19 May 2022: Animal Study
Anti-Inflammatory and Anti-Oxidative Effects of Isorhamnetin for Protection Against Lung Injury in a Rat Model of Heatstroke in a Dry-Heat Environment
Xiang Dong1BDEF, Jia-Jia Li1BCDF, Na Ma1BC, Ai-Zhong Liu1DF, Jiang-Wei Liu1AEG*DOI: 10.12659/MSM.935426
Med Sci Monit 2022; 28:e935426
Abstract
BACKGROUND: Isorhamnetin is a natural flavonoid compound with anti-inflammatory and antioxidant properties. However, its roles in alleviating lung injury associated with heatstroke remain unclear. Therefore, this study aimed to evaluate the protective effects of different isorhamnetin doses on lung injury in heatstroke rat models exposed to a dry-heat environment.
MATERIAL AND METHODS: Fifty Sprague-Dawley rats were randomly divided into 5 groups: normal control (0.9% saline), heatstroke (0.5% CMCNa), and isorhamnetin (25, 50, and 100 mg/kg) groups; treatments were administered by gavage daily for 7 days. All rats, except those in the control group, were exposed to a dry-heat environment (41±1°C, 10±2% relative humidity) for 150 min to induce heatstroke. Pathological changes, ultrastructure, edema, inflammation, and oxidative stress in the lungs were assessed.
RESULTS: Compared with the heatstroke group, rats treated with 100 mg/kg isorhamnetin showed amelioration of histopathological and ultrastructural changes in the lungs; decreased lung injury scores (P<0.05) and wet/dry weight ratios (P<0.01); lower levels of phospho-nuclear factor-κB (P<0.05), high-mobility group box 1 (P<0.01), tumor necrosis factor-α (P<0.01), interleukin (IL)-1β (P<0.01), and IL-6 (P<0.01); lower malondialdehyde contents (P<0.01); and higher superoxide dismutase (P<0.01) and catalase activities (P<0.05).
CONCLUSIONS: In a dry-heat environment, isorhamnetin protected against lung injury in heatstroke rat models via anti-inflammatory and anti-oxidative mechanisms.
Keywords: 3-methylquercetin, acute lung injury, Heat Stroke, Inflammation, Oxidative Stress, Animals, Anti-Inflammatory Agents, Antioxidants, Hot Temperature, Lung, Lung Injury, Quercetin, Rats, Rats, Sprague-Dawley, Tumor Necrosis Factor-alpha
Background
Heatstroke is a severe life-threatening condition. Its pathophysiological characteristics are severe hyperthermia (>40°C) and systemic inflammatory response, which can lead to multiple organ dysfunction and even death [1]. The 28-day and 2-year mortality rates can be as high as 58% and 71%, respectively [1,2]. Acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) are the most common complications of heatstroke [3]. Moreover, 85.7% of patients experiencing heatstroke with organ failure exhibit respiratory failure [4], which severely affects survival rates and prognoses. Excessive heat exposure and subsequent exposure to harmful substances, such as pro-inflammatory mediators, can increase pulmonary microvascular and epithelial permeability [5], resulting in the accumulation of large amounts of fluid and proteins in the interstitium and alveolar spaces. The process of abnormal pulmonary edema fluid accumulation impairs alveolar gas exchange, which is an important cause of ALI and respiratory failure related to heatstroke [6,7].
With the persistence of global warming and the surge of extreme weather events, more people may face the challenge of heat-related illnesses and deaths [8,9]. Past studies have mostly been conducted in humid-heat environments, but, contrary to popular expectations, there is limited evidence of a positive correlation between high humidity and mortality [10]. However, exposure to a dry-heat environment increases the risk of heatstroke under the influence of dehydration and other adverse factors [11]. Therefore, viable methods for preventing and treating heatstroke combined with lung injury are urgently needed. Existing management is more oriented toward rapid cooling and symptomatic support of patients, and there is no standardized, systematic treatment for heatstroke [12]. Moreover, several potential therapeutic approaches such as xanthine oxidase inhibitors and recombinant active protein C are in the stage of animal testing and preliminary clinical studies [13].
Isorhamnetin (3,5,7-trihydroxy-2-[4-hydroxy-3-methoxy-phenyl] chromium-4-one) is a natural methylated flavonoid with a wide range of pharmacological effects and superior absorption and metabolic stability compared to the much-studied quercetin [14]. Isorhamnetin was reported to attenuate acute lung injury caused by lipopolysaccharide inhalation in mice and was associated with the regulation of MAPKs and NF-KB signaling pathways and inhibition of pro-inflammatory factors [15]. Isorhamnetin also attenuated bleomycin-induced pulmonary fibrosis in mice by inhibiting endoplasmic reticulum stress and epithelial-mesenchymal transition [16]. In addition, isorhamnetin has antioxidant effects, blocking early intracellular signal cascades by inhibiting reactive oxygen species (ROS) accumulation [17]. Therefore, we speculate that isorhamnetin may be a potential drug for the prevention and treatment of lung injury caused by heatstroke. In this study, we pretreated heatstroke rat models with isorhamnetin in a dry-heat environment. The anti-inflammatory and antioxidant effects of isorhamnetin were detected to further evaluate the applications of this drug in the prevention of heatstroke-related lung injury.
