24 December 2020: Clinical Research
Comparison of Second- and Third-Generation Parathyroid Hormone Test Results in Patients with Chronic Kidney Disease
Magdalena Wójtowicz1ABCDEF, Wiesław Piechota1CDEF*, Zofia Wańkowicz2DEF, Jerzy Smoszna2DE, Stanisław Niemczyk2DEDOI: 10.12659/MSM.928301
Med Sci Monit 2020; 26:e928301
Abstract
BACKGROUND: In patients with chronic kidney disease (CKD), secondary hyperparathyroidism is assessed by measuring serum parathyroid hormone (PTH) levels. Well-established, recommended, second-generation intact parathyroid hormone (iPTH) tests are typical; rarely are more recent third-generation PTH 1–84 assays used. The agreement between results of the 2 tests in patients with CKD has not been sufficiently defined.
MATERIAL AND METHODS: This study aimed to compare Roche second- and third-generation PTH assays by establishing a quantitative relationship between the results of assays in patients with CKD and assessing degree of their correlation with kidney function and calcium-phosphate and bone metabolism parameters. In 205 patients with stages 3 to 5D CKD and 30 healthy controls, we measured levels of iPTH and PTH (1–84), creatinine, urea, cystatin C, calcium, inorganic phosphate, magnesium, alkaline phosphatase, bone alkaline phosphatase, osteocalcin, and β-CrossLaps.
RESULTS: The third-generation PTH assay results were more than 40% lower than those obtained with the second-generation test in patients undergoing dialysis and approximately 30% lower in patients in the pre-dialysis period. PTH concentrations determined with both assays were almost to the same extent correlated with calcium-phosphate and bone metabolism parameters, and renal function indices. Formulas have been developed enabling 2-way conversion of PTH results determined with both the second- and third-generation PTH assays: For dialyzed patients, PTH (1–84)=0.5181iPTH+18.0595. Serum osteocalcin, β-CrossLaps, and total calcium were independent predictors of PTH levels.
CONCLUSIONS: Correcting for the established quantitative differences, the second-and third-generation PTH tests can be used interchangeably, given the almost identical pathophysiological correlations of their results with calcium-phosphate and bone metabolism parameters.
Keywords: Hyperparathyroidism, Secondary, Parathyroid Hormone, chronic kidney disease, Case-Control Studies, Kidney Function Tests, Linear Models, Phosphates, Renal Dialysis, Renal Insufficiency, Chronic
Background
Chronic kidney disease (CKD) is considered to be a disease of 21st century civilization. Its occurrence may be the result of complications of other conditions, such as diabetes, cardiovascular disease, or hypertension. CKD is also a common and final pathway to the vast majority of primary kidney diseases. During its course, patients develop other disorders, including those of the endocrine system, such as secondary hyperparathyroidism (SHPT). SHPT incidence increases with the decrease in glomerular filtration rate (GFR) and it affects up to 20% to 25% of patients who have stage 5 CKD [1].
The basic diagnostic criterion for SHPT is serum parathyroid hormone (PTH) concentration. Currently, the commonly used and recommended test for PTH determination is the second-generation intact PTH (iPTH) test [2]. Apart from estimating the whole biologically active molecule, 1–84 PTH, the test also measures its forms and fragments that are inactive or probably exerting opposite effects. In patients with CKD, as the GFR decreases, fragments of 7–84 PTH that are physiologically cleared by the kidneys accumulate in the circulation. The PTH concentrations determined by the second-generation test may be overestimated in these patients because the total concentrations of the whole particle 1–84 PTH and the 7–84 fragments are measured together, which can lead to an erroneous assessment of the severity of SHPT [3,4]. Consequently, the result may be inappropriate therapeutic decisions. The solution to the problem may be the third-generation test for PTH (1–84), which measures only the whole hormone molecule and would appear to be more appropriate than the first- and second-generation PTH tests. However, practical application of the third-generation test is hindered because the optimal range of PTH results in patients with stage 5 CKD who are undergoing dialysis is still unknown.
The main objective of the current project was to establish quantitative relationships between PTH measurements obtained with the second- and third-generation tests in patients with stages 3 to 5D CKD. The specific objectives were to assess the correlations between PTH levels obtained with both the second- and third-generation tests and estimated GFRs (eGFRs) and calcium-phosphate and bone metabolism parameters, as well as to attempt to select among them potential predictors of PTH concentrations in patients with CKD.
Material and Methods
The study included 205 patients with stages 3 to 5D CKD (127 men and 78 women, mean age 65±13) who were in the care of the Department of Internal Medicine, Nephrology and Dialysis of the Military Institute of Medicine in Warsaw and a control group of 30 healthy volunteers (16 men and 14 women aged 59±13 years). Healthy volunteers were recruited from consecutive willing laboratory technicians and their family members. The study was performed with the consent of the Bioethical Committee of the Military Institute of Medicine in Warsaw, which was given on February 17, 2016 in Resolution No. 10/WIM/2016. The characteristics of the study groups are presented in Table 1.
Venous blood was collected in appropriate vacuum tubes using a closed system (BD Vacutainer®). In patients with CKD in the pre-dialysis period and on home peritoneal dialysis (HPD), blood was collected during follow-up visits to the Nephrological Outpatient Clinic. In patients treated with hemodialysis (HD), blood was collected before mid-week dialysis in the Dialysis Department. Blood samples (approximately 10 mL) were collected from the control group after they gave written informed consent.
The serum required for the tests was obtained by centrifugation with cooling of the blood samples under standard conditions, ie 10 min at 4000 rpm. The serum samples used were free of visible traces of hemolysis and significant lipemia. All of the routine tests were performed on the same day. The remaining serum was frozen at −70°C and used for subsequent scheduled tests up to 3 months after collection. Ionized calcium levels were determined in serum from anaerobic blood tubes. The planned set of laboratory tests for all 235 subjects included: PTH determined with the second-generation tests (intact PTH, iPTH) and the third-generation PTH (1–84) test, creatinine, urea, cystatin C, total calcium, ionized calcium, inorganic phosphate, magnesium, alkaline phosphatase (ALP), bone alkaline phosphatase (BAP), osteocalcin, and isomerized C-terminal telopeptides of type I collagen (β-CrossLaps). GFRs were calculated using eGFR according to the abbreviated Modification of Diet in Renal Disease study equation, and GFR based on the concentration of creatinine and cystatin C as calculated with the CKD-EPI Creatinine-Cystatin Equation (2012) [5]. The use of the second equation was intended to increase the accuracy of the study.
The serum PTH concentrations were determined with Roche Diagnostics second- and third-generation tests using an automated Cobas e601 analyzer from the same manufacturer. That analyzer also was used to determine osteocalcin and β-CrossLaps concentrations.
BAP levels were determined with an immunoenzymatic method from Immunodiagnostic Systems (IDS). Biochemical analytes in serum were determined using ready-made reagent kits for automatic analyzers from Beckman Coulter (AU) and Roche Diagnostics (c501). The concentration of ionized calcium was determined with a Siemens 900 Series blood gas analyzer.
Statistical analysis of the results was carried out using Statistica 12 software (StatSoft). Descriptive statistics were used for the characteristics of the study groups and the control group. The normality of the distributions of all analytes was determined with a Shapiro-Wilk test. None of the analytes showed a distribution close to normal in any of the groups studied, hence the use of non-parametric methods prevailed in this research. Multiple regression analysis was used after the data were logarithmically transformed to normalize their distribution. This analysis was used to select independent predictors of PTH concentration. Linear regression was used to describe the relationship between iPTH and PTH (1–84) concentrations, and to obtain the equations for each patient group. Spearman rank correlations were used to determine the correlation between iPTH and PTH (1–84) and renal function biochemical tests, calcium, phosphate levels, and bone metabolism parameters. The significance of the differences in the results between the groups was verified with Kruskal-Wallis and Mann-Whitney U tests, and with a Significance of the Difference Between Two Slopes Calculator (
Results
Table 2 lists the concentrations of the measured analytes and the ages of the patients in the studied groups and the subjects in the control group presented as the means and standard deviations together with the significance of differences in comparison with the controls and between studied groups. With the exception of age, all parameters in the patients with CKD differed in terms of statistical significance compared with the control group. There were no statistically significant differences in mean iPTH and PTH (1–84) concentrations between the groups of patients on HD and HPD. PTH concentrations determined with the third-generation test were lower than those determined with the second-generation test by more than 40% in patients on dialysis, approximately 30% in patients in the pre-dialysis period, and more than 10% in the subjects in the control group.
