06 December 2023: Clinical Research
Dermoscopic Evaluation of Actinic Changes in the Lips of Indigenous Children Living at High Altitude in Ecuador: A Descriptive Study
Julia Elisa CabezasDOI: 10.12659/MSM.942554
Med Sci Monit 2023; 29:e942554
Abstract
BACKGROUND: High altitude increases sunlight exposure, resulting in actinic keratosis, which predisposes people to skin cancer. The dermoscopy procedure evaluates keratotic and pigmented skin changes. This study aimed to describe the clinical and dermoscopic actinic changes in the lips of 25 indigenous children living at high altitude in Ecuador.
MATERIAL AND METHODS: An observational study was conducted in a public school in the Andes region of Ecuador (August-November 2019). Twenty-five children, males and females, age 5-15 years were assessed by complete physical examination, digital dermoscopic photographs, and punch biopsies. Descriptive statistics and Fisher’s exact test were used to summarize and analyze the data.
RESULTS: We included 17 (68%) boys and 8 (32%) girls with a mean age of 9.8±2.0 years. Clinical lips findings reported desquamation [52% Upper Lip (UL); 40% Lower Lip (LL)], fissuring (8% UL; 8% LL), scabs (8% UL; 8% LL), and discoloration (40% UL; 20% LL). Dermoscopic features included a white-yellow lip color (24% UL; p=0.02). The main morphologic pattern of blood vessels was monomorphic (88% UL; p<0.001), polymorphous (60% LL; p<0.001), dotted pattern (64% UL; 28% LL; p=0.02), and linear-irregular (32% UL; 72% LL; p=0.01). Girls had radiating white structures on UL (p=0.025), while boys presented white structureless areas (UL 63.6%; LL 77.8%; p=0.032). No differences in dermoscopic findings were observed according to Fitzpatrick scale score (FSS). Punch biopsies showed no indications of actinic cheilitis.
CONCLUSIONS: Dermoscopic features in indigenous children living in high altitudes were related to actinic damage, but histopathological findings were negative.
Keywords: Actinic Cheilitis, Dermatology, Pediatrics, South America, Sunlight, Male, Female, Humans, Child, Child, Preschool, Adolescent, Lip, Altitude, Ecuador, Skin Neoplasms, Keratosis, Actinic
Background
Chronic sun exposure and other environmental factors like dust, dryness, cold, and wind during time spent outside are involved in actinic damage and cancer of the lower lip (LL) [1]. Actinic damage explains the molecular mechanism of how ultraviolet (UV) radiation generates reactive oxygen species that damage skin cells’ DNA, proteins, and membranes, causing burning, solar elastosis, and skin cancer [2]. Solar elastosis is the accumulation of dystrophic elastotic material causing an imbalance between adequate loss and replenishment of elastic dermal fibers [3].
Chronic actinic cheilitis is a high-altitude permanent dermatosis of the LL [2]. Living at high altitude can lead to increased sun exposure, which in turn can result in actinic cheilitis, a precursor of squamous cell carcinoma [4,5]. This condition has been reported in middle-aged populations that lived or spent most of their lifetime at altitudes over 2700 meters, where climate and sunlight are harmful to exposed skin [6]. Cheilitis indicates inflammation of the lip and includes many types [7]. Proposed terms for its classification are mostly reversible cheilitis, mostly persistent cheilitis and cheilitis in association with systemic diseases and other dermatoses [6]. In children, mostly reversible cheilitis such as cheilitis simplex, angular cheilitis, and other inflammatory and infectious conditions are more common than mostly permanent disorders such as actinic cheilitis and other potential malignancies seen in adolescents and adults [7]. However, lips conditions in children have been poorly reported so far, especially in high-altitude Latin American populations [8].
When diagnosing cheilitis, some lips lesions require histopathology assessment, especially when mostly persistent cheilitis is suspected [7]. Dermoscopy is a non-invasive diagnostic method that uses a dermatoscope, an optic magnification and adjustable inbuilt illuminating system for inspection of the skin [9,10]. The method of dermoscopy could be done without contact, without lens-to-skin contact, or contact technique, when a linkage fluid is used between the instrument and the lesion [10]. Moreover, it may be regarded as a reliable tool for reducing unnecessary biopsies [11].
Dermoscopic features in adults have been described in some reports as normal variants, inflammatory, vascular, pigmented, autoimmune, and neoplastic conditions on the lips [12,13]. Although dermoscopy is a promising tool to assess localized skin architecture defects in children, the dermoscopic description of lips in infants is scarce [14]. This study aims to describe the dermoscopic features of lips alterations in children living in the Ecuadorian Andes, a high-altitude area. Therefore, this study aimed to use dermoscopy and histopathology to examine actinic changes in the lips of 25 indigenous children living at high altitude in Ecuador.
Material and Methods
ETHICS APPROVAL AND INFORMED CONSENT:
The Institutional Review Board Ethics Committee of “Centro de la Piel” reviewed and approved the study protocol and informed consent. Furthermore, written informed consent was obtained from all the participants’ parents or guardians.
STUDY DESIGN:
This observational, descriptive, and non-randomized study was conducted in a public school at 3580 m above sea level (a.s.l.) in Cayambe, in the Andes region in Ecuador, from August to November 2019, and was implemented in accordance with Good Clinical Practice guidelines and STROBE guidelines.
OUTCOMES:
The primary outcome of this study was to describe clinical and dermoscopic lips characteristics in indigenous children living in high-altitude areas. Secondary outcomes included a description of dermatoscopic findings related to actinic damage and a comparison of dermatoscopic characteristics of lips according to children’s age, sex, and FSS.