Material and Methods
EXPERIMENTAL ANIMALS AND ETHICAL CONSIDERATIONS:
Male Sprague-Dawley rats (n=50; age: 8–10 weeks; body weight: 230–250 g) were purchased from the Animal Experiment Center of Xinjiang Medical University (Production Certificate, SCXK [Xin] 2016-0003). These specific pathogen-free animals were housed in a controlled standard laboratory environment (ambient temperature, 22±1°C; relative humidity, 50±5%), fed unlimited water and food, and exposed to a 12/12-h light/dark cycle. All animal experiments were approved by the Ethics Committee of Xinjiang Military Command General Hospital (approval number: DWLL2019004). Animal care and experiments were conducted according to the National Science Council guidelines and the World Medical Association Declaration of Helsinki.
EXPERIMENTAL DESIGN:
The animals were randomly divided into 5 groups (n=10/group): normal control (NC) group, heatstroke (HS) group, low-dose isorhamnetin (L-AS) group, medium-dose isorhamnetin (M-AS) group, and high-dose isorhamnetin (H-AS) group. Isorhamnetin (Shanghai Macklin Biochemical Ltd; Shanghai, China) was dissolved in a 0.5% sodium carboxymethyl cellulose (CMCNa) solution as a vehicle. Rats in the NC, HS, and isorhamnetin groups were intragastrically administered 0.9% saline, 0.5% CMCNa, or specific doses of isorhamnetin (25, 50, and 100 mg/kg), respectively, once a day for 7 days. On the second day after gavage, rats from all groups except the NC group were placed in an experimental cabin (Simulated Climate Cabin for Special Environment of Northwest of China, Urumqi), which imitated a dry-heat environment (42.2±1°C, 10±5% relative humidity). During heat exposure, fasting and water deprivation were enforced. After 150 min, the core body temperature of the HS group reached above 40.5°C, and the dry-heat heatstroke rat model was successfully established. The process of model creation replicated our previous study [11]. All rats were subsequently anesthetized with 3% pentobarbital sodium and killed. Lung tissues were preserved for subsequent experiments.
LUNG MORPHOLOGY:
Lung tissues were fixed with 10% polyformaldehyde for 24 h, and paraffin-embedded lung tissues were cut into 3-μm-thick sections. The sections were stained with hematoxylin and eosin for histological examination. Morphological evaluation was performed using optical microscopy as previously reported [18], and 4 items – neutrophil clearing, hemorrhage, alveolar septal thickening, and tracheal epithelial cell injury – were evaluated. The degree of damage was expressed on a scale of 0–4 points: 0, normal; 1, slight damage; 2, mild damage; 3, moderate damage; and 4, severe damage. Each photograph was analyzed by a blinded observer in at least 10 fields of view, and then the scores for each item were summarized to obtain an overall lung injury score.
LUNG WET/DRY WEIGHT RATIOS:
The surface of the lung tissue was washed with saline. The wet weight was determined immediately using a precise balance after the water was absorbed by filter paper. The lung tissues were then dried in an oven at 80°C for 48 h to determine the dry weight. Finally, the wet/dry weight ratio was calculated as an indicator of lung edema [19].
CHANGES IN LUNG ULTRASTRUCTURE:
Lung tissue (1–2 mm3) was immersed in 2.5% glutaraldehyde at 4°C overnight, washed 3 times in 0.1 M phosphate buffer, and fixed with 1% osmium tetroxide for 2 h. After dehydration, replacement, and infiltration, the tissue was embedded with epoxy resin. The ultrastructure of alveolar epithelial type II cells was observed by transmission electron microscopy with uranyl acetate and lead citrate double staining.
WESTERN BLOTTING:
Lung tissues were ground in liquid nitrogen, and total proteins were extracted in lysis buffer. The total protein concentration was determined using bicinchoninic acid assays (Thermo Fisher Scientific, Waltham, MA, USA). Equal amounts of proteins were mixed with 2×loading buffer and then boiled for 10 min. Protein samples were separated using sodium dodecyl sulfate-polyacrylamide gel electrophoresis on 10% gels and transferred to polyvinylidene difluoride membranes. The membranes were blocked with 5% nonfat dried milk for 2 h at 20±2°C before incubation with the primary antibody at 4°C overnight. The membranes were then incubated with horseradish peroxidase-coupled secondary antibodies for 2 h at 20±2°C. The target bands were visualized using an enhanced chemiluminescence kit and a ChemiDoc-It 510 Imager (Ultra-Violet Products Ltd., Cambridge, UK), and the data were then quantitatively analyzed based on the intensity of protein bands. The antibodies used in this study were as follows: anti-phospho-nuclear factor (NF)-κB (1: 1000; Cell Signaling Technology, Danvers, MA, USA), anti-NF-κB (1: 1000; Cell Signaling Technology), anti-high-mobility group box 1 (HMGB1; 1: 1000; Abcam, Cambridge, UK), anti-β-actin (1: 2000; Abcam), goat anti-rabbit IgG (1: 5000; Abcam), and goat anti-mouse IgG (1: 5000; Abcam).
INFLAMMATORY FACTORS AND OXIDATIVE STRESS INDEX:
The concentrations of tumor necrosis factor (TNF)-α, interleukin (IL)-1β, and IL-6 in lung tissues were measured using an antibody-sandwich enzyme-linked immunosorbent assay with commercial kits from Anhui Qiaoyi Biotechnology (Anhui, China). The activities of superoxide dismutase (SOD) and catalase (CAT) were evaluated in lung tissues using the xanthine oxidase method, and spectrophotometry was performed using commercial kits from Nanjing Jiancheng Bioengineering Institute (Nanjing, China). Malondialdehyde (MDA) content in lung tissues was measured using the thiobarbituric acid method with commercial kits (Nanjing, China). All procedures were performed in accordance with the manufacturers’ instructions.
