04 February 2023: Database Analysis
A National Registry-Based Epidemiological Study to Evaluate 395 646 Patients Hospitalized Due to Eye Diseases in Poland in 2019
Agnieszka Kamińska1ABCDEF*, Jarosław Pinkas2DE, Paweł Goryński3BE, Mateusz JankowskiDOI: 10.12659/MSM.939351
Med Sci Monit 2023; 29:e939351
Abstract
BACKGROUND: The Nationwide General Hospital Morbidity Study Registry collects demographic, health, and medical data on patients hospitalized throughout Poland, and acts as a registry for epidemiological, public health, and hospital administrative studies. This epidemiological national registry-based study aimed to evaluate the characteristics of 395 646 patients hospitalized due to eye diseases in Poland in 2019.
MATERIAL AND METHODS: This study is a retrospective nationwide registry-based analysis. Data on all patients hospitalized due to eye diseases in 2019 were obtained from the Nationwide General Hospital Morbidity Study Registry. Demographic characteristics of patients hospitalized due to eye diseases as well as the hospitalization course were analyzed using descriptive epidemiology tools.
RESULTS: Disorders of the lens accounted for 68.6% of all hospital admissions, and disorders of the choroid and retina were the second most common (13.9%) cause of hospital admission due to eye diseases in 2019. Over three-quarters of hospital admissions (77.4%) lasted less than 24 h, and 86.8% were scheduled admissions. Most of the patients hospitalized due to eye diseases were females (59.9%) and over 70% lived in urban areas. There were regional differences in the hospital admissions rate per 100 000 inhabitants. According to the data presented in the registry, less than one-third of patients had comorbidities.
CONCLUSIONS: Hospital ophthalmological care in Poland is based mainly on planned hospitalizations lasting less than 24 h and related to ophthalmological surgery. Data on the comorbidity of ophthalmologic patients suggest that ophthalmologists do not pay enough attention to identifying and recording the patient’s health status.
Keywords: Cataract, Eye Diseases, Hospitalization, Macular Degeneration, Poland, Registries, Female, Humans, Male
Background
According to World Health Organization (WHO) estimates, over 2 billion people globally have vision impairment, of which 1 billion could have been prevented or have yet to be addressed [1,2]. The leading causes of vision impairment are uncorrected refractive errors or age-related eye diseases, including cataracts, age-related macular degeneration (AMD), glaucoma, and diabetic retinopathy [1–3]. A substantial variation in the causes of vision impairment within countries was observed. The proportion of vision impairment attributable to cataracts is higher in low- or middle-income countries, while glaucoma or AMD is more common in high-income countries [2,4]
Most cases of vision impairment occur in people aged 50 years and older [2,5]. Demographic changes, aging of the population (including longer life expectancy), and lifestyle changes are the most important factors that will lead to an increased incidence of vision impairment in the next decade [5,6]. Age-related changes in the ocular surface and corneal tissues affect vision and cause major eye diseases [7]. Lower-quality foods, low physical activity levels, and tobacco use are the most important lifestyle factors associated with increased risk for visual impairment [6]. Decreased visual acuity can significantly affect the quality of life in patients with eye diseases [8,9]. Moreover, major eye diseases like cataracts, AMD, and diabetic retinopathy are associated with increased mortality risk [10]. Vision impairment can also lead to functional disability, reduced social interaction, and increased risk of falls, accidents, and fractures [6,11,12]. Vision impairment also affects the individual’s workforce participation and productivity [13]. The global financial burden due to productivity losses from vision impairment is estimated at 411 billion US dollars [13].
Due to the social burden of vision impartments and its economic consequences, numerous strategies to address eye conditions have been implemented globally [14], but most focused on providing timely access to healthcare and eye care services [2,14]. A significant proportion of refractive error can be corrected with eyeglasses or contact lenses [2–4]. However, age-related eye disease often requires eye surgery. Cataract surgery is one of the most cost-effective healthcare interventions [15].
Providing access to eye health services is crucial to reduce the burden of visual impairment. However, the availability of eye care services differs among countries [16]. The upcoming demographic and social changes will increase demands for eye health services [4,5,14]. Low- and middle-income countries may learn from high-income countries how to develop eye health services. Moreover, differences in the organization of health care in particular countries may also affect eye health services utilization [17].
Poland is an example of a European Union (EU) country that moved from a being a middle- to a high-income country in less than 15 years [18]. A relatively large national income increase leads to social changes and a life expectancy increase [19]. In the Polish health system, mandatory health insurance provides access to a variety of health care services [20]. According to the data of the Supreme Medical Council, as of 30 November 2022 a total number of 4842 ophthalmologists provided medical services in Poland [21]. Eye health services are mostly provided in outpatient clinics [14,17]. However, eye surgery (eg, cataract surgery) is provided in dedicated hospital wards (ophthalmology departments) or single-profile ophthalmology hospitals [15,17]. Patients requiring eye surgery are admitted to the hospital, usually for less than 24 h, and are discharged the same day [22]. Regular monitoring of health services is necessary to evaluate and improve eye health care [23]. Moreover, characteristics of hospital eye care in countries such as Poland can be the basis for comparisons for countries with a similar demographic situation and can be the basis for healthcare resource planning, especially in the face of challenges resulting from population aging [24]. Data from the United States [25], England, and Wales [26] showed that national hospital registries may be used for epidemiological analyses of eye-related hospital admissions. In Poland, data on hospitalizations are collected by the Nationwide General Hospital Morbidity Study Registry [27], but there has been a lack of nationwide data on hospitalization due to eye diseases in Poland.
Therefore, this epidemiological national registry-based study aimed to evaluate the characteristics of 395 646 patients hospitalized due to eye diseases in Poland in 2019.
Material and Methods
ETHICS:
The study protocol was reviewed and approved by the Ethics Committee at the Centre of Postgraduate Medical Education (Warsaw, Poland), decision number 154/2022, November 16, 2022. This was a retrospective analysis of the Nationwide General Hospital Morbidity Study Registry, so datasets were anonymous and patient consent was waived.
DATA SOURCE:
This study was a retrospective nationwide registry-based analysis. Data on patients hospitalized due to eye diseases were obtained from the Nationwide General Hospital Morbidity Study Registry [27], managed by the Department of Population Health Monitoring and Analysis, National Institute of Public Health – National Institute of Hygiene (Warsaw, Poland). Data were gathered under the official Statistical Research Program of Public Statistics [28]. All hospitals (both public and private facilities) operating in Poland (with some exceptions for psychiatric departments) are legally obligated to report data on hospitalizations. Data are reported using a standard template ensuring patients’ anonymity [27]. Data are verified by trained public health specialists tasked with managing the registry, and are aggregated and analyzed for purposes such as healthcare planning and public statistics.
