410 MCP joints, 87 showed synovial hyperplasia, 31 showed tenosynovitis, and 2 showed bone erosion (Figure 2). Among 410 PIP joints, 35 exhibited synovial hyperplasia, 27 exhibited tenosynovitis, and 1 exhibited bone erosion. Among 82 knee joints, there were 19 synovial hyperplasia (1 with CDFI signal) and 56 joint effusion (Figure 2). Among all 984 joints in 41 patients with SLE, the most frequently detected type was synovitis (194/984, 19.7%), followed by tenosynovitis (70/984, 7.1%), joint effusion (56/984, 5.7%), and bone erosion (6/984, 0.6%) (Figure 2).
ESTIMATION OF MUSCULOSKELETAL ULTRASOUND SCORES IN DIFFERENT JOINTS OF PATIENTS WITH SLE:
In the patients with SLE, scores of musculoskeletal ultrasound OMERACT evaluation of joint involvement directly reflected the severity of joint involvement. The findings indicated that the score of the MCP group was significantly higher compared to that of the other groups (Table 2, P<0.05). Therefore, musculoskeletal ultrasound evaluations demonstrated that MCP was the most seriously affected, followed by the wrist joint, knee joint, and PIP (Table 2).
DATA ANALYSIS OF PATIENTS WITH SLE WITH OR WITHOUT ARTHRALGIA:
According to the existence of arthralgia or not, the patients with SLE were divided into a group of patients with SLE with arthralgia and a group of patients with SLE without arthralgia, and we compared them (95% confidence interval). ESR (P=0.002), CRP (P=0.020), and SLEDAI score (P=0.011) of patients with SLE with arthralgia were significantly higher compared to those of patients with SLE without arthralgia (Table 3). However, there was no significant difference in ultrasound scores between patients with arthralgia and patients with SLE without arthralgia (Table 3, P=0.812). These results suggest that the patients with SLE without arthralgia may be abnormal in musculoskeletal ultrasound evaluation, suggesting that the musculoskeletal ultrasound evaluation for SLE arthritis is more sensitive than the physical examinations.
DIFFERENCES BETWEEN PATIENTS WITH SLE AND RA IN MUSCULOSKELETAL ULTRASOUND, LABORATORY INDEXES, AND DAS28 SCORES:
We also enrolled 20 patients with RA to compare them with patients with SLE and to establish a more practical musculoskeletal ultrasound evaluation system. We found significant differences in ESR (P=0.000), CRP (P=0.001), DAS28 (P=0.000), and ultrasonic score (P=0.000) between patients with SLE and patients with RA (Table 4).
CORRELATION BETWEEN MUSCULOSKELETAL ULTRASOUND SCORES AND INFLAMMATORY INDEXES:
There were significant correlations between ESR (r=0.932, P=0.000) or CRP (r=0.906, P=0.000) and the musculoskeletal ultrasound scores in the patients with RA (Table 5). However, there were no significant differences between ESR (r=0.215, P=0.117) or CRP (r=0.124, P=0.439) and the musculoskeletal ultrasound scores in patients with SLE (Table 5).
MUSCULOSKELETAL ULTRASOUND SCORE WAS CORRELATED WITH IL-6:
We also analyzed correlation between cytokine, IL-6, and musculoskeletal ultrasound scores. The results showed that musculoskeletal ultrasound scores of patients with RA (r=0.834, p=0.000) and patients with SLE (r=0.580, P=0.000) were positively correlated with the serum IL-6 (Figure 3).
CORRELATION BETWEEN MUSCULOSKELETAL ULTRASOUND SCORES AND AUTOANTIBODIES:
In the patients with RA, there were significant positive correlations between the RF (r=0.776, P=0.000) or CCP antibody titer (r=0.682, P=0.000) and the musculoskeletal ultrasound scores (Table 5). In the patients with SLE, there were significant correlations between titer of dsDNA (r=0.384, P=0.013) or RNP autoantibodies (r=0.366, P=0.019) and musculoskeletal ultrasound scores (Table 5). However, there were no significant correlations between the other autoantibodies and musculoskeletal ultrasound scores in patients with SLE (Table 5).
CORRELATION BETWEEN MUSCULOSKELETAL ULTRASOUND SCORES AND DAS28/SLEDAI SCORES:
For the patients with RA, the DAS28 score was positively correlated with the musculoskeletal ultrasound score (Table 5, r=0.591, P=0.000). For the patients with SLE, the DAS28 score was also positively correlated with musculoskeletal ultrasound score (Table 5, r=0.905, P=0.000); however, there was no correlation between SLEDAI score and musculoskeletal ultrasound score (Table 5, r=0.161, P=0.314).
Discussion
Among 41 patients with SLE, 26 had joint pain and 39 had at least 1 joint abnormality. A total of 13 patients with SLE had wrist joint involvement, 7 had MCP1 involvement, 8 had MCP2 involvement, 17 had MCP3 involvement, 14 (34.1%) had MCP4 involvement, and 5 had MCP5 involvement. Meanwhile, 2 had PIP1 involvement, 10 had PIP2 involvement, 17 had PIP3 involvement, 12 had PIP4 involvement, and 3 had PIP4 involvement. The MCP joints demonstrated the highest involvement frequency. The most frequently detected disease was synovitis, followed by tenosynovitis, joint effusion, and bone erosion. ESR, CRP, and SLEDAI of patients with SLE were significantly higher compared to patients without arthralgia. Musculoskeletal ultrasound scores were correlated with ESR, CRP, DAS28, and IL-6 in patients with RA and were correlated with dsDNA, RNP, DAS28, and IL-6 in patients with SLE.
In recent years, more and more studies have proven that musculoskeletal ultrasound, as a new imaging technology, plays an important role in assessment of rheumatic diseases, especially for joint and tendon abnormalities [27–29]. Musculoskeletal ultrasound is now increasingly used in patients with rheumatoid arthritis (RA) and spinal arthritis to detect inflammatory injuries [30], such as joint effusion, synovitis, tendinitis, tenosynovitis, and bone erosion. A relatively mature evaluation system has been established for patients with RA. The frequency of the affected joint observed by ultrasound in patients with RA was consistent with the clinical manifestations, and the score of color Doppler ultrasound was also significantly correlated with the inflammatory index and DAS28 score. However, for patients with SLE, although joint involvement is one of the most common clinical manifestations, musculoskeletal ultrasound assessment is rarely used to detect joint diseases [31].