STATISTICAL ANALYSIS:
SPSS 25.0 statistical software (SPSS, Inc., Chicago, IL, USA) was used for the analysis. The data for each experimental group (showing a normal distribution) were analyzed using a one-way analysis of variance. Data are expressed as means ± standard deviations, and results with
Results
PRETREATMENT WITH ISORHAMNETIN ALLEVIATED PATHOLOGICAL INJURY AND LUNG EDEMA:
Alveolar structures were intact without pathological changes in the NC group. In the HS group, partial lung consolidation, thickened alveolar septum, collapsed alveoli, and compensated alveoli were observed. Additionally, neutrophil infiltration, capillary congestion, and bleeding were observed in the interstitium. Some epithelial cells in the bronchus showed condensed nuclei, along with degeneration, necrosis, and shedding. Pathological changes in the lung were alleviated in the isorhamnetin groups. In particular, lung injury in the H-AS group showed partial alveolar fullness and few compensatory alveoli. The interstitial capillaries were slightly congested without neutrophil infiltration (Figure 1A). The injury scores and wet/dry weight ratios of the lungs in the HS group were higher than those in the NC group. Compared with those in the HS group, injury scores and wet/dry weight ratios in the H-AS group were lower (P<0.05, P<0.01; Figure 1B, 1C).
PRETREATMENT WITH ISORHAMNETIN ATTENUATED CHANGES IN LUNG ULTRASTRUCTURE:
The results of transmission electron microscopy demonstrated the presence of normal alveolar epithelial type II cells in the NC group. The nuclear structure was abnormal, the mitochondria were very swollen and showed a vacuole-like structure, and lamellar bodies and microvilli were absent in alveolar epithelial type II cells from the HS group. In the M-AS and H-AS groups, the marked mitochondrial swelling and lamellar body vacuolation observed in the HS group were decreased (Figure 2).
PRETREATMENT WITH ISORHAMNETIN REDUCED PHOSPHO-NF-κB AND HMGB1 LEVELS IN LUNG TISSUES:
Phospho-NF-κB and HMGB1 levels were significantly higher in the HS group than in the NC group (P<0.01; Figure 3). Moreover, the expression of phospho-NF-κB and HMGB1 was significantly lower in the M-AS and H-AS groups than in the HS group (P<0.01). Thus, pretreatment with isorhamnetin reduced phospho-NF-κB and HMGB1 levels in the dry-heat environment.
PRETREATMENT WITH ISORHAMNETIN DECREASED INFLAMMATORY FACTORS IN LUNG TISSUES:
Next, we analyzed the levels of inflammatory factors to further evaluate the anti-inflammatory effects of isorhamnetin. TNF-α, IL-1β, and IL-6 levels were significantly higher in the HS group than in the NC group (P<0.01; Figure 4). The levels of TNF-α, IL-1β, and IL-6 were lower in the M-AS and H-AS groups than in the HS group (P<0.05, P<0.01); this effect was dose-dependent.
PRETREATMENT WITH ISORHAMNETIN RESTORED SOD AND CAT ACTIVITIES BUT SUPPRESSED MDA CONTENTS IN LUNG TISSUES:
Compared with those in the NC group, the activities of SOD and CAT in the HS group were significantly lower (P<0.01), whereas MDA content significantly increased (P<0.01; Figure 5). However, pretreatment with isorhamnetin (M-AS or H-AS group) significantly suppressed MDA content (P<0.01) and restored SOD and CAT activities (P<0.05 and P<0.01, respectively).
Discussion
As the most important organ for heat dissipation and oxygen exchange, the lungs are composed of alveoli surrounded by numerous capillary networks. The physiological response to heat stress causes skin vasodilation, sweating, and increased respiratory rate, consequently inducing visceral blood flow to the skin to dissipate heat. These factors increase the burden on blood circulation and lung function [5,20]. The lungs are one of the first organs to be affected and damaged during heatstroke. A low-level core temperature (39°C) can cause significant pathological changes in the lungs [21]. Impairment of lung function can further induce and promote the anoxic injury of other vital organs [22]. In this study, we established a heatstroke rat model by exposure to a dry-heat environment. Histopathological and ultrastructural changes in the lungs in heatstroke rats were observed. Moreover, an increase in the lung wet/dry weight ratio, an important indicator of lung water content, supported the pathological injury. However, pretreatment with isorhamnetin reduced heatstroke-induced lung injury in a dose-dependent manner.