STUDY SUBJECTS:
The study sample consisted of Ecuadorian children who attended the public school and had lived in the “La Espiga de Oro” community all their lives. Inclusion criteria were age 5–15 years old, access to the community public school, and comprehension of the Spanish language. Exclusion criteria comprised a previous diagnosis of acute or chronic illnesses and refusal to participate in the present study.
TRIAL ASSESSMENTS:
A complete physical examination was performed for each child. Sociodemographic variables included age, sex, ethnicity, FSS, height, weight, and body mass index (BMI). FSS is a phototype skin scale that classifies skin tone coloring in response to UV radiation [15]. The FSS was evaluated as “I: Always burn, never tan; II: Usually burn, tan less than average (with difficulty); III: Sometimes mild burn, tan about average; IV: Rarely burn, tan more than average (with ease); V: Brown skin, doesn’t burn, tans with ease; VI: Black skin, doesn’t burn, tans with ease” [15,16]. In addition, children underwent an in-depth clinical examination of the lips to evaluate the presence or absence of desquamation, fissuring, scabs, and loss of the sharp demarcation of the vermilion border.
Entire face photographs were taken with an iPad ® (Apple, Inc. CA, United States). Digital dermoscopic photographs of the lips were taken using a polarized dermatoscope Dermlite DL200 HR® (CA, United States). Dermatoscopic findings were described on the upper lip (UL) and LL. Dermoscopic evaluation included blood vessel morphology analysis in function of their broad morphologic pattern (monomorphic or polymorphic). Monomorphism was defined as ≥90% of blood vessels observed in a dermoscopic field following 1 particular morphology with any other morphology occupying <10% of the field, while polymorphism was defined by at least 2 or more morphologies of blood vessels, with presence of abundant different types and no predominance of 1 major type [17]. All the examiners had to reach a consensus on the dermatoscopic patterns found in each participant.
Punch biopsies were performed, and a trained dermatopathologist evaluated the standard histologic sections with hematoxylin-eosin stain. Histological findings for actinic cheilitis were defined as changes in the epithelium (such as hyperplasia, acanthosis or atrophy, hyperkeratosis, and atypia) and in the connective tissue (such as solar elastosis, which refers to the basophilic degeneration of collagen fibers), inflammatory infiltrate, and vasodilatation [18,19].
STATISTICAL ANALYSIS:
Results were expressed as mean and standard deviation (SD) for quantitative variables while frequency tables (numbers and percentages) were reported for categorical (clinical and dermoscopic) findings. Given the limited sample size, proportions were compared by the Fisher exact test. Results were considered significant at the 5% critical level (p<0.05). All statistical calculations were performed with software R (version 4.1.3).
Results
DEMOGRAPHIC CHARACTERISTICS OF THE STUDY SAMPLE:
A total of 25 children, 17 (68%) boys and 8 (32%) girls, were included in the current study. Their mean age was 9.8±2.0 years, and 13 (52%) of them were in the 9–11 years age group. Their ethnicity consisted of 15 (60%) Indigenous and 10 (40%) Hispanic children. Participants presented a FSS of III (36%), IV (60%), and V (4%). The mean weight and height were 27.6±5.5 kg and 127±10 cm, respectively. The mean BMI was 17.0±1.4 kg/m2 (28th percentile), with 23 (92%) children in the normal BMI category (Table 1).
PRIMARY OUTCOMES:
Clinical findings included desquamation (52% on the UL and 40% on the LL), fissuring (8% UL and 8% LL), scabs (8% UL and 8% LL), and discoloration at the borders of the lips (40% UL and 20% LL). In the dermoscopic findings, the lip color was white-yellow in 24% of UL (p=0.02), white-red in 68% of UL, and 84% of LL, and red in 8% of UL and 16% of LL. The broad morphologic pattern of the blood vessels was monomorphic in 88% of UL (p<0.001) and polymorphous in 60% of LL (p<0.001). Furthermore, vessel morphology consisted of dotted pattern (64% UL and 28% LL; p=0.02), linear irregular (32% of UL and 72% of LL; p=0.01), and hairpin morphology (4% UL). Desquamation was present in 60% of UL and 76% of LL, while white scales were found in 93.3% of UL and 94.7% of LL. Scabs were observed in 4% of the children and erosion was reported in 4% of UL and LL. White structures consisted of radiating lines (50.0% of UL and 38.5% of LL) and structureless white areas (43.8% of UL and 61.5% of LL) (Table 2).
SECONDARY OUTCOMES:
The dermoscopic findings distribution in children 5–8 years old was white-red [6 (100%) in UL (p=0.04) and 5 (83.3%) in LL], while in children 9–11 years old it was white-red [10 (76.9%) in LL and 6 (46.2%) in UL] and white-yellow [5 (38.5%) in UL] lip color. In the 12–15 years age category, children presented white-red [5 (83.3%) in UL and 6 (100%) in LL] and white-yellow [1 (16.7%) in UL] lip color.
The vessels’ broad morphologic pattern in the 5–8 years old group was monomorphic in all children’s UL (100%), while LL presented monomorphic and polymorphous vessels in 3 (50%) children. The 9–11 years old group showed a monomorphic pattern in 10 (76.9%) UL and 4 (30.8%) LL, while polymorphous vessels were found in 3 (23.1%) UL and 9 (69.2%) LL. Children in the 12–15 years age group evidenced monomorphic vessels in 6 (100%) UL, while the same pattern was only found in 3 (50%) LL.