SLE is a serious disease with genetic heterogeneity, and the recurrence and remission of which are unpredictable. However, musculoskeletal system involvement is the most common symptom of SLE. Therefore, accurate assessment of joints in patients with SLE is a critical step in diagnosis, treatment, and prognosis evaluation. The purpose of this study was to evaluate the joint status of patients with SLE from aspects of joint effusion, synovitis, tenosynovitis and bone erosion. We also explored the relationship between ultrasound and autoantibody, inflammation index, SLEDAI score, and DAS28 score to establish a joint evaluation system for patients with SLE. Additionally, our results may help in development of personalized treatment programs for patients with SLE, so as to increase the accuracy of overall assessment of disease in patients with SLE.
Among the 41 patients with SLE involved in this study, musculoskeletal ultrasound demonstrated that more than 90% of the affected joints had SLE arthritis. In contrast to the affected joints in patients with RA, SLE arthritis mainly involved the MCP joint group, which was also the most affected joint. Among the MCP joints, the most commonly affected joint was the MCP3 joint, followed by the MCP4 joint, MCP2 joint, MCP1 joint, and MCP5 joint. In 41 patients with SLE, 63.4% had arthralgia, 95.1% of whom had joint abnormality. This phenomenon suggests that arthritis in patients with SLE might not show arthralgia symptoms, and physical examination may not reveal joint tenderness and swelling. Patients with SLE were divided into SLE without arthralgia and SLE with arthralgia patients, according to whether there was arthralgia, and then the data were compared. Our results showed that there were significant differences in ESR, CPR, and SLEDAI scores between SLE with arthralgia and SLE without arthralgia patients. However, there was no significant difference between the 2 groups in musculoskeletal ultrasound scores, which suggests that the joint abnormalities detected by musculoskeletal ultrasound might not be shown by clinical manifestations and physical examination. Meanwhile, the sensitivity of musculoskeletal ultrasound was much better than that of clinical manifestations and physical examination [32], which suggests that musculoskeletal ultrasound can accurately detect subclinical synovitis in patients with SLE. We also found that the most common joint problem of patients with SLE was synovitis (with a frequency of 19.7%), following with tenosynovitis (7.1%), joint effusion (5.7%), and bone erosion (0.6%). This is also in line with the clinical characteristics of SLE arthritis, which in most cases is non-erosive arthritis.
In patients with RA, we studied the correlation between musculoskeletal ultrasound and laboratory examination, SLEDAI score, and DAS28 score. The findings showed that musculoskeletal ultrasound evaluation was correlated with inflammatory indexes, including ESR and CRP. Research on correlations between IL-6 level and arthritis has increased in recent years. In the present investigation, musculoskeletal ultrasound confirmed the correlation between musculoskeletal ultrasound evaluation of arthritis in patients with RA and inflammatory indexes, and revealed correlations between IL-6 level and RA ultrasonic evaluation. Most importantly, this study analyzed the correlation between musculoskeletal ultrasound scores of patients with SLE and the autoantibodies (including ANA, dsDNA, SM, SSA, SSB, RNP, RIB, C3, C4), laboratory indexes (ESR, CRP, IL-6), SLEDAI scores, and DAS28 scores. Our data showed that musculoskeletal ultrasound scores were positively correlated with dsDNA antibody, RNP antibody, serum IL-6, and DAS28 scores. In other words, the above laboratory data and DAS28 scores reflect arthritis status in patients with SLE, and also provides strong evidence for establishing a more complete, sensitive, and specific evaluation system [33]. Actually, except for the SLEDAI score and DAS28 score, the Systemic Lupus International Collaborating Clinics (SLICC) could also be applied for evaluating systemic lupus erythematosus [34], which could be used in further study. In addition to the present study, there are also a few other published articles involving the determination of joint involvement in hands and wrists of patients with SLE [35,36]. Ruano et al. [35] evaluated the subclinical joint inflammation of patients with SLE using global ultrasound and power Doppler ultrasound, but they evaluated SLE using inflammation indexes (ESR, CRP, and IL-6) and according to EULAR guidelines for musculoskeletal US in rheumatology and Outcome Measures in RA Clinical Trials (OMERACT). Gabba et al. [36] also reported that musculoskeletal ultrasound is a reliable tool for monitoring musculoskeletal characteristics for patient with SLE; however, SLE was classified with using the British Isles Lupus Assessment Group (BILAG) 2004 score (we used SLEDAI score and DAS28 score). Moreover, Iagnocco et al. [37] found that foot joints were the most frequently involved joints; however, the present findings demonstrated the highest involvement frequency in MCP joints. The difference might be due to the different involved joints of patient with SLE.
Although our study produced some interesting results, it also has some limitations. First, the sample size was small and the number of joints detected was limited; therefore, the results may not be accurate. Second, there is no specific treatment strategy for SLE. Treatment of SLE includes non-steroidal anti-inflammatory drugs, glucocorticoid, and disease modifying anti-rheumatic drugs, which have certain impacts on evaluation of arthritis and are uncontrollable factors in this study. Third, this was a single-center and retrospective analysis, and the age groups were not uniform. Fourth, we did not evaluate the involvement of foot joints in patients with SLE, which might show higher involvement than in MCP joints. Fifth, the present retrospective investigation relied on archived clinical data, mainly including patients with SLE examined 5 year ago. Finally, only the EULAR- and OMERACT-based musculoskeletal ultrasound and SLEDAI score and DAS28 score were used in this study, while the other ultrasound methods and scoring systems were not applied.
Conclusions
As a powerful tool for evaluating and predicting joint involvement, musculoskeletal ultrasound has the advantages of safety, non-invasiveness, low cost, and high acceptability [38] compared with the traditional X-ray, computed tomography (CT), and MRI technologies. Musculoskeletal ultrasound has become an important method in diagnosis and treatment of rheumatic diseases. Musculoskeletal ultrasound is very sensitive in evaluating subclinical synovitis in patients with SLE. We found a Iannucci positive correlation between musculoskeletal ultrasound score and levels of autoantibodies, IL-6, and DAS28 in patients with SLE.
This study provides a basis for establishment of an arthritis evaluation system in patients with SLE. For patients with SLE, especially those with increased inflammation indexes, increased DAS28 score, increased dsDNA and RNP, even if there is no clinical manifestation of arthralgia, it is necessary to improve musculoskeletal ultrasound to evaluate activity of arthritis to guide adjustment of drug regimens. However, it is not clear whether subclinical synovitis in early treatment of SLE improves the prognosis of joints and tendons. Therefore, further research with larger samples and more in-depth evaluation of early treatment efficacy is needed. To improve the individualized treatment of patients with SLE, further research is needed on the correlations between musculoskeletal ultrasound examination and drug therapy, and to explore targeted drug therapy guided by ultrasound.