DATA REPORTING METHODS:
Data on patients hospitalized in Poland are reported using a template covering the following range of data: (1) sex (male/female); (2) age; (3) place of residence; (4) type of hospital and location; (5) cause of hospitalization; (6) co-existing diseases (comorbidities); (7) duration of hospitalization and detailed information on the type of wards and potential transfer to another ward during the hospitalization; (8) type of admission (emergency/scheduled); (9) medical services provided during the hospitalization; and (10) hospitalization outcome (death/discharge/transfer for further treatment).
Data on medical conditions and diagnoses are reported by trained physicians using the 10th revision of the International Statistical Classification of Diseases and Related Health Problems ICD-10 classification (ICD-10 codes) [29].
Patients hospitalized due to eye diseases were identified using ICD-10 codes: H00–H59 [29]. All the patients with primary diagnosis (cause of hospitalization) reported by a doctor using codes H00–H59 were included in this analysis. Based on the primary diagnosis, patients were assigned into one of the following groups of eye diseases: H00–H05 – disorders of the eyelid, lacrimal system, and orbit; H10–H11 – disorders of conjunctiva; H15–H22 – disorders of sclera, cornea, iris and ciliary body; H25–H28 – disorders of the lens; H30–H36 – disorders of choroid and retina; H40–H42 – glaucoma; H43–H44 – disorders of vitreous body and globe; H46–H47 – disorders of the optic nerve and visual pathways; H49–H52 – disorders of ocular muscles, binocular movement, accommodation, and refraction; H53–H54 – visual disturbances and blindness; and H55–H59 – other disorders of eye and adnexa [29].
The following ICD-10 codes were used to identify patients with selected eye diseases: (1) H25.0–H25.9 – age-related nuclear cataract; H26.2 – complicated cataract; and H35.3 – age-related macular degeneration (AMD) [29].
Data from the Nationwide General Hospital Morbidity Study Registry were previously used for nationwide analyses on COVID-19 and diabetes, published in peer-reviewed journals [30,31].
Data on the demographic characteristics of the Polish population were obtained from an official demographic registry regularly published by Statistics Poland [32].
STATISTICAL ANALYSIS:
The data were analyzed with MS Excel (USA: Microsoft Corporation, Redmond, WA) and SPSS v.28 (USA: IBM, Armonk, NY). Epidemiological characteristics of patients hospitalized due to eye diseases were presented using descriptive statistics. Hospital admissions per 100 000 inhabitants were calculated based on the demographic data (sex, age, place of residence – administrative region) from Statistics Poland. The following age groups were included in the analysis: 0–17 (children), 18–29; 30–39; 40–49; 50–59; 60–69; 70–79; and 80 and over years. Epidemiological characteristics of patients hospitalized due to eye diseases were provided separately for a major group of diseases based on ICD-10 codes, as well as for the most common causes of hospitalization (cataract and AMD).
Results
HOSPITALIZATIONS DUE TO EYE DISEASES BETWEEN JANUARY AND DECEMBER 2019 IN POLAND:
In 2019, a total of 395 646 hospital admissions due to eye conditions and diseases were reported in the Nationwide General Hospital Morbidity Study Registry. The highest numbers of hospitalizations due to eye diseases was reported in October (38 507) and May (35 650), while the lowest numbers were reported in February (29 839) and (27 629) December (Figure 1). There were regional differences in the hospital admissions rate per 100 000 inhabitants (Table 1). Out of 16 administrative regions (voivodships) in Poland, the highest hospital admissions rate per 100 000 inhabitants was in Lower Silesia (1331.6 hospital admissions per 100 000 inhabitants) and Silesia region (1322.9 hospital admissions per 100 000 inhabitants), and the lowest were in Pomerania (756.7 hospital admissions per 100 000 inhabitants) and Warmia-Masuria (740.7 hospital admissions per 100 000 inhabitants) (Table 1).
CAUSES OF HOSPITAL ADMISSIONS DUE TO DISEASES OF THE EYE AND ADNEXA (H00–H59):
The most common causes for hospital admissions were: other age-related cataracts (code H25.8; (n=130 624; 33.0%), complicated cataracts (code H26.2; n=56 892; 14.4%), age-related nuclear cataract (code H25.1; n=42 519; 10.7%); age-related incipient cataract (code H25.0; n=18 318; 4.6%); degeneration of macula and posterior pole (code H35.3; n=23 677; 6.0%); and other specified retinal disorders (code H35.8; n=12 785; n=3.2%). Disorders of the lens (codes H25–H28) accounted for 68.6% of all hospital admissions due to eye diseases in 2019 in Poland (Table 2). Disorders of the choroid and retina (H30–H36) were the second most common (13.9% of total hospitalizations due to eye diseases) cause of hospital admission due to eye diseases in 2019. Hospital admissions rate per 100 000 inhabitants varied from 707.8 for disorders of the lens to 5.3 for disorders of the optic nerve and visual pathways (Table 2).
Over three-quarters of hospital admissions (77.4%) were 1-day admission (less than 24 h), and 86.8% were scheduled admissions (Table 3). Most of the patients hospitalized due to eye diseases in Poland were females (59.9%) and over 70% lived in urban areas. There were differences in duration of hospitalization, type of admissions, sex, and place of residence by cause of admission. Over 90% of patients hospitalized due to disorders of conjunctiva were hospitalized for less than 24 h, but only 14.7% of patients hospitalized due to disorders of the optic nerve and visual pathways were hospitalized for less than 24 h (Table 3). Over 80% of patients hospitalized due to disorders of the conjunctiva or disorders of the sclera, cornea, iris, and the ciliary body were admitted in emergency mode (Table 3). Out of 11 different groups of eye diseases, most of the patients hospitalized due to disorders of the conjunctiva (52.0%), disorders of the sclera, cornea, iris, and ciliary body (53.3%), disorders of the vitreous body and globe (51.5%), and other disorders of eye and adnexa (56.3%; code H55–H59) were males (Table 3). Regardless of the cause of hospital admission, most of the patients lived in urban areas.
Out of 395 646 hospital admissions due to eye diseases in Poland, only 4.1% were among children (Table 4). Among adults hospitalized due to eye diseases, the hospitalization rate per 100 000 inhabitants increased with age – the hospitalization rate significantly increased after 50 years of age, and the highest hospitalization rate was observed among adults aged 70 years and over (Table 4).
EPIDEMIOLOGICAL CHARACTERISTICS OF HOSPITAL ADMISSIONS DUE TO CATARACT:
Age-related nuclear cataract (H25.0–H25.9) was the most common cause of hospitalization, with 198 896 hospital admissions reported in 2019 (Table 5). Almost two-thirds of patients hospitalized due to age-related nuclear cataracts were females (63.8%). One-quarter of patients were aged 60–69 years, more than 40% were aged 70–79 years, and 28.8% were aged 80 years or over (Table 5). Over 95% of hospitalizations due to age-related nuclear cataracts were scheduled admissions and 86.6% of hospitalizations lasted less than 24 h. Over 90% of patients stayed in the ophthalmology department. According to the data presented in the registry, only 28.6% of patients had comorbidities (Table 5).
