15 May 2022: Database Analysis
Bibliometric Visualization Analysis of Microbiome-Gut-Brain Axis from 2004 to 2020
Hui Wang1ABE, Tianlin Long2ACG, Jing You2BC, Ping Li23ACDF*, Quanhua Xu2AGDOI: 10.12659/MSM.936037
Med Sci Monit 2022; 28:e936037
Abstract
BACKGROUND: The microbiome-gut-brain axis (MGBA) is the biochemical signal of the digestive tract and central nervous system. MGBA disorders have been increasingly involved in the pathological process of neurological diseases. This study aimed to investigate the research hot spots of MGBA from 2004 to 2020.
MATERIAL AND METHODS: Using bibliometric analysis from the Web of Science Core Collection (WOSCC) database, 3993 documents on the MGBA were retrieved and visual analysis was conducted.
RESULTS: The MGBA has received attention worldwide and will continue to be a research hot spot. Emerging research organizations and scholars of the MGBA and the research of John F. Cryan and colleagues from Ireland in the MGBA have been recognized by many scholars. However, the research of Chinese scholars and organizations appeared to have less impact due to lack of research innovation and collaboration with other countries/regions. Keyword analysis showed that neuroinflammation was a hot spot and that eminent scholars had begun to work in the field of MGBA.
CONCLUSIONS: This work provided an overall view of the literature on the MGBA worldwide, and the analysis provided a comprehensive overview of MGBA research. It further revealed the interaction between the gut microbiota (eg, Akkermansia, Parabacteroides) and the specific regulatory network of the gut microbiota and metabolites, neuroinflammation, and neural networks, which can facilitate the development of effective treatment strategies using microbiota for targeting neuroinflammation and conducting large-scale clinical trials of neurological diseases.
Keywords: Bibliometrics, Gastrointestinal Microbiome, Nervous System Diseases, brain-gut axis, Humans, Microbiota
Background
A large number of bacteria, fungi, viruses, protozoa, and other microorganisms populate the normal human intestinal tract, and their collective genome that is found on and within the body comprises the microbiome [1]. There are more than 1014 bacterial cells in the gastrointestinal tract, the vast majority of which are located in the ileum and colon [2]. The digestive tract of a healthy person contains about 1000 kinds of microbes, and the total number of cells of these microbes is about 10 times the number of cells in the body [3,4]. The gut microbiome can be regarded as a functional organ, which is acquired after the individual is born. The number of genes encoded by the intestinal flora is about 150 times that of the host’s genes [3]. The sum of the genomic information of these intestinal microorganisms is also called “gut metagenome”, which is the “second genome” that controls the health of the body [4,5], and the host’s physiological metabolic activities are jointly affected through the interaction with the host genome [6]. The human gut microbiome is a complex ecosystem with important physiological functions and psychological activities in its host, such as digestion, metabolism, immunity, and emotion [7,8]. The use of 16S ribosomal RNA and whole genome sequencing techniques has enabled us to understand the diversity of intestinal flora [9]. Through metagenomics, metabolomics, and other omics analysis techniques, microbiome-wide association studies, host-reaction mechanism analysis, and germ-free animal disease replication models can be combined to determine the types of intestinal flora causing disease and the molecular mechanisms of specific interactions [10,11].
Over the past 2 decades, researchers have come to recognize the interconnection between gut microbiota and biomedical sciences and the important role microorganisms play in maintaining homeostasis and regulating body systems [1,7,8], including the central nervous system (CNS) [12,13]. The microbiome-gut-brain axis (MGBA) is the biochemical signal of the digestive tract and CNS. The intestinal flora and the brain have 2-way communication through the autonomic nervous system, intestinal nervous system, immune system, intestinal endocrine signals, neurotransmitters, branch-chain amino acids, bile acids, short-chain fatty acids (SCFA), spinal cord, hypothalamic-pituitary-adrenal axis, peptidoglycan, and other pathways and media [14,15]. Animal experiments are helpful to reveal the important roles of MGBA in brain development, neuroinflammation, anxiety, cognition, and pain [16,17]. Many reports have been devoted to explaining the bidirectional communication pathway between the gut microbiota and the CNS, and MGBA disorders are increasingly involved in the pathological process of nervous system diseases, such as multiple sclerosis (MS), Parkinson disease (PD), Alzheimer disease (AD), autism spectrum disorder (ASD), stroke, brain injury, epilepsy, and depression [16–19].
Experiments have confirmed that intestinal barrier defects connect intestinal flora with immune activation, which can trigger a systemic inflammatory response, further damage the blood-brain barrier (BBB), promote neuroinflammation, and eventually lead to nerve damage and degeneration [15,20]. An abnormal MGBA is believed to cause the deposition of β-amyloid in AD and the neuropathological features unique to PD, including the misfolding and aggregation of α-synuclein. In some cases, specific microbial populations are closely related to the progression of diseases, such as the types of bacteria in the periodontal, oral, and nasal cavities of patients with AD and PD and the abundance of
In this work, we visually analyzed the research hot spots on the MGBA from 2004 to 2020 by bibliometric analysis from the Web of Science Core Collection (WOSCC) database. These data revealed the research hot spots of MGBA and new ideas for the molecular mechanism of the MGBA, and provided a new platform for the therapy and intervention of neurological diseases.
Material and Methods
DATA COLLECTION:
We searched all literature data on the MGBA index in the WOSCC (Clarivate Analysis, Boston, MA, USA;
DATA ANALYSIS:
The general information about the distribution of publication year, organization, journal, and authors were analyzed by the WOS-based literature analysis. The publication number, article type, and citation h-index were assessed by the “citation report” function of the WOS. The bibliometric analysis and network visualization were performed using VOSviewer (version 1.6.15; Centre for Science and Technology Studies, Leiden University, the Netherlands) and CiteSpace (version 5.7. R3; College of Information Science and Technology, Leisel University, USA), and the ranking order was performed using the standard competition ranking method. The parameters of the VOSviewer method (Linlog/modularity) and CiteSpace were conducted as described by Chen et al [27]. The parameters of CiteSpace were set as follows: Method (LLR), time slicing (2004–2020), years per slice (1), term source (all selection), term type (burst terms), node type (1 chosen at a time), selection criteria (top 50 objects), and pruning (pathfinder) [27].
Results
PUBLICATION OUTPUTS:
From 2004 to 2020, there were 159 316 publications related to the microbiota (76.75% articles and 13.02% reviews), while there were 2262 (56.65%) articles, 1402 (35.11%) reviews, and 329 (8.24%) other documents, such as editorials, meetings, book chapters, or letters, among the 3993 documents on the MGBA. By contrast, the high proportion of reviews on the MGBA indicated that it has received more attention and deserved to be discussed. Publications related to the MGBA are shown in Figure 1. The data showed that the first publication of MGBA appeared in 2004. It was not until 2008 that a few more articles appeared, and then documents continued to be published, with the number rising steadily beginning in 2010 (Figure 1).
COUNTRIES/REGIONS AND ORGANIZATION:
A total of 98 countries/regions were involved in research on the MGBA. The number of documents and citations for countries/regions are presented in Figure 2A and 2B, respectively. Some of the research was based on the cooperation between different countries/regions, such as the United States and Ireland (Figure 2B). Three of the 10 most productive countries/regions were the United States (1355), China (660), and Canada (296) (Table 1). The United States and China were responsible for most of the study of the MGBA, accounting for about 50.06% of all publications. Although China had a large number of documents, the number of citations (9451) was lower than that of Canada (14 602), the United Kingdom (10 213), Ireland (19 415), and the United States 39 757 (Figure 2B). This suggests that China needs to increase its influence by cooperating more closely with other countries/regions and producing more innovative research.