The correlations between PTH concentrations measured with second- and third-generation tests in the patients and in the control group, as well as in all subjects who took part in the study, are shown in Table 3. The strength of these correlations is very high in all the studied groups.
Scattergrams of results of PTH (1–84) versus iPTH are shown in Figures 1–3, respectively, for all the patients with CKD, the patients on hemodialysis, and the patients in the pre-dialysis period. The differences in PTH concentration determined with the 2 tests increased with rising PTH concentration, which is illustrated by the Bland-Altman graph in Figure 4 for the patients with stages 3 to 5 CKD. Table 4 shows the original conversion formulas for clinical practice developed by our team, allowing comparison of the results of PTH determinations between the second- and third-generation tests. There is a statistically significant difference between slopes of the linear regression equations for the patients on dialysis and those in the pre-dialysis period.
Table 5 shows correlations between the PTH concentrations obtained with the second- and third-generation tests and other laboratory parameters, that is, with biochemical indicators of renal function, GFR, calcium-phosphate metabolism parameters, and bone turnover markers. The estimated correlations show that the strength of the association between the PTH levels determined with tests of both generations and renal function indicators is statistically significant in all patients with CKD and in the subgroup in the pre-dialysis period, and disappears in patients on dialysis. The correlation coefficients between PTH concentration measured with the-second generation test and kidney function indicators are slightly higher than those for the third-generation test, but without statistical significance. This may be a result of recognition by the second-generation test of the epitopes of PTH fragments. Removal of the fragments is impaired in patients with CKD and the second-generation tests have lower analytical specificity for biologically active PTH. PTH measurements with the second- and third-generation tests show a similar strength of association with calcium and phosphate concentrations.
Pathophysiological associations between PTH levels and serum concentrations of bone mineral components are strong in the patients in the pre-dialysis period and all of the patients with CKD. A similarly strong correlation was observed between PTH results obtained with the tests of both generations and bone turnover markers. The strong correlation between PTH concentrations and β-CrossLaps, BAP, and osteocalcin in almost all the groups studied (with the exception of patients on HPD in the case of BAP and osteocalcin) is noteworthy.
In multiple linear regression models, only analytes were included that were significantly correlated with iPTH and PTH (1–84), according to the Spearman test. The independent predictors of both iPTH and PTH (1–84) levels in all 205 patients with CKD were total calcium, osteocalcin, and β-CrossLaps (Table 6). In the patients with CKD in the pre-dialysis period, independent predictors of both iPTH and PTH (1–84) levels were GFR expressed by the CKD-EPI creatinine-cystatin formula and serum osteocalcin concentration (Table 7). In patients on HD, independent predictors of both iPTH and PTH (1–84) levels were serum ionized calcium and osteocalcin (Table 8), and in patients treated with HPD, only osteocalcin (Table 9).
Discussion
The results of the present study show that PTH concentrations determined with the third-generation test in 205 patients with CKD stages 3 to 5 were lower by more than 40% than those determined with the second-generation test in patients on dialysis (HD and HPD), and by approximately 30% in patients in the pre-dialysis period of CKD. Similar discrepancies were reported when a third-generation PTH test first became available in clinical laboratories [6,7]. Later, Bekő et al. compared the third-generation Elecsys PTH (1–84) and Liaison PTH (1–84) tests with 3 second-generation tests (Elecsys iPTH, Architect iPTH, and Liaison N-tact) and found that average iPTH levels in 110 patients on HD were about 33% to 51% higher than PTH (1–84) levels (
Second-generation PTH assays measure both the active 1–84 PTH molecule and its fragments, mainly 7-84 PTH. The third-generation PTH test measures the concentration of the whole physiologically active PTH molecule. As the concentration of iPTH increases and the GFR decreases, the discrepancies increase, not only between the results of the second- and third-generation tests but also within the individual second-generation tests from different manufacturers [10,11]. These discrepancies may result from the severity of CKD and the number of fragments and forms of PTH assessed with these tests [10]. Eddington et al. compared the results of PTH tests performed in 17 laboratories in samples obtained from the same group of 37 patients on HD. These laboratories used the second-generation PTH tests. Eight methods were used for testing, with 5 different assays from 4 different manufacturers. Because the PTH concentrations were significantly different, even using the same method, the results were adjusted using correction factors, which led to the conclusion that as many as 21% of the patients would require a change in clinical management [12]. Also, Kuczera et al. compared the results of PTH concentration determined with chemiluminescence (Architect Intact PTH) and electrochemiluminescence (Elecsys iPTH) in 77 patients on HD and found that they were significantly different (
Taniguchi et al. and Donati et al. described the challenge posed when the type of test used has the potential to impact therapeutic decisions [14,15]. Taniguchi et al. used second- and third-generation tests to measure PTH concentrations in 738 patients on HD and demonstrated that 18% of those who were tested with the third-generation assay would be classified into a different therapeutic category, possibly requiring different treatment [14]. In 19 patients on HD, Donati et al. compared PTH concentrations measured with second-generation tests from 2 different manufacturers, which resulted in statistically significant differences in the results. The authors suggested that the transfer of a patient to another dialysis center, combined with changes in the method used to determine the PTH concentration, might affect therapeutic decisions [15].
Our study showed that PTH concentrations obtained with the second- and third-generation tests were strongly correlated in all patients with CKD and in the control group. In addition, the relationship between these concentrations was highly linear. Thanks to this, regression equations were created, which can serve as simple formulas to compare the results obtained with both tests. Similar relationships of PTH concentrations determined with both generations of Roche Diagnostics tests have been established for patients in the pre-dialysis period and on dialysis. The formula put forth for the former patients O’Flaherty et al. was biointact PTH (1–84)=0.62 intact PTH+9.88 [16]. The formula put forth for the latter patients by Fukagawa M et al. was intact PTH=whole PTH×1.7 [17]. Because the present study included a large number of patients, we were able to show that the formulas for the patients in the pre-dialysis period and on dialysis were different. Therefore, we suggest that the practical application of such formulas should take into account this finding.
In our study, iPTH and PTH (1–84) concentrations were correlated with calcium-phosphate and bone metabolism parameters and GFR values in the same way, i.e., with similar strength and statistical significance. Similar conclusions have been presented by Rodriguez-Osorio et al., Kurajoh et al., and Graf et al. [18–20]. A study also has been published, however, suggesting that the results obtained with the third-generation PTH tests are more strongly correlated with calcium-phosphate and bone metabolism parameters in patients with CKD than those measured with second-generation tests. The study also suggested that the PTH (1–84) assay may better reflect mineral disorders, probably with more accurate assessment of bone turnover in CKD, but additional confirmatory studies are needed, including bone biopsy [16]. Many correlations found in our study confirm the pathophysiological relationship between PTH and eGFR, calcium, and inorganic phosphate concentrations in the serum of patients with CKD that have been demonstrated by other authors [21,22].
The present study of bone metabolism markers in patients in the pre-dialysis period and on dialysis showed that PTH levels determined with the second- and third-generation tests strongly were positively correlated with these markers, especially with serum concentrations of osteocalcin and β-CrossLaps. Also noteworthy are the positive correlations between PTH levels determined with both the tests and ALP activity and BAP concentration (except in patients on HPD). These statistically significant correlations of varying strengths also have been demonstrated by other researchers [10,18,23–26]. Davina et al., in 32 men who were not diabetic and had stages 4 to 5 CKD in the pre-dialysis period, showed the usefulness of the combined BAP and iPTH determination as a set of reliable predictors of reduced bone mineral density (sensitivity 79.9%, specificity 81.5%). They also found a significant positive correlation between BAP and iPTH levels and a statistically significant negative correlation between BAP and eGFR values, suggesting that high BAP concentration is associated with SHPT and decreasing renal function [27]. Other authors have indicated that determining the concentration of 3 or more bone turnover markers more accurately evaluates the course of mineral and bone disorders in patients with CKD than determination of single markers [28,29]. Despite many studies, no ideal single biomarker of bone turnover has been discovered that can be used to guide treatment of patients with CKD and secondary hyperparathyroidism [30,31].
Along with PTH, ALP, and BAP, osteocalcin is considered a useful marker of mineral and bone disorders in the course of CKD [28]. In all of the patients in our study, osteocalcin concentration was an independent parameter associated with PTH concentration determined by second- and third-generation tests. We also found that the independent predictors of PTH levels were β-CrossLaps concentration in all the patients with CKD, CKD-EPI creatinine-cystatin in patients in the pre-dialysis period, and ionized calcium in patients on HD. Results of both generations of PTH tests showed very strong and similar correlations with bone marker levels. Other researchers, using multiple regression models, have been able to demonstrate correlations between PTH concentrations determined with the third-generation DiaSorin Liaison XL PTH and Fujirebio Lumipulse PTH tests and BAP concentrations in patients on HD [23].