Figures
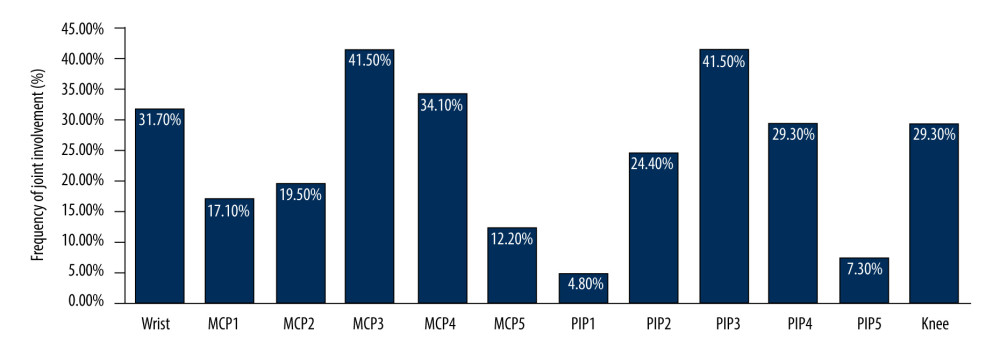 Figure 1. Statistical analysis of joint involvement frequency in patients with SLE undergoing evaluation by musculoskeletal ultrasound. Among the 410 MCP joints, frequency of involvement from high to low was: MCP3, MCP4, MCP2, MCP1, and MCP5. MCP – metacarpal phalangeal, PIP – proximal interphalangeal.
Figure 1. Statistical analysis of joint involvement frequency in patients with SLE undergoing evaluation by musculoskeletal ultrasound. Among the 410 MCP joints, frequency of involvement from high to low was: MCP3, MCP4, MCP2, MCP1, and MCP5. MCP – metacarpal phalangeal, PIP – proximal interphalangeal. 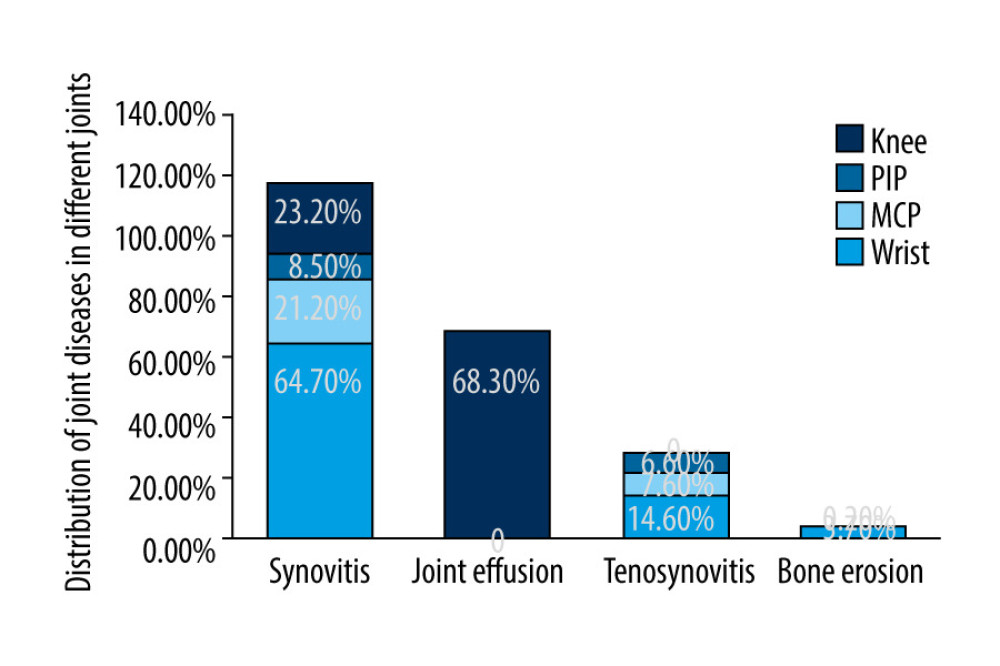 Figure 2. Musculoskeletal ultrasound evaluation for the joint diseases in the joints of patients with SLE. Among all 984 joints, the frequency of joint disease type from high to low was: synovitis, tenosynovitis, joint effusion, and bone erosion. MCP – metacarpal phalangeal, PIP – proximal interphalangeal.
Figure 2. Musculoskeletal ultrasound evaluation for the joint diseases in the joints of patients with SLE. Among all 984 joints, the frequency of joint disease type from high to low was: synovitis, tenosynovitis, joint effusion, and bone erosion. MCP – metacarpal phalangeal, PIP – proximal interphalangeal. 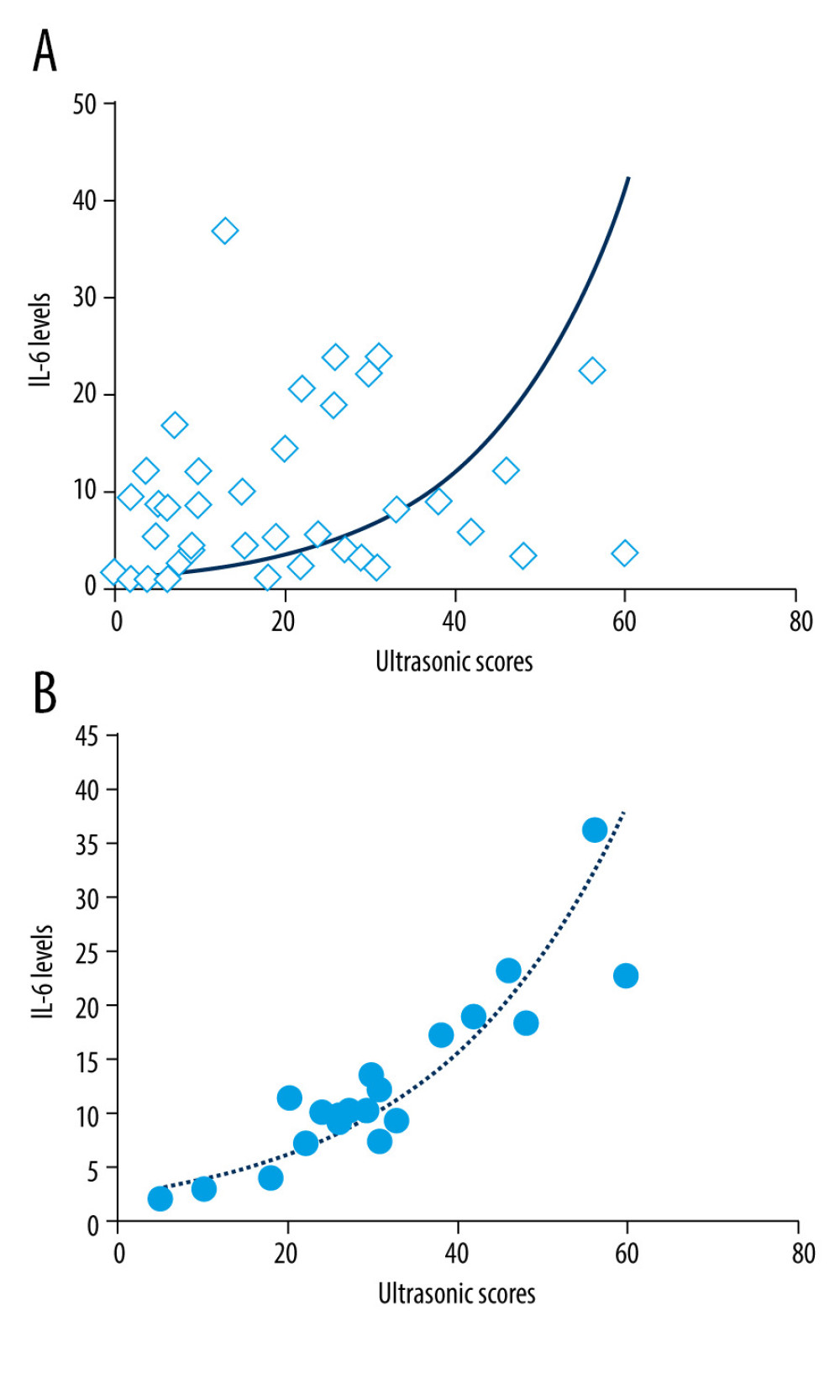 Figure 3. The musculoskeletal ultrasound scores of patients with SLE (A) and patients with RA (B) were positively correlated with the serum level of IL-6. SLE – systemic lupus erythematosus; RA – rheumatoid arthritis; IL-6 – interleukin-6.