About 3835 organizations participated in the 3993 publications on the MGBA. Three of the 10 most productive organizations were the University College Cork, McMaster University, and University of California Los Angeles (Table 2). The biggest surprise was the University College Cork in Ireland, with 180 documents and 9154 citations. McMaster University had 98 documents, 8933 citations, and 52 total link strengths. Zhejiang University had 43 documents, 1104 citations, and 11 total link strengths. Another organization from Ireland, the National University Ireland University College Cork, also did well, with 68 documents and 9660 citations. However, the United States had a clear advantage in the number of institutions (the 5 US organizations had 276 documents and 10 827 citations). The co-authorship of the organization showed that some organizations existed in isolation, such as the Federal University of Rio De Janeiro and Basque Foundation for Science (Figure 3A). It is clear that documents from Ireland had a wider range of influence, and University College Cork dominated the field of MGBA research with more cooperation with other organizations. The Chinese Zhejiang University had less cooperation with other organizations (Figure 3A). VOSviewer analysis showed that there were 193 organizations with a minimum of 10 documents, including Central South University in China (Figure 3B). Central South University was the most recent active organization with the most articles on the MGBA and it worked with institutions including the University California San Diego, University of Chicago, Yale University, University of Helsinki, and Nanjing Medical University (Figure 3B). This indicates that Central South University is an emerging research organization in the MGBA.
JOURNAL ANALYSIS:
The 3993 documents on the MGBA were published in 1190 journals from 2004 to 2020, and the top 15 journals are listed in Table 3, including Scientific Reports, Nutrients, and Brain Behavior and Immunity. The journal with the most publications was Scientific Reports with 96 documents (impact factor [IF] 3.998, and journal citation reports [JCR] Q1). For the JCR partition analysis, 8 journals were Q1, 1 journal was Q1/Q2, 4 journals were Q2, and 2 journals were Q2/Q3. Scientific Reports, Nutrients, and Brain Behavior and Immunity may be the most popular journals and have different IF distributions. In general, documents on the MGBA have been accepted by excellent journals, which helps to promote the awareness of the MGBA to a wide range of readers and researchers.
AUTHORS ANALYSIS:
A total of 17 357 authors participated in the publication of MGBA-related documents. A total of 338 authors with at least 5 MGBA-related documents were visualized. As shown in Figure 4A, the overlay visualization shows the co-authorship relations of authors. John F. Cryan and his colleagues, Timothy G. Dinan, Gerard Clarke, Catherine Stanton, and Fergus Shanahan, are linked with the red cluster, indicating they had close cooperation in MGBA authorship (Figure 4A). However, authors including Dong H. Kim, Kenji Hashimoto, and Jasmohan S. Bajaj lack contact with other peripheral scholars (Figure 4A). Furthermore, John F. Cryan had more extensive cooperation with other peripheral scholars (Figure 4B), and Emeran A. Mayer also had collaborated with other authors, including John F. Cryan, Rob Knight, and Yolanda Snaz (Figure 4B). The top 10 core authors in MGBA research from 2005 to 2020 are listed (Table 4), including John F. Cryan, Timothy G. Dinan, and Gerard Clarke. John F. Cryan and his colleagues Timothy G. Dinan, Gerard Clarke, Catherine Stanton, and Fergus Shanahan from the University College Cork accounted for 5 seats. John F. Cryan was the first with 187 documents and 16 808 total citations and was followed by Timothy G. Dinan with 169 documents and 16 131 citations (Table 4). Fergus Shanahan was the last who was from University College Cork, with 22 documents and 1681 citations. John F. Cryan and Dong H. Kim had an h-index of 88 and 84, respectively. Thus, this indicates that the research on the MGBA of John F. Cryan and his colleagues is widely recognized.
CITATION ANALYSIS:
The top 10 co-citation analysis of documents on MGBA are listed in Table 5 and include 3 reviews and 7 articles. A recent article “Gut microbiota regulate motor deficits and neuroinflammation in a model of Parkinson’s disease” (Cell, 2016) by Timothy R. Sampson had 869 citations and revealed the relationship between gut bacteria and neuroinflammation and motor symptoms [28] (Table 5). The articles of MGBA with high citations have been widely accepted and have inspired recent research, and these recent studies will have a positive influence on this field.
KEYWORD ANALYSIS:
A total of 5928 keywords were included in the 3993 documents on the MGBA and 220 authors were visualized. According to the number of occurrences, the keywords included gut-microbiota, microbiota, microbiome, gut-brain axis, probiotics, inflammation, depression, gut microbiome, stress, anxiety, Alzheimer’s disease, dysbiosis, obesity, Parkinson’s diseases, microbiota-gut-brain-axis, and neuroinflammation. Mapping analysis shows the relevant author keywords related to microbiota-gut-brain-axis, inflammation, or probiotics (Figure 5A). According to the statistical analysis of the author keywords, many events were associated with the blood-brain barrier, hippocampus, and microglia, including the processes of inflammation, neuroinflammation, and oxidative stress, which were involved in depression, stroke, ASD, MS, PD, and AD (Figure 5A). The average publication year for the keyword neuroinflammation was 2019 (Figure 5B; yellow circle). The keyword irritable bowel syndrome showed the highest burst strength with 9.85, which burst in 2014 and continued until 2020, and the keyword Bifidobacterium showed the lowest burst strength with 2.91, which burst in 2015 and continued until 2020 (Figure 5C). The keywords epigenetics, autoimmunity, stroke, short-chain fatty acid, immunity, and gluten had the strongest high citation bursts, and the keyword immunity had 3.49 burst strength, which burst in 2018 (Figure 5C). The data show that neuroinflammation is a hot spot of research and eminent scholars have begun to work in field of the MGBA.
Discussion
This is the latest application of bibliometric analysis on MGBA research, involving 3993 publications retrieved from the WOS core database. The results of bibliometrics analysis presented a comprehensive overview of the development of MGBA articles over the past 15 years. The field of MGBA research has increased tremendously over the last decade. The number of MGBA publications rapidly increased from 12 in 2010 (n=12) to 1078 by December 30, 2020. Some rapidly developing organizations and scholars joined the research work in this field. Increases in recent studies have further revealed the important role of the MGBA in neurological diseases, and the scope of research has also become more extensive, including preclinical animal experiments and numerous clinical trials. The MGBA will continue to attract a great deal of interest and research and to be a hot topic in the coming decade, revealing detailed signaling pathways and molecular mechanisms associated with diseases.
The United States has been the most productive country in MGBA research, followed by China, probably due to the launch of the second phase of the Integrative Human Microbiome Project by the National Institutes of Health in 2013 and the Microbiome Program of the Chinese Academy of Sciences in 2017, which has attracted a wide range of scholars with an interest in the field of the MGBA and has provided substantial financial support. Since then, the MGBA has become immensely popular and has had many citations [28–32]. However, John F. Cryan and Timothy G. Dinan from University College Cork (Cork, Ireland), are among the top 2 authors with publications in this field, are far ahead of other authors, and have led the work of research in Ireland and worldwide in the field of MGBA. John F. Cryan, Timothy G. Dinan, Sarkis K. Mazmanian, Paul H. Patterson, Jeremy K. Nicholson, Sven Pettersson, and other scholars in the fields of gastroenterology, microbiology, and neurology suggest discoveries for new research fields, which provide an emerging platform for treatment and intervention of multiple diseases, such as depression, autoimmune disease, MS, ASD, PD, and obesity.
Keyword analysis suggested that inflammation and neuroinflammation are the research hot spots in the field of MGBA. The MGBA involves the host immune system [33], and unbalanced immune-inflammatory issues cause neurological disorders [34]. In recent years, communication of the peripheral immune cells to the brain and the MGBA has received increasing attention for its ability to modulate brain function [35]. Gut microbiota alteration impairs cognitive functioning via an increase of systemic inflammation [36]. The microbiota metabolic and immune-inflammatory axes are involved in brain development and behavior and CNS diseases via the MGBA [32]. The process of neuroinflammation that underlies several neurological disorders, such as PD, AD, ASD, and MS, may involve, or be strengthened by, peripheral inflammatory processes, such as the NF-κB, JAK/STAT, MAPKs, PPARs, NLRP3, and other signaling pathways involved in chronic intestinal inflammation [37].