A recent study showed that the heatstroke reaction was similar to septic shock caused by endotoxins [23]. Excessive exercise and heat stress lead to endotoxemia by damaging intestinal barrier integrity, thus activating heatstroke pathophysiological development [24]. Lipopolysaccharide (LPS) is a common endotoxin that can be recognized by the transmembrane receptor Toll-like receptor 4 (TLR4), which mediates the inflammatory signaling pathway and activates downstream NF-κB, thereby triggering the transcription of inflammatory cytokines such as TNF-α, IL-1β, and IL-6 [25]. Inflammatory cytokines can damage the alveolar-capillary barrier, which induces lung tissue injury and neutrophil aggregation and aggravates the obstruction of alveolar cell perfusion and oxygen exchange, resulting in ALI and pulmonary edema [26]. Various experimental murine models and human genetic studies have shown that inhibiting NF-κB overexpression plays a key role in preventing uncontrolled inflammation and developing inflammation-related diseases [27,28]. Similarly, HMGB1 plays multiple roles in the regulation of inflammatory responses and cellular and tissue stress responses. When HMGB1 is released into the extracellular space through active or passive mechanisms and transmits damage signals to adjacent cells, it can activate the inflammatory response, leading to injury and necrosis [29,30]. HMGB1 is a marker and advanced inflammatory factor of endotoxemia; however, increased HMGB1 levels in tissues and blood circulation have been observed in the early stages of heatstroke in animal models [31]. HMGB1 can bind to the receptors TLR2 and TLR4 and act as a receptor for advanced glycation end-products to activate various inflammation-related signaling pathways, such as the NF-κB pathway, thereby promoting the expression of inflammatory factors in the context of pulmonary dysfunction [32]. In particular, elevated HMGB1 levels are accompanied by upregulation of their specific receptor RAGE, and activation of RAGE induced a positive feedback mechanism, which further promotes HMGB1 expression [33]. In germ-free and infectious inflammation animal models, the removal or neutralization of HMGB1 can significantly inhibit the activation of innate immune responses and reduce tissue damage [34]. Our experimental results showed that pretreatment with isorhamnetin in each group reduced the protein levels of phospho-NF-κB and HMGB1 and the expression of TNF-α, IL-1β, and IL-6 to varying degrees. Decreases in these inflammatory indicators may explain why pretreatment with isorhamnetin inhibits lung injury in heatstroke model rats exposed to a dry-heat environment.
In addition to inflammatory damage, excessive levels of ROS produced by damaged endothelial/epithelial cells and recruited leukocytes is an important factor that affects lung injury and ARDS progression [35]. Importantly, heat stress can induce oxidative stress [36]. Recently, high-throughput sequencing technology identified gene expression profiles in the lung tissues of heatstroke model rats. In total, 471 differentially expressed genes (257 upregulated genes and 214 downregulated genes) were identified, most of which were found to be closely related to inflammation and oxidative stress [22]. Our experimental results showed that pretreatment with isorhamnetin could increase the activities of SOD and CAT in the lung tissues of heatstroke model rats and reduce the levels of the lipid peroxidation product MDA. The enzymatic antioxidants SOD and CAT can exert more powerful protective effects against active and massive oxidative attacks compared to other antioxidants. When exposed to oxidative stress, SOD appears to be the first line of defense against oxygen free radicals. SOD can be rapidly induced under certain conditions, catalyzing superoxide to hydrogen peroxide (H2O2). H2O2 can then be neutralized by CAT and decomposed into H2O and oxygen [37]. Studies have reported that the mechanism of pulmonary fibrosis damage caused by paraquat poisoning is related to oxidative stress. Vitamin C, an effective antioxidant, mitigates pulmonary fibrosis by increasing the activity of SOD and CAT [38]. In addition,
Conclusions
In conclusion, pretreatment with isorhamnetin, particularly when the gavage dose reaches 100 mg/kg, could inhibit pathological damage and edema of lung tissue by regulating NF-κB and HMGB1 protein expression, downstream pro-inflammatory factors, and oxidative stress. Since there is currently no specific drug for the treatment of heatstroke, only symptomatic treatment is provided. Therefore, by comparing the anti-inflammatory and antioxidant capacities of different concentrations of isorhamnetin, we concluded that it is a potential drug for the prevention and treatment of lung injury in heatstroke rats. Additional in vivo and in vitro experiments are needed to elucidate the exact molecular mechanisms and toxic effects of isorhamnetin that may occur following long-term administration.
Figures
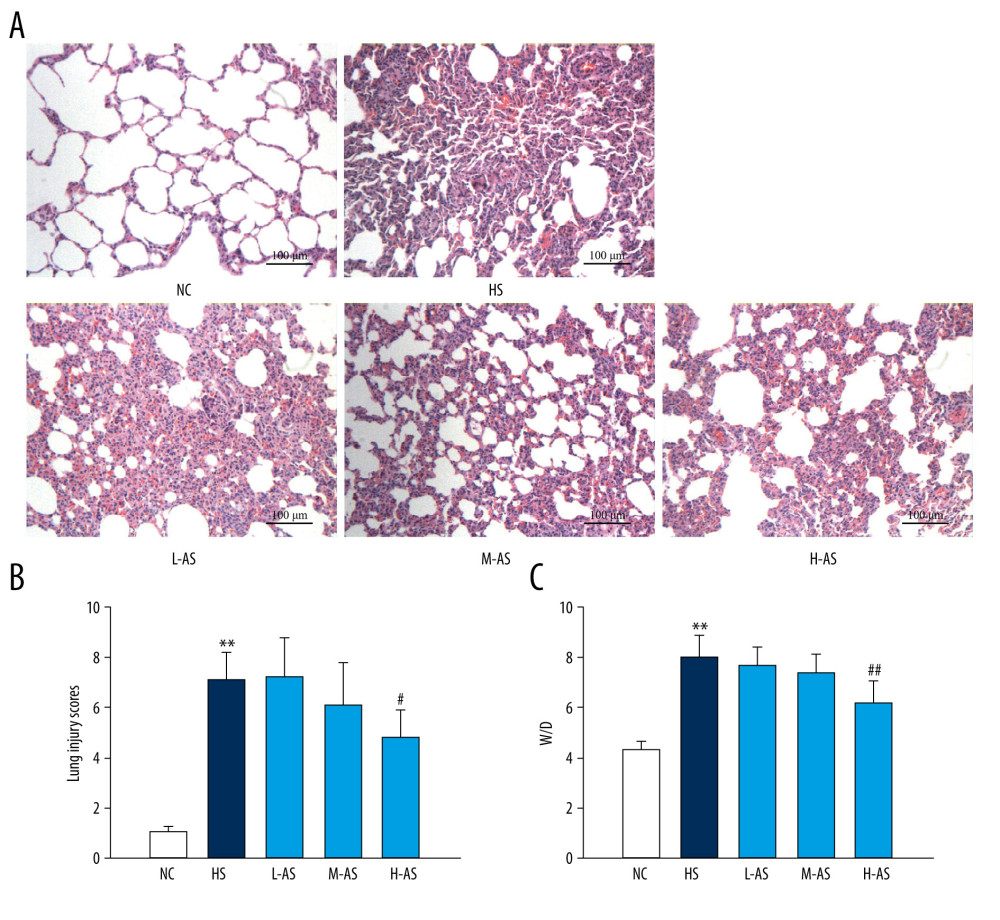 Figure 1. Pathological changes and edema of the lungs in a heatstroke rat model pretreated with isorhamnetin. (A) Pulmonary pathological changes, (B) lung injury scores, (C) lung wet/dry weight ratios. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS– low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation.
