19 July 2021: Clinical Research
Comparison Between the Modified External Fixation and Calcaneal Traction in Ruedi-Allgower Type II/III Pilon Fractures
Wen Shu1ACE*, Xiaodong Hu1BC, Xiaofan Yang1BCFDOI: 10.12659/MSM.933385
Med Sci Monit 2021; 27:e933385
Abstract
BACKGROUND: To compare the effect of modified external fixation and calcaneal traction in a staged management of Ruedi-Allgower type II/III tibial pilon fractures.
MATERIAL AND METHODS: The data of 62 patients with Ruedi-Allgower type II/III tibial pilon fractures who were treated in Liuzhou People’s hospital from January 2017 to December 2018 were extracted in this retrospective analysis. There were 32 patients in the temporary external fixation (TEF) group and 30 patients in calcaneal traction (CT) group. Outcomes, including the duration of the surgical procedure, pin track infection, degree of limb swelling, time to second-stage operation, postoperative comfort score, and visual analog scale (VAS) score, were compared.
RESULTS: The effective rate of swelling reduction after treatment was 85% in the TEF group and 60% in the CT group; the average time to the second-stage operation was 8.34±1.29 days in the TEF group and 10.60±2.27 days in the CT group; the postoperative comfort scores were 70.1±3.2 and 61.3±3.5 in the TEF group and CT group, respectively; the postoperative VAS scores at 24 h, 48 h, and 7 days were 7.90±1.06, 4.88±0.83, 2.72±1.14 in TEF group, and 8.50±0.86, 6.27±1.36, 3.57±1.19 in CT group, respectively. There were 1 case of pin tract infection identified in the TEF group and 4 in the CT group. All differences were statistically significant (P<0.05).
CONCLUSIONS: The modified external fixation is more effective than calcaneal traction in treatment of Ruedi-Allgower type II/III tibial pilon fractures in the first-stage of combined management.
Keywords: Anesthesia, Conduction, External Fixators, Tibial Fractures, Traction, ankle fractures, Calcaneus, Fracture Fixation, Fracture Fixation, Internal, young adult
Background
Fracture of the distal tibial plafond, also termed pilon fracture, is caused by high-energy axial compression force of the tibia, driving vertically into the talus [1–3], which accounts for about 5% of tibial fractures [4,5]. Described by the Ruedi and Allgower X-ray classification scheme, tibial pilon fractures can be specified into 3 categories according to the size and displacement of articular fragments [6]. Type I fractures are defined as nondisplaced “cleavage fractures” of the tibial plafond, whereas type II and type III fractures are defined as simple displacement to substantial comminution of the articular surface. Serious ankle injuries often result from high-energy trauma such as war wounds or fall from a height, and the surgical choices varies based on the severity of bone defect [7–9]. Management of tibial fractures is a great challenge for orthopedic surgeons, particularly for the Ruedi-Allgower type II and III pilon fractures, due to the severe impaction of the distal tibia and soft tissue damage [10,11].
Although various operations have been proposed to treat tibial pilon fractures, no consensus has been achieved. From the perspective of soft tissue preservation, staged surgical reconstruction remains the standard treatment for the management of high-energy pilon fractures owing to its good management of both the osseous and soft tissue elements of the injury [12–15]. This management includes applications of a temporary spanning external fixator or calcaneal traction at the early stage, followed by open reduction and internal fixation (ORIF) once the surrounding soft tissues are amendable.
The temporary external fixator is relatively stable to fix the fractured end, but it needs to be implemented under general anesthesia or spinal anesthesia. In such instances, this approach would result in an increased financial cost and would potentially increase the risk from anesthesia. Therefore, our institution managed to modified this approach by using a simplified external fixation combined with regional anesthesia in the early stage of management to reduce the damage from anesthesia. In regards to the calcaneal traction, axial traction at the fracture site aids in recovering the limb length and alignment while reducing pain and providing favorable conditions for the elimination of swelling [16]. However, although it is easy to conduct, patients tend to become less physically active due to the unstable fixation of the fractured end.