The second most common cause of hospital admissions was complicated cataracts (H26.2), with 56 892 hospital admissions in 2019 (Table 5). Epidemiological characteristics of patients hospitalized due to complicated cataracts were comparable to those hospitalized due to age-related nuclear cataracts, except for the presence of comorbidities, which was 2 times higher among those with complicated cataracts (61.8% vs 28.6%). Moreover, 78.1% of patients hospitalized due to complicated cataracts were referred for further treatment in outpatient clinics compared to 70.9% of patients with age-related nuclear cataracts (Table 5).
EPIDEMIOLOGICAL CHARACTERISTICS OF HOSPITAL ADMISSIONS DUE TO AGE-RELATED MACULAR DEGENERATION (AMD):
The third most common cause of hospital admissions was degeneration of the macula and posterior pole, mostly used as a medical code for age-related macular degeneration (AMD). In 2019, a total of 23 677 hospital admissions due to AMD were reported (Table 6). More than half of patients hospitalized due to AMD were females (58.3%) and almost 90% of hospitalized patients were aged 60 years and over. Three-quarters of patients hospitalized due to AMD lived in urban areas. Over 90% of hospitalizations due to AMD were scheduled admissions, mostly to the ophthalmology department (96.2%). According to the data presented in the registry, only 29.0% of patients had comorbidities (Table 6).
Discussion
This registry-based study provides a comprehensive summary and analysis of epidemiological characteristics of 395 646 patients hospitalized due to eye diseases in Poland. Major causes of hospital admissions due to eye diseases were identified and the demographic characteristics of patients were provided. Over 60% of hospital admissions due to eye diseases were attributed to cataract surgery. A detailed analysis of the hospitalization course, including its duration and type of admission, was described in this study. This study also revealed that there is an urgent need to improve the quality of data reporting (especially related to patients’ comorbidities) by physicians providing 1-day surgery medical services.
Public registries may provide a comprehensive overview of the medical services offered by health systems in particular countries. In Poland, eye health services are provided by outpatient clinics as well as ophthalmologic wards or single-profile ophthalmologic hospitals [33]. Most patients with vision impairment visit outpatient clinics, but those with acute injuries or chronic age-related eye diseases may require surgery. According to Polish law, ophthalmologic surgery is mostly provided in hospitals, but within 1-day surgery department/hospitalization. For example, a patient is admitted to the hospital in the morning and discharged home several hours after the surgery (mostly in the afternoon of the same day). However, in other countries ophthalmologic surgery may be provided on an outpatient basis, depending on the local health system.
Public registries were used for epidemiological analyses on hospitalizations due to eye diseases in England and Wales [26] as well as in the United States [25]. Between 1999 and 2019, the hospital admission rate for diseases of the eye and adnexa increased in England and Wales increased by 73.8% [26]. The hospital admission rate due to eye diseases increased by 91.2% among males and 63.2% among females [26]. In a study from England and Wales, the most common causes of hospitalization due to eye diseases were disorders of the lens (62.3%), disorders of the choroid and retina (14.2%), and disorders of the eyelid, lacrimal system, and orbit (11.5%) [26]. Similar epidemiological trends were observed in this study. In 2019 in Poland, 68.6% of hospital admissions due to eye diseases were caused by disorders of the lens and 13.9% were caused by disorders of the choroid and retina. However, only 4.4% of hospital admissions were caused by disorders of the eyelid, lacrimal system, and orbit, which is 2.5 times lower than in England and Wales [26]. Between 2006 and 2011, a total of 11.9 million emergency department visits for eye problems were reported in the United States [25], of which 44.3% were nonemergent problems [25]. Female sex, lower income, and younger age were significantly associated with emergency department visits for nonemergent eye problems in the United States [25]. In this study, only 13.2% of hospital admissions due to eye diseases were emergency admissions. Between 2006 and 2011 in the United States, more than 4 million emergency department visits occurred for conjunctivitis, subconjunctival hemorrhages, and stye [25]. In this study, most of the hospitalizations due to disorders of the conjunctiva (81.7%) were emergency admission, which is in line with the data from the United States. Moreover, in this study, over 80% of hospital admissions due to disorders of the sclera, cornea, iris, and ciliary body were also emergency admissions. National registries may be a valuable data source for the international comparison of eye care.
In 2019, the major cause of eye-related hospitalizations in Poland was disorders of the lens, responsible for over two-thirds of hospital admissions. Cataracts remain one of the leading causes of blindness [3,4]. Cataract surgery is a fast and cost-effective intervention with rapid visual recovery and good visual outcomes [34]. Findings from this study showed that most patients hospitalized due to cataracts were females and >90% of patients were aged 60 years and over. This is in line with the global data on cataract epidemiology [35]. Disorders of the choroid and retina (mainly AMD) were the second most common cause of hospitalization. AMD is a growing eye health problem in developed countries, mostly due to population aging and lifestyle factors associated with the development of AMD, like smoking, and low dietary intake of antioxidants [36]. The number of patients hospitalized due to AMD may increase because of socio-economic changes in Poland [18]. Characteristics of the major causes of ophthalmological hospitalizations presented in this study can be used by other countries (mostly developing countries) to estimate further eye healthcare needs.
In 2019, every month approximately 30 000 patients were admitted to the hospital due to eye diseases, except the December, when the number of hospital admissions due to eye diseases reached 27 629 admissions. This drop may result from the fact that the winter season and Christmas can affect patients’ willingness to visit a doctor. In the case of many ophthalmological procedures financed from public funds, medical facilities have a limit on the number of performed procedures each year [20]. However, in April 2019, the limits on cataract procedures financed from public funds were lifted, and facilities could perform the procedure on any patient who met the indications for surgery. Monthly differences in eye healthcare utilization require further investigation.
In this study, regional differences in hospital admission rates per 100 000 inhabitants were noticed. Eye care services in Poland are provided by less than 5000 ophthalmologists [21], so the limited number of healthcare workers may be a major barrier to eye health care. Vision care inequity is a relatively common phenomenon, observed also in high-income countries like the USA [37]. In addition to the organization of healthcare, other important factors affecting the utilization of eye healthcare include financial, logistics, and awareness barriers [37]. In this study, 30% of patients hospitalized due to eye diseases lived in rural areas. It is estimated that 40% of Poles live in rural areas [32]. Ophthalmologic departments are located mostly in medium-size or large cities, so we cannot exclude that some patients living in rural areas may face transportation barriers to accessing eye health care [38], but this hypothesis requires further investigation.
National data on the duration of hospitalization and type of admissions presented in this study, especially in particular health indications (ICD-10 codes), may be used as a benchmark for ophthalmology departments and hospitals. Length of stay is a commonly used measure for quality of care [39]. In this study, the duration of hospitalization differed by cause of admission. Most of the patients were hospitalized for less than 24 h. Only 5% of patients hospitalized due to cataracts were hospitalized for 2 days. This finding may be used to evaluate the quality of eye care in medical facilities with longer lengths of stay.