UL vessel morphology UL was dotted in 5 (83.3) children, while LL presented a linear-irregular in 5 (83.3%) children of the 5–8 years age group. The UL in the 9–11 years age group presented linear-irregular morphology in 6 (46.2%) cases and dotted vessels were also found in 6 (46.2%) cases, whereas vessels in the LL of this age group were linear-irregular in 9 (69.2%) children and dotted in 4 (30.8%) children. Blood vessels in the UL of the 12–15 years old group were dotted in 5 (83.3%) children, and linear-irregular morphology in the LL of 4 (66.7%) children.
In children aged 5–8 years, desquamation was evident in 3 (50%) cases, both in the UL and LL. The 9–11 years old group presented desquamation in 8 (61.5%) cases in UL and in 12 (93.3%) cases in LL. Desquamation was found in the UL of 4 (66.7%) infants as well as in the LL of 4 (66.7%) children from the 12–15 years age group. Scabs were only found in the LL of 1 (7.7%) child in the 9–11 years age group. Erosion was only apparent in this same group, being observed in 1 (7.7%) child on the UL and in 1 (7.7%) child on the LL.
White structures were found in all age groups. The 5–8 years old group presented radiating lines on the UL in 2 (50%) instances, and structureless areas in 2 (50%) instances. White structures observed on the LL of the same group were radiating lines in 2 (40%) participants, and structureless in 3 (60%) participants. The 9–11 years age group presented radiating lines on the UL of 4 (44.4%) children and structureless areas in 4 (44.4%) children, whereas the LL of the same age group presented radiating lines in 2 (33.3%) cases and structureless areas in 4 (66.7%) cases. Furthermore, the UL of the 12–15 years age group presented radiating lines in 2 (66.7%) participants, while the LL of this group presented radiating lines in 1 (50%) child, and structureless areas also in 1 (50%) child (Table 3). The distribution of dermoscopic findings according to sex reported white-red lips color in 75% of girls both in UL and LL, while in boys it was present in 64.7% of UL and 88.2% of LL. White-yellow lips color was present only in the UL (12.5% of girls and 29.4% of boys). The vessels morphologic pattern was monomorphic in 87.5% of UL of girls, 88.2% of UL of boys, 37.5% of LL of girls and 41% of LL of boys. Polymorphous pattern was observed in 12.5% of UL of girls, 11.8% of UL of boys, 62.5% of LL of boys and 59% of LL of boys. Vessel morphology was linear-irregular in 25% of UL of girls, 35.5% of UL of boys, 75% of LL of girls and 71% of LL of boys. In addition, dotted pattern was observed in 75% of UL of girls, 58.5% of UL of boys, 25% of LL of girls and 29% of LL of boys. Hairpin pattern was observed in 5.9% of UL of boys.
Desquamation was reported in 75% of both UL and LL in girls, while in boys it was found in 52.9% of UL and 76.5% of LL. Scabs were found only in 12.5% of LL of girls. Erosion also was found solely in girls, with 12.5% of UL and 12.5% of LL.
All the white radiating lines were found on UL in girls (p=0.025), while white structures on LL in these subjects consisted of radiating lines in 80% and structureless areas in 20% (p=0.025). Boys presented radiating lines in 27.3% of UL and 11.1% of LL, while structureless areas were found in 63.6% of UL and 77.8% of LL (p=0.032) (Table 4). The distribution of dermoscopic findings according to FSS reported white-red color in 8 (88.9%) subjects in UL, while white-red color was found in 7 (77.8%) subjects in LL with FSS of III. The UL lip color in the FSS-IV group was white-yellow in 5 (33.3%) cases and white-red in 9 (60.0%) cases. The LL lip color was white-red in 13 (86.7%) children and red in 2 (13.3%) children. The FSS-V group presented red lip color in 1 and white-red color in 1. The broad morphologic pattern of vessels in the FSS-III group was monomorphic in 8 (88.9%) children on UL and 4 (44.4%) children on LL, while polymorphous pattern was observed in 5 (55.6%) children on LL. The FSS-IV group presented monomorphic vessels in 13 (86.7%) subjects on UL and in 5 (33.3%) subjects on LL, whereas a polymorphous pattern was observed in 10 (66.7%) participants on LL. Children with FSS-V displayed only polymorphous morphology (1 UL and 1 LL).
Vessel morphology in the FSS-III group was dotted in 7 (77.9%) cases on UL, while on LL this group displayed a linear-irregular morphology in 7 (77.8%) cases. The UL of children of the FSS-IV group presented linear-irregular morphology in 5 (33.3%) cases and dotted morphology in 9 (60.0%) cases. Further in this group, vessels on LL showed linear-irregular morphology in 10 (66.7%) cases and dotted morphology in 5 (33.3%) cases. The FSS-V group presented linear-irregular vessels in 1 child on UL and in 1 child on LL.
Desquamation was found on the UL of 5 (55.6%) children and on the LL of 6 (66.7%) children of the FSS-III group. The FSS-IV group presented desquamation in 10 (66.7%) subjects on UL and in 12 (80.0%) subjects on LL. In the FSS-V group, this finding was only seen on the LL of 1 child. Scabs were found on the LL of 1 child from the FSS-IV group. Erosion was found only in the FSS-IV group, being 1 case on both UL and LL.