In the past 2 decades, neuroimmunology has gradually become a research hot spot [38]. Some preclinical studies have found that the gut microbiome is critical for the pro-inflammatory and anti-inflammatory activities of microglia [39]. Therefore, gut microbiota imbalance may interfere with the maturation and activity of these brain-resident immune cells and may be a key driver in nervous system disorders. A high level of α-synuclein in the gut is positively correlated with brain damage, neuroinflammation, and neurodegeneration of dopaminergic neurons in patients with PD [40,41]. Extensive evidence from human samples and animal models support the involvement of inflammation in the onset or progression of PD [42], and fecal samples from patients with PD present low levels of
The MGBA, as a bridge between inflammation and CNS diseases, is an attractive strategy, but still, some questions need to be answered: Which species or groups of bacteria play a dominant role in different diseases? What is the significance of the different microbiota represented by the same disease in different stages or different populations? What is the interaction between different microflora? Lastly, what is the specific regulatory mechanism of microbiota in inflammatory and oxidative biomarkers? For example, a ketogenic diet or treatment with both
There were some limitations to this bibliometric analysis of the MGBA. Firstly, the publications were limited to the WOSCC database with the deadline of December 30, 2020. Although the WOSCC is the most frequently used database for bibliometric analyses, not all MGBA-relevant publications were contained in our search terms of the title, abstract, keywords, literature type, and language. Secondly, the document type labels assigned by WOS may be inaccurate. Thirdly, the bibliometrics method did not weigh the quality or scientific rigor of any individual publication. However, we still believed that the present findings provided an effective representative of the overall situation and general trend for MGBA research.
Conclusions
This work provided an overview of the further literature analysis of MGBA worldwide, and the analysis provided a comprehensive overview of MGBA research. This field is gradually gaining interest by many scholars, and we believe the MGBA will be a hot spot in the coming decade, revealing detailed molecular mechanisms and providing a new platform for the therapy and intervention of neurological diseases. The MGBA, as a bridge between inflammation and CNS diseases, is an attractive strategy. We further revealed the interaction between the gut microbiota (eg,
Figures
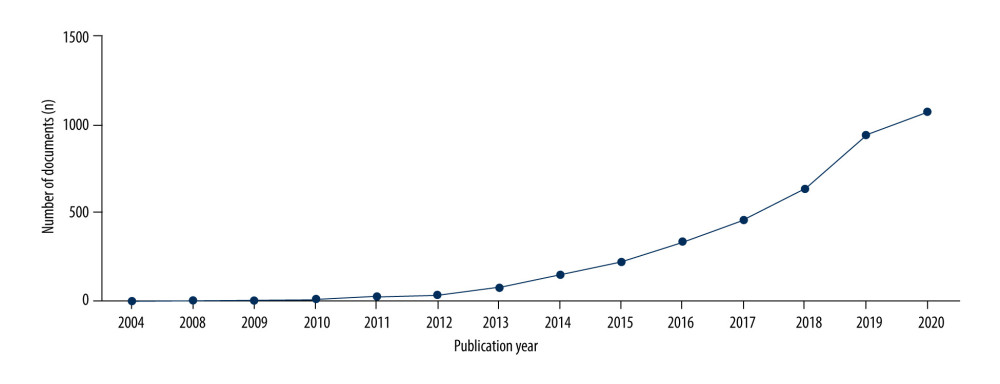 Figure 1. Distribution of publications of the microbiome-gut-brain axis (MGBA) from 2004 to 2020, by the GraphPad Prism (version 5.0; University of California San Diego, San Diego, CA, USA).
Figure 1. Distribution of publications of the microbiome-gut-brain axis (MGBA) from 2004 to 2020, by the GraphPad Prism (version 5.0; University of California San Diego, San Diego, CA, USA). 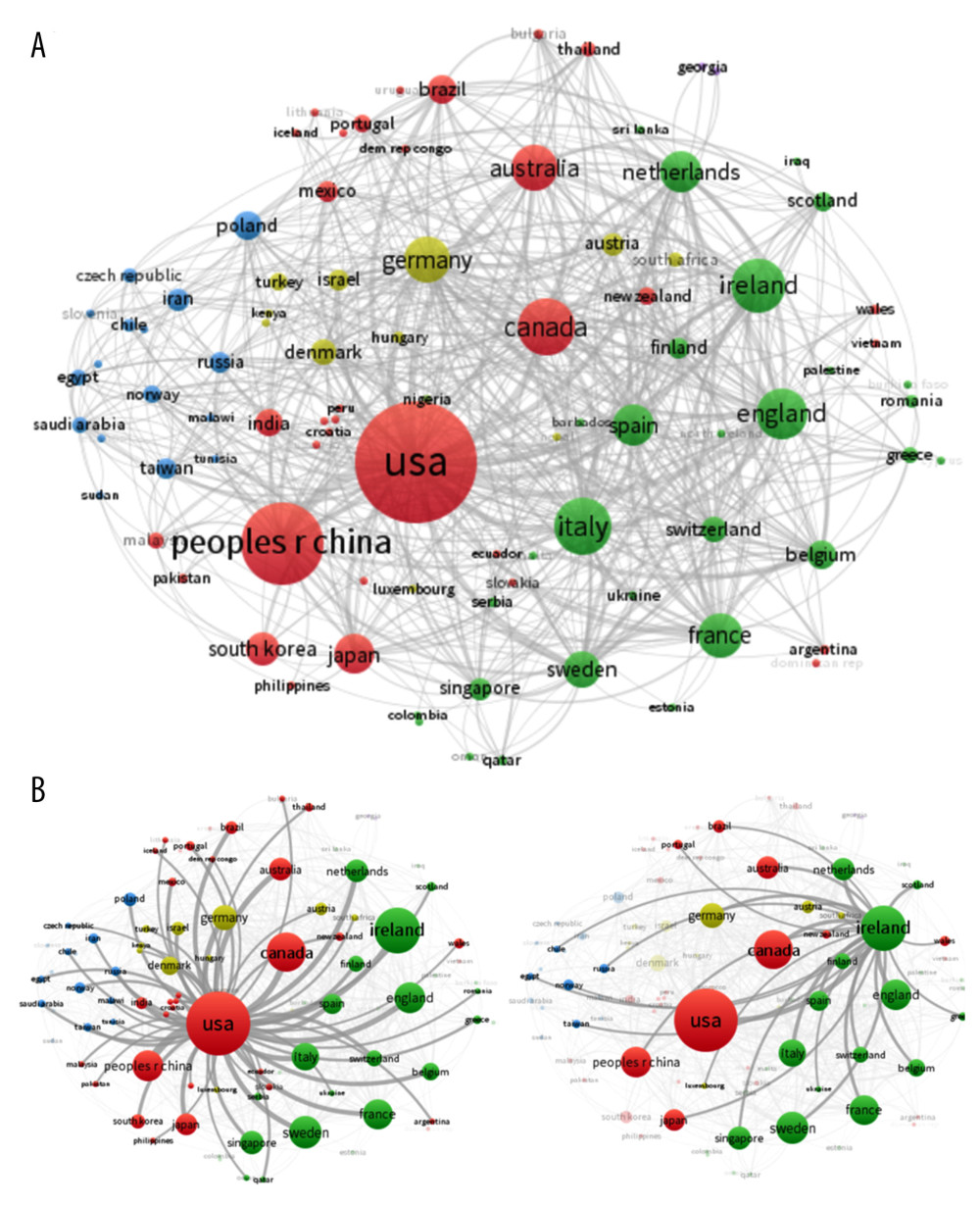 Figure 2. The documents on the microbiome-gut-brain axis (MGBA) in different countries/regions. (A) Map of the cooperation between 34 countries by the VOSviewer. (B) The cooperation between the United States and Ireland. Different colors indicate clusters of collaboration between countries, the size of the circle indicates citations to the publication, and the thickness of the line indicates the extent of collaboration. The network visualization was performed by VOSviewer (version 1.6.15; Centre for Science and Technology Studies, Leiden University, the Netherlands).