The third-generation PTH tests measure the whole molecule of the hormone, hence, the ranges recommended for patients on dialysis can be determined with much greater accuracy and in a narrower range. The great advantage of the third-generation tests is the possibility of their standardization and clinically meaningful stratification for different groups of patients. The study of 119 patients on dialysis conducted by Cavalier et al. [23], who compared the results of the third-generation DiaSorin Liaison XL PTH and Fujirebio Lumipulse PTH tests with those of the PTH 1–84 Roche Diagnostics, showed that test re-standardization using the WHO 1–84 PTH standard significantly reduces the differences between results from various manufacturers. Taking into account the Kidney Disease Improving Global Outcomes (KDIGO) recommendations, Cavalier et al. determined that when using the Fujirebio third-generation PTH test for patients on dialysis, the optimal range should be 84 to 378 pg/mL, and for DiaSorin, 76 to 342 pg/mL. Bekő et al. set new, much lower recommended target ranges for patients on dialysis using third-generation tests: 65 to 258 pg/mL for Liaison PTH 1–84 and 68 to 288 pg/mL for Elecsys PTH (1–84) [8]. These ranges are much lower (and narrower) than those recommended by the KDIGO, i.e., 2 and 9 times the upper limit of normal for second-generation PTH tests. Cavalier et al., after re-standardization of the third-generation PTH tests of DiaSorin and Roche, also established reference ranges for a healthy population of 11 to 46 pg/mL and 8 to 45 pg/mL, respectively [32]. PTH (1–84) concentration has been shown to be a good indicator of SHPT (area under the curve=0.926;
Since the introduction of the third-generation tests (IRMA w-PTH Scanti Body Co. Ltd.), it has been established that the second-generation tests overestimate the concentration of PTH, i.e., 1–84 PTH [35]. Recommendations for use of third-generation tests for patients with CKD in everyday practice are still lacking [36]. In addition, the interpretation of the third-generation tests in a manner similar to the interpretation of the second-generation tests does not bring new information about mineral and bone disorders in patients on dialysis [36,37]. The inability to optimally interpret results of PTH tests and make therapeutic decisions based on them is mainly associated with the determination of PTH C-terminal fragments (not determined solely by third-generation tests) [38]. Until now, the presence of oxidative forms of PTH (physiologically inactive) also has been ignored in development of subsequent generations of PTH tests [39].
When using the second-generation PTH tests, KDIGO currently recommends additional, regular determination of calcium, inorganic phosphate, and possibly ALP and BAP levels in serum. In the case of patients on dialysis, it is suggested that interpretation and therapeutic decision-making using third-generation PTH tests should be based on BAP concentration, and modification of therapy in these individuals should be considered when significant dynamics of change in PTH concentration occur, even within the recommended ranges [40,41].
The precise PTH concentrations from second- or third-generation tests that represent the occurrence of secondary hyperparathyroidism in patients with CKD are unknown [39]. At the same time, new drugs and therapies are emerging for this group of patients, and a good marker is needed to monitor their efficacy [42]. Such a marker should be easily available, as is the case with PTH, which has become a routine test in many laboratories [43].
The third-generation PTH tests actually measure the entire PTH molecule. Recalibration of these tests using the IS 95/646 standard reduces the discrepancies between the results obtained with different third-generation PTH assays. In practice, this makes it possible to determine cut-off points, which are useful in the diagnosis and treatment of mineral and bone disorders in patients on dialysis. The correlations between the results of the second- and third-generation PTH tests in our patients with CKD in the pre-dialysis period and those on renal replacement therapy may be a starting point for further studies to improve the usefulness of third-generation PTH tests for the diagnosis and treatment of secondary hyperparathyroidism in these individuals.
Conclusions
The third-generation test for the determination of PTH in serum produces results lower than the second-generation test. The differences increase with the degree of renal impairment and amount to about 30% in patients with CKD during the pre-dialysis period and over 40% in patients on dialysis.
PTH concentrations determined with the second- and third-generation tests are strongly linearly correlated in all patients with stages 3 to 5 CKD, including those on dialysis. The formulas we have developed allow for 2-way recalculation of the concentrations obtained with the second- and third-generation tests and preliminary interpretation of the results obtained with the third-generation test on the basis of previous experience.
PTH concentrations determined with the second- and third-generation tests were were correlated to almost the same degree with calcium-phosphate and bone metabolism parameters, GFR, and biochemical renal function indices. None of these methods show an advantage in this respect.
Osteocalcin, β-CrossLaps, and calcium concentrations were independent predictors of PTH concentrations determined by both generations of tests in patients with CKD. The statistical significance of the PTH predicators depends on the stage of CKD.
Correcting for the established quantitative differences in the second- and third-generation PTH tests, these assays can be used interchangeably because of the almost identical pathophysiological correlations of their results with calcium-phosphate and bone metabolism parameters.
Figures
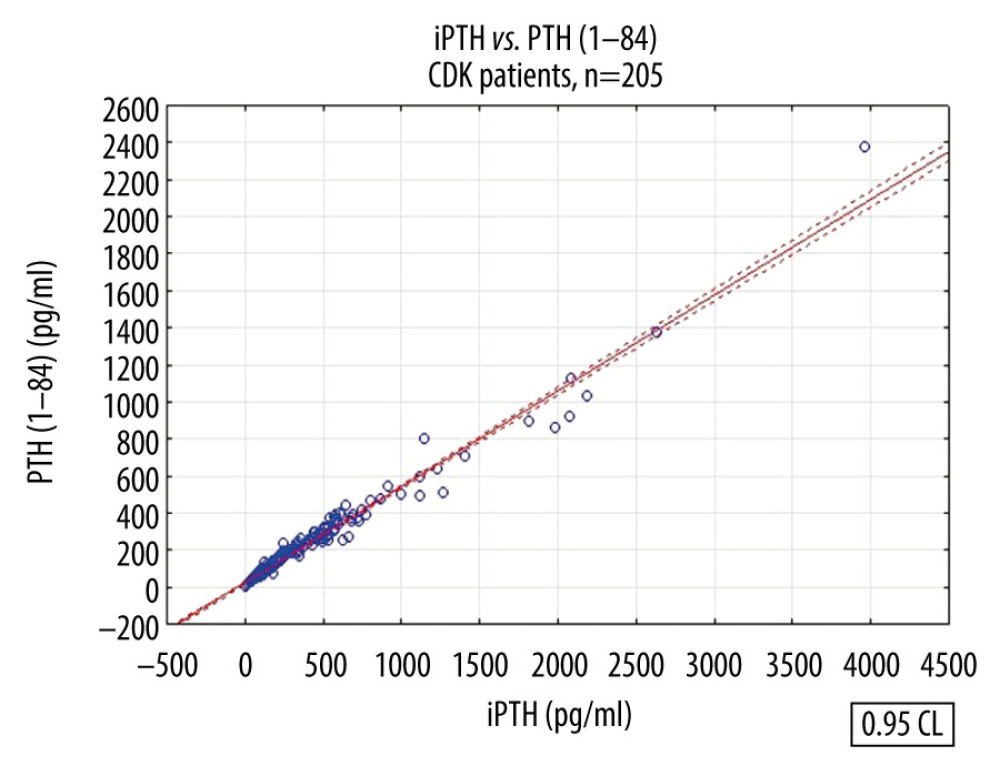 Figure 1. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in patients with CKD stages 3 to 5D.