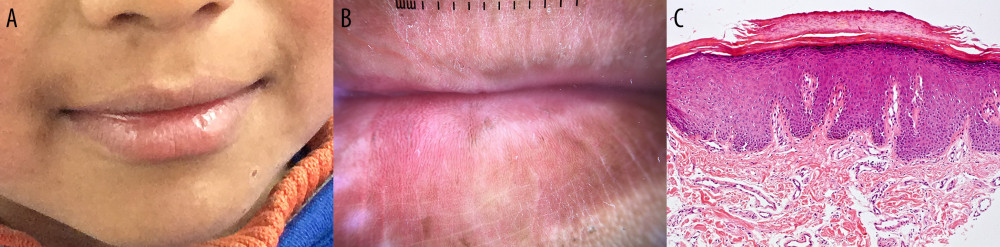
The UL in the FSS-III group presented radiating lines in 2 (40.0%) children and structureless areas in 3 (60.0%) children, while the LL presented radiating lines in 1 (20.0%) individual and structureless areas in 4 (80.0%) others. The UL of the FSS-IV group presented radiating lines in 6 (54.5%) children and structureless areas in 4 (36.4%) children, whereas the LL of this group evidenced 4 (50.0%) cases with radiating lines and 4 (50.0%) cases with structureless areas. There were no white structures found on the FSS-V group (Table 5). Punch biopsies were performed in 5 children whose lesions were indicative of actinic damage. Biopsy and histopathological report showed no indications of actinic cheilitis (Figure 1).
Discussion
This observational study was based on 25 indigenous children, mostly boys. Most of the children had an FSS of IV, in line with their Indigenous and Hispanic ethnicity. The predominant clinical findings were desquamation and discoloration at the borders of the lips, which was twice as common in upper lips than in lower lips, although the difference was not statistically significant. Based on dermoscopic assessment, the most prevalent lips color was white-red and the vessels showed mostly monomorphic pattern on UL, while on LL vessels showed both polymorphous and monomorphic patterns. Furthermore, vessel morphology differed between UL and LL; dotted vessels being more common on UL and linear-irregular pattern more common on LL. Dermoscopic assessment also revealed desquamation on UL and LL, with most of the scales being white. Scabs and erosion were fairly uncommon. White structures were predominantly radiating lines and structureless areas. It is noteworthy that most children who had LL lesions also had UL lesions. Unfortunately, the lack of similar studies limits the comparison of our results.
White structures showed a different distribution according to sex. Girls presented radiating lines more often than boys, while the most common white structures in boys were structureless areas. There were no differences in dermoscopic findings according to FSS. Biopsies showed no indication of actinic damage. Instead, these findings were consistent with cheilitis simplex, which is frequent in people who live in cold, windy, and dry climates [7].
Dermoscopic findings in the study children were comparable with those reported in adults with actinic cheilitis (which are usually located on LL, although also present here in UL), but no histopathological evidence was observed to corroborate the diagnosis [13]. This falls in line with previous reports such as the cross-sectional study carried out in 210 fishermen and women from Brazil by Oliveira et al (2010), which found that actinic cheilitis is prevalent among people aged >50 years or those with cumulative sun exposure of >30 years [20]. Also, the study by Cavalcante et al (2008) found that over 75% of patients with actinic cheilitis were ≥40 years old [19].
Moreover, a cross-sectional study reported a high prevalence of photodermatoses among pediatric population living at high altitudes (over 3500 a.s.l.) in Peru with an adjusted odds ratio of 2.76; CI 95%: 1.57–4.86 [21]. Interestingly, study children often presented with melanotic lesions, not considered here, but which would require further investigation and characterization.
This study has several limitations, including the small sample size. This considerably restricts the generalization of the findings and certainly calls for caution in their interpretation. Further, biopsies were performed in only 5 children. Nonetheless, the study was based on a relatively homogenous sample of young individuals, which is noteworthy due to the lack of information of actinic damage in this population. Another important limitation was the methodology assessment of the study. Clinical and dermoscopic evaluation can be subjective, but histopathological studies were only carried out in children whose lesions were indicative of actinic damage. Because previously published studies in high-altitude populations and climates are scarce, the present study sheds light on an important and neglected domain of dermatological damages of people living in high-altitude areas. Additionally, larger studies should be conducted from this perspective. They will allow the assessment of the distribution of actinic lesions in these specific populations, as well as identifying salient dermoscopic patterns that characterize them, particularly with respect to premalignant or malignant lesions.
Conclusions
According to our findings, indigenous Ecuadorian children living in high-altitude areas present actinic skin lesions in the lips, but no histopathological evidence of actinic cheilitis.