Figure 2. The documents on the microbiome-gut-brain axis (MGBA) in different countries/regions. (A) Map of the cooperation between 34 countries by the VOSviewer. (B) The cooperation between the United States and Ireland. Different colors indicate clusters of collaboration between countries, the size of the circle indicates citations to the publication, and the thickness of the line indicates the extent of collaboration. The network visualization was performed by VOSviewer (version 1.6.15; Centre for Science and Technology Studies, Leiden University, the Netherlands). 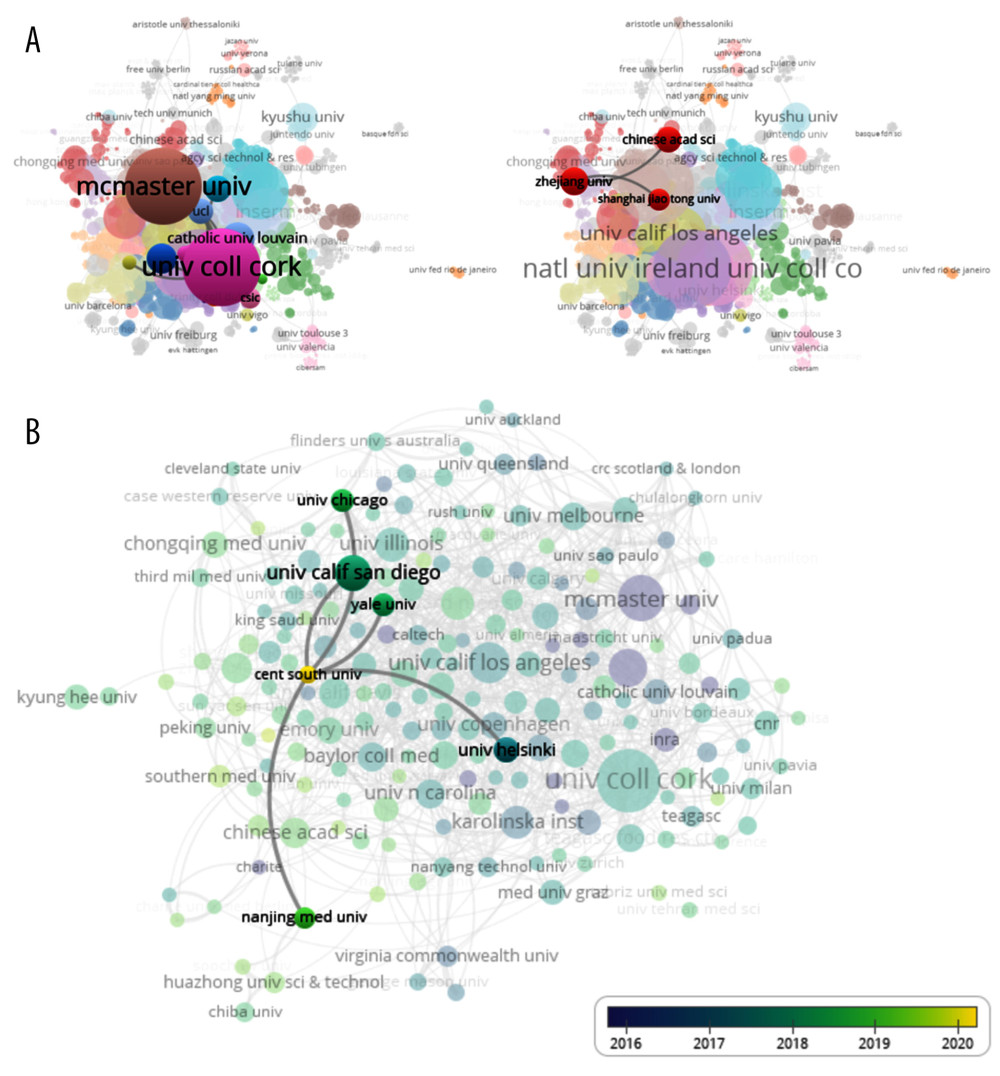 Figure 3. Co-author analysis of organizations. (A) The co-authorship of organizations showed the collaboration of University College Cork and Zhejiang Univ. (B) The average published year showed the recent active organization, Central South University. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands).
Figure 3. Co-author analysis of organizations. (A) The co-authorship of organizations showed the collaboration of University College Cork and Zhejiang Univ. (B) The average published year showed the recent active organization, Central South University. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). 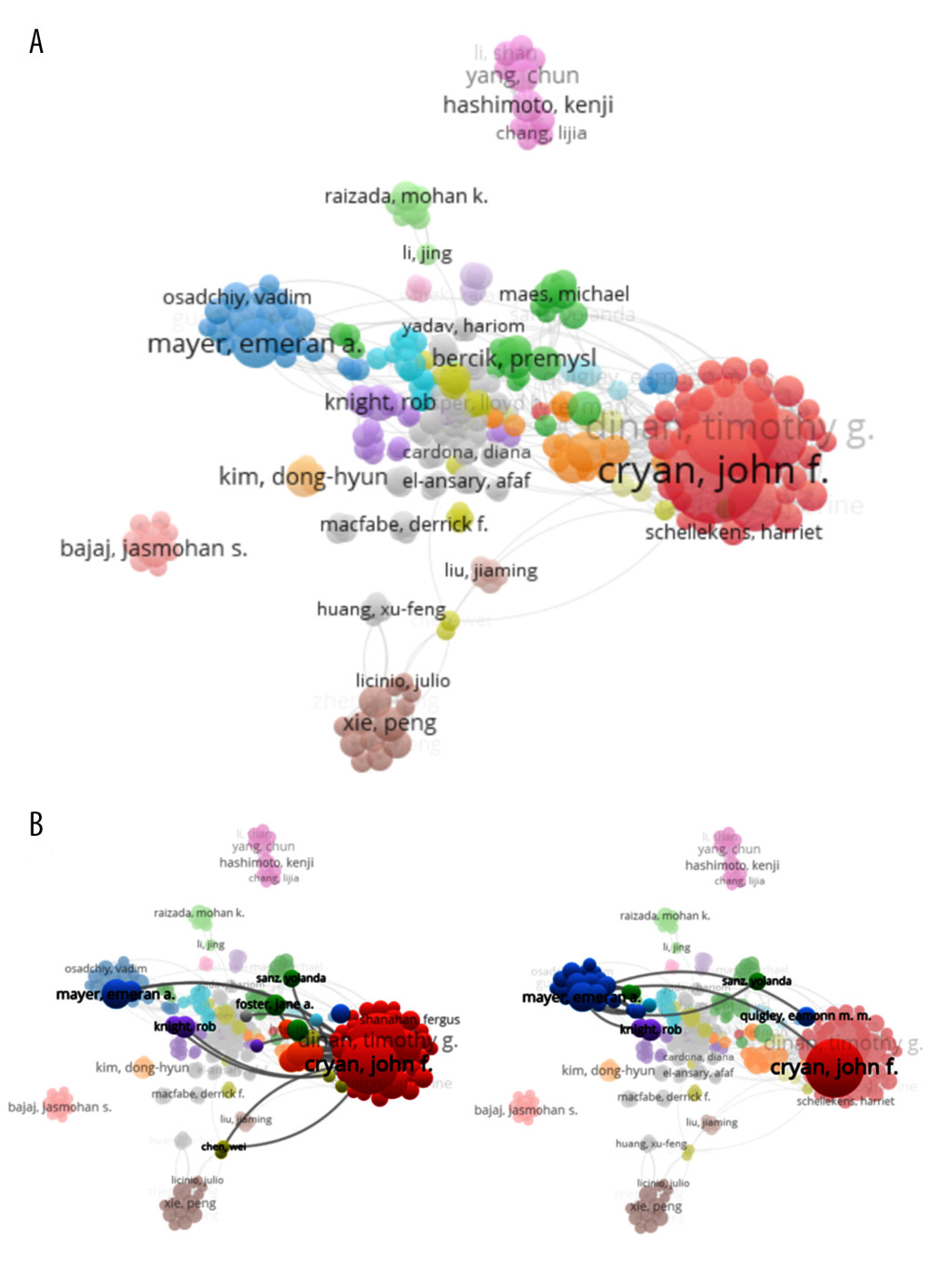 Figure 4. Co-authorship analysis of authors. (A) Map of the cooperation between 338 authors by the VOSviewer. (B) Analysis of the authors who cooperated with John F. Cryan or Emeran A. Mayer. Different colors indicate clusters of collaboration between authors, the size of the circle indicates citations to the publication, and the thickness of the line indicates the size of collaboration. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands).