Figure 1. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in patients with CKD stages 3 to 5D. 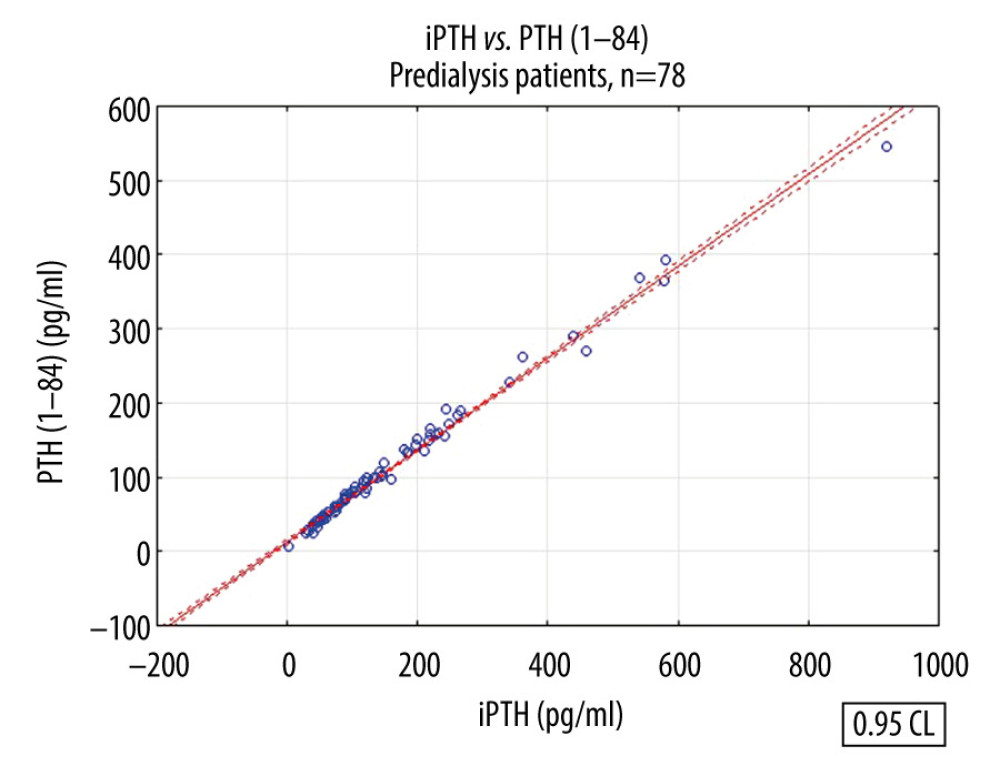 Figure 2. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in pre-dialysis patients.
Figure 2. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in pre-dialysis patients. 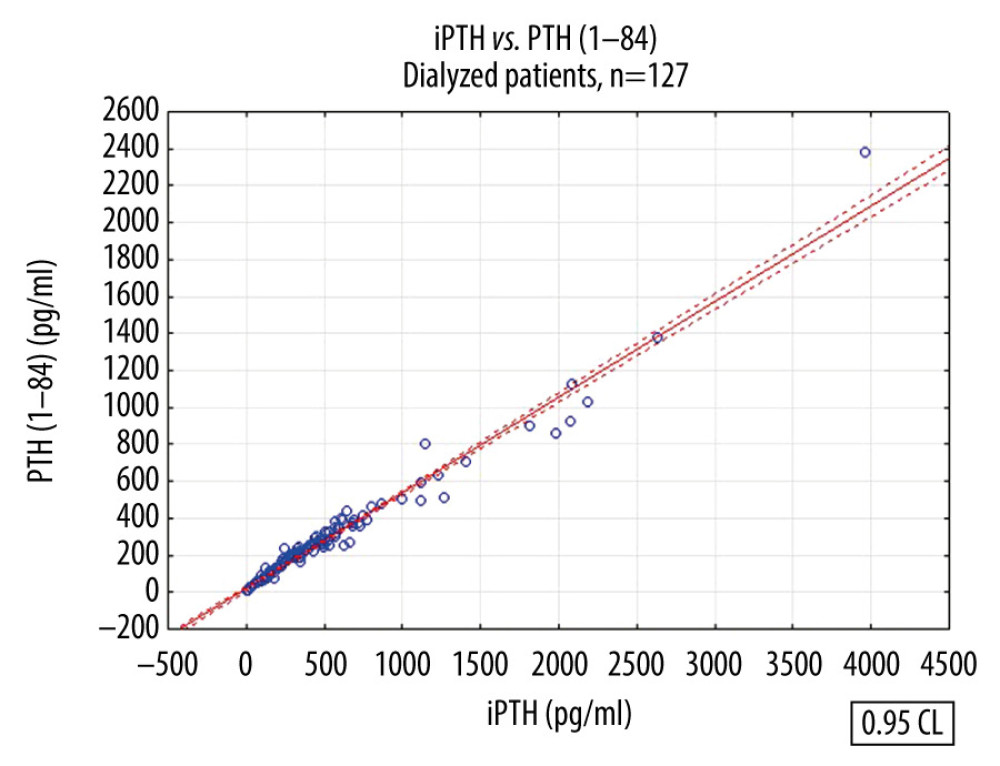 Figure 3. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in dialyzed patients.
Figure 3. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in dialyzed patients. 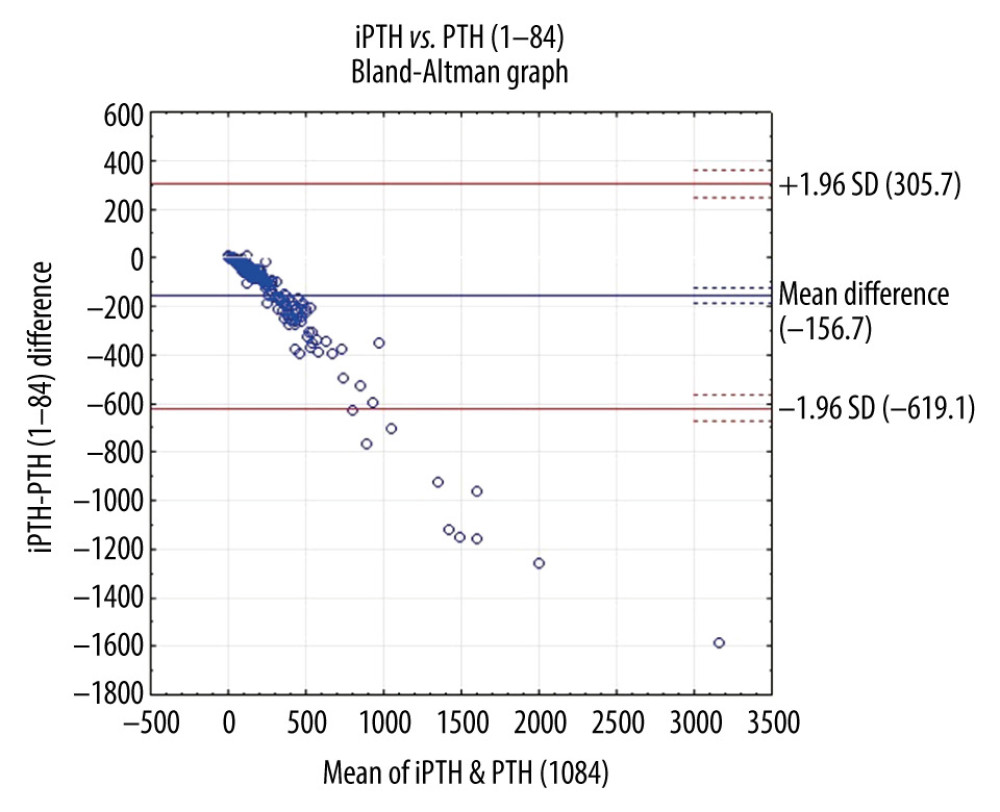 Figure 4. Comparison of second- and third-generation parathyroid hormone assays in patients with chronic kidney disease (n=205) (Bland-Altman method).
Figure 4. Comparison of second- and third-generation parathyroid hormone assays in patients with chronic kidney disease (n=205) (Bland-Altman method). Tables
Table 1. Characteristics of the study group and the control group. Table 2. Intact parathyroid hormone, parathyroid hormone 1–84, and other laboratory parameters and age in various subgroups of patients with CKD and in the control group.