Age is a significant risk factor for eye diseases [1–4]. Eye diseases can occur at any age, but most of them are age-related and start after 40 years of age. The findings from this study are in line with the global data on aging and eye diseases [3–5]. In this study, a significant peak of hospitalizations was observed between patients aged 50–59 and 60–69 years. This observation suggests that eye disease screening programs should pay particular attention to those aged 50–60 years, especially those who currently work. Out of all hospitalizations due to eye diseases reported in 2019, only 4.1% were among children. The most common cause of hospital admissions among children were disorders of the eyelid, lacrimal system, and orbit (20.7% of all pediatric hospitalizations due to eye diseases). In addition to congenital eye and adnexa disorders, injuries and acute inflammations are also common causes of hospitalization among children. Nevertheless, vision screening programs are needed to identify vision impairments among children [40]. In Poland, vision screening is a part of the regular medical check-ups provided by general practitioners. ICD-10 code H35.3 is used for AMD diagnosis, but this code also includes “degeneration of macula and posterior pole” [29]. It may be that younger patients (especially those aged 30 and below) admitted to the hospital due to eye diseases defined using code H35.3 have other degeneration of the macula and posterior pole, rather than AMD. However, there were only 114 patients under 30 years of age hospitalized with the H35.3 diagnostic code.
As data on underlying conditions (comorbidities) are reported to the Polish National Hospital Register, an attempt to provide characteristics of comorbidities among patients hospitalized due to eye diseases was carried out. However, the prevalence of chronic diseases was 28.6% among patients with age-related cataracts and 29.0% among patients with AMD. As most of the patients were over 60 years old and age is a significant risk factor for chronic diseases [41], this finding suggests that numerous physicians miss data on co-existing diseases among patients hospitalized due to eye diseases. Most eye surgeries are low-invasive, and patients can leave the hospital on the same day, so ophthalmologists might miss comorbidities in discharge records. High-quality data are necessary to develop public health policies, so physicians who performed 1-day surgery should pay more attention to medical documentation.
There are numerous practical implications resulting from this study. Epidemiological characteristics of patients hospitalized due to eye diseases may be used by clinicians to monitor and evaluate eye disease management in Poland. Moreover, data presented in this study may be used as a benchmark for ophthalmological wards in Poland. Policymakers tasked with the organization of healthcare in Poland may use the presented data to plan further improvements in the health policy related to eye diseases. Regional differences in the hospitalization rate due to eye diseases presented in this study underline the need to reduce regional gaps in access to ophthalmological care. Moreover, data on causes of hospitalizations in different age groups may be used by healthcare professionals during the implementation of eye disease prevention programs.
The following limitations of this study should be underlined. First, this analysis is based on hospital admissions due to eye diseases. Data on patients visiting outpatient clinics were not included, so this study is limited to hospital-based ophthalmological care. Second, data on comorbidities should be analyzed carefully, as the prevalence of co-existing diseases reported by ophthalmologists in discharge records is lower than that shown in the epidemiological data on the health status of the Polish population, especially among elderly patients with cataracts [42]. Therefore, sub-analysis based on the prevalence of chronic diseases such as diabetes or hypertension was missed. Third, data on surgical procedures and types of treatment was not included in this analysis.
Conclusions
This study showed that disorders of the lens are the major cause of hospitalizations due to eye diseases in Poland. Significant regional differences in the hospitalization rate were observed. Hospital ophthalmological care in Poland is based mainly on planned hospitalizations lasting less than 24 h and related to ophthalmological surgery. Data on the comorbidity of ophthalmologic patients suggest that ophthalmologists do not pay enough attention to identifying and recording the patient’s health status.
Tables
Table 1. Regional differences in hospital admissions due to eye diseases (H00–H59) in Poland, January–December 2019.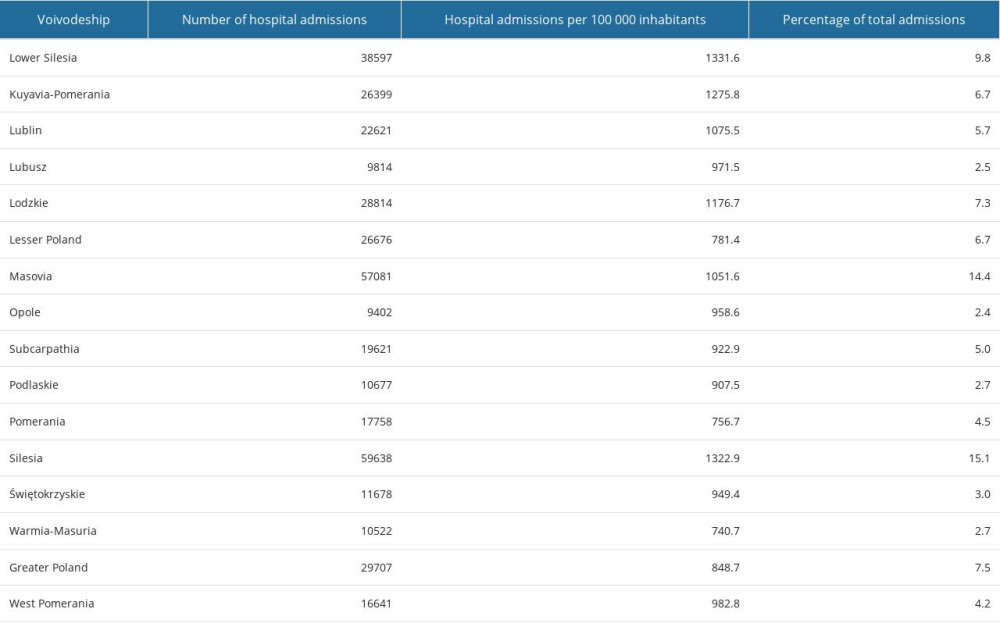 Table 2. Causes of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.