To the best of our knowledge, no previous study has directly compared the effect of temporizing external fixation under regional anesthesia with calcaneal traction in staged management. In view of this, we retrospectively compared the treatment of modified external fixation and calcaneal traction before ORIF for Chinese patients with Ruedi-Allgower type II and III pilon fractures.
Material and Methods
STUDY DESIGN AND PARTICIPANTS:
In the period between January 2017 to December 2018, patients with Ruedi-Allgower type II/III pilon factures who were diagnosed and treated in Liuzhou People’s hospital were analyzed in this retrospective cohort study. Inclusion criteria were: 1) adults older than 18 years; and 2) unilateral Ruedi-Allgower type II/III pilon fractures with newly closed fractures (injured <48 h). Exclusion criteria were: 1) skin damage at the pin penetration site at admission; 2) severe soft tissue injury; and 3) complicated with diabetes and severe heart failure. The study was approved by the Ethics Committee of our hospital. Informed consents were waived due to the retrospective nature of this study.
TREATMENT PROCEDURE:
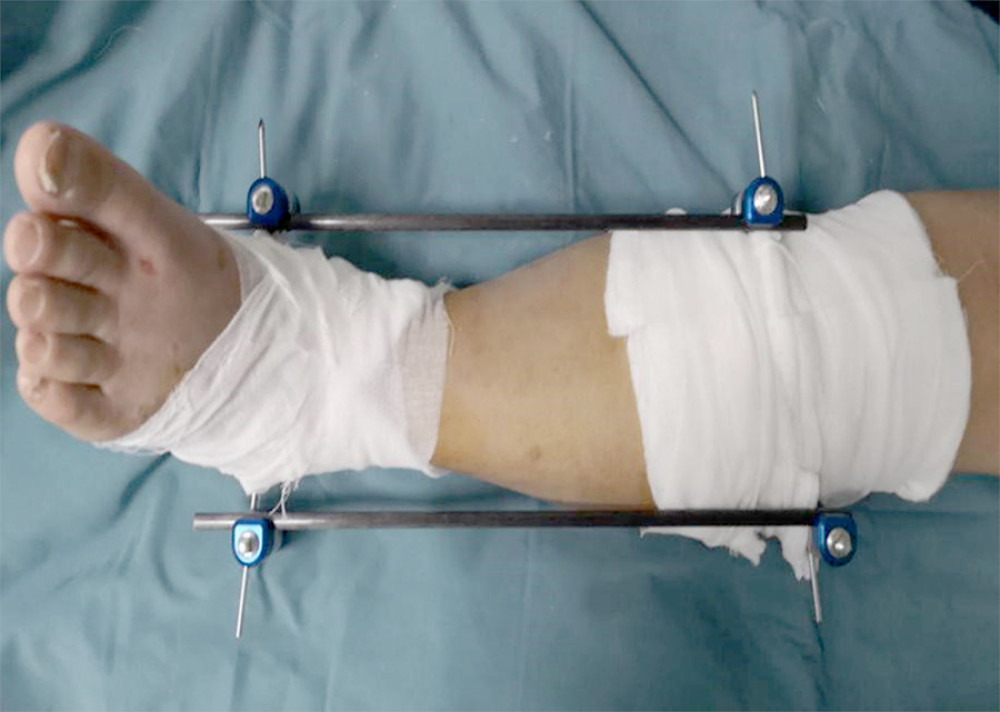
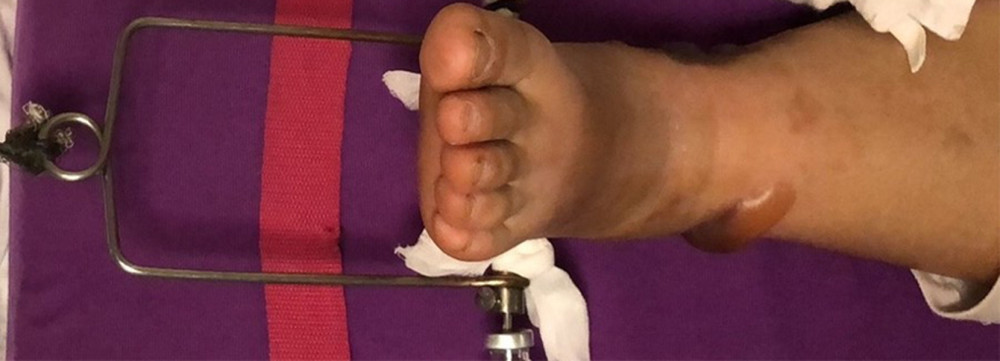
Patients were grouped according to the surgical procedures they received. In our institution, the routine steps of modified external fixation (MEF group) were as follow. The patient was in the supine position, the affected limb was routinely disinfected, covered with a sterile drape, and local anesthesia was performed on the tibial tubercle and the inner and outer sides of the calcaneus with 1% lidocaine. A 3.5-mm Schanz wire was drilled into the tibial tubercle and calcaneus. Then, the connecting rod was installed. A proximal buckle was tightened and pulled to the distal end to reposition the fixator, the device was placed as an angular deformity, and we tightened the distal buckle of the fixator (Figure 1). In the calcaneal traction (CT group), the following steps were performed. We selected the midpoint of the line between the tip of the medial malleolus and the posterior inferior edge of the calcaneus as the puncture site. After sterilizing the drape, we used 1% lidocaine for internal and external local anesthesia, and inserted a 4.0 bone round needle from the medial to the lateral penetrate the skin with a bone hammer to penetrate the calcaneus, and then connected the bone traction bow device. The weight of the traction was 1/7~1/10 of the patient’s weight (Figure 2). After the operation, both groups had the affected limb elevated, we changed the dressing frequently, and kept the local incision dry. X-rays were reviewed for the assessment of reduction of fracture 24 h after first-stage surgery. All patients were asked to stay in bed and remain in the hospital for the evaluation of outcomes. The determination to proceed with the later stage of ORIF was made by the treating surgeon whenever the soft tissue was deemed amendable.