Figure 3. The musculoskeletal ultrasound scores of patients with SLE (A) and patients with RA (B) were positively correlated with the serum level of IL-6. SLE – systemic lupus erythematosus; RA – rheumatoid arthritis; IL-6 – interleukin-6. Tables
Table 1. Demographic and clinical characteristics for 41 patients with SLE and 20 patients with RA involved in this study. We assessed the disease course and joint involvement, laboratory indexes (ANA titer, ENA spectrum, ESR, CRP and IL-6, C3, C4, RF, CCP) and scoring data (DAS28 score, SLEDAI score and ultrasonic score).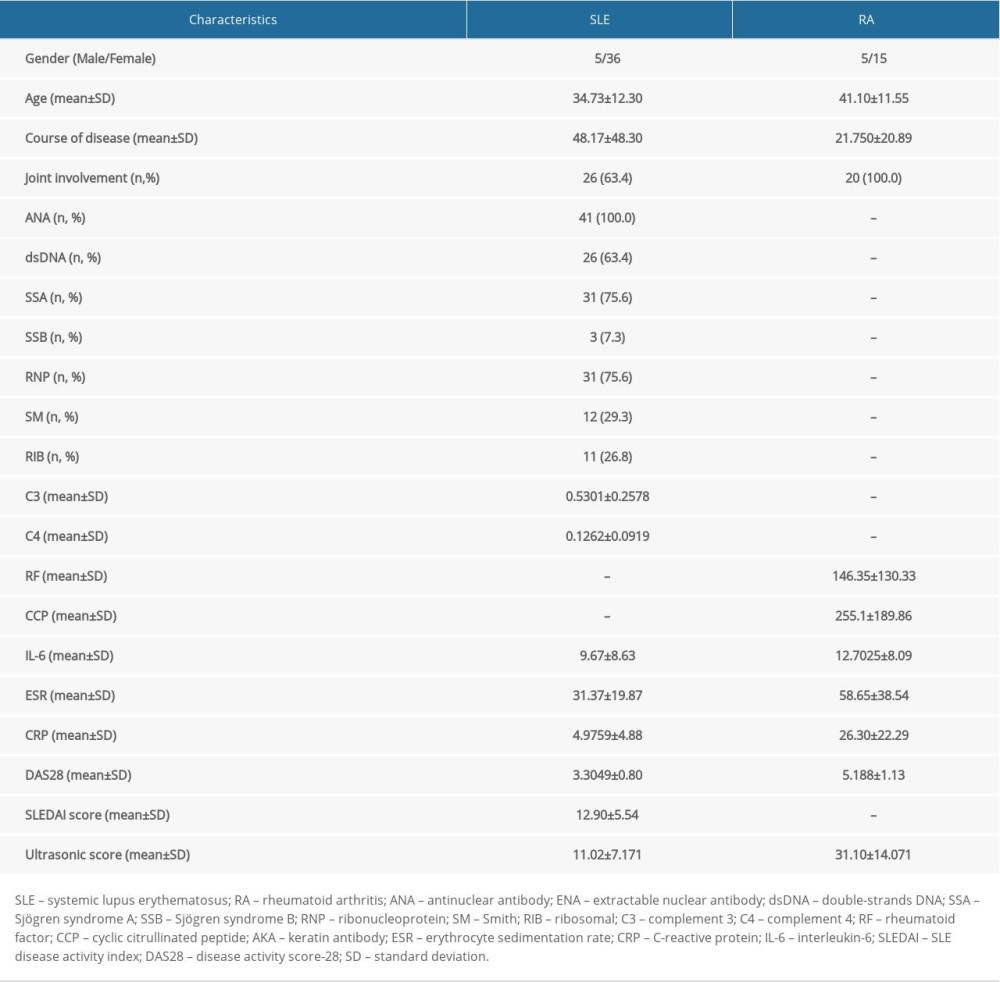 Table 2. Semi-quantitative assessment of degree of joint involvement in patients with SLE using ultrasonography. The MCP was the most seriously affected joint, followed by wrist joints, knee joints, and PIP joints.