Figure 1. Pathological changes and edema of the lungs in a heatstroke rat model pretreated with isorhamnetin. (A) Pulmonary pathological changes, (B) lung injury scores, (C) lung wet/dry weight ratios. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS– low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation. 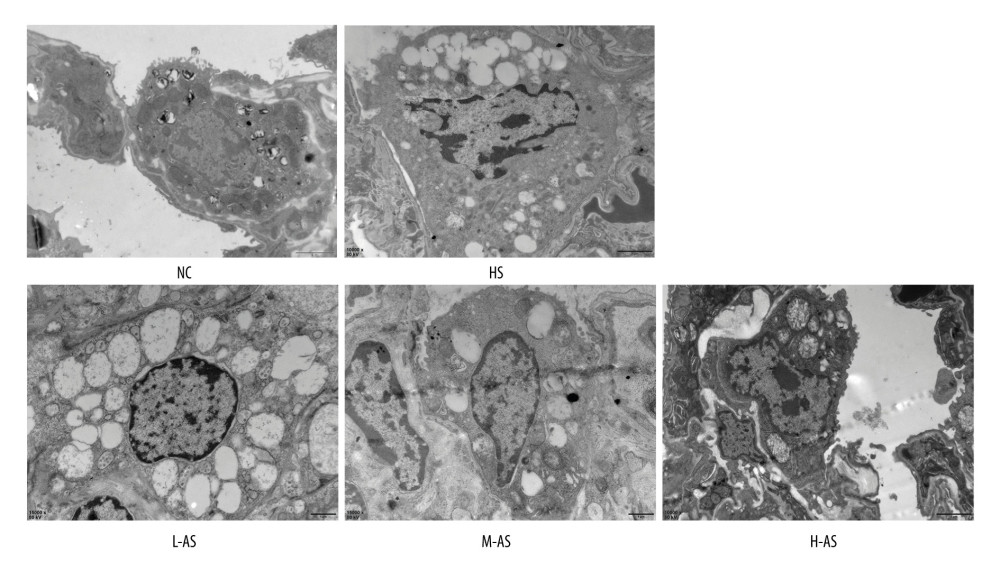 Figure 2. Changes in lung ultrastructure in a heatstroke rat model pretreated with isorhamnetin. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin.
Figure 2. Changes in lung ultrastructure in a heatstroke rat model pretreated with isorhamnetin. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. 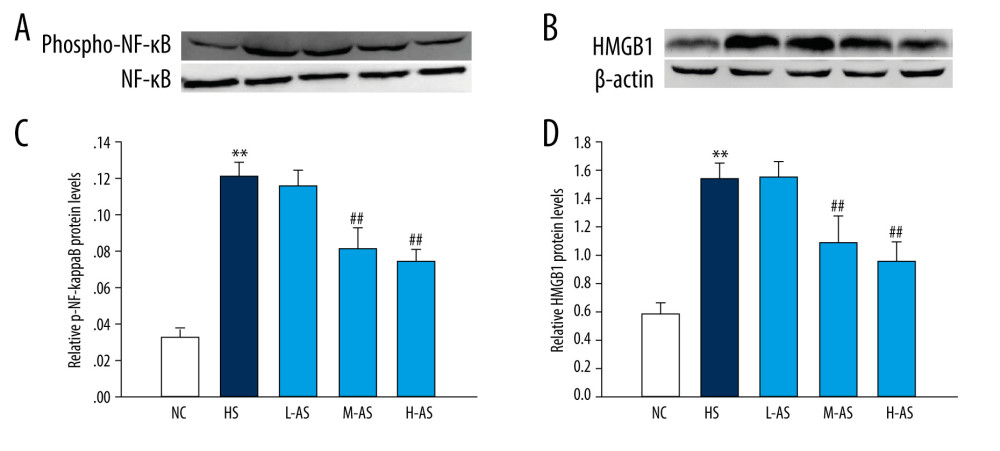 Figure 3. Phospho-NF-κB and HMGB1 levels in the lungs of a heatstroke rat model pretreated with isorhamnetin. Levels of phospho-NF-κB (A, C) and HMGB1 (B, D) proteins, as detected by western blotting. Date represent the mean±SD, (n=5/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. VisionWorksLS 8.1.2 (UVP, LLC.) and SigmaPlot 12.5 (Systat Software, Inc.) were used for figure creation.