DATA COLLECTION:
The patients’ demographics (eg, age, sex), the fracture classification according to Ruedi-Allgower, causes of injury, degree of limb swelling, time from injury to surgical procedure, and duration of operation were recorded. Preoperative limb swelling was defined as Degree I: the skin of the affected limb is tighter than normal skin, but dermatoglyphs present; Degree II: the skin of the affected limb is tighter than normal skin, and the streak disappears, the skin temperature is slightly higher than normal, but no tension blisters appear; and Degree III: the skin of the affected limb was tense and shiny, the streak disappeared, the skin temperature increased significantly, and tension blisters appeared.
FOLLOW-UP AND OUTCOMES:
Outcomes were evaluated by one senior surgeon at each postoperative visit. Clinical evaluation included the reduction of the swelling, pin site infection, and time from treatments to ORIF. The evaluation for the reduction of swelling was frequently used in the literature among Chinese patients, which was recorded as markedly effective [17]: swelling reduction time <3 days; effective: swelling reduction time 3~6 days; and invalid: swelling reduction time >6 days, the total effective rate was calculated by (markedly cases+effective cases)/total cases×100%.
The 28-item shortened General Comfort Questionnaire (GCQ) developed by Kolcaba in 2003 was used to measure the postoperative comfort score, which had been translated in a Chinese version to adapt to the target audience [18]. The questionnaire measures comfort in 4 contexts (physical, psychospiritual, social, and environmental) based on a 4-point Likert-type scale ranging from “Strongly Disagree” to “Strongly Agree”. A higher score indicates a higher level of comfort. Patients were also asked to subjectively report their postoperative pain level at rest on a visual analog scale (VAS) in 1-digit increments from 0, “none” to 10, “disabling” at 24 h, 48 h, and 7 days after the operation.
STATISTICAL ANALYSIS:
All analyses were performed in SPSS version 17.0 (Chicago, IL, USA). The normality of data distribution was tested by Kolmogorov-Smirnov test. Continuous variables are expressed as means±standard deviation or medians (IQR), as appropriate for the data distribution. Group differences were assessed by independent-samples
Results
STUDY POPULATION AND PATIENT CHARACTERISTICS:
Of the 62 patients (34 males and 28 females) whose age ranged from 20 to 62 years, 32 patients were grouped into the MEF group and 30 patients into the CT group. The characteristics of the patients in the 2 groups are summarized in Table 1. No significant differences were observed between the 2 treatment groups (all P>0.05, Table 1).