Table 2. Semi-quantitative assessment of degree of joint involvement in patients with SLE using ultrasonography. The MCP was the most seriously affected joint, followed by wrist joints, knee joints, and PIP joints.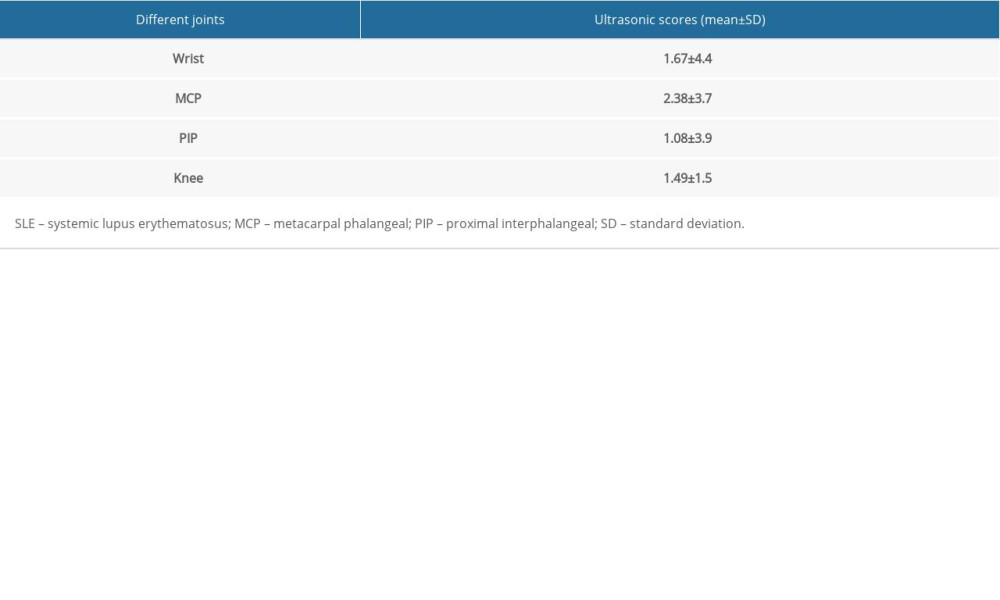 Table 3. Comparative analysis of patients with SLE with and without arthralgia. The results showed that patients with SLE without arthralgia tended to demonstrate abnormality according to the musculoskeletal ultrasound, which suggests that musculoskeletal ultrasound is more sensitive for evaluating SLE arthritis.
Table 3. Comparative analysis of patients with SLE with and without arthralgia. The results showed that patients with SLE without arthralgia tended to demonstrate abnormality according to the musculoskeletal ultrasound, which suggests that musculoskeletal ultrasound is more sensitive for evaluating SLE arthritis.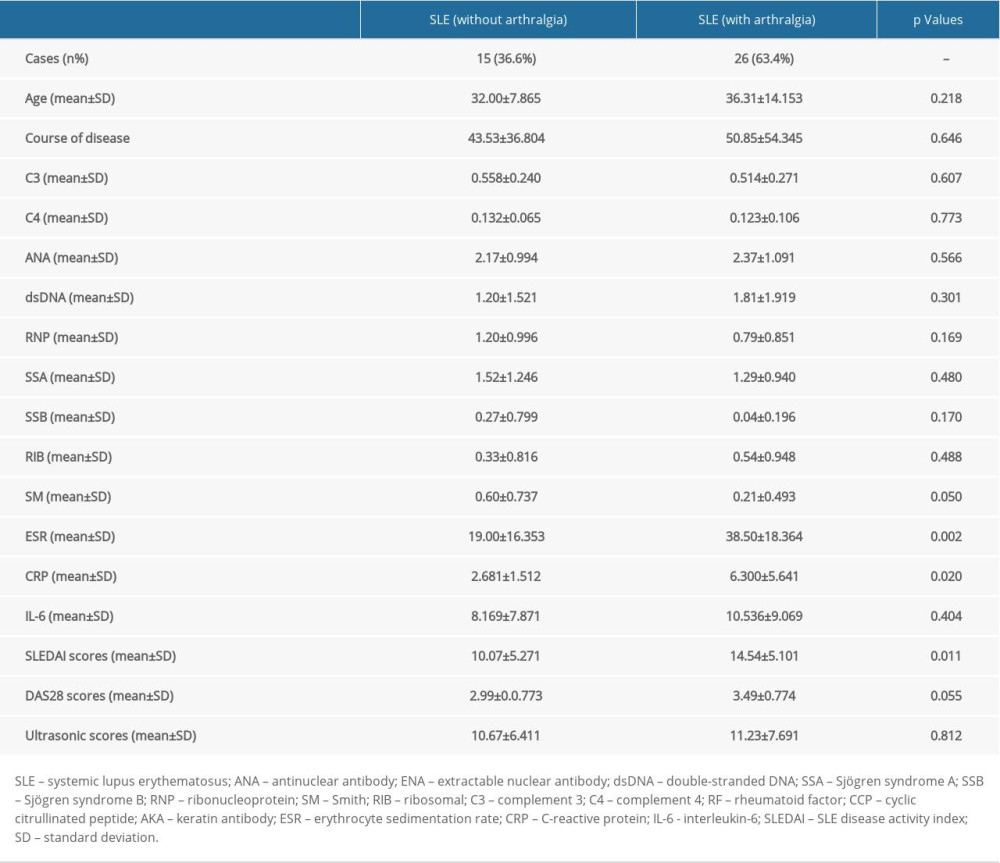 Table 4. Differences between patients with SLE and patients with RA determined using musculoskeletal ultrasound, laboratory indexes (including ESR and CRP), and DAS28 scores.
Table 4. Differences between patients with SLE and patients with RA determined using musculoskeletal ultrasound, laboratory indexes (including ESR and CRP), and DAS28 scores.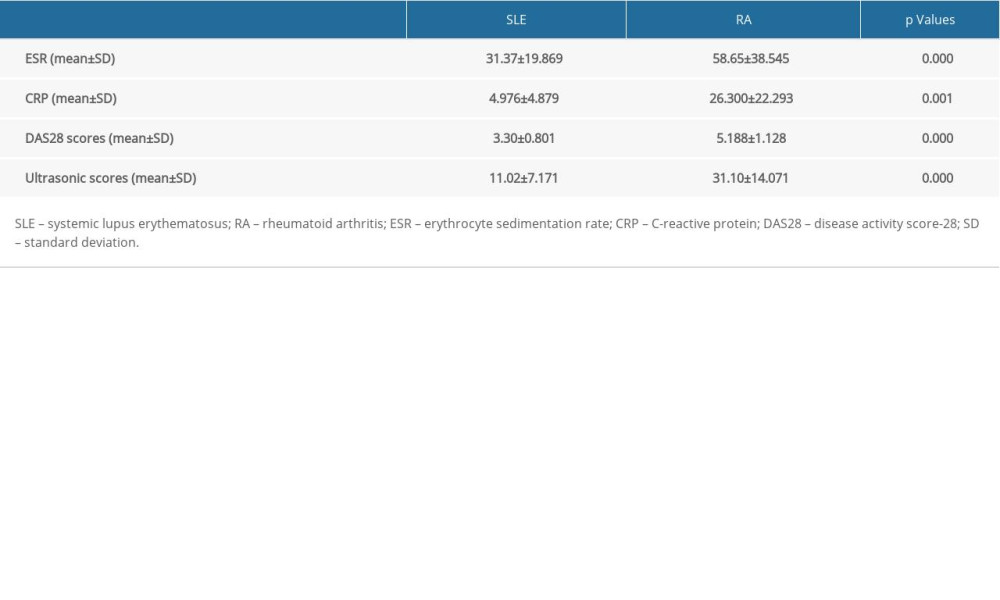 Table 5. Correlation analysis between musculoskeletal ultrasound scores and inflammatory indexes/autoantibodies. There were positive correlations between RF/CCP antibody titer and ultrasound scores in patients with RA. There were significant correlations between dsDNA titer/RNP autoantibodies and ultrasound scores in patients with SLE. DAS28 score was positively correlated with ultrasound score in patients with RA and in patients with SLE.