References
1. De Visscher JGAM, Van Der Waal I, Etiology of cancer of the lip: A review: Int J Oral Maxillofac Surg, 1998; 27; 199-203
2. Bilaç C, Şahin MT, Öztürkcan S, Chronic actinic damage of facial skin: Clin Dermatol, 2014; 32(6); 752-62
3. Weihermann AC, Lorencini M, Brohem CA, de Carvalho CM, Elastin structure and its involvement in skin photoageing: Int J Cosmet Sci, 2017; 39(3); 241-47
4. Muse ME, Crane JS, Actinic cheilitis: StatPearls, 2023, Treasure Island (FL), StatPearls Publishing Available from:https://www.ncbi.nlm.nih.gov/books/NBK551553/
5. Singh LC, High altitude dermatology: Indian J Dermatol, 2017; 62(1); 59-65
6. Singh GK, Chatterjee M, Grewal RS, Verma R, Incidence and care of environmental dermatoses in the high-altitude region of Ladakh, India: Indian J Dermatol, 2013; 58(2); 107-12
7. Lugović-Mihić L, Pilipović K, Crnarić I, Differential diagnosis of cheilitis – how to classify cheilitis?: Acta Clin Croat, 2018; 57(2); 342-51
8. de Almeida ASCB, Kato C, de NA, de O, Jácome-Santos H, A retrospective analysis of oral and maxillofacial lesions in children and adolescents reported in two different services: J Clin Exp Dent, 2021; 13(9); e894-e905
9. Argenziano G, Soyer HP, Chimenti S, Dermoscopy of pigmented skin lesions: Results of a consensus meeting via the internet: J Am Acad Dermatol, 2003; 48(5); 679-93
10. Sonthalia S, Yumeen S, Kaliyadan F, Dermoscopy overview and extradiagnostic applications: StatPearls, 2023, Treasure Island (FL) Available from: https://www.ncbi.nlm.nih.gov/books/NBK537131/
11. Elwan NM, Gheida SF, El-Toukhey AM, Radwan NS, Dermoscopic and histopathological correlation in some epidermal tumors: A preliminary study: Journal of the Egyptian Women’s Dermatologic Society, 2015; 12(1); 24-31
12. Jha AK, Sonthalia S, Slawinska M, Mucoscopy of lip squamous cell carcinoma and correlation with skin phototype and histological differentiation: A multicentric retrospective observational study by the International Dermoscopy Society: Int J Dermatol, 2021; 60; 489-96
13. Kumar Jha A, Vinay K, Slawinska M, Application of mucous membrane dermoscopy (mucoscopy) in diagnostics of benign oral lesions – literature review and preliminary observations from International Dermoscopy Society study: Dermatol Ther, 2021; 34; e14478
14. Silverberg NB, A pilot trial of dermoscopy as a rapid assessment tool in pediatric dermatoses: Cutis, 2011; 87(3); 148-54
15. Fitzpatrick TB, The validity and practicality of sun-reactive skin types I through VI: Arch Dermatol, 1988; 124; 869-71
16. Gupta V, Sharma VK, Skin typing: Fitzpatrick grading and others: Clin Dermatol, 2019; 37; 430-36
17. Jha AK, Sławińska M, Vinay K, Dermoscopic features of actinic cheilitis and other common inflammatory cheilitis: A multicentric retrospective observational study by the international dermoscopy society: Dermatology, 2022; 238(5); 870-75
18. de Santana Sarmento DJ, da Costa Miguel MC, Actinic cheilitis: Clinicopathologic profile and association with degree of dysplasia: Int J Dermatol, 2014; 53; 466-72
19. Cavalcante ASR, Anbinder AL, Carvalho YR, Actinic cheilitis: Clinical and histological features: J Oral Maxillofac Surg, 2008; 66; 498-503
20. de Oliveira Ribeiro A, da Silva LCF, Martins-Filho PRS, Prevalence of and risk factors for actinic cheilitis in Brazilian fishermen and women: Int J Dermatol, 2014; 53(11); 1370-76
21. Ramos W, Gutierrez EL, De La Cruz-Vargas JA, Exposure to atmospheric ozone disruption and altitude over 3500 m.a.s.l. are associated with a higher prevalence of photodermatoses in pediatric population of high-altitude in Peru: Clin Cosmet Investig Dermatol, 2022; 15; 1779-86
Tables
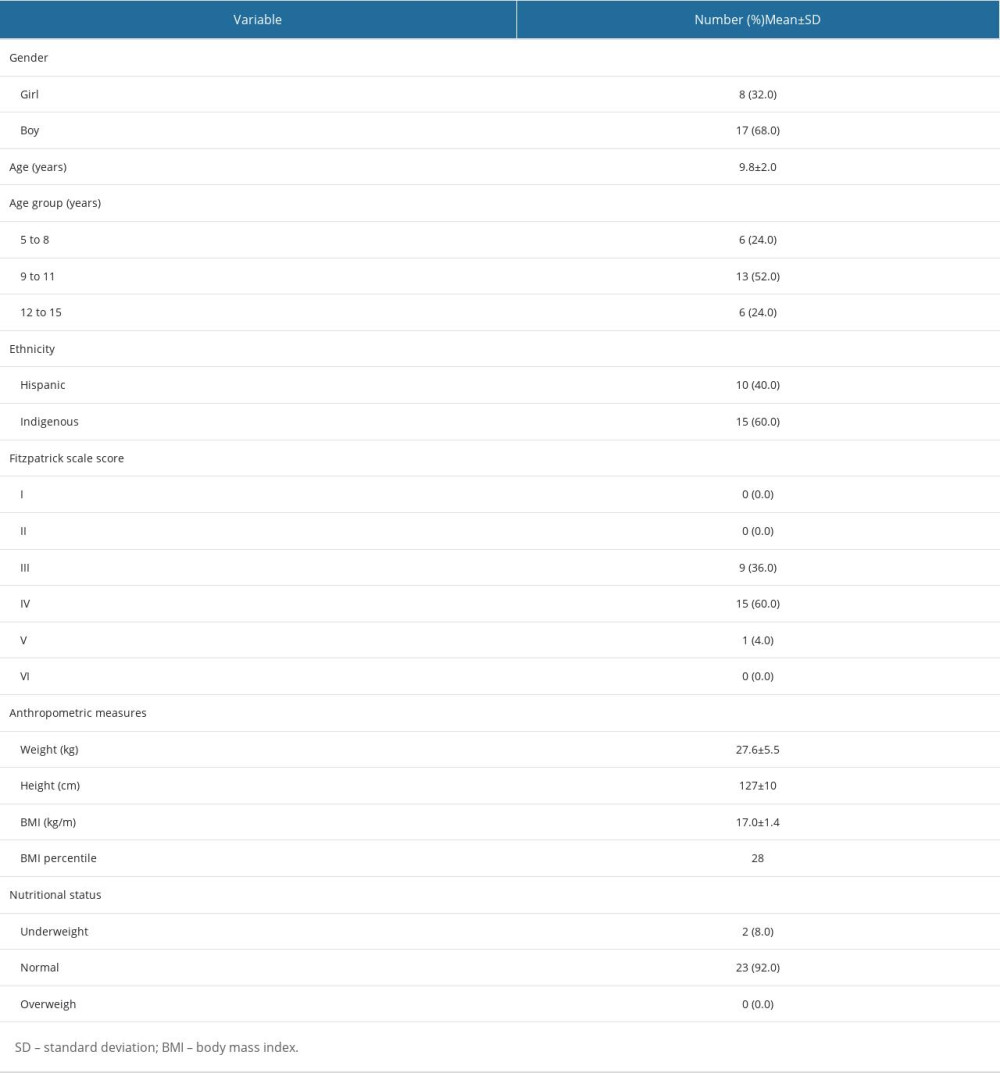 Table 1. Baseline characteristics of the study population (N=25).