STATUS OF POSTOPERATIVE SWELLING:
Twenty-one patients were grouped to Degree II according to the preoperative evaluation for the degree of swelling. Of the 10 patients in the MEF group, 3 were evaluated as remarkedly effective and 7 were evaluated as effective, in terms of the postoperative swelling reduction. For the 11 patients in the CT group, the reduction of swelling in 2 patients was evaluated as remarkedly effective, 5 were effective, and 4 were ineffective. Of the 41 patients who were at Degree III of preoperative swelling, 22 patients were in the MEF group and 19 patients were in the CT group. In MEF group, there were 2, 15, and 5 patients evaluated as remarkedly effective, effective, and ineffective, respectively. In CT group, there were 1, 10, and 8 patients evaluated as remarkedly effective, effective, and ineffective, respectively. The total effective rate was significantly better in the MEF group compared to the CT group (84% vs 60%, P=0.032, Table 2).
PIN SITE INFECTION:
Pin site infection occurred in 1 and 4 patients from the MEF group and CT group, respectively. The percentages of occurrence were statistically higher in the CT group compared to the MEF group (13.3% vs 3.1, P=0.189, Table 3).
TIME TO ORIF:
The average times from treatment to ORIF were 8.34±1.29 days and 10.60±2.27 days in the MEF group and CT group, respectively, which differed significantly (P<0.001, Table 3).
POSTOPERATIVE COMFORT SCORE AND VAS SCORE:
The total comfort scores were 70.1±3.2 and 61.3±3.5 in MEF group and CT group, respectively (P<0.001). Compared to patients in the CT group, the comfort scores were significantly higher in the MEF group at each individual level (all P<0.05). Regarding the subjectively reported pain level, the VAS scores were significantly lower in the TEF group compared to the CT group at 24 h, 48 h, and 7 days after the treatment, respectively (all P<0.05, Table 3).
Discussion
This retrospective cohort study compared the effect of modified external fixation and calcaneal traction priori to ORIF for Chinese patients who were injured within 48 h and classified into Ruedi-Allgower type II and III tibial pilon fractures. The results suggested a significantly higher effective rate in terms of the swelling reduction in the MEF group compared to the CT group, irrespective of the Ruedi-Allgower type. The cases of pin site infection, time to proceed to ORIF, the total postoperative comfort score, and VAS score were also found to be significantly better in the MEF group.
In the context of lower-limb fractures, assessments of feasibility and quality of life, including the reduction of fracture, infection and union complication, soft tissue recovery, and functional outcomes, were commonly evaluated in the literature [19,20]. Various clinical studies have discussed the conventional strategies such as intramedullary nailing, locked plate, and external fixation in terms of the effectiveness in tibial or peroneal factures [21,22]. However, although all strategies were valid, the results indicated a comparable clinical outcome in the treatment of these fractures. A staged therapeutic strategy that considered the early application of temporary external fixation to avoid aggravating joint trauma and peripheral soft tissue injury was first introduced to treat high-energy fracture by Rotondo et al in 1993 [23]. Although multiple approaches are viable for pilon fractures, temporary external fixation in the staged approach allows for excellent restoration of anatomical structure of articular and fracture-dislocation of the ankle, with less medial soft tissue damage and low complication rates [24]. Soft tissue injury is an important reference when determining the optimal timing of internal fixation surgery, and swelling is a direct indicator. In this study, both groups presented promising results in the total effective rate of swelling reduction (MEF group: 84%, CT group: 60%). The duration from treatment to ORIF also indicated the swelling was notably reduced in both groups (MEF group: 8.34±1.29 days, CT group: 10.60±2.27 days). In a study on the staged treatment of pilon fractures, Zelle et al [11] stated that severe soft tissue injuries usually require a transitional stage of 1–4 weeks. Canton et al [25] reported that internal fixation can be attempted for tibial fractures combined with soft tissue injuries 2–13 days after the injury. A retrospective review [26] that investigated the treatment results of 35 Chinese patients with Ruedi-Allgower type I to type III pilon fractures reported an average of 11.8 days (range: 8–16 days) from external fixation or traction of calcaneal tubercle to definite initial fixation, which is congruent with the results of our study.