Table 2. Causes of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.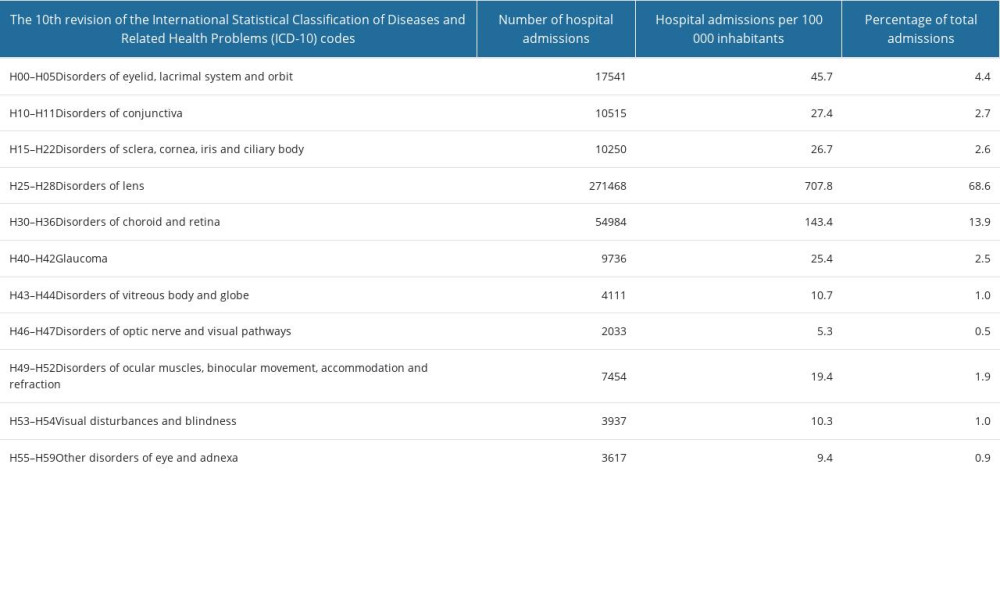 Table 3. Epidemiological characteristics of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.
Table 3. Epidemiological characteristics of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.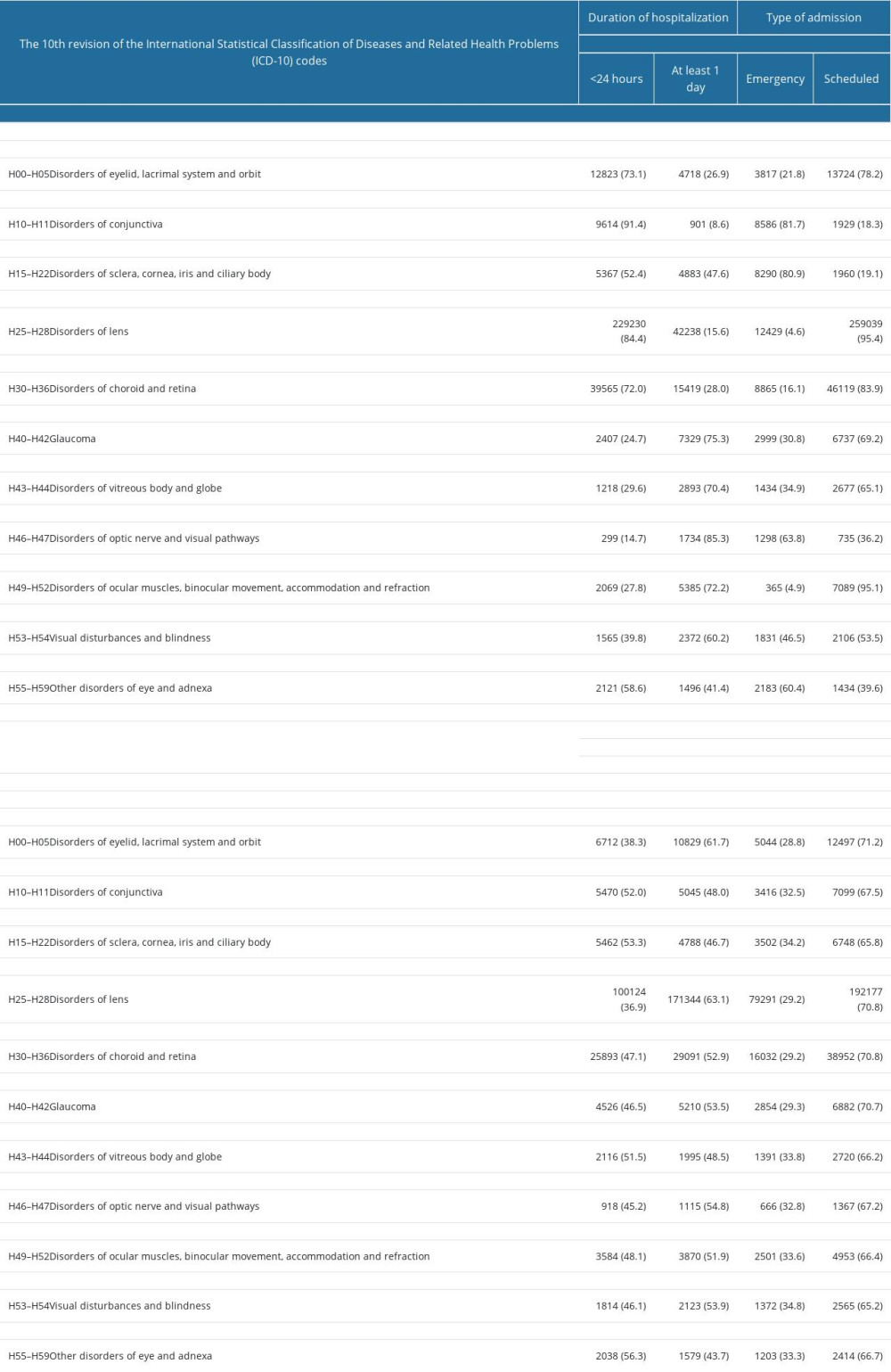 Table 4. Hospital admissions due to diseases of the eye and adnexa (H00–H59) by age groups in Poland, January–December 2019.