Figure 4. Co-authorship analysis of authors. (A) Map of the cooperation between 338 authors by the VOSviewer. (B) Analysis of the authors who cooperated with John F. Cryan or Emeran A. Mayer. Different colors indicate clusters of collaboration between authors, the size of the circle indicates citations to the publication, and the thickness of the line indicates the size of collaboration. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). 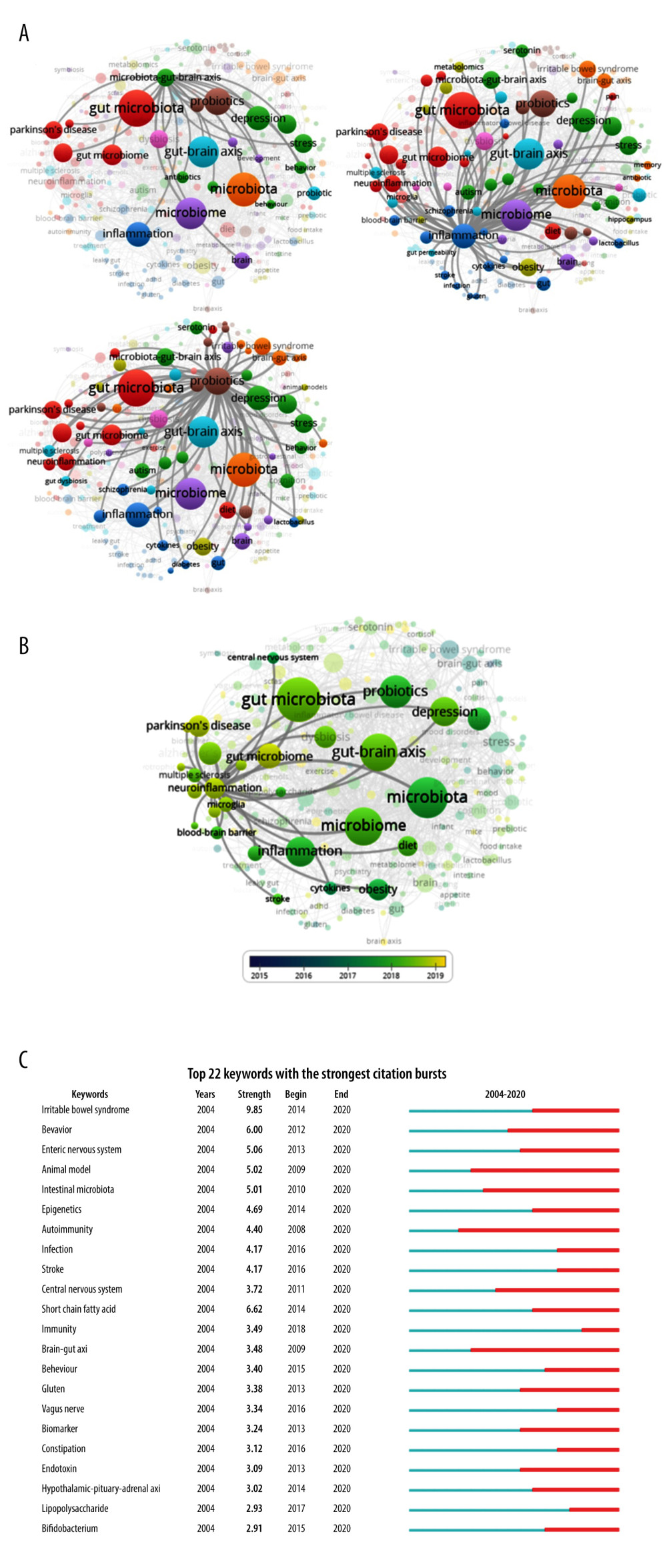 Figure 5. Co-occurrence analysis of author keywords. (A) Map of the relevant author keywords of microbiota-gut-brain-axis, inflammation, or probiotics. (B) The average published year shows the relationship of neuroinflammation between other author keywords. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). (C) Top 20 keywords with the strongest citation bursts by Citespace (5.7. R3 versions; College of Information Science and Technology, Leisel University, USA). ɣ: 1.0; minimum duration: 2.
Figure 5. Co-occurrence analysis of author keywords. (A) Map of the relevant author keywords of microbiota-gut-brain-axis, inflammation, or probiotics. (B) The average published year shows the relationship of neuroinflammation between other author keywords. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). (C) Top 20 keywords with the strongest citation bursts by Citespace (5.7. R3 versions; College of Information Science and Technology, Leisel University, USA). ɣ: 1.0; minimum duration: 2. Tables
Table 1. The top 10 most productive countries/regions on the microbiome-gut-brain axis.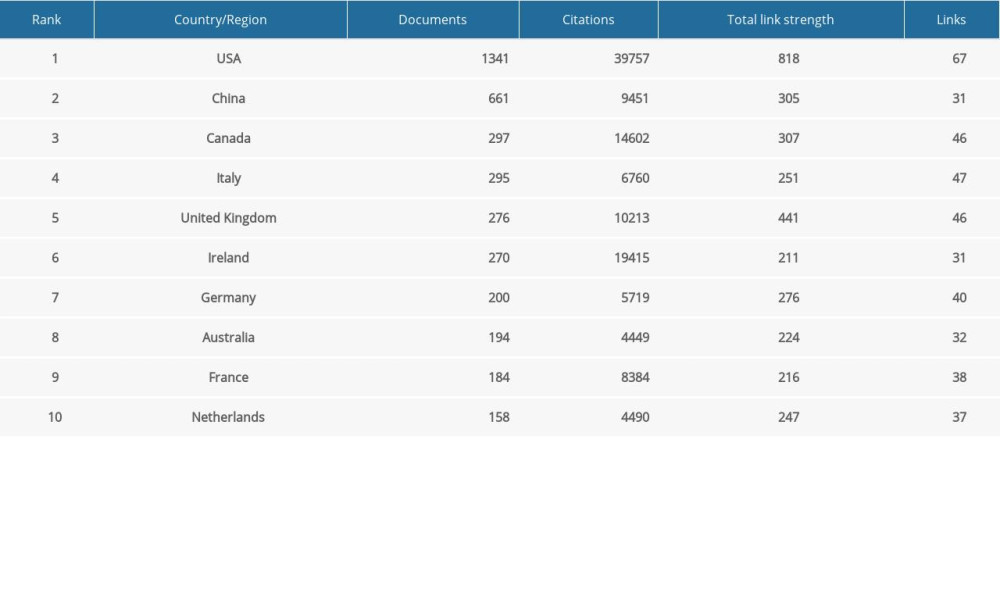 Table 2. The top 10 most productive organizations.