Regarding pin site infection, it is difficult to compare our results with other published series since many articles did not break down their infection type, but usually reported the superficial infection, which showing minor infection rates to 80% [27–29]. Despite a lack of research in this field, we found a recent study [30] analyzing a series of 402 patient who underwent external traction fixation in the staged management of tibial fracture, which found a relatively lower incidence of pin site infection compared to our study (0.2% vs 3.1%); this might be explained by the milder impairment on the tibial fractures in patients in their study. In addition, the process of regional anesthesia in the MEF group was not conducted in a sterilized operating room, which might also account for the higher incidence of pin site infection.
In 2017, Manoli et al [31] concluded that the use of regional anesthesia in treatment of tibial plateau fractures is associated with decreased pain levels in the early postoperative period (<3 months). For tibial pilon fractures, there was a significant difference between the MEF group and CT group in the VAS scores as well as the comfort scores. It should be noted that the VAS scores in each follow-up visit were lower in the MEF group compared to the CT group, indicating patients in the MEF group had less pain compared to patients in the CT group and therefore might require fewer pain-reducing medications during management. This assumption might be inconclusive since previous studies [32,33] have not demonstrated a significant improvement in pain reduction comparing with external fixation in a 2-stage approach vs other treatment procedures.
Limitations of this study include the retrospective design and small sample size, which might reduce the strength of the study. Second, although no significant differences were found between the groups in patient characteristics, we did not conduct a multivariate analysis to balance the potential effect from other covariates because we felt the relatively small sample size may affect the statistical power of regression analysis. Some bias may have existed in the selection of the technique due to the choice of surgical procedure depending on the surgeon’s preference. Finally, outcomes after the second-stage of this staged management that reflect patient ability to function and their quality of life were not assessed in this study.
Conclusions
Our results suggest that the simplified temporizing external fixation under regional anesthesia is superior to calcaneal traction in the first stage of combined management for Chinese patients with Ruedi-Allgower type II/III tibial pilon fractures. However, due to the insufficient sample size in this retrospective study, the results might be biased and should be validated in a prospective study with a larger sample size.