Table 2. Intact parathyroid hormone, parathyroid hormone 1–84, and other laboratory parameters and age in various subgroups of patients with CKD and in the control group.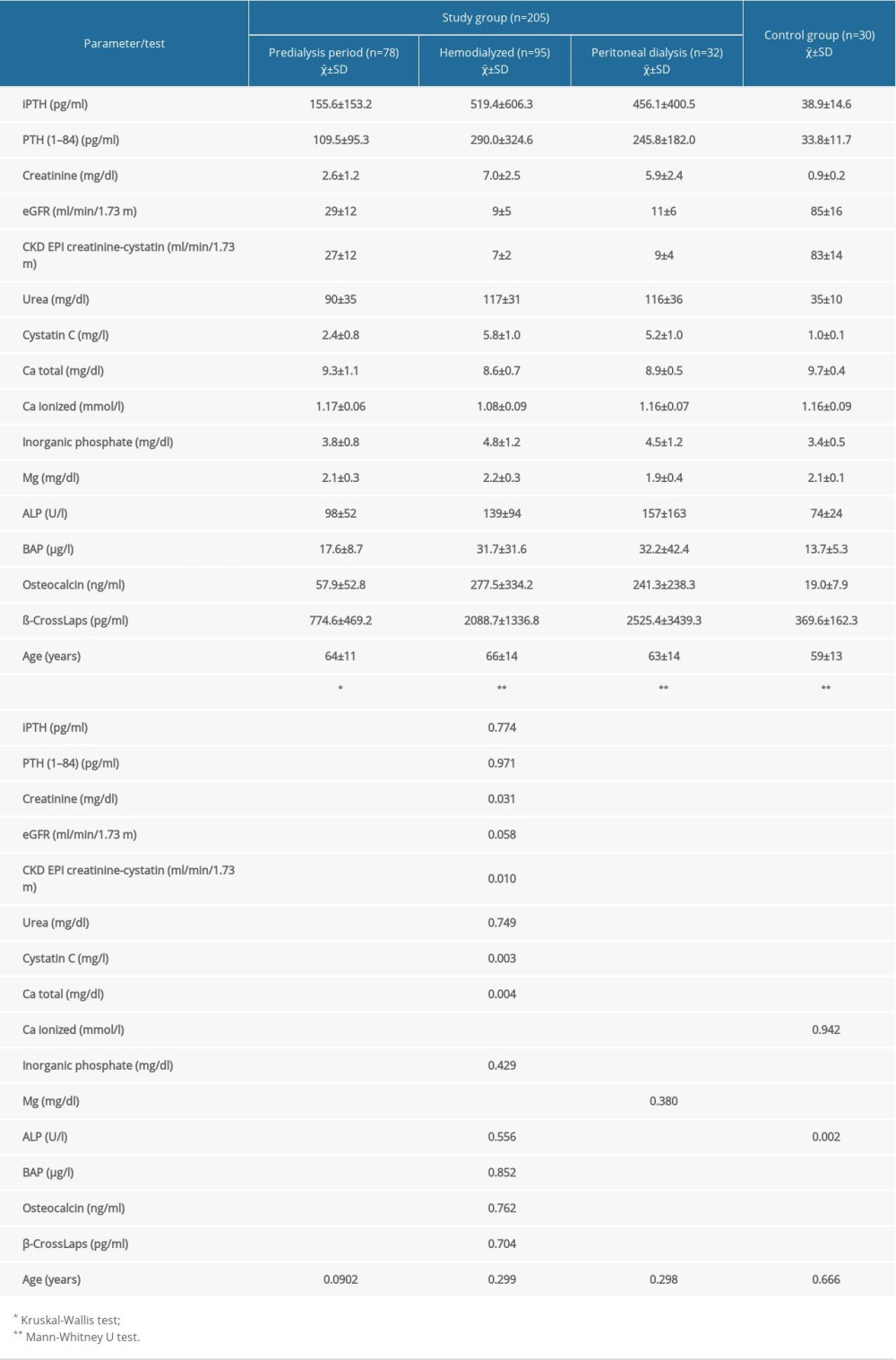 Table 3. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in different study groups (Spearman method).
Table 3. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in different study groups (Spearman method).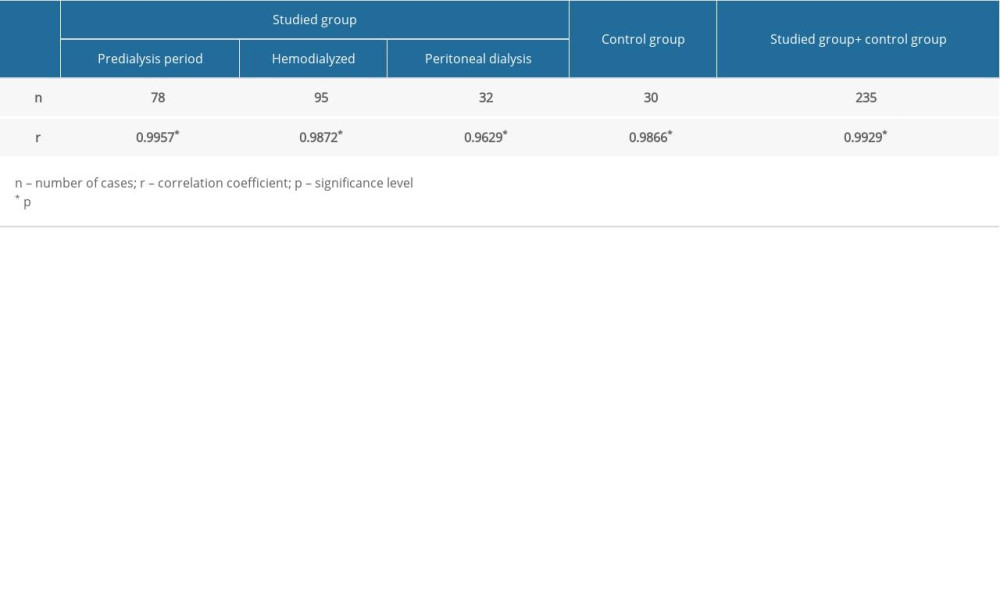 Table 4. Formulas enabling comparison of parathyroid hormone concentration results determined with second- and third-generation tests*.
Table 4. Formulas enabling comparison of parathyroid hormone concentration results determined with second- and third-generation tests*.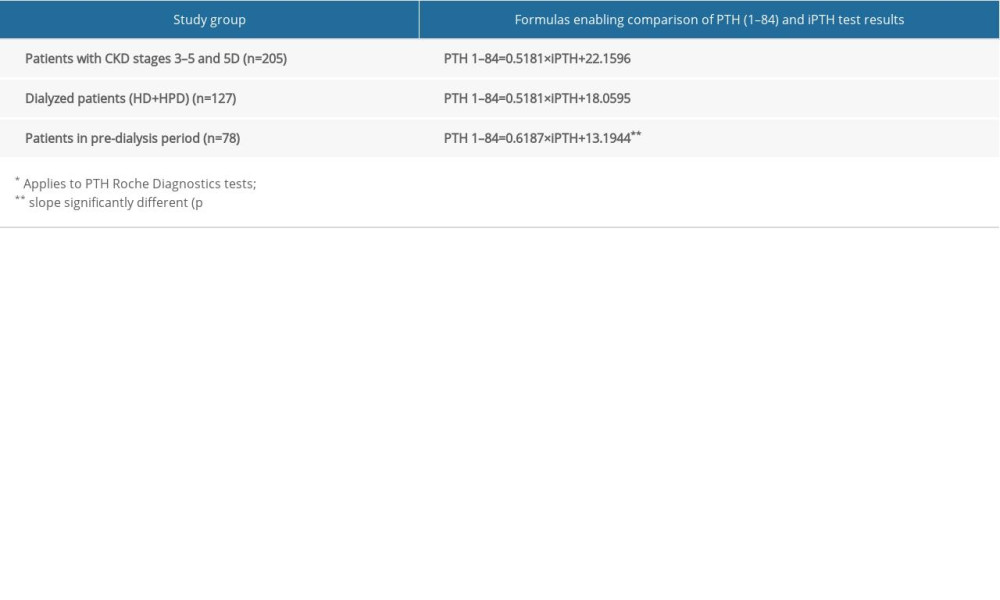 Table 5. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations and kidney function indices, calcium-phosphate metabolism parameters, and bone metabolism markers (Spearman method).