Table 1. Baseline characteristics of the study population (N=25).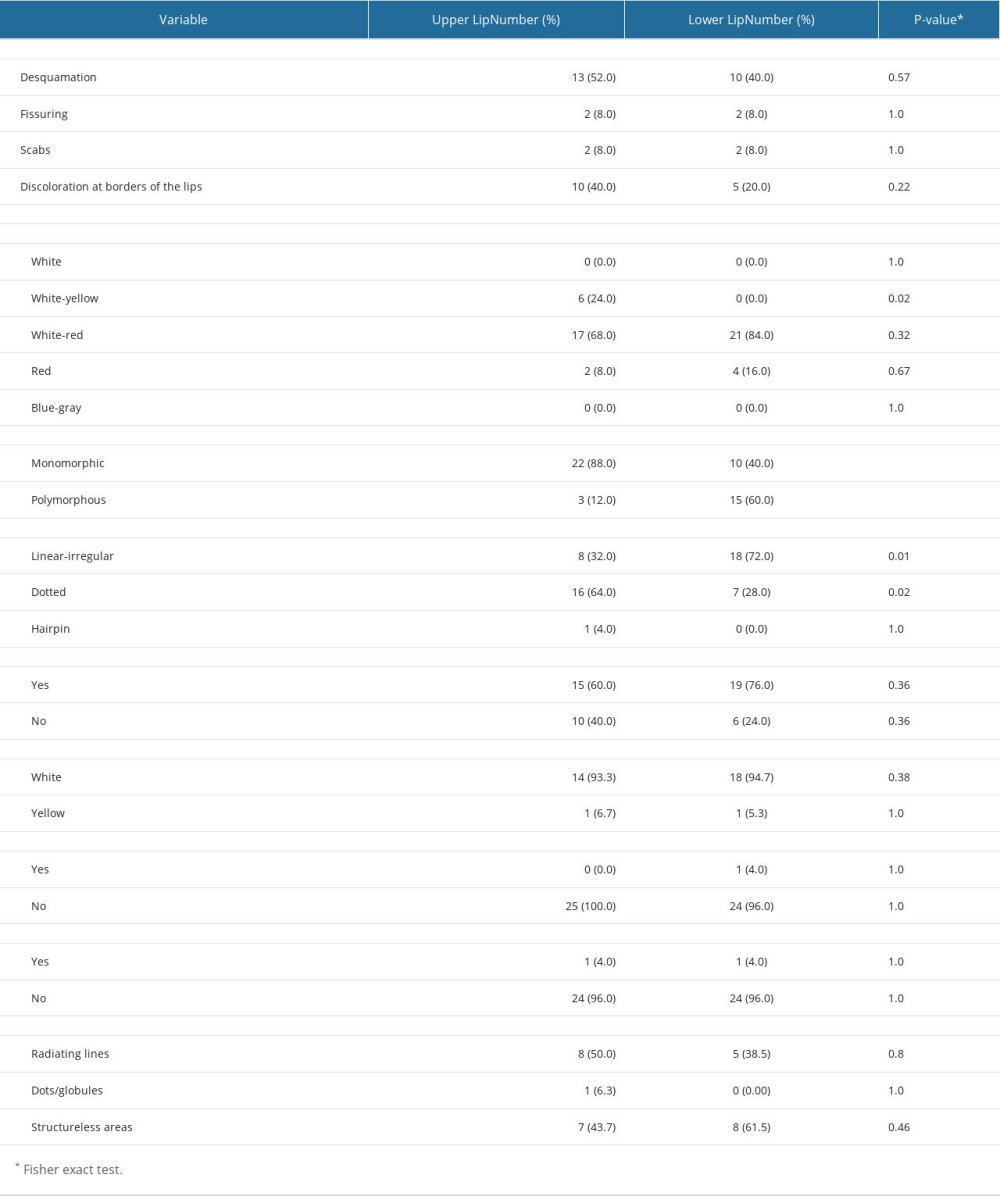 Table 2. Clinical and dermoscopic patterns.