Table 4. Hospital admissions due to diseases of the eye and adnexa (H00–H59) by age groups in Poland, January–December 2019.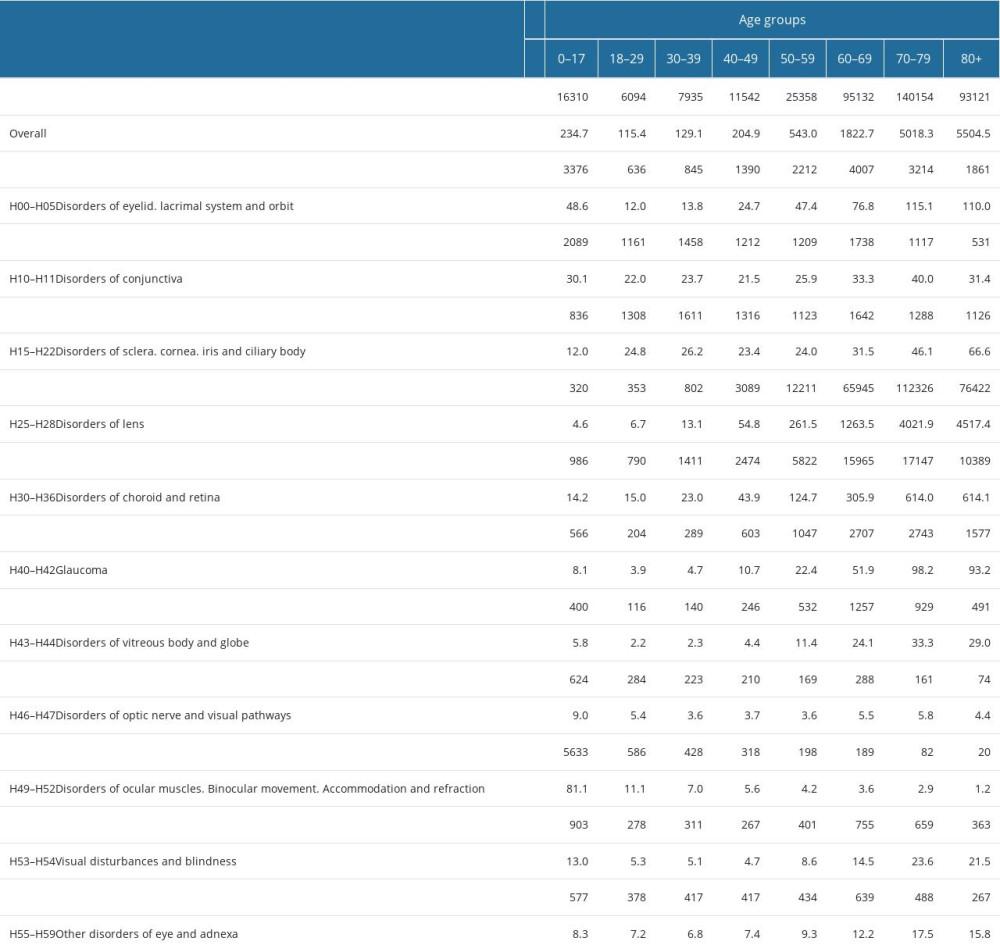 Table 5. Epidemiological characteristics of 254 788 hospital admissions due to cataract in Poland, January–December 2019.
Table 5. Epidemiological characteristics of 254 788 hospital admissions due to cataract in Poland, January–December 2019.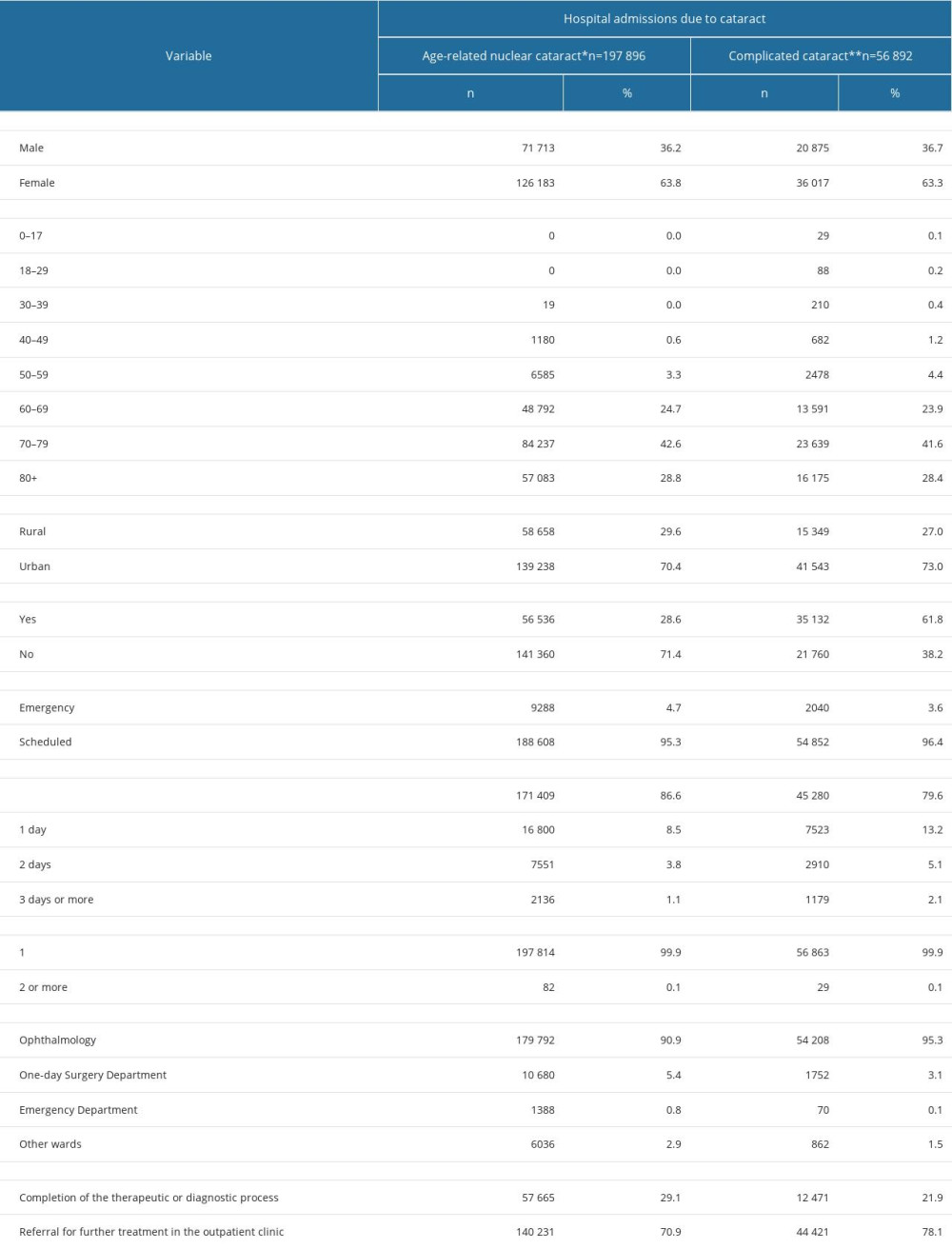 Table 6. Epidemiological characteristics of 23 677 hospital admissions (H35.3) due to age-related macular degeneration (AMD) in Poland, January–December 2019.