Table 5. Correlation analysis between musculoskeletal ultrasound scores and inflammatory indexes/autoantibodies. There were positive correlations between RF/CCP antibody titer and ultrasound scores in patients with RA. There were significant correlations between dsDNA titer/RNP autoantibodies and ultrasound scores in patients with SLE. DAS28 score was positively correlated with ultrasound score in patients with RA and in patients with SLE.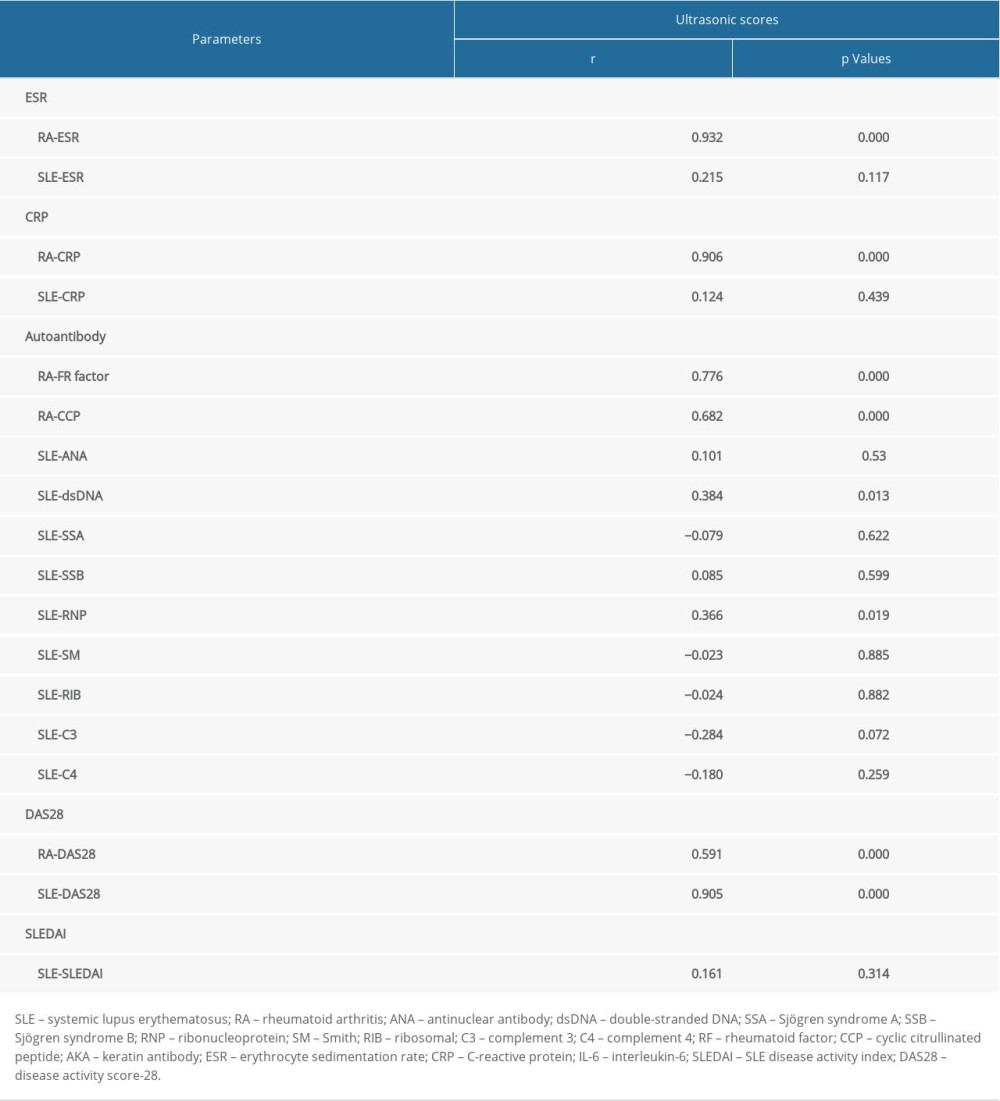
References
1. Chen Q, Qiu F, Liu H, Altered olfactory function in patients with systemic lupus erythematosus: Med Sci Monit, 2019; 25; 5929-33
2. Li Z, Jiang C, Ye C, miR-10a-5p, miR-99a-5p and miR-21-5p are steroid-responsive circulating microRNAs: Am J Transl Res, 2018; 10; 1490-97
3. Lisnevskaia L, Murphy G, Isenberg D, Systemic lupus erythematosus: Lancet, 2014; 384; 1878-88
4. Sestak AL, Nath SK, Kelly JA, Patients with familial and sporadic onset SLE have similar clinical profiles but vary profoundly by race: Lupus, 2008; 17; 1004-9
5. Rees F, Doherty M, Grainge M, The incidence and prevalence of systemic lupus erythematosus in the UK, 1999–2012: Ann Rheum Dis, 2016; 75; 136-41
6. Dall’Era M, Cisternas MG, Snipes K, The incidence and prevalence of systemic lupus erythematosus in San Francisco County, California: The California lupus surveillance project: Arthritis Rheumatol, 2017; 69; 1996-2005
7. Pentony P, Duquenne L, Dutton K, The initiation of autoimmunity at epithelial surfaces: A focus on rheumatoid arthritis and systemic lupus erythematosus: Discov Med, 2017; 24; 191-200
8. Ceccarelli F, Perricone C, Cipriano E, Joint involvement in systemic lupus erythematosus: From pathogenesis to clinical assessment: Semin Arthritis Rheum, 2017; 47; 53-64
9. Grunke M, Antoni CE, Kavanaugh A, Standardization of joint examination technique leads to a significant decrease in variability among different examiners: J Rheumatol, 2010; 37; 860-64
10. Karp G, Wolak A, Baumfeld Y, Assessment of aortic stiffness among patients with systemic lupus erythematosus and rheumatoid arthritis by magnetic resonance imaging: Int J Cardiovasc Imaging, 2016; 32; 935-44
11. Piga M, Saba L, Gabba A, Ultrasonographic assessment of bone erosions in the different subtypes of systemic lupus erythematosus arthritis: Comparison with computed tomography: Arthritis Res Ther, 2016; 18; 222
12. Zoma A, Musculoskeletal involvement in systemic lupus erythematosus: Lupus, 2004; 13; 851-53
13. Ilgen U, Yayla ME, Ates A, Antiphospholipid antibodies and non-thrombotic manifestations of systemic lupus: Lupus, 2018; 27; 665-69
14. Khan A, Shah MH, Nauman M, Clinical manifestations of patients with systemic lupus erythematosus (SLE) in Khyber Pakhtunkhwa: J Pak Med Assoc, 2017; 67; 1180-85
15. Uribe AG, Vila LM, McGwin G, The systemic lupus activity measure-revised, the Mexican systemic lupus erythematosus disease activity index (SLEDAI), and a modified SLEDAI-2K are adequate instruments to measure disease activity in systemic lupus erythematosus: J Rheumatol, 2004; 31; 1934-40
16. Ceccarelli F, Perricone C, Massaro L, The role of disease activity score 28 in the evaluation of articular involvement in systemic lupus erythematosus: Sci World J, 2014; 2014 236842
17. Juang YT, Peoples C, Kafri R, A systemic lupus erythematosus gene expression array in disease diagnosis and classification: A preliminary report: Lupus, 2011; 20; 243-49
18. Ball EM, Bell AL, Lupus arthritis, do we have a clinically useful classification?: Rheumatology (Oxford), 2012; 51; 771-79
19. Tan EM, Cohen AS, Fries JF, The 1982 revised criteria for the classification of systemic lupus erythematosus: Arthritis Rheum, 1982; 25; 1271-77
20. Romero-Diaz J, Isenberg D, Ramsey-Goldman R, Measures of adult systemic lupus erythematosus: Updated version of British Isles Lupus Assessment Group (BILAG 2004), European Consensus Lupus Activity Measurements (ECLAM), Systemic Lupus Activity Measure, Revised (SLAM-R), Systemic Lupus Activity Questionnaire for Population Studies (SLAQ), Systemic Lupus Erythematosus Disease Activity Index 2000 (SLEDAI-2K), and Systemic Lupus International Collaborating Clinics/American College of Rheumatology Damage Index (SDI): Arthritis Care Res, 2011; 63; S37-46