Table 2. The top 10 most productive organizations.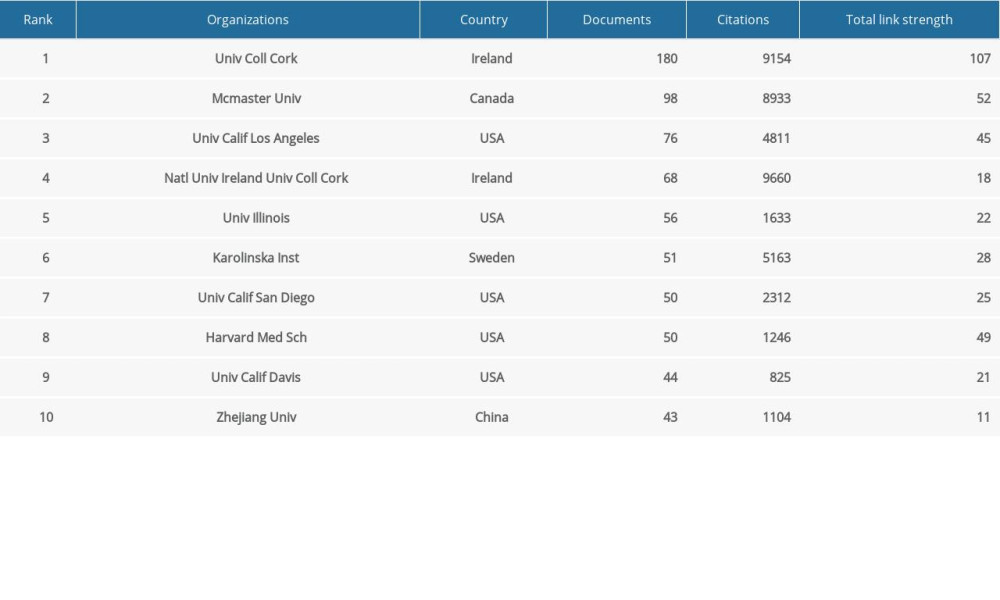 Table 3. The top 15 journals with largest number of publications.
Table 3. The top 15 journals with largest number of publications.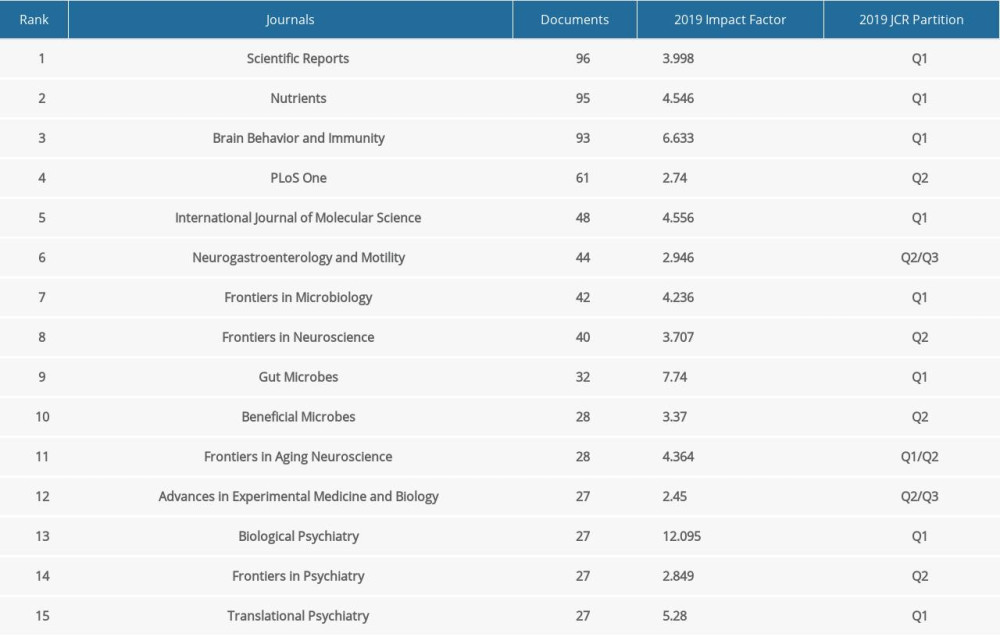 Table 4. Core-authors on the microbiome-gut-brain axis.
Table 4. Core-authors on the microbiome-gut-brain axis.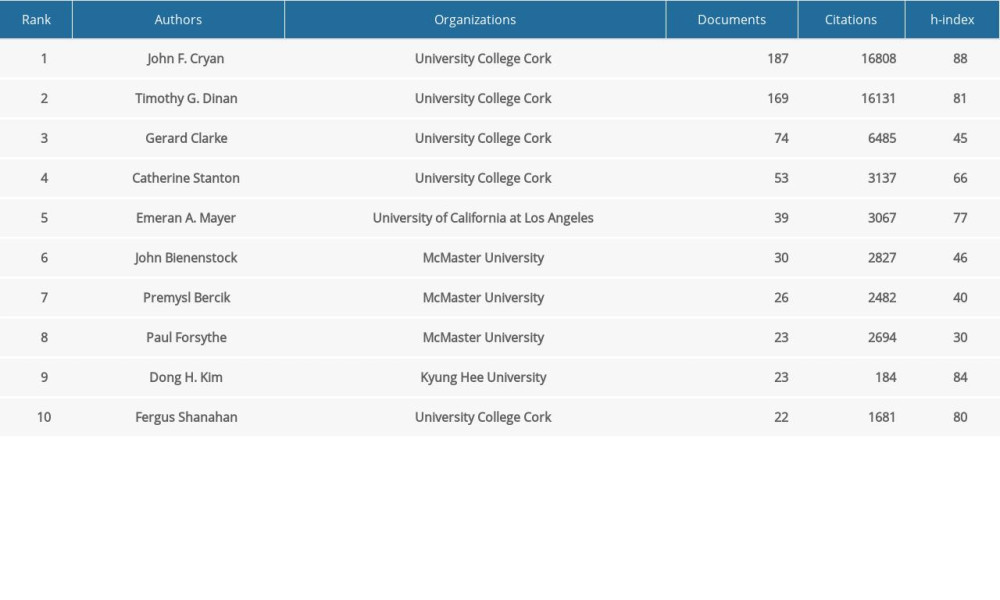 Table 5. Top 10 co-citation analysis of documents on the microbiome-gut-brain axis.