Figure 3. Phospho-NF-κB and HMGB1 levels in the lungs of a heatstroke rat model pretreated with isorhamnetin. Levels of phospho-NF-κB (A, C) and HMGB1 (B, D) proteins, as detected by western blotting. Date represent the mean±SD, (n=5/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. VisionWorksLS 8.1.2 (UVP, LLC.) and SigmaPlot 12.5 (Systat Software, Inc.) were used for figure creation. 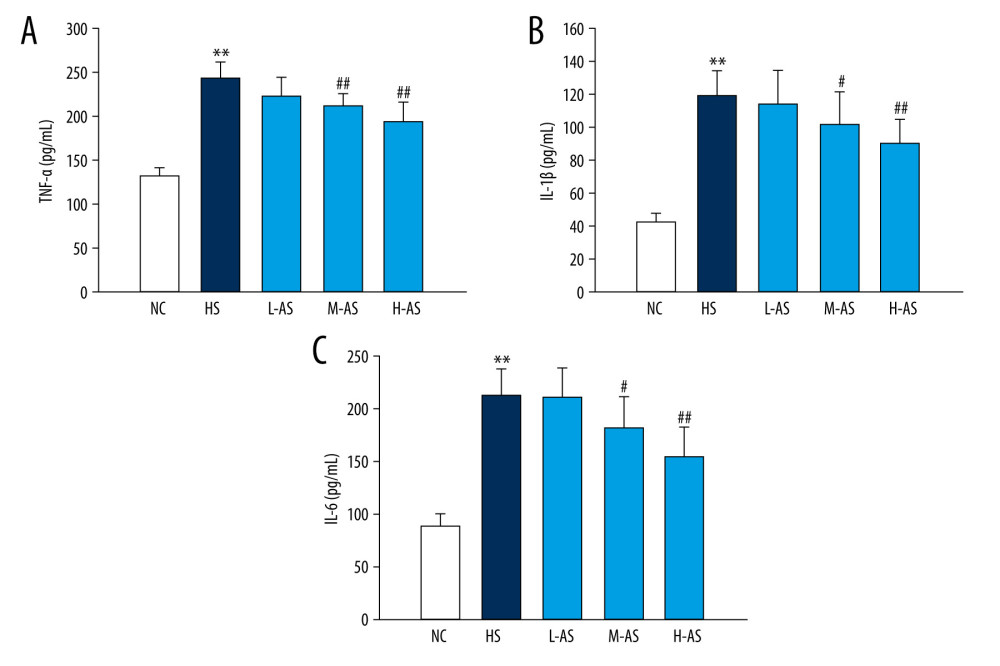 Figure 4. Pulmonary inflammatory factors in a heatstroke rat model pretreated with isorhamnetin. (A) TNF-α, (B) IL-1β, (C) IL-6. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation.
Figure 4. Pulmonary inflammatory factors in a heatstroke rat model pretreated with isorhamnetin. (A) TNF-α, (B) IL-1β, (C) IL-6. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation. 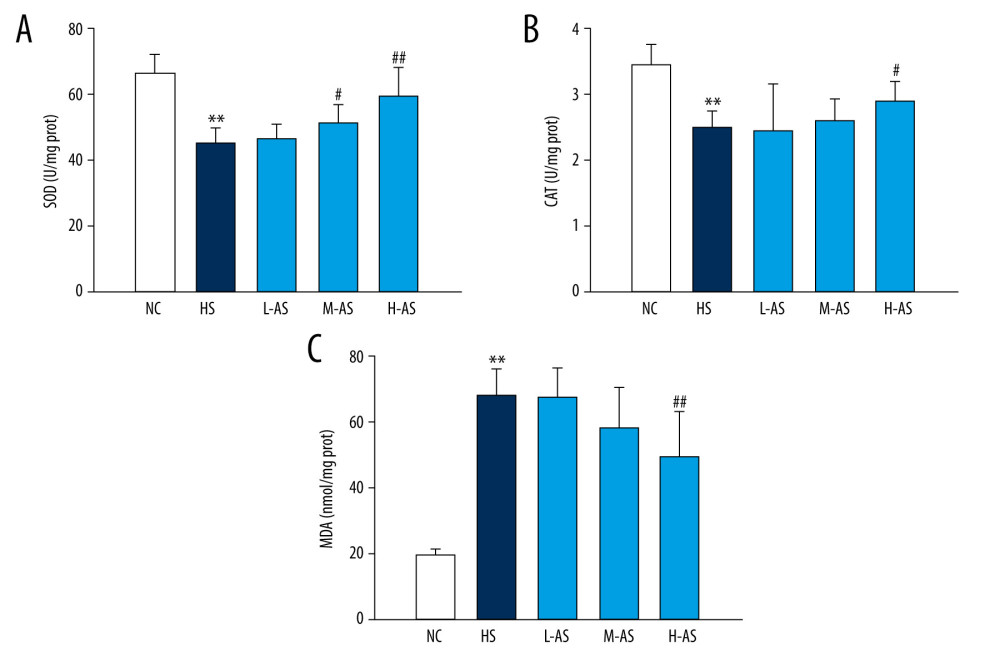 Figure 5. Pulmonary oxidative stress index in a heatstroke rat model pretreated with isorhamnetin. Levels of (A) SOD, (B) CAT, and (C) MDA in lung tissues. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation.