21. Arnett FC, Edworthy SM, Bloch DA, The American rheumatism association 1987 revised criteria for the classification of rheumatoid arthritis: Arthritis Rheum, 1988; 33; 315-24
22. Backhaus M, Burmester GR, Gerber T, Guidelines for musculoskeletal ultrasound in rheumatology: Ann Rheum Dis, 2001; 60; 641-49
23. Wakefield RJ, Balint PV, Szkudlarek M, Musculoskeletal ultrasound including definitions for ultrasonographic pathology: J Rheumatol, 2005; 32; 2485-87
24. Bizzaro N, Tozzoli R, Tonutti E, Variability between methods to determine ANA, anti-dsDAN and anti-ENA autoantibodies: A collaborative study with the biomedical industry: J Immunol Methods, 1998; 219; 99-107
25. Gezer O, Batmaz I, Sariyildiz MA, Sleep quality in patients with psoriatic arthritis: Int J Rheum Dis, 2017; 20; 1212-18
26. Xue C, Liu WL, Sun YHAssociation between systemic inflammation and autoimmunity parameters and plasma lipid in patients with rheumatoid arthritis: Zhonghua Xin Xue Guan Bing Za Zhi, 2011; 39; 941-45 [in Chinese]
27. Zhang YH, Li K, Xiao J, Comparison of ultrasound, radiography, and clinical investigations in the diagnosis of early rheumatoid synovitis in patients with nonspecific musculoskeletal symptoms: A multicenter cross-sectional study: Med Sci Monit, 2018; 24; 4372-78
28. Delle Sedie A, Riente L, Filippucci E, Ultrasound imaging for the rheumatologist. XV. Ultrasound imaging in vasculitis: Clin Exp Rheumatol, 2008; 26; 391-94
29. Micu MC, Berghea F, Fodor D, Concepts in diagnosing, scoring, and monitoring tenosynovitis and other tendon abnormalities in patients with rheumatoid arthritis, the role of musculoskeletal ultrasound: Med Ultrason, 2016; 18; 370-77
30. Liang C, Yang T, Wu G, Therapeutic effect of low-intensity pulsed ultrasound on temporomandibular joint injury induced by chronic sleep deprivation in rats: Am J Transl Res, 2019; 11; 3328-40
31. Iagnocco A, Ossandon A, Coari G, Wrist joint involvement in systemic lupus erythematosus. An ultrasonographic study: Clin Exp Rheurmatol, 2004; 22; 621-24
32. Hmamouchi I, Bahiri R, Srifi N, A comparison of ultrasound and clinical examination in the detection of flexor tenosynovitis in early arthritis: BMC Musculoskelet Disord, 2011; 12; 91
33. Ceccarelli F, Sciandrone M, Perricone C, Biomarkers of erosive arthritis in systemic lupus erythematosus: Application of machine leading models: PLoS One, 2018; 13; e0207926
34. Gladman D, Ginzler E, Goldsmith C, The development and initial validation of the systemic lupus international collaborating clinics/American College of Rheumatology Damage Index for Systemic Lupus Erythematosus: Arthritis Rheum, 1996; 39; 363-69
35. Ruano CA, Malheiro R, Oliveira JF, Ultrasound detects subclinical joint inflammation in the hands and wrists of patients with systemic lupus erythematosus without musculoskeletal symptoms: Lupus Sci Med, 2017; 4; e000184
36. Gabba A, Piga M, Vacca A, Joint and tendon involvement in systemic lupus erythematosus: An ultrasound study of hands and wrists in 108 patients: Rheumatol, 2012; 51; 2278-85
37. Iagnocco A, Ceccarelli F, Rizzo C, Ultrasound evaluation of hand, wrist and foot joint synovitis in systemic lupus erythematosus: Rheumatol, 2014; 53; 465-72
38. Ruiz-Curiel A, Diaz-Barreda MD, Gonzalez-Rodriguez M, Musculoskeletal ultrasound: An effective tool to help medical students improve joint inflammation: Med Ultrason, 2016; 18; 294-98
Figures
 Figure 1. Statistical analysis of joint involvement frequency in patients with SLE undergoing evaluation by musculoskeletal ultrasound. Among the 410 MCP joints, frequency of involvement from high to low was: MCP3, MCP4, MCP2, MCP1, and MCP5. MCP – metacarpal phalangeal, PIP – proximal interphalangeal.