Table 6. Epidemiological characteristics of 23 677 hospital admissions (H35.3) due to age-related macular degeneration (AMD) in Poland, January–December 2019.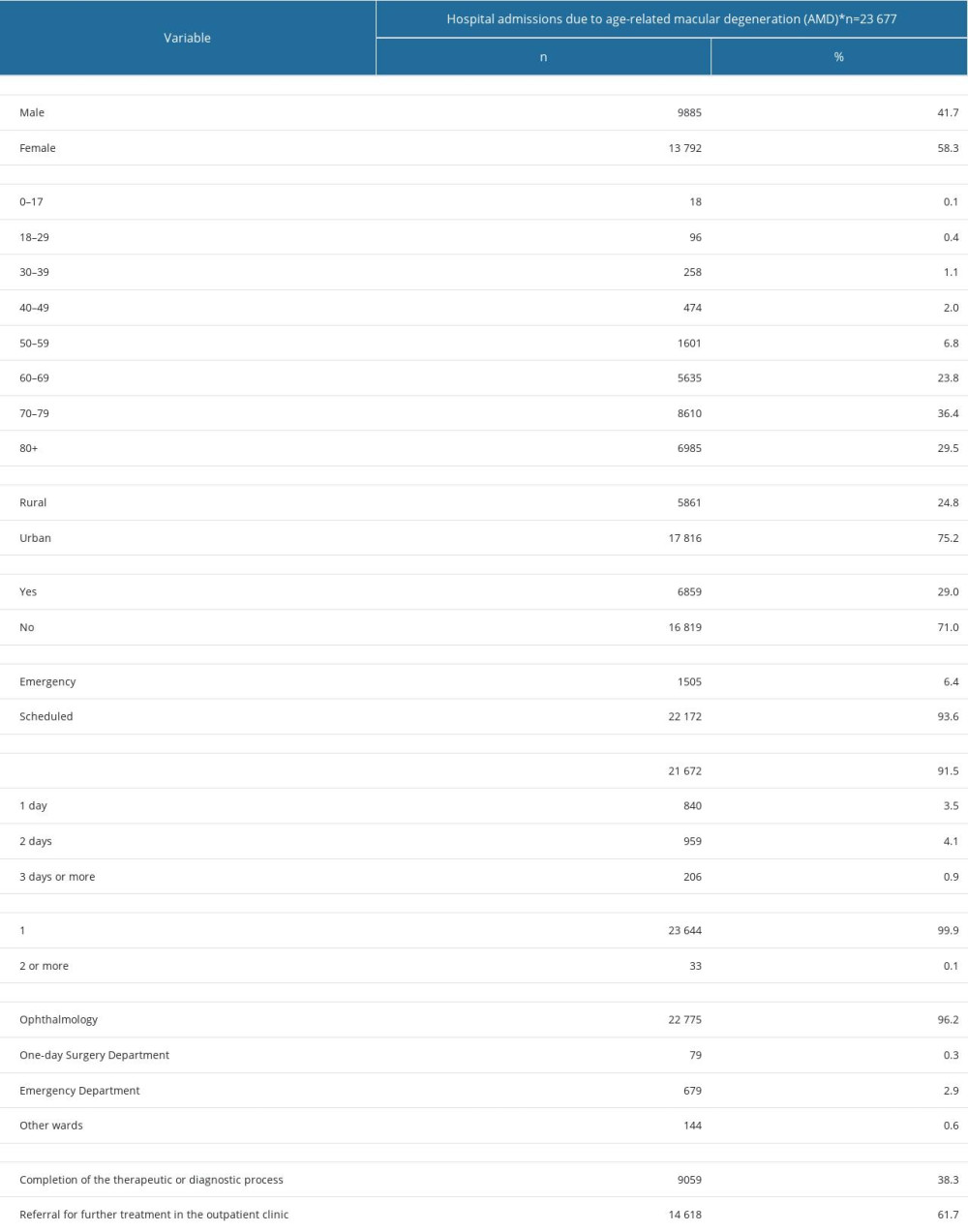
References
1. GBD 2019 Blindness and Vision Impairment Collaborators; Vision Loss Expert Group of the Global Burden of Disease Study, Trends in prevalence of blindness and distance and near vision impairment over 30 years: An analysis for the Global Burden of Disease Study: Lancet Glob Health, 2021; 9(2); e130-e43
2. World Health Organization (WHO), Factsheet: Blindness and vision impairment October 13, 2022 Available at: https://www.who.int/news-room/fact-sheets/detail/blindness-and-visual-impairment#
3. Fricke TR, Tahhan N, Resnikoff S, Global prevalence of presbyopia and vision impairment from uncorrected presbyopia: Systematic review, meta-analysis, and modelling: Ophthalmology, 2018; 125(10); 1492-99
4. GBD 2019 Blindness and Vision Impairment Collaborators; Vision Loss Expert Group of the Global Burden of Disease Study, Causes of blindness and vision impairment in 2020 and trends over 30 years, and prevalence of avoidable blindness in relation to VISION 2020: The Right to Sight: An analysis for the Global Burden of Disease Study: Lancet Glob Health, 2021; 9(2); e144-e60
5. Varma R, Vajaranant TS, Burkemper B, Visual impairment and blindness in adults in the United States: Demographic and geographic variations from 2015 to 2050: JAMA Ophthalmol, 2016; 134(7); 802-9
6. Merle BMJ, Moreau G, Ozguler A, Unhealthy behaviours and risk of visual impairment: The CONSTANCES population-based cohort: Sci Rep, 2018; 8(1); 6569
7. Hashemi H, Asgari S, Emamian MH, Age-related changes in corneal curvature and shape: the shahroud eye cohort study: Cornea, 2015; 34(11); 1456-58
8. Purola PKM, Nättinen JE, Ojamo MUI, Prevalence and 11-year incidence of common eye diseases and their relation to health-related quality of life, mental health, and visual impairment: Qual Life Res, 2021; 30(8); 2311-27
9. Seland JH, Vingerling JR, Augood CA, Visual impairment and quality of life in the older European population, the EUREYE study: Acta Ophthalmol, 2011; 89(7); 608-13
10. Ehrlich JR, Ramke J, Macleod D, Association between vision impairment and mortality: A systematic review and meta-analysis: Lancet Glob Health, 2021; 9(4); e418-e30
11. Park SJ, Ahn S, Park KH, Burden of visual impairment and chronic diseases: JAMA Ophthalmol, 2016; 134(7); 778-84
12. Källstrand-Ericson J, Hildingh C, Visual impairment and falls: A register study: J Clin Nurs, 2009; 18(3); 366-72
13. Marques AP, Ramke J, Cairns J, Global economic productivity losses from vision impairment and blindness: EClinicalMedicine, 2021; 35; 100852
14. Burton MJ, Ramke J, Marques AP, The Lancet Global Health Commission on Global Eye Health: Vision beyond 2020: Lancet Glob Health, 2021; 9(4); e489-e551
15. Horton S, Gelband H, Jamison D, Levin C, Ranking 93 health interventions for low- and middle-income countries by cost-effectiveness: PLoS One, 2017; 12(8); e0182951
16. Ehrlich JR, Stagg BC, Andrews C, Vision impairment and receipt of eye care among older adults in low- and middle-income countries: JAMA Ophthalmol, 2019; 137(2); 146-58
17. Ono K, Hiratsuka Y, Murakami A, Global inequality in eye health: Country-level analysis from the Global Burden of Disease Study: Am J Public Health, 2010; 100(9); 1784-88
18. World Bank Group (WBG), Open Knowledge Repository: Lessons from Poland, insights for Poland: A sustainable and inclusive transition to high income status January 31, 2022 Available at: https://openknowledge.worldbank.org/handle/10986/28960
19. Kobza J, Geremek M, Exploring the life expectancy increase in Poland in the context of CVD mortality fall: The risk assessment bottom-up approach, from health outcome to policies: Inquiry, 2015; 52; 0046958015613091
20. Sagan A, Panteli D, Borkowski W, Poland health system review: Health Syst Transit, 2011; 13(8); 1-193
21. The Supreme Medical Council, Poland: Number of physicians and dentists by field and degree of specialization December 03, 2022 Available at: [in Polish]https://nil.org.pl/uploaded_files/1670080999_zestawienie-nr-4-za-listopad-2022.pdf
22. Rush SW, Gerald AE, Smith JC, Prospective analysis of outcomes and economic factors of same-day bilateral cataract surgery in the United States: J Cataract Refract Surg, 2015; 41(4); 732-39
23. Reeve C, Humphreys J, Wakerman J, A comprehensive health service evaluation and monitoring framework: Eval Program Plann, 2015; 53; 91-98
24. Schütte S, Acevedo PNM, Flahault A, Health systems around the world – a comparison of existing health system rankings: J Glob Health, 2018; 8(1); 010407
25. Channa R, Zafar SN, Canner JK, Epidemiology of eye-related Emergency Department visits: JAMA Ophthalmol, 2016; 134(3); 312-19
26. Alrawashdeh HM, Naser AY, Alwafi H, Trends in hospital admission due to diseases of the eye and adnexa in the past two decades in England and Wales: An ecological study: Int J Gen Med, 2022; 15; 1097-110
27. Poznańska A, Goryński P, Seroka W, Nationwide General Hospital Morbidity Study as a source of data about Polish population health: Przegl Epidemiol, 2019; 73(1); 69-80
28. Goryński P, Moskalewicz B, Seroka W, Analysis of diabetic patients hospitalizations in Poland by gender, age and place of residence: Rocz Panstw Zakl Hig, 2022; 73(1); 99-108