Table 2. Clinical and dermoscopic patterns.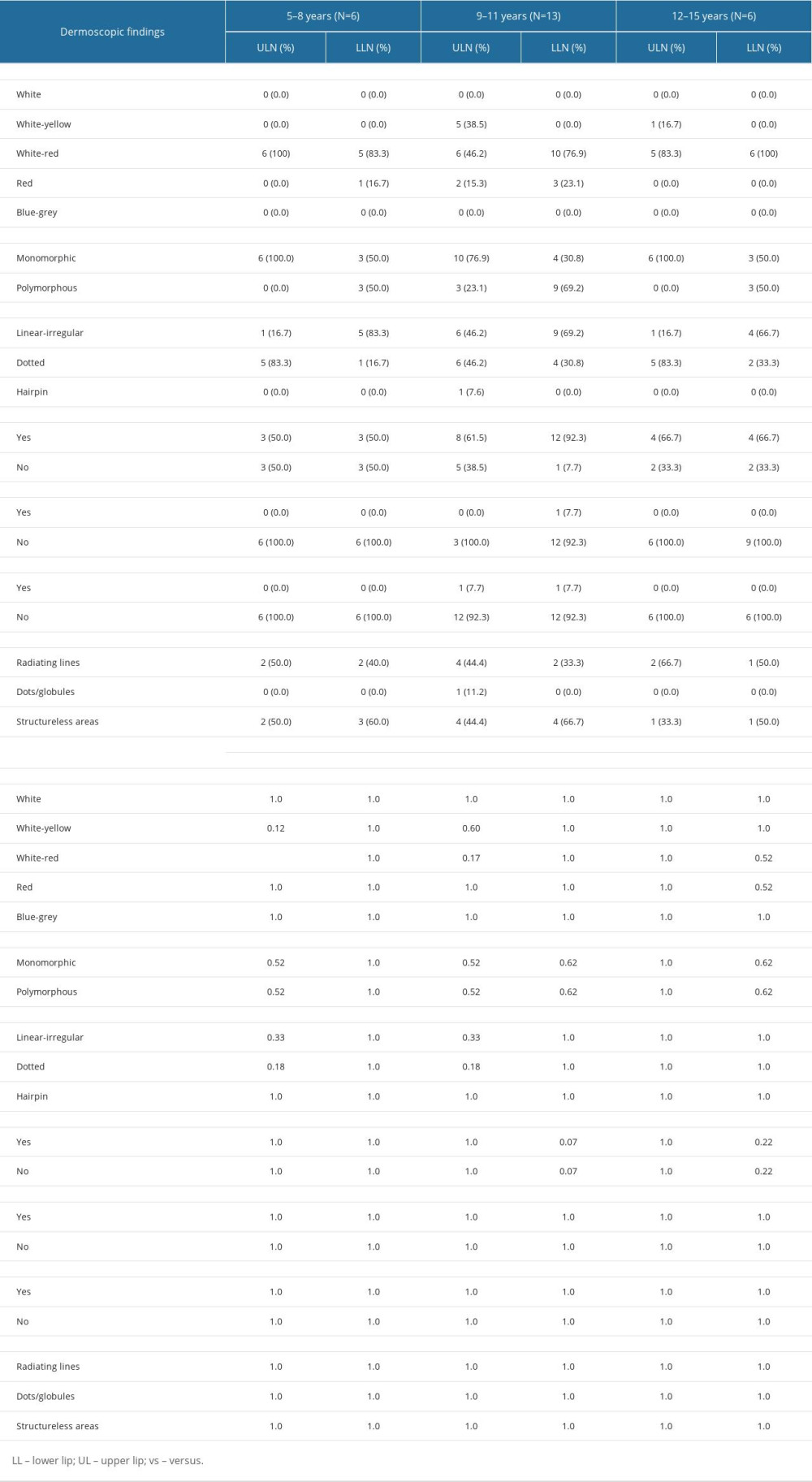 Table 3. Distribution of dermoscopic findings among study age groups.
Table 3. Distribution of dermoscopic findings among study age groups.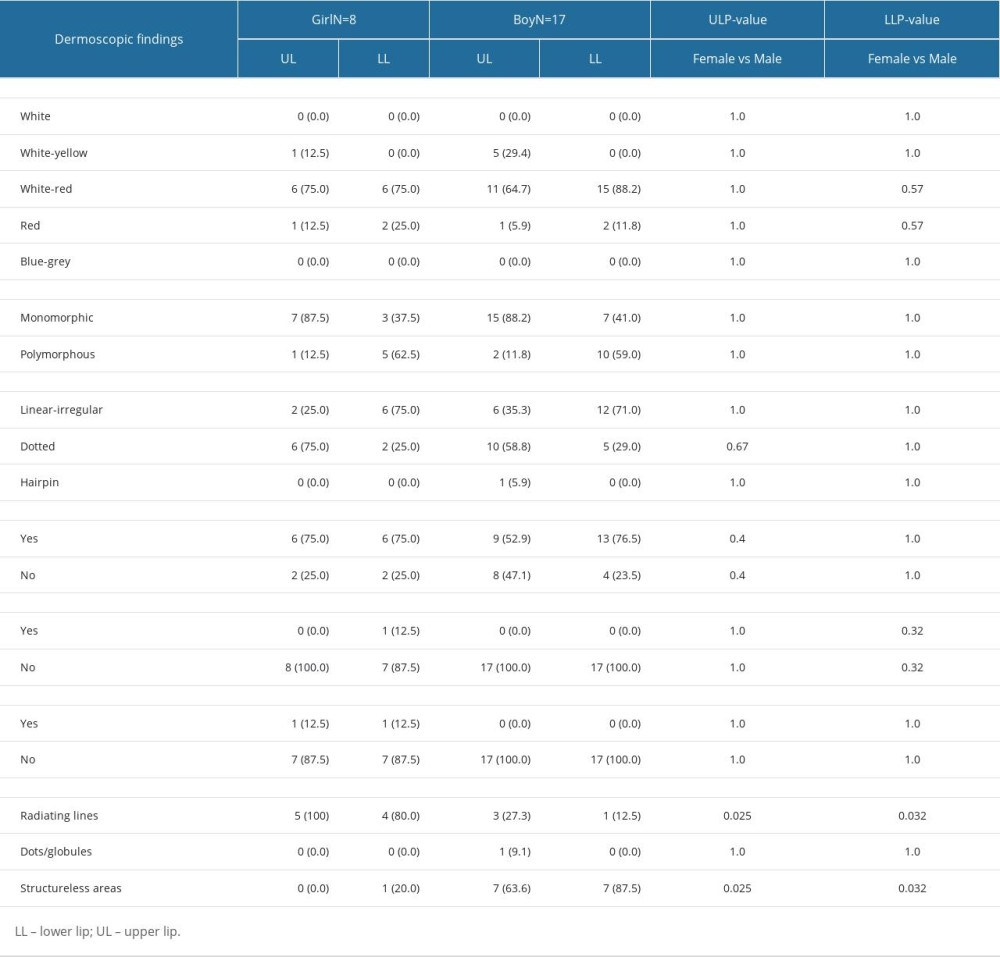 Table 4. Distribution of dermoscopic findings according to sex.