Figure 5. Pulmonary oxidative stress index in a heatstroke rat model pretreated with isorhamnetin. Levels of (A) SOD, (B) CAT, and (C) MDA in lung tissues. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation. References
1. Hifumi T, Kondo Y, Shimizu K, Miyake Y, Heat stroke: J Intensive Care, 2018; 6; 30
2. Nzvere FP, Tariq E, Nishanth K, Long-term cardiovascular diseases of heatstroke: A delayed pathophysiology outcome: Cureus, 2020; 12; e9595
3. Xu Q, Liu J, Wang Z, Heat stress-induced disruption of endothelial barrier function is via PAR1 signaling and suppressed by Xuebijing injection: PLoS One, 2015; 10; e0118057
4. Varghese GM, John G, Thomas K, Predictors of multi-organ dysfunction in heatstroke: Emerg Med J, 2005; 22; 185-87
5. Scheraga RG, Thompson C, Tulapurkar ME, Activation of heat shock response augments fibroblast growth factor-1 expression in wounded lung epithelium: Am J Physiol Lung Cell Mol Physiol, 2016; 311; L941-45
6. Zhou G, Chen Z, Li J, Role of the receptor for advanced glycation end products in heat stress-induced endothelial hyperpermeability in acute lung injury: Front Physiol, 2020; 11; 1087
7. Huppert LA, Matthay MA, Ware LB, Pathogenesis of acute respiratory distress syndrome: Semin Respir Crit Care Med, 2019; 40; 31-39
8. Wang Y, Bobb JF, Papi B, Heat stroke admissions during heat waves in 1916 US counties for the period from 1999 to 2010 and their effect modifiers: Environ Health, 2016; 15; 83
9. Alizadeh MR, Adamowski J, Nikoo MR, A century of observations reveals increasing likelihood of continental-scale compound dry-hot extremes: Sci Adv, 2020; 6; eaaz4571
10. Armstrong B, Sera F, Vicedo-Cabrera AM, The role of humidity in associations of high temperature with mortality: A multicountry, multicity study: Environ Health Perspect, 2019; 127; 97007
11. Zhao YH, Shen CF, Wang GJ, Curcumin alleviates acute kidney injury in a dry-heat environment by reducing oxidative stress and inflammation in a rat model: J Biochem Mol Toxicol, 2021; 35; e22630
12. Rublee C, Dresser C, Giudice C, Evidence-based heatstroke management in the Emergency Department: West J Emerg Med, 2021; 22; 186-95
13. Epstein Y, Yanovich R, Heatstroke: N Engl J Med, 2019; 380; 2449-59
14. Ganbold M, Owada Y, Ozawa Y, Isorhamnetin alleviates steatosis and fibrosis in mice with nonalcoholic steatohepatitis: Sci Rep, 2019; 9; 16210
15. Chi G, Zhong W, Liu Y, Isorhamnetin protects mice from lipopolysaccharide-induced acute lung injury via the inhibition of inflammatory responses: Inflamm Res, 2016; 65; 33-41
16. Zheng Q, Tong M, Ou B, Isorhamnetin protects against bleomycin-induced pulmonary fibrosis by inhibiting endoplasmic reticulum stress and epithelial-mesenchymal transition: Int J Mol Med, 2019; 43; 117-26
17. Kim SY, Jin CY, Kim CH, Isorhamnetin alleviates lipopolysaccharide-induced inflammatory responses in BV2 microglia by inactivating NF-κB, blocking the TLR4 pathway and reducing ROS generation: Int J Mol Med, 2019; 43; 682-92
18. Mikawa K, Nishina K, Takao Y, Obara H, ONO-1714, a nitric oxide synthase inhibitor, attenuates endotoxin-induced acute lung injury in rabbits: Anesth Analg, 2003; 97; 1751-55
19. Wu X, Kong Q, Zhan L, TIPE2 ameliorates lipopolysaccharide-induced apoptosis and inflammation in acute lung injury: Inflamm Res, 2019; 68; 981-92
20. Schlader ZJ, Wilson TE, Crandall CG, Mechanisms of orthostatic intolerance during heat stress: Auton Neurosci, 2016; 196; 37-46
21. Liu ZF, Li BL, Tong HS, Pathological changes in the lung and brain of mice during heat stress and cooling treatment: World J Emerg Med, 2011; 2; 50-53
22. Liu Z, Chen J, Hu L, Expression profiles of genes associated with inflammatory responses and oxidative stress in lung after heat stroke: Biosci Rep, 2020; 40; BSR20192048
23. Lin CH, Tsai CC, Chen TH, Oxytocin maintains lung histological and functional integrity to confer protection in heat stroke: Sci Rep, 2019; 9; 18390
24. Lim CL, Heat sepsis precedes heat toxicity in the pathophysiology of heat stroke – a new paradigm on an ancient disease: Antioxidants (Basel), 2018; 7; 149
25. Li X, Jamal M, Guo P, Irisin alleviates pulmonary epithelial barrier dysfunction in sepsis-induced acute lung injury via activation of AMPK/SIRT1 pathways: Biomed Pharmacother, 2019; 118; 109363
26. Cheng K, Yang A, Hu X, Curcumin attenuates pulmonary inflammation in lipopolysaccharide induced acute lung injury in neonatal rat model by activating peroxisome proliferator-activated receptor γ (PPARγ) pathway: Med Sci Monit, 2018; 24; 1178-84
27. Rahman A, Fazal F, Blocking NF-κkB: An inflammatory issue: Proc Am Thorac Soc, 2011; 8; 497-503
28. Bartuzi P, Hofker MH, van de Sluis B, Tuning NF-κB activity: A touch of COMMD proteins: Biochim Biophys Acta, 2013; 1832; 2315-21
29. Deng M, Scott MJ, Fan J, Billiar TR, Location is the key to function: HMGB1 in sepsis and trauma-induced inflammation: J Leukoc Biol, 2019; 106; 161-69