Table 5. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations and kidney function indices, calcium-phosphate metabolism parameters, and bone metabolism markers (Spearman method).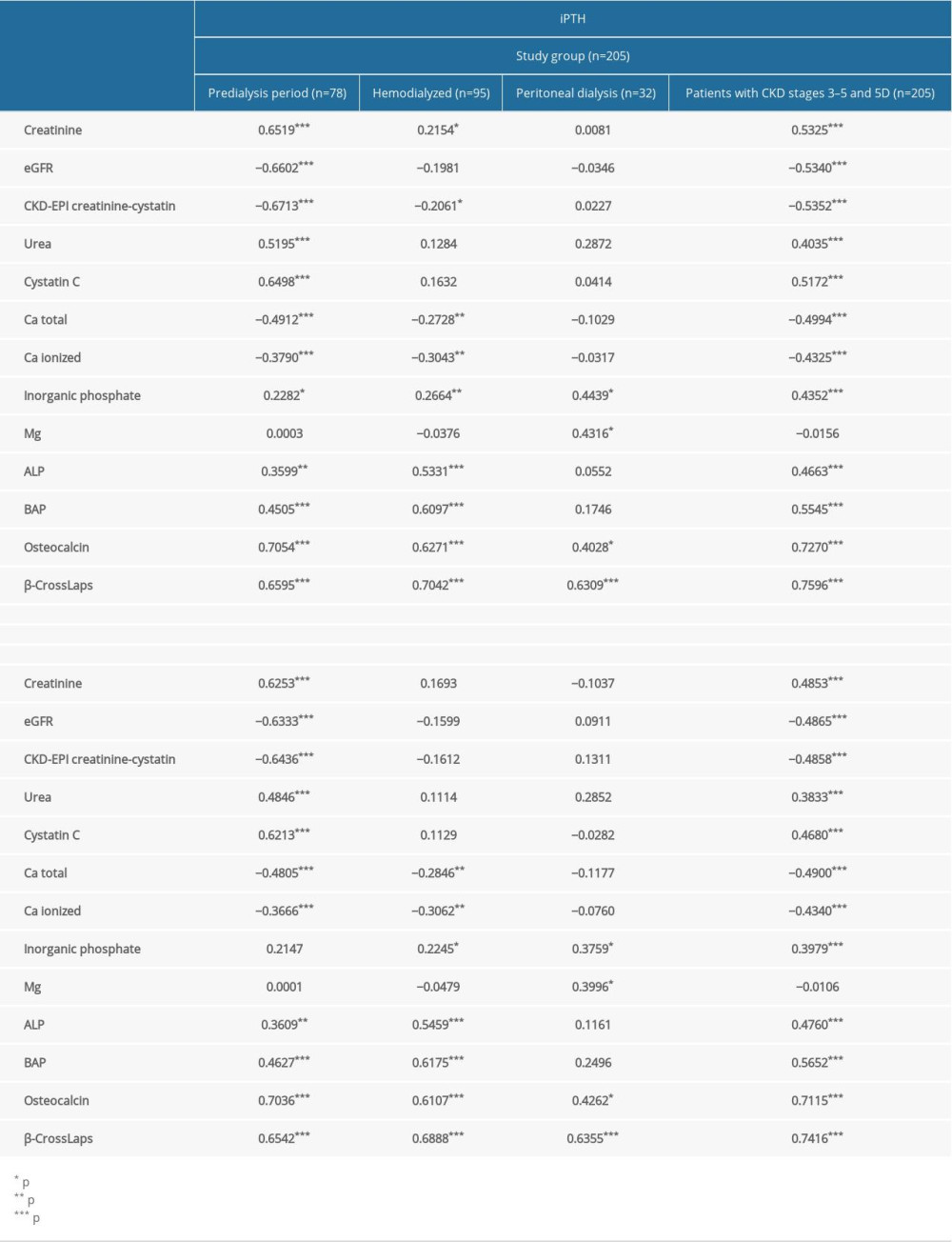 Table 6. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with stages 3 to 5D CKD (n=205).
Table 6. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with stages 3 to 5D CKD (n=205).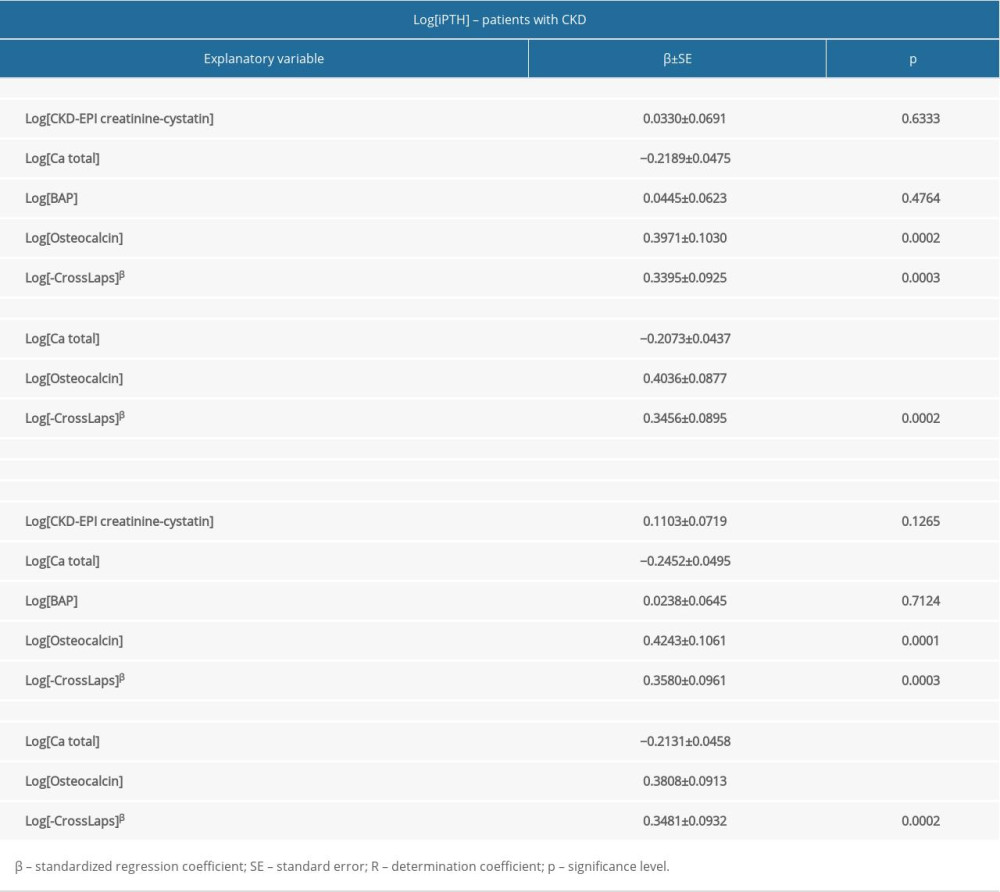 Table 7. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with CKD in the pre-dialysis period (n=78).
Table 7. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with CKD in the pre-dialysis period (n=78).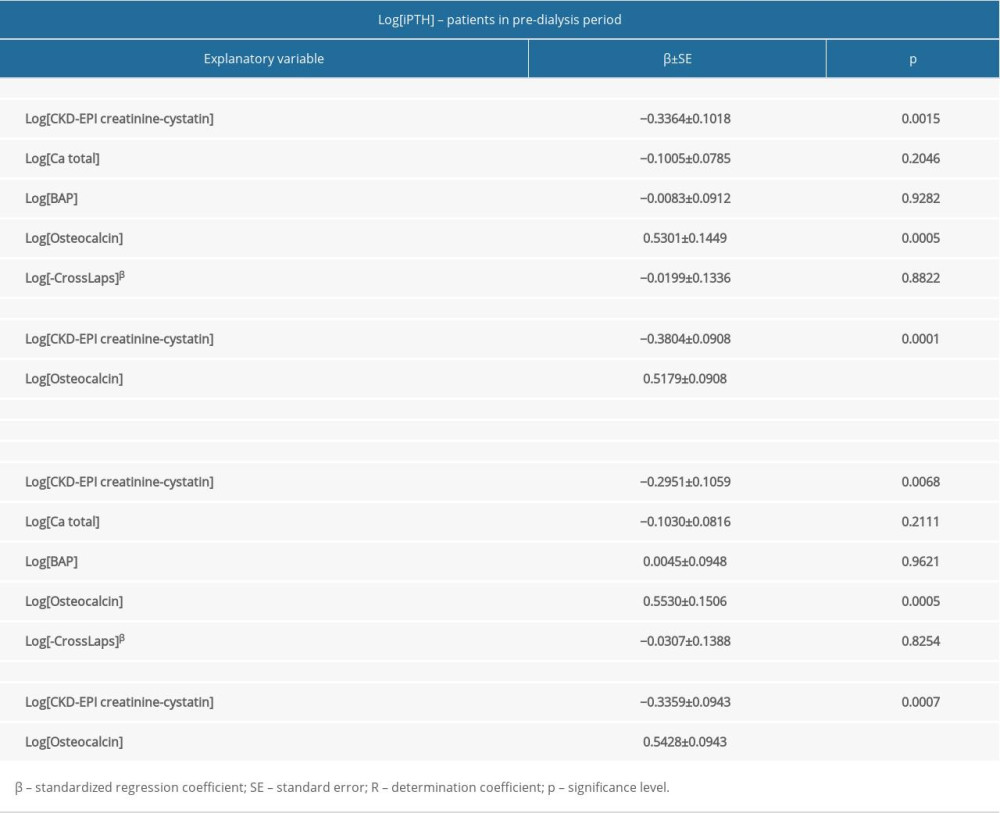 Table 8. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in hemodialyzed patients (n=95).