Table 5. Top 10 co-citation analysis of documents on the microbiome-gut-brain axis.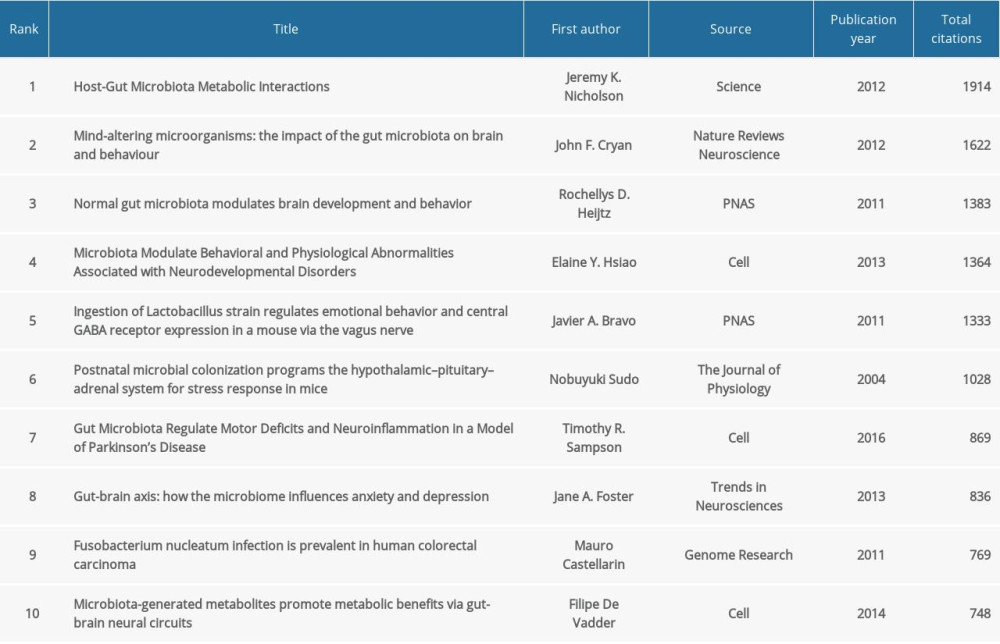
References
1. Barko PC, McMichael MA, Swanson KS, Williams DA, The gastrointestinal microbiome: A review: J Vet Intern Med, 2018; 32; 9-25
2. Parker A, Fonseca S, Carding SR, Gut microbes and metabolites as modulators of blood-brain barrier integrity and brain health: Gut Microbes, 2020; 11; 135-57
3. Dinan TG, Cryan JF, Regulation of the stress response by the gut microbiota: Implications for psychoneuroendocrinology: Psychoneuroendocrinology, 2012; 37; 1369-78
4. Mailhe M, Ricaboni D, Vitton V, Repertoire of the gut microbiota from stomach to colon using culturomics and next-generation sequencing: BMC Microbiol, 2018; 18; 157
5. Lepage P, Leclerc MC, Joossens M, A metagenomic insight into our gut’s microbiome: Gut, 2013; 62; 46-58
6. Kishikawa T, Maeda Y, Nii T, Metagenome-wide association study of gut microbiome revealed novel aetiology of rheumatoid arthritis in the Japanese population: Ann Rheum Dis, 2020; 79; 103-11
7. Schmidt TSB, Raes J, Bork P, The human gut microbiome: From association to modulation: Cell, 2018; 172; 1198-215
8. Heintz-Buschart A, Wilmes P, Human gut microbiome: function matters: Trends Microbiol, 2018; 26; 563-74
9. Laudadio I, Fulci V, Palone F, Quantitative assessment of shotgun metagenomics and 16S rDNA amplicon sequencing in the study of human gut microbiome: OMICS, 2018; 22; 248-54
10. Liu R, Hong J, Xu X, Gut microbiome and serum metabolome alterations in obesity and after weight-loss intervention: Nat Med, 2017; 23; 859-68
11. Kishikawa T, Ogawa K, Motooka D, A metagenome-wide association study of gut microbiome in patients with multiple sclerosis revealed novel disease pathology: Front Cell Infect Microbiol, 2020; 10; 585973
12. Altveş S, Yildiz HK, Vural HC, Interaction of the microbiota with the human body in health and diseases: Biosci Microbiota Food Health, 2020; 39; 23-32
13. Capuco A, Urits I, Hasoon J, Current perspectives on gut microbiome dysbiosis and depression: Adv Ther, 2020; 37; 1328-46
14. Fung TC, The microbiota-immune axis as a central mediator of gut-brain communication: Neurobiol Dis, 2020; 136; 104714
15. Cryan JF, O’Riordan KJ, Cowan CSM, The microbiota-gut-brain axis: Physiol Rev, 2019; 99; 1877-2013
16. Cryan JF, O’Riordan KJ, Sandhu K, The gut microbiome in neurological disorders: Lancet Neurol, 2020; 19; 179-94
17. Benakis C, Martin-Gallausiaux C, Trezzi JP, The microbiome-gut-brain axis in acute and chronic brain diseases: Curr Opin Neurobiol, 2020; 61; 1-9
18. Ma EL, Smith AD, Desai N, Bidirectional brain-gut interactions and chronic pathological changes after traumatic brain injury in mice: Brain Behav Immun, 2017; 66; 56-69
19. Nicholson SE, Watts LT, Burmeister DM, Moderate traumatic brain injury alters the gastrointestinal microbiome in a time-dependent manner: Shock, 2019; 52; 240-48
20. Sharon G, Sampson TR, Geschwind DH, The central nervous system and the gut microbiome: Cell, 2016; 167; 915-32
21. Farzi A, Fröhlich EE, Holzer P, Gut microbiota and the neuroendocrine system: Neurotherapeutics, 2018; 15; 5-22
22. Rothhammer V, Borucki DM, Tjon EC, Microglial control of astrocytes in response to microbial metabolites: Nature, 2018; 557; 724-28
23. Tankou SK, Regev K, Healy BC, A probiotic modulates the microbiome and immunity in multiple sclerosis: Ann Neurol, 2018; 83; 1147-61
24. Sharon G, Cruz NJ, Kang DW, Human gut microbiota from autism spectrum disorder promote behavioral symptoms in mice: Cell, 2019; 177; 1600-18
25. Arulsamy A, Tan QY, Balasubramaniam V, Gut microbiota and epilepsy: A systematic review on their relationship and possible therapeutics: ACS Chem Neurosci, 2020; 11; 3488-98
26. Bear TLK, Dalziel JE, Coad J, The Role of the gut microbiota in dietary interventions for depression and anxiety: Adv Nutr, 2020; 11; 890-907
27. Chen Y, Li Y, Guo L, Bibliometric analysis of the inflammasome and pyroptosis in brain: Front Pharmacol, 2021; 11; 626502
28. Sampson TR, Debelius JW, Thron T, Gut microbiota regulate motor deficits and neuroinflammation in a model of Parkinson’s disease: Cell, 2016; 167; 1469-80
29. Cryan JF, Dinan TG, Mind-altering microorganisms: The impact of the gut microbiota on brain and behaviour: Nat Rev Neurosci, 2012; 13; 701-12
30. Diaz Heijtz R, Wang S, Anuar F, Normal gut microbiota modulates brain development and behavior: Proc Natl Acad Sci USA, 2011; 108; 3047-52
31. Hsiao EY, McBride SW, Hsien S, Microbiota modulate behavioral and physiological abnormalities associated with neurodevelopmental disorders: Cell, 2013; 155; 1451-63
32. Nicholson JK, Holmes E, Kinross J, Host-gut microbiota metabolic interactions: Science, 2012; 336; 1262-67
33. Stephenson J, Nutma E, van der Valk P, Inflammation in CNS neurodegenerative diseases: Immunology, 2018; 154; 204-19
34. Lahooti B, Chhibber T, Bagchi S, Therapeutic role of inflammasome inhibitors in neurodegenerative disorders: Brain Behav Immun, 2021; 91; 771-83
35. D’Mello C, Swain MG, Immune-to-brain communication pathways in inflammation-associated sickness and depression: Curr Top Behav Neurosci, 2017; 31; 73-94
36. Wang YF, Zheng LJ, Liu Y, The gut microbiota-inflammation-brain axis in end-stage renal disease: Perspectives from default mode network: Theranostics, 2019; 9; 8171-81
37. Serra D, Almeida LM, Dinis TCP, The impact of chronic intestinal inflammation on brain disorders: The microbiota-gut-brain axis: Mol Neurobiol, 2019; 56; 6941-51
38. Bassett DS, Cullen KE, Eickhoff SB, Reflections on the past two decades of neuroscience: Nat Rev Neurosci, 2020; 21; 524-34
39. Abdel-Haq R, Schlachetzki JCM, Glass CK, Mazmanian SK, Microbiome-microglia connections via the gut-brain axis: J Exp Med, 2019; 216; 41-59
40. Holmqvist S, Chutna O, Bousset L, Direct evidence of Parkinson pathology spread from the gastrointestinal tract to the brain in rats: Acta Neuropathol, 2014; 128; 805-20
41. Houser MC, Tansey MG, The gut-brain axis: is intestinal inflammation a silent driver of Parkinson’s disease pathogenesis?: NPJ Parkinsons Dis, 2017; 3; 3
42. Pajares M, Rojo IA, Manda G, Inflammation in Parkinson’s disease: Mechanisms and therapeutic implications: Cells, 2020; 9; 1687
43. Scheperjans F, Aho V, Pereira PA, Gut microbiota are related to Parkinson’s disease and clinical phenotype: Mov Disord, 2015; 30; 350-58
44. Sochocka M, Donskow-Łysoniewska K, Diniz BS, The Gut microbiome alterations and inflammation-driven pathogenesis of Alzheimer’s disease – a critical review: Mol Neurobiol, 2019; 56; 1841-51
45. Giau VV, Wu SY, Jamerlan A, Gut microbiota and their neuroinflammatory implications in Alzheimer’s disease: Nutrients, 2018; 10; 1765
46. Jiang C, Li G, Huang P, The gut microbiota and Alzheimer’s disease: J Alzheimers Dis, 2017; 58; 1-15
47. Abraham D, Feher J, Scuderi GL, Exercise and probiotics attenuate the development of Alzheimer’s disease in transgenic mice: Role of microbiome: Exp Gerontol, 2019; 115; 122-31
48. Sun J, Xu J, Yang B, Effect of clostridium butyricum against microglia-mediated neuroinflammation in Alzheimer’s disease via regulating gut microbiota and metabolites butyrate: Mol Nutr Food Res, 2020; 64; e1900636
49. Den H, Dong X, Chen M, Zou Z, Efficacy of probiotics on cognition, and biomarkers of inflammation and oxidative stress in adults with Alzheimer’s disease or mild cognitive impairment – a meta-analysis of randomized controlled trials: Aging (Albany NY), 2020; 12; 4010-39