29. World Health Organization (WHO): ICD-10 Version: 2010 January 02, 2023 Available at: https://icd.who.int/browse10/2010/en
30. Gujski M, Jankowski M, Rabczenko D, Characteristics and clinical outcomes of 116,539 patients hospitalized with COVID-19 – Poland, March–December 2020: Viruses, 2021; 13(8); 1458
31. Sękowski K, Grudziąż-Sękowska J, Goryński P, Epidemiological analysis of diabetes-related hospitalization in Poland before and during the COVID-19 pandemic, 2014–2020: Int J Environ Res Public Health, 2022; 19(16); 10030
32. Statistics Poland (GUS), Statistical Yearbooks: Demographic Yearbook of Poland 2022 December 22, 2022 Available at: https://stat.gov.pl/en/topics/statistical-yearbooks/statistical-yearbooks/demographic-yearbook-of-poland-2022,3,16.html
33. Partka O, Wysocki MJ, Epidemiology of eye diseases and infrastructure of ophthalmology in Poland: Epidemiological Review, 2015; 69(4); 905-8
34. Jaggernath J, Gogate P, Moodley V, Naidoo KS, Comparison of cataract surgery techniques: Safety, efficacy, and cost-effectiveness: Eur J Ophthalmol, 2014; 24(4); 520-26
35. Fang R, Yu YF, Li EJ, Global, regional, national burden and gender disparity of cataract: Findings from the global burden of disease study 2019: BMC Public Health, 2022; 22(1); 2068
36. Mitchell P, Liew G, Gopinath B, Wong TY, Age-related macular degeneration: Lancet, 2018; 392(10153); 1147-59
37. Goyal A, Richards C, Patel V, The Vision Detroit Project: Visual burden, barriers, and access to eye care in an urban setting: Ophthalmic Epidemiol, 2022; 29(1); 13-24
38. Lechowski Ł, Jasion A, Spatial accessibility of primary health care in rural areas in Poland: Int J Environ Res Public Health, 2021; 18(17); 9282
39. Lingsma HF, Bottle A, Middleton S, Evaluation of hospital outcomes: The relation between length-of-stay, readmission, and mortality in a large international administrative database: BMC Health Serv Res, 2018; 18(1); 116
40. Atowa UC, Wajuihian SO, Hansraj R, A review of paediatric vision screening protocols and guidelines: Int J Ophthalmol, 2019; 12(7); 1194-201
41. Li Z, Zhang Z, Ren Y, Aging and age-related diseases: From mechanisms to therapeutic strategies: Biogerontology, 2021; 22(2); 165-87
42. OECD/European Observatory on Health Systems and Policies: 2021 Poland: Country Health Profile 2021, State of Health in the EU, 2021, Brussels, OECD Publishing, Paris/European Observatory on Health Systems and Policies
Figures
Tables
 Table 1. Regional differences in hospital admissions due to eye diseases (H00–H59) in Poland, January–December 2019.
Table 1. Regional differences in hospital admissions due to eye diseases (H00–H59) in Poland, January–December 2019. Table 2. Causes of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.
Table 2. Causes of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019. Table 3. Epidemiological characteristics of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.
Table 3. Epidemiological characteristics of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019. Table 4. Hospital admissions due to diseases of the eye and adnexa (H00–H59) by age groups in Poland, January–December 2019.
Table 4. Hospital admissions due to diseases of the eye and adnexa (H00–H59) by age groups in Poland, January–December 2019. Table 5. Epidemiological characteristics of 254 788 hospital admissions due to cataract in Poland, January–December 2019.
Table 5. Epidemiological characteristics of 254 788 hospital admissions due to cataract in Poland, January–December 2019. Table 6. Epidemiological characteristics of 23 677 hospital admissions (H35.3) due to age-related macular degeneration (AMD) in Poland, January–December 2019.
Table 6. Epidemiological characteristics of 23 677 hospital admissions (H35.3) due to age-related macular degeneration (AMD) in Poland, January–December 2019. Table 1. Regional differences in hospital admissions due to eye diseases (H00–H59) in Poland, January–December 2019.
Table 1. Regional differences in hospital admissions due to eye diseases (H00–H59) in Poland, January–December 2019. Table 2. Causes of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.
Table 2. Causes of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019. Table 3. Epidemiological characteristics of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019.
Table 3. Epidemiological characteristics of hospital admissions due to diseases of the eye and adnexa (H00–H59) in Poland, January–December 2019. Table 4. Hospital admissions due to diseases of the eye and adnexa (H00–H59) by age groups in Poland, January–December 2019.
Table 4. Hospital admissions due to diseases of the eye and adnexa (H00–H59) by age groups in Poland, January–December 2019. Table 5. Epidemiological characteristics of 254 788 hospital admissions due to cataract in Poland, January–December 2019.
Table 5. Epidemiological characteristics of 254 788 hospital admissions due to cataract in Poland, January–December 2019. Table 6. Epidemiological characteristics of 23 677 hospital admissions (H35.3) due to age-related macular degeneration (AMD) in Poland, January–December 2019.
Table 6. Epidemiological characteristics of 23 677 hospital admissions (H35.3) due to age-related macular degeneration (AMD) in Poland, January–December 2019. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387