References
1. Jacob N, Amin A, Giotakis N, Management of high-energy tibial pilon fractures: Strategies Trauma Limb Reconstr, 2015; 10; 137-47
2. Cole PA, Mehrle RK, Bhandari M, Zlowodzki M, The pilon map: Fracture lines and comminution zones in OTA/AO type 43C3 pilon fractures: J Orthop Trauma, 2013; 27; e152-56
3. Di Giorgio L, Touloupakis G, Theodorakis E, Sodano L, A two-choice strategy through a medial tibial approach for the treatment of pilon fractures with posterior or anterior fragmentation: Chin J Traumatol, 2013; 16; 272-76
4. Mauffrey C, Vasario G, Battiston B, Tibial pilon fractures: A review of incidence, diagnosis, treatment, and complications: Acta Orthop Belg, 2011; 77; 432-40
5. Ballal A, Rai HR, Shetty SM, A prospective study on functional outcome of internal fixation of tibial pilon fractures with locking plate using minimally invasive plate osteosynthesis technique: J Clin Diagn Res, 2016; 10; Rc01-4
6. Rüedi TP, Allgöwer M, The operative treatment of intra-articular fractures of the lower end of the tibia: Clin Orthop Relat Res, 1979(138); 105-10
7. Rollo G, Falzarano G, Ronga M, Challenges in the management of floating knee injuries: Results of treatment and outcomes of 224 consecutive cases in 10 years: Injury, 2019; 50(Suppl 4); S30-38
8. Grubor P, Milicevic S, Grubor M, Meccariello L, Treatment of bone defects in war wounds: Retrospective study: Med Arch, 2015; 69; 260-64
9. Fortina M, Maniscalco P, Carulli C, Jockey injuries during the Siena “Palio”. A 72-year analysis of the oldest horse race in Italy: Injury, 2019; 50(Suppl 4); S56-59
10. Bear J, Rollick N, Helfet D, Evolution in management of tibial pilon fractures: Curr Rev Musculoskelet Med, 2018; 11; 537-45
11. Zelle BA, Dang KH, Ornell SS, High-energy tibial pilon fractures: An instructional review: Int Orthop, 2019; 43; 1939-50
12. Patterson MJ, Cole JD, Two-staged delayed open reduction and internal fixation of severe pilon fractures: J Orthop Trauma, 1999; 13; 85-91
13. Shah KN, Johnson JP, O’Donnell SW, External fixation in the Emergency Department for pilon and unstable ankle fractures: J Am Acad Orthop Surg, 2019; 27; e577-84
14. Hebert-Davies J, Kleweno CP, Nork SE, Contemporary strategies in pilon fixation: J Orthop Trauma, 2020; 34(Suppl 1); S14-20
15. Boraiah S, Kemp TJ, Erwteman A, Outcome following open reduction and internal fixation of open pilon fractures: J Bone Joint Surg Am, 2010; 92; 346-52
16. Sobol G, Gibson P, Patel P, Low incidence of neurovascular complications after placement of proximal tibial traction pins: Orthopedics, 2017; 40; e1004-8
17. Sun GC, Fu BJ, Zhao YJPerioperative application of different calcaneal traction weights in the treatment of Pilon fracture: Journal of Traumatic Surgery, 2020; 22; 541-43 [in Chinese]
18. Kolcaba K, Schirm V, Steiner R, Effects of hand massage on comfort of nursing home residents: Geriatr Nurs, 2006; 27; 85-91