50. Dinan TG, Cryan JF, The microbiome-gut-brain axis in health and disease: Gastroenterol Clin North Am, 2017; 46; 77-89
51. Carlessi AS, Borba LA, Zugno AI, Gut microbiota-brain axis in depression: The role of neuroinflammation: Eur J Neurosci, 2019; 53; 222-35
52. Howard BM, Kornblith LZ, Christie SA, Characterizing the gut microbiome in trauma: Significant changes in microbial diversity occur early after severe injury: Trauma Surg Acute Care Open, 2017; 2; e000108
53. Urban RJ, Pyles RB, Stewart CJ, Altered fecal microbiome years after traumatic brain injury: J Neurotrauma, 2020; 37; 1037-51
54. Sundman MH, Chen NK, Subbian V, The bidirectional gut-brain-microbiota axis as a potential nexus between traumatic brain injury, inflammation, and disease: Brain Behav Immun, 2017; 66; 31-44
55. Olson CA, Vuong HE, Yano JM, The gut microbiota mediates the anti-seizure effects of the ketogenic diet: Cell, 2018; 173; 1728-41
56. Plovier H, Everard A, Druart C, A purified membrane protein from Akkermansia muciniphila or the pasteurized bacterium improves metabolism in obese and diabetic mice: Nat Med, 2017; 23; 107-13
57. Li J, Lin S, Vanhoutte PM: Circulation, 2016; 133; 2434-46
58. Huck O, Mulhall H, Rubin G, Akkermansia muciniphila reduces Porphyromonas gingivalis-induced inflammation and periodontal bone destruction: J Clin Periodontol, 2020; 47; 202-12
59. Wang L, Tang L, Feng Y, A purified membrane protein from Akkermansia muciniphila or the pasteurised bacterium blunts colitis associated tumourigenesis by modulation of CD8(+) T cells in mice: Gut, 2020; 69; 1988-97
Figures
 Figure 1. Distribution of publications of the microbiome-gut-brain axis (MGBA) from 2004 to 2020, by the GraphPad Prism (version 5.0; University of California San Diego, San Diego, CA, USA).
Figure 1. Distribution of publications of the microbiome-gut-brain axis (MGBA) from 2004 to 2020, by the GraphPad Prism (version 5.0; University of California San Diego, San Diego, CA, USA). Figure 2. The documents on the microbiome-gut-brain axis (MGBA) in different countries/regions. (A) Map of the cooperation between 34 countries by the VOSviewer. (B) The cooperation between the United States and Ireland. Different colors indicate clusters of collaboration between countries, the size of the circle indicates citations to the publication, and the thickness of the line indicates the extent of collaboration. The network visualization was performed by VOSviewer (version 1.6.15; Centre for Science and Technology Studies, Leiden University, the Netherlands).
Figure 2. The documents on the microbiome-gut-brain axis (MGBA) in different countries/regions. (A) Map of the cooperation between 34 countries by the VOSviewer. (B) The cooperation between the United States and Ireland. Different colors indicate clusters of collaboration between countries, the size of the circle indicates citations to the publication, and the thickness of the line indicates the extent of collaboration. The network visualization was performed by VOSviewer (version 1.6.15; Centre for Science and Technology Studies, Leiden University, the Netherlands). Figure 3. Co-author analysis of organizations. (A) The co-authorship of organizations showed the collaboration of University College Cork and Zhejiang Univ. (B) The average published year showed the recent active organization, Central South University. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands).
Figure 3. Co-author analysis of organizations. (A) The co-authorship of organizations showed the collaboration of University College Cork and Zhejiang Univ. (B) The average published year showed the recent active organization, Central South University. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). Figure 4. Co-authorship analysis of authors. (A) Map of the cooperation between 338 authors by the VOSviewer. (B) Analysis of the authors who cooperated with John F. Cryan or Emeran A. Mayer. Different colors indicate clusters of collaboration between authors, the size of the circle indicates citations to the publication, and the thickness of the line indicates the size of collaboration. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands).
Figure 4. Co-authorship analysis of authors. (A) Map of the cooperation between 338 authors by the VOSviewer. (B) Analysis of the authors who cooperated with John F. Cryan or Emeran A. Mayer. Different colors indicate clusters of collaboration between authors, the size of the circle indicates citations to the publication, and the thickness of the line indicates the size of collaboration. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). Figure 5. Co-occurrence analysis of author keywords. (A) Map of the relevant author keywords of microbiota-gut-brain-axis, inflammation, or probiotics. (B) The average published year shows the relationship of neuroinflammation between other author keywords. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). (C) Top 20 keywords with the strongest citation bursts by Citespace (5.7. R3 versions; College of Information Science and Technology, Leisel University, USA). ɣ: 1.0; minimum duration: 2.
Figure 5. Co-occurrence analysis of author keywords. (A) Map of the relevant author keywords of microbiota-gut-brain-axis, inflammation, or probiotics. (B) The average published year shows the relationship of neuroinflammation between other author keywords. The color shows the average published year. The network visualization was performed by VOSviewer (1.6.15 versions; Centre for Science and Technology Studies, Leiden University, the Netherlands). (C) Top 20 keywords with the strongest citation bursts by Citespace (5.7. R3 versions; College of Information Science and Technology, Leisel University, USA). ɣ: 1.0; minimum duration: 2. Tables
 Table 1. The top 10 most productive countries/regions on the microbiome-gut-brain axis.
Table 1. The top 10 most productive countries/regions on the microbiome-gut-brain axis. Table 2. The top 10 most productive organizations.
Table 2. The top 10 most productive organizations. Table 3. The top 15 journals with largest number of publications.
Table 3. The top 15 journals with largest number of publications. Table 4. Core-authors on the microbiome-gut-brain axis.
Table 4. Core-authors on the microbiome-gut-brain axis. Table 5. Top 10 co-citation analysis of documents on the microbiome-gut-brain axis.
Table 5. Top 10 co-citation analysis of documents on the microbiome-gut-brain axis. Table 1. The top 10 most productive countries/regions on the microbiome-gut-brain axis.
Table 1. The top 10 most productive countries/regions on the microbiome-gut-brain axis. Table 2. The top 10 most productive organizations.
Table 2. The top 10 most productive organizations. Table 3. The top 15 journals with largest number of publications.
Table 3. The top 15 journals with largest number of publications. Table 4. Core-authors on the microbiome-gut-brain axis.
Table 4. Core-authors on the microbiome-gut-brain axis. Table 5. Top 10 co-citation analysis of documents on the microbiome-gut-brain axis.
Table 5. Top 10 co-citation analysis of documents on the microbiome-gut-brain axis. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