Table 8. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in hemodialyzed patients (n=95).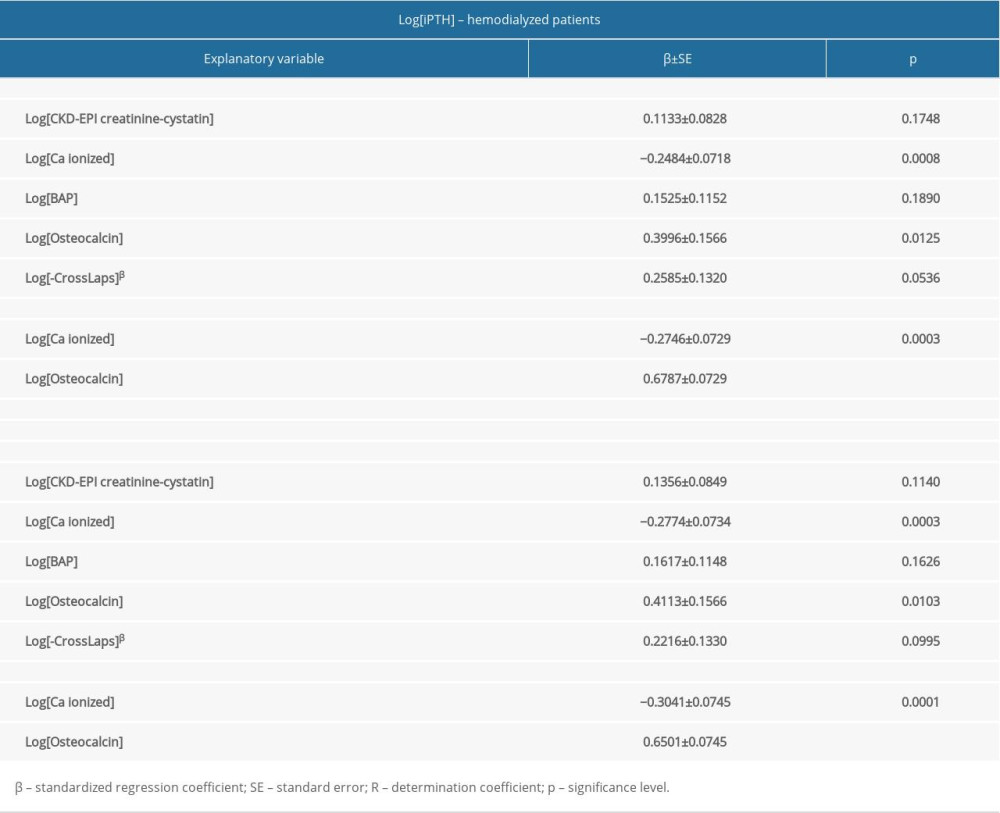 Table 9. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients on home peritoneal dialysis (n=32).
Table 9. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients on home peritoneal dialysis (n=32).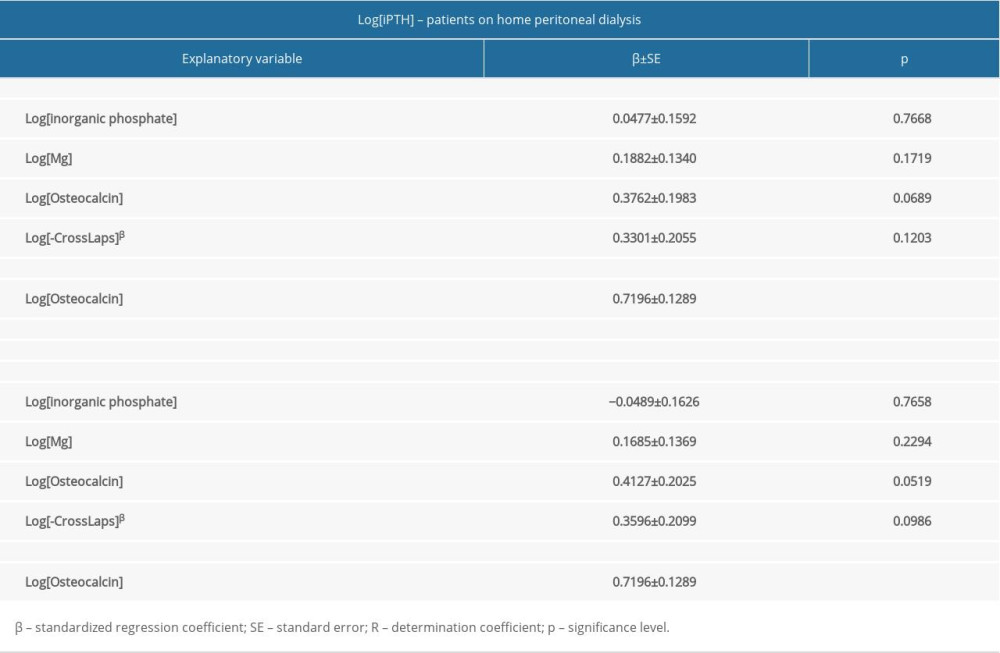
References
1. Zawierucha J, Małyszko J, Małyszko JContemporary opinions on the diagnosis and treatment of secondary hyperparathyroidism: Przeglad Lekarski, 2016; 73; 497-94 [in Chinese]
2. Ketteler M, Block GA, Evenepoel P, Diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder: Synopsis of the kidney disease: Improving global outcomes 2017 clinical practice guideline update: Ann Intern Med, 2018; 168; 422-30
3. Kłos K, Szczepańska S, Janas RMParathormone 1–84 and its antagonist parathormone 7–84 in circulation – what should we determine?: Stand Med Pediat, 2011; 8; 112-19 [in Polish]
4. Kokot F, Hyla-Klekot L, Optimal concentrations of plasma parathyroid hormone and vitamin D in patients with chronic renal diseases – why are they object of controversy: Nefrol Dial Pol, 2011; 15; 184-88
5. : National Kidney Foundation GFR calculator https://www.kidney.org/professionals/kdoqi/gfr_calculator
6. Nakanishi S, Kazama JJ, Shigematsu T, Comparison of intact PTH assay and whole PTH assay in long-term dialysis patients: Am J Kidney Dis, 2001; 38; 172-74
7. Marangella M, PTH measurement: Where do we stand?: G Ital Nefrol, 2009; 26; 600-7
8. Bekő G, Butz H, Berta K, Switching between parathormone (PTH) assays: the impact on the diagnosis of renal osteodystrophy: Clin Chem Lab Med, 2013; 51; 1251-6
9. Gannage-Yared MH, Fares C, Ibrahim T, Comparison between a second and third generation parathyroid hormone assays in hemodialysis patients: Metab Clin Exp, 2013; 62; 1416-22
10. Tan K, Ong L, Sethi SK, Comparison of the Elecsys (1–84) assay with four contemporary second generation intact PTH assays and association with other biomarkers in chronic kidney disease patients: Clin Biochem, 2013; 46; 781-86
11. Cantor T, Parathyroid hormone assay drift: An unappreciated problem in dialysis patient management: Semin Dial, 2005; 18; 359-64
12. Eddington H, Hudson JE, Oliver RL, Variability in parathyroid hormone assays confounds clinical practice in chronic kidney disease patients: Ann Clin Biochem, 2014; 51; 228-36
13. Kuczera P, Maszczyk A, Machura E, Serum parathyroid hormone concentrations measured by chemiluminescence and electrochemiluminescence methods – are the results comparable in hemodialysis patients with chronic kidney disease?: Endokrynol Pol, 2015; 66; 219-23
14. Taniguchi M, Tanaka M, Hamano T, Comparison between whole and intact parathyroid hormone assays: Ther Apher Dial, 2011; 15(Suppl 1); 42-49
15. Donati G, Cianciolo G, Capelli I, Comparison of two parathyroid hormone assays in hemodialysis patients: Artif Organs, 2016; 40; 1013-16
16. O’Flaherty D, Sankaralingam A, Scully P, The relationship between intact PTH and biointact PTH (1–84) with bone and mineral metabolism in pre-dialysis chronic kidney disease (CKD): Clin Biochem, 2013; 46; 1405-9
17. Fukagawa M, Yokoyama K, Koiwa F, Guidelines: Clinical practice guideline for the management of chronic kidney disease – mineral and bone disorders: Ther Apher Dial, 2013; 17; 247-88
18. Rodriguez-Osorio L, de la Piedra C, Rubert M: Nefrologia, 2017; 27; 389-96
19. Kurajoh M, Inaba M, Yamada S, Association of increased active PTH(1–84) fraction with decreased GFR and serum Ca in predialysis CRF patients: modulation by serum 25-OH-D: Osteoporos Int, 2008; 19; 709-16
20. Graf S, Bohner J, Hertel A, Comparison of total and whole PTH with direct markers of bone metabolism in haemodialysis patients: Nephrol Dial Transplant, 2003; 18(Suppl 4); 406
21. Einbinder Y, Benchetrit S, Golan E, Comparison of intact PTH and Bio-Intact PTH assays among non-dialysis dependent chronic kidney disease patients: Ann Lab Med, 2017; 37; 381-87
22. Patel S, Barron JL, Mirzazedeh M, Changes in bone mineral parameters, vitamin D metabolites, and PTH measurements with varying chronic kidney disease stages: J Bone Miner Metab, 2011; 29; 71-79
23. Cavalier E, Salsé M, Dupuy AM: Clin Biochem, 2018; 54; 119-22
24. Jabbar Z, Aggarwal PK, Chandel N, Noninvasive assessment of bone health in Indian patients with chronic kidney disease: Indian J Nephrol, 2013; 23; 161-67
25. Bunio A, Steciwko A, Mastalerz-Migas A, Markers of bone metabolism and its usefulness in assessment of bone turnover in hemodialysis patients in relation to PTH concentration: Nefrol Dial Pol, 2006; 10; 7-11
26. Sprague SM, Bellorin-Font E, Jorgetti V, Diagnostic accuracy of bone turnover markers and bone histology in patients with CKD treated by dialysis: Am J Kidney Dis, 2016; 67; 559-66
27. Davina J, Priyadarssini M, Rajappa M, Assessment of bone turnover markers to predict mineral and bone disorder in men with pre-dialysis non-diabetic chronic kidney disease: Clin Chim Acta, 2017; 469; 195-200
28. Khan SS, Iraniha MR, Diagnosis of renal osteodystrophy among chronic kidney disease patients: Dial Transplant, 2009; 38; 45-57
29. Chiang C, The use of bone turnover markers in chronic kidney disease-mineral and bone disorders: Nephrology (Carlton), 2017; 22(Suppl 2); 11-13
30. Delanaye P, Souberbielle JC, Lafage-Proust MH, Can we use circulating biomarkers to monitor bone turnover in CKD haemodialysis patients? Hypotheses and facts: Nephrol Dial Transplant, 2014; 29; 997-1004
31. Herberth J, Monier-Faugere M-C, Mawad HW, The five most commonly used intact parathyroid hormone assays are useful for screening but not for diagnosing bone turnover abnormalities in CKD-5 patients: Clin Nephrol, 2009; 72; 5-14
32. Cavalier E, Delanaye P, Lukas P, Standardization of DiaSorin and Roche automated third generation PTH assays with an international standard: Impact on clinical populations: Clin Chem Lab Med, 2014; 52; 1137-41
33. Jenabi A, Jabbari M, Ziaie H, Comparing the values of intact parathormone and 1–84 PTH to predict hyperparathyroidism in hemodialysis patients: J Nephropathol, 2017; 6; 248-53
34. Kakuta T, Ischida M, Fukagawa M, Clinical governance issue of parathyroid hormone assays and its selection in the management of chronic kidney disease mineral and bone disorders: Ther Apher Dial, 2018; 22; 220-28
35. Tanno Y, Yokoyama K, Nakayama M, IRMA (whole PTH) is a more useful assay for the effect of PTH on bone than Allegro Intact PTH assay in CAPD patients with low bone turnover marker: Nephrol Dial Transplant, 2003; 18(Suppl 3); iii97-98