19. Petruccelli R, Bisaccia M, Rinonapoli G, Tubular vs profile plate in peroneal or bimalleolar fractures: Is there a real difference in skin complication? A retrospective study in three level I trauma center: Med Arch, 2017; 71; 265-69
20. Rollo G, Pasquino A, Pichierri P, The damage control in tibial pilon open fractures with a new external fixator delta frame: Journal of Acute Disease, 2017; 6; 222-26
21. Bisaccia M, Cappiello A, Meccariello L, Nail or plate in the management of distal extra-articular tibial fracture, what is better? Valutation of outcomes: SICOT J, 2018; 4; 2
22. Falzarano G, Pica G, Medici A, Foot loading and gait analysis evaluation of nonarticular tibial pilon fracture: A comparison of three surgical techniques: J Foot Ankle Surg, 2018; 57; 894-98
23. Rotondo MF, Schwab CW, McGonigal MD, ‘Damage control’: An approach for improved survival in exsanguinating penetrating abdominal injury: J Trauma, 1993; 35; 375-82 discussion 382–83
24. Lavini F, Dall’Oca C, Mezzari S, Temporary bridging external fixation in distal tibial fracture: Injury, 2014; 45(Suppl 6); S58-63
25. Canton G, Santolini F, Stella M, Strategies to minimize soft tissues and septic complications in staged management of high-energy proximal tibia fractures: Eur J Orthop Surg Traumatol, 2020; 30; 671-80
26. Hu C, Zhu W, Chahal K, Open reduction and internal fixation of Gustilo type-I and type-II open pilon fractures using a lateral approach: J Orthop Surg (Hong Kong), 2019; 27; 2309499019864722
27. Green SA, Complications of external skeletal fixation: Clin Orthop Relat Res, 1983(180); 109-16
28. Haller JM, Holt D, Rothberg DL, Does early versus delayed spanning external fixation impact complication rates for high-energy tibial plateau and plafond fractures?: Clin Orthop Relat Res, 2016; 474; 1436-44
29. Sirkin M, Sanders R, DiPasquale T, Herscovici D, A staged protocol for soft tissue management in the treatment of complex pilon fractures: J Orthop Trauma, 1999; 13; 78-84
30. Yang JZ, Zhu WB, Li LB, Dong QR, Early complications of preoperative external traction fixation in the staged treatment of tibial fractures: A series of 402 cases: World J Clin Cases, 2020; 8; 4743-52
31. Manoli A, Atchabahian A, Davidovitch RI, Egol KA, Spinal anesthesia improves early pain levels after surgical treatment of tibial plateau fractures: J Orthop Trauma, 2017; 31; 164-67
32. Wang Z, Qu W, Liu T, A two-stage protocol with vacuum sealing drainage for the treatment of type C pilon fractures: J Foot Ankle Surg, 2016; 55; 1117-20
33. Minator Sajjadi M, Ebrahimpour A, Okhovatpour MA, The outcomes of pilon fracture treatment: Primary open reduction and internal fixation versus two-stage approach: Arch Bone Jt Surg, 2018; 6; 412-19
Tables
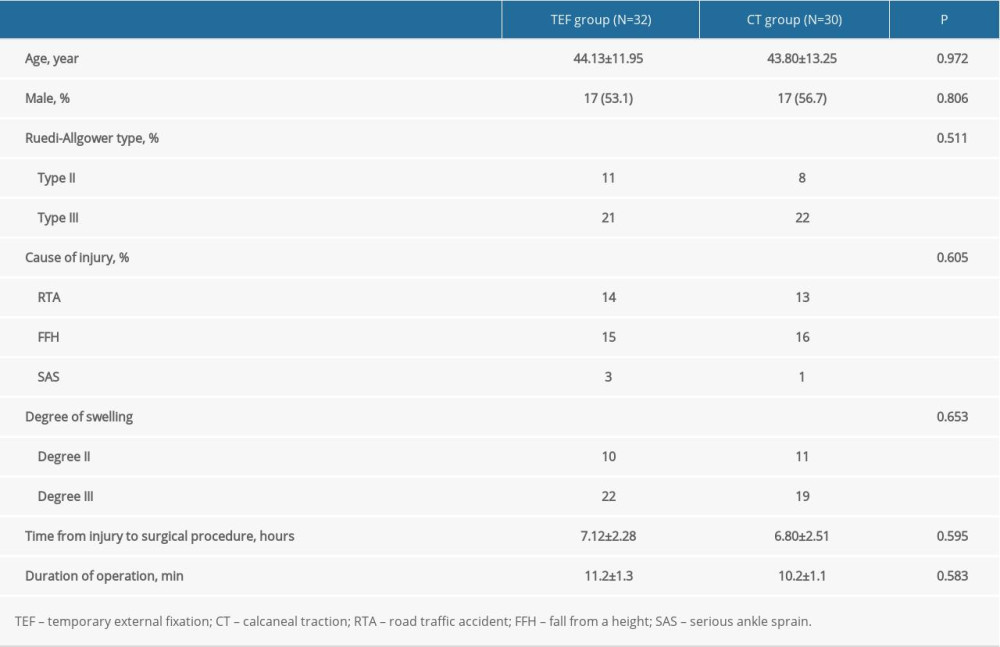 Table 1. Characteristics of the patients.