Table 4. Distribution of dermoscopic findings according to sex.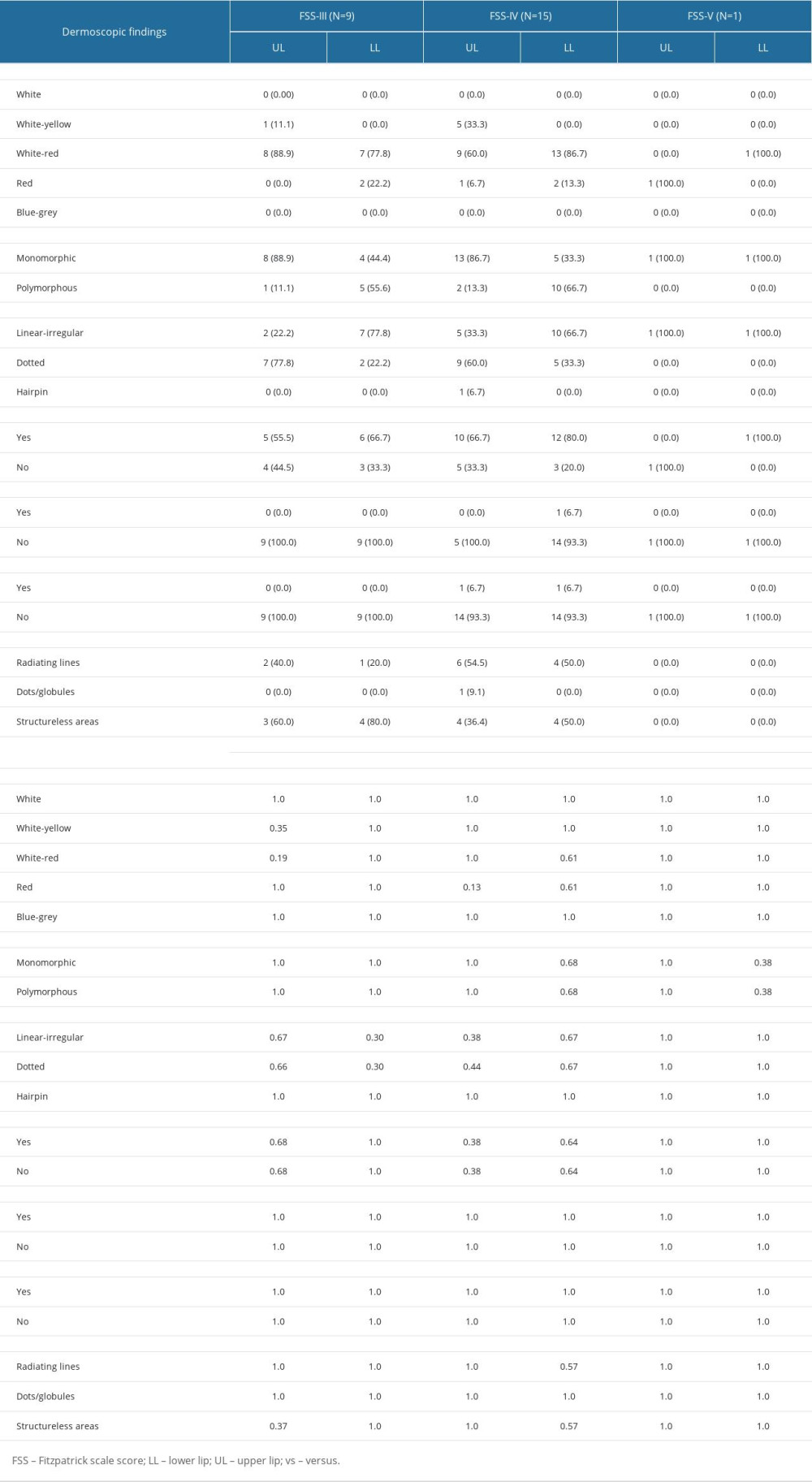 Table 5. Demographic findings.
Table 5. Demographic findings. Table 1. Baseline characteristics of the study population (N=25).
Table 1. Baseline characteristics of the study population (N=25). Table 2. Clinical and dermoscopic patterns.
Table 2. Clinical and dermoscopic patterns. Table 3. Distribution of dermoscopic findings among study age groups.
Table 3. Distribution of dermoscopic findings among study age groups. Table 4. Distribution of dermoscopic findings according to sex.
Table 4. Distribution of dermoscopic findings according to sex. Table 5. Demographic findings.
Table 5. Demographic findings. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387