36. Souberbielle JC, Roth H, Fouque DP, Parathyroid hormone measurement in CKD: Kidney Int, 2010; 77; 93-100
37. Przedlacki J, Serafińska B, Żebrowski P, Assessment of clinical utility of the whole parathyroid hormone assay (1–84 PTH) in patients with end-stage renal disease on maintenance dialysis: Diagn Lab, 2013; 49; 365-68
38. D’Amour P, Acute and chronic regulation of circulating PTH: Significance in health and in disease: Clin Biochem, 2012; 45; 964-69
39. Hocher B, Yin L, Why current PTH assays mislead clinical decision making in patients with secondary hyperparathyroidism: Nephron, 2017; 136; 137-42
40. Dupuy AM, Bargnoux AS, Morena M, Moving from the second to the third generation Roche PTH assays: What are the consequences for clinical practice?: Clin Chem Lab Med, 2018; 57; 244-49
41. Sturgeon CM, Sprague S, Almond A, Perspective and priorities for improvement of parathyroid hormone (PTH) measurement. A view from the IFCC Working Group for PTH: Clin Chim Acta, 2017; 467; 42-47
42. Hocher B, Zeng S, Need for better PTH assays for clinical research and patient treatment: Clin Chem Lab Med, 2018; 56; 183-85
43. Cavalier E, Parathyroid hormone results interpretation in the background of variable analytical performance: J Lab Precis Med, 2019; 4; 1-10
Figures
 Figure 1. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in patients with CKD stages 3 to 5D.
Figure 1. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in patients with CKD stages 3 to 5D. Figure 2. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in pre-dialysis patients.
Figure 2. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in pre-dialysis patients. Figure 3. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in dialyzed patients.
Figure 3. Linear regression between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in dialyzed patients. Figure 4. Comparison of second- and third-generation parathyroid hormone assays in patients with chronic kidney disease (n=205) (Bland-Altman method).
Figure 4. Comparison of second- and third-generation parathyroid hormone assays in patients with chronic kidney disease (n=205) (Bland-Altman method). Tables
 Table 1. Characteristics of the study group and the control group.
Table 1. Characteristics of the study group and the control group. Table 2. Intact parathyroid hormone, parathyroid hormone 1–84, and other laboratory parameters and age in various subgroups of patients with CKD and in the control group.
Table 2. Intact parathyroid hormone, parathyroid hormone 1–84, and other laboratory parameters and age in various subgroups of patients with CKD and in the control group. Table 3. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in different study groups (Spearman method).
Table 3. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in different study groups (Spearman method). Table 4. Formulas enabling comparison of parathyroid hormone concentration results determined with second- and third-generation tests*.
Table 4. Formulas enabling comparison of parathyroid hormone concentration results determined with second- and third-generation tests*. Table 5. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations and kidney function indices, calcium-phosphate metabolism parameters, and bone metabolism markers (Spearman method).
Table 5. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations and kidney function indices, calcium-phosphate metabolism parameters, and bone metabolism markers (Spearman method). Table 6. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with stages 3 to 5D CKD (n=205).
Table 6. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with stages 3 to 5D CKD (n=205). Table 7. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with CKD in the pre-dialysis period (n=78).
Table 7. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with CKD in the pre-dialysis period (n=78). Table 8. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in hemodialyzed patients (n=95).
Table 8. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in hemodialyzed patients (n=95). Table 9. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients on home peritoneal dialysis (n=32).
Table 9. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients on home peritoneal dialysis (n=32). Table 1. Characteristics of the study group and the control group.
Table 1. Characteristics of the study group and the control group. Table 2. Intact parathyroid hormone, parathyroid hormone 1–84, and other laboratory parameters and age in various subgroups of patients with CKD and in the control group.
Table 2. Intact parathyroid hormone, parathyroid hormone 1–84, and other laboratory parameters and age in various subgroups of patients with CKD and in the control group. Table 3. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in different study groups (Spearman method).
Table 3. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations in different study groups (Spearman method). Table 4. Formulas enabling comparison of parathyroid hormone concentration results determined with second- and third-generation tests*.
Table 4. Formulas enabling comparison of parathyroid hormone concentration results determined with second- and third-generation tests*. Table 5. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations and kidney function indices, calcium-phosphate metabolism parameters, and bone metabolism markers (Spearman method).
Table 5. Correlations between intact parathyroid hormone and parathyroid hormone 1–84 concentrations and kidney function indices, calcium-phosphate metabolism parameters, and bone metabolism markers (Spearman method). Table 6. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with stages 3 to 5D CKD (n=205).
Table 6. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with stages 3 to 5D CKD (n=205). Table 7. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with CKD in the pre-dialysis period (n=78).
Table 7. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients with CKD in the pre-dialysis period (n=78). Table 8. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in hemodialyzed patients (n=95).
Table 8. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in hemodialyzed patients (n=95). Table 9. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients on home peritoneal dialysis (n=32).
Table 9. Multiple regression analysis for correlates of intact parathyroid hormone and parathyroid hormone 1–84 in patients on home peritoneal dialysis (n=32). In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