Table 1. Characteristics of the patients.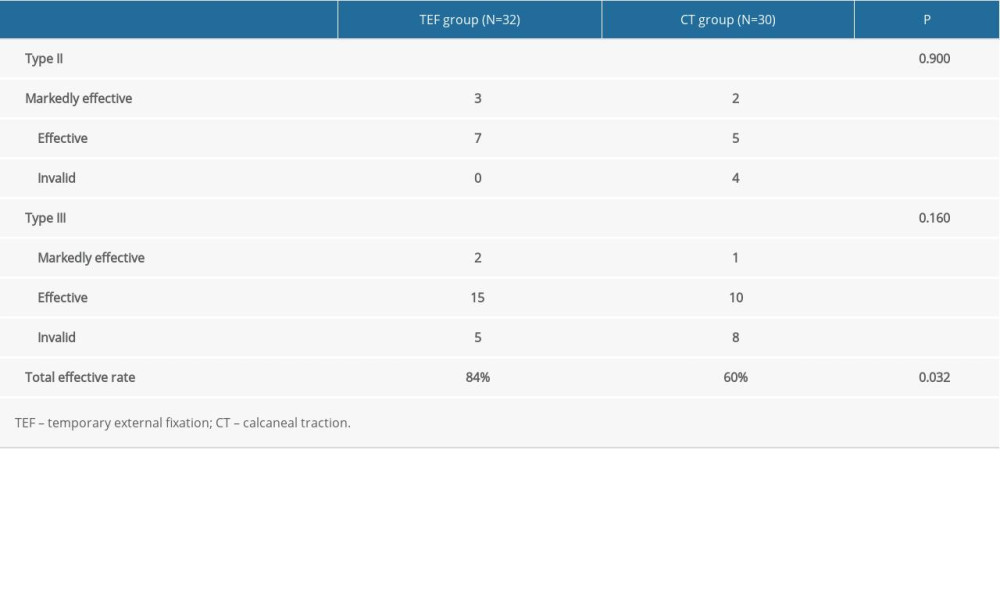 Table 2. Outcome assessments for swelling subsided by fracture type of patients.
Table 2. Outcome assessments for swelling subsided by fracture type of patients.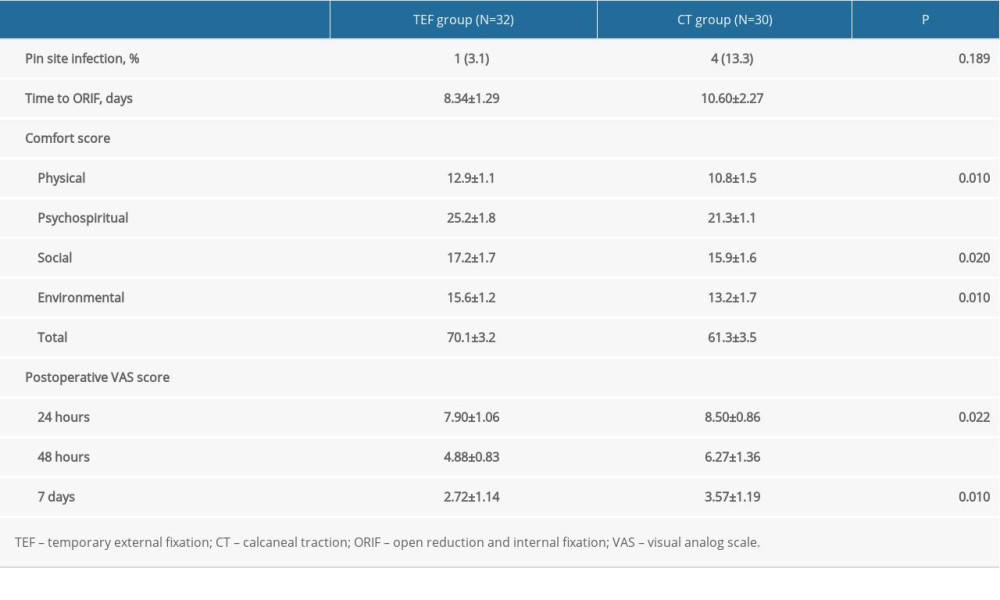 Table 3. Postoperative outcomes.
Table 3. Postoperative outcomes. Table 1. Characteristics of the patients.
Table 1. Characteristics of the patients. Table 2. Outcome assessments for swelling subsided by fracture type of patients.
Table 2. Outcome assessments for swelling subsided by fracture type of patients. Table 3. Postoperative outcomes.
Table 3. Postoperative outcomes. In Press
05 Mar 2024 : Clinical Research
Muscular Function Recovery from General Anesthesia in 132 Patients Undergoing Surgery with Acceleromyograph...Med Sci Monit In Press; DOI: 10.12659/MSM.942780
05 Mar 2024 : Clinical Research
Effects of Thermal Insulation on Recovery and Comfort of Patients Undergoing Holmium Laser LithotripsyMed Sci Monit In Press; DOI: 10.12659/MSM.942836
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952