30. Tang J, Deng P, Jiang Y, Role of HMGB1 in propofol protection of rat intestinal epithelial cells injured by heat shock: Cell Biol Int, 2013; 37; 262-66
31. Todani M, Fujita M, Tsuruta R, Moderate hypothermia suppressed excessive generation of superoxide anion radical and inflammatory reactions in blood and liver in heatstroke: Laboratory study in rats: Free Radic Res, 2010; 44; 462-72
32. Liu X, Xu Q, Mei L, Paeonol attenuates acute lung injury by inhibiting HMGB1 in lipopolysaccharide-induced shock rats: Int Immunopharmacol, 2018; 61; 169-77
33. Qu L, Chen C, Chen Y, High-mobility group box 1 (HMGB1) and autophagy in acute lung injury (ALI): A review: Med Sci Monit, 2019; 25; 1828-37
34. Andersson U, Tracey KJ, HMGB1 is a therapeutic target for sterile inflammation and infection: Annu Rev Immunol, 2011; 29; 139-62
35. Kellner M, Noonepalle S, Lu Q, ROS signaling in the pathogenesis of acute lung injury (ALI) and acute respiratory distress syndrome (ARDS): Adv Exp Med Biol, 2017; 967; 105-37
36. Akbarian A, Michiels J, Degroote J, Association between heat stress and oxidative stress in poultry; Mitochondrial dysfunction and dietary interventions with phytochemicals: J Anim Sci Biotechnol, 2016; 7; 37
37. He L, He T, Farrar S, Antioxidants maintain cellular redox homeostasis by elimination of reactive oxygen species: Cell Physiol Biochem, 2017; 44; 532-53
38. Rodrigues da Silva M, Schapochnik A, Peres Leal M, Beneficial effects of ascorbic acid to treat lung fibrosis induced by paraquat: PLoS One, 2018; 13; e0205535
39. Zaki SM, Evaluation of antioxidant and anti-lipid peroxidation potentials of Nigella sativa and onion extract on nicotine-induced lung damage: Folia Morphol (Warsz), 2019; 78; 554-63
Figures
 Figure 1. Pathological changes and edema of the lungs in a heatstroke rat model pretreated with isorhamnetin. (A) Pulmonary pathological changes, (B) lung injury scores, (C) lung wet/dry weight ratios. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS– low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation.
Figure 1. Pathological changes and edema of the lungs in a heatstroke rat model pretreated with isorhamnetin. (A) Pulmonary pathological changes, (B) lung injury scores, (C) lung wet/dry weight ratios. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS– low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation. Figure 2. Changes in lung ultrastructure in a heatstroke rat model pretreated with isorhamnetin. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin.
Figure 2. Changes in lung ultrastructure in a heatstroke rat model pretreated with isorhamnetin. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. Figure 3. Phospho-NF-κB and HMGB1 levels in the lungs of a heatstroke rat model pretreated with isorhamnetin. Levels of phospho-NF-κB (A, C) and HMGB1 (B, D) proteins, as detected by western blotting. Date represent the mean±SD, (n=5/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. VisionWorksLS 8.1.2 (UVP, LLC.) and SigmaPlot 12.5 (Systat Software, Inc.) were used for figure creation.
Figure 3. Phospho-NF-κB and HMGB1 levels in the lungs of a heatstroke rat model pretreated with isorhamnetin. Levels of phospho-NF-κB (A, C) and HMGB1 (B, D) proteins, as detected by western blotting. Date represent the mean±SD, (n=5/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. VisionWorksLS 8.1.2 (UVP, LLC.) and SigmaPlot 12.5 (Systat Software, Inc.) were used for figure creation. Figure 4. Pulmonary inflammatory factors in a heatstroke rat model pretreated with isorhamnetin. (A) TNF-α, (B) IL-1β, (C) IL-6. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation.
Figure 4. Pulmonary inflammatory factors in a heatstroke rat model pretreated with isorhamnetin. (A) TNF-α, (B) IL-1β, (C) IL-6. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group; # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation. Figure 5. Pulmonary oxidative stress index in a heatstroke rat model pretreated with isorhamnetin. Levels of (A) SOD, (B) CAT, and (C) MDA in lung tissues. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation.
Figure 5. Pulmonary oxidative stress index in a heatstroke rat model pretreated with isorhamnetin. Levels of (A) SOD, (B) CAT, and (C) MDA in lung tissues. Date represent the mean±SD, (n=10/group). ** P<0.01 compared with the NC group, # P<0.05 and ## P<0.01 compared with the HS group. NC – normal control; HS – heatstroke; L-AS – low-dose isorhamnetin; M-AS – medium-dose isorhamnetin; H-AS – high-dose isorhamnetin. SigmaPlot 12.5 (Systat Software, Inc.) was used for figure creation. In Press
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
06 Mar 2024 : Clinical Research
Prevalence and Variation of Medical Comorbidities in Oral Surgery Patients: A Retrospective Study at Jazan ...Med Sci Monit In Press; DOI: 10.12659/MSM.943884
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