Figure 1. Statistical analysis of joint involvement frequency in patients with SLE undergoing evaluation by musculoskeletal ultrasound. Among the 410 MCP joints, frequency of involvement from high to low was: MCP3, MCP4, MCP2, MCP1, and MCP5. MCP – metacarpal phalangeal, PIP – proximal interphalangeal. Figure 2. Musculoskeletal ultrasound evaluation for the joint diseases in the joints of patients with SLE. Among all 984 joints, the frequency of joint disease type from high to low was: synovitis, tenosynovitis, joint effusion, and bone erosion. MCP – metacarpal phalangeal, PIP – proximal interphalangeal.
Figure 2. Musculoskeletal ultrasound evaluation for the joint diseases in the joints of patients with SLE. Among all 984 joints, the frequency of joint disease type from high to low was: synovitis, tenosynovitis, joint effusion, and bone erosion. MCP – metacarpal phalangeal, PIP – proximal interphalangeal. Figure 3. The musculoskeletal ultrasound scores of patients with SLE (A) and patients with RA (B) were positively correlated with the serum level of IL-6. SLE – systemic lupus erythematosus; RA – rheumatoid arthritis; IL-6 – interleukin-6.
Figure 3. The musculoskeletal ultrasound scores of patients with SLE (A) and patients with RA (B) were positively correlated with the serum level of IL-6. SLE – systemic lupus erythematosus; RA – rheumatoid arthritis; IL-6 – interleukin-6. Tables
 Table 1. Demographic and clinical characteristics for 41 patients with SLE and 20 patients with RA involved in this study. We assessed the disease course and joint involvement, laboratory indexes (ANA titer, ENA spectrum, ESR, CRP and IL-6, C3, C4, RF, CCP) and scoring data (DAS28 score, SLEDAI score and ultrasonic score).
Table 1. Demographic and clinical characteristics for 41 patients with SLE and 20 patients with RA involved in this study. We assessed the disease course and joint involvement, laboratory indexes (ANA titer, ENA spectrum, ESR, CRP and IL-6, C3, C4, RF, CCP) and scoring data (DAS28 score, SLEDAI score and ultrasonic score). Table 2. Semi-quantitative assessment of degree of joint involvement in patients with SLE using ultrasonography. The MCP was the most seriously affected joint, followed by wrist joints, knee joints, and PIP joints.
Table 2. Semi-quantitative assessment of degree of joint involvement in patients with SLE using ultrasonography. The MCP was the most seriously affected joint, followed by wrist joints, knee joints, and PIP joints. Table 3. Comparative analysis of patients with SLE with and without arthralgia. The results showed that patients with SLE without arthralgia tended to demonstrate abnormality according to the musculoskeletal ultrasound, which suggests that musculoskeletal ultrasound is more sensitive for evaluating SLE arthritis.
Table 3. Comparative analysis of patients with SLE with and without arthralgia. The results showed that patients with SLE without arthralgia tended to demonstrate abnormality according to the musculoskeletal ultrasound, which suggests that musculoskeletal ultrasound is more sensitive for evaluating SLE arthritis. Table 4. Differences between patients with SLE and patients with RA determined using musculoskeletal ultrasound, laboratory indexes (including ESR and CRP), and DAS28 scores.
Table 4. Differences between patients with SLE and patients with RA determined using musculoskeletal ultrasound, laboratory indexes (including ESR and CRP), and DAS28 scores. Table 5. Correlation analysis between musculoskeletal ultrasound scores and inflammatory indexes/autoantibodies. There were positive correlations between RF/CCP antibody titer and ultrasound scores in patients with RA. There were significant correlations between dsDNA titer/RNP autoantibodies and ultrasound scores in patients with SLE. DAS28 score was positively correlated with ultrasound score in patients with RA and in patients with SLE.
Table 5. Correlation analysis between musculoskeletal ultrasound scores and inflammatory indexes/autoantibodies. There were positive correlations between RF/CCP antibody titer and ultrasound scores in patients with RA. There were significant correlations between dsDNA titer/RNP autoantibodies and ultrasound scores in patients with SLE. DAS28 score was positively correlated with ultrasound score in patients with RA and in patients with SLE. Table 1. Demographic and clinical characteristics for 41 patients with SLE and 20 patients with RA involved in this study. We assessed the disease course and joint involvement, laboratory indexes (ANA titer, ENA spectrum, ESR, CRP and IL-6, C3, C4, RF, CCP) and scoring data (DAS28 score, SLEDAI score and ultrasonic score).
Table 1. Demographic and clinical characteristics for 41 patients with SLE and 20 patients with RA involved in this study. We assessed the disease course and joint involvement, laboratory indexes (ANA titer, ENA spectrum, ESR, CRP and IL-6, C3, C4, RF, CCP) and scoring data (DAS28 score, SLEDAI score and ultrasonic score). Table 2. Semi-quantitative assessment of degree of joint involvement in patients with SLE using ultrasonography. The MCP was the most seriously affected joint, followed by wrist joints, knee joints, and PIP joints.
Table 2. Semi-quantitative assessment of degree of joint involvement in patients with SLE using ultrasonography. The MCP was the most seriously affected joint, followed by wrist joints, knee joints, and PIP joints. Table 3. Comparative analysis of patients with SLE with and without arthralgia. The results showed that patients with SLE without arthralgia tended to demonstrate abnormality according to the musculoskeletal ultrasound, which suggests that musculoskeletal ultrasound is more sensitive for evaluating SLE arthritis.
Table 3. Comparative analysis of patients with SLE with and without arthralgia. The results showed that patients with SLE without arthralgia tended to demonstrate abnormality according to the musculoskeletal ultrasound, which suggests that musculoskeletal ultrasound is more sensitive for evaluating SLE arthritis. Table 4. Differences between patients with SLE and patients with RA determined using musculoskeletal ultrasound, laboratory indexes (including ESR and CRP), and DAS28 scores.
Table 4. Differences between patients with SLE and patients with RA determined using musculoskeletal ultrasound, laboratory indexes (including ESR and CRP), and DAS28 scores. Table 5. Correlation analysis between musculoskeletal ultrasound scores and inflammatory indexes/autoantibodies. There were positive correlations between RF/CCP antibody titer and ultrasound scores in patients with RA. There were significant correlations between dsDNA titer/RNP autoantibodies and ultrasound scores in patients with SLE. DAS28 score was positively correlated with ultrasound score in patients with RA and in patients with SLE.
Table 5. Correlation analysis between musculoskeletal ultrasound scores and inflammatory indexes/autoantibodies. There were positive correlations between RF/CCP antibody titer and ultrasound scores in patients with RA. There were significant correlations between dsDNA titer/RNP autoantibodies and ultrasound scores in patients with SLE. DAS28 score was positively correlated with ultrasound score in patients with RA and in patients with SLE. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








