11 December 2021: Clinical Research
Retrospective Study of 1255 Non-Anticoagulated Patients with Nonvalvular Atrial Fibrillation to Determine the Risk of Ischemic Stroke Associated with Left Atrial Spontaneous Echo Contrast on Transesophageal Echocardiography
Kesen Liu1ABCDEF, Yukun Li1B, Kui Wu1B, Junlei Li1C, Yong Zhu1CD, Fei Guo1CD, Rong Bai1AEF, Jianzeng Dong1ADEFG*DOI: 10.12659/MSM.934795
Med Sci Monit 2021; 27:e934795
Abstract
BACKGROUND: Left atrial spontaneous echo contrast (LASEC) is associated with an increased risk of stroke in patients with nonvalvular atrial fibrillation (NVAF). Therefore, a tool that identifies the risk of LASEC in non-anticoagulated patients with NVAF may be helpful for stroke risk stratification and early stroke prevention in these patients. The aim of this retrospective study was to establish a novel risk score model to determine the risk of ischemic stroke associated with LASEC on transesophageal echocardiography (TEE).
MATERIAL AND METHODS: This study retrospectively and consecutively enrolled 1255 non-anticoagulated patients with NVAF who underwent TEE prior to catheter ablation or left atrial appendage occlusion. Most importantly, a novel nomogram was developed using a logistic regression model to predict the risk of LASEC.
RESULTS: A nomogram was established for LASEC prediction which included 5 independent risk factors determined by multivariable logistic regression analysis: increased age, non-paroxysmal atrial fibrillation, previous stroke/transient ischemic attack, congestive heart failure, and left atrial enlargement. The receiver operating characteristic curve analysis showed that the area under the curve (AUC) of the novel risk score model was 0.879 (95% confidence interval: 0.849-0.909, P<0.001). Compared with the CHA2DS2-VASc score, the novel risk score model had a better predictive power (AUC: 0.879 vs 0.617, P<0.001).
CONCLUSIONS: This novel risk score model effectively predicted the presence of LASEC in non-anticoagulated patients with NVAF.
Keywords: Atrial Fibrillation, nomograms, Thrombosis, Cross-Sectional Studies, Echocardiography, Transesophageal, Female, Heart Atria, Humans, ischemic stroke, Male, Predictive Value of Tests, Risk Assessment
Background
In clinical practice, atrial fibrillation (AF) is associated with a substantial risk of morbidity and mortality [1]. One of the most serious complications of AF is thromboembolism. AF increases the risk of ischemic stroke by 5-fold [1], and 15% to 25% of ischemic strokes are associated with AF [2]. Left atrial spontaneous echo contrast (LASEC) is relatively common in patients with AF [3]. In addition, LASEC is a risk factor for left atrial thrombus (LAT) formation and an indicator of stroke events [4]. The prediction of LASEC may contribute to stroke risk stratification and early stroke prevention in patients with NVAF.
The CHA2DS2-VASc scoring system is recommended to evaluate the risk of stroke in patients with NVAF [1]. Some studies have shown that the CHA2DS2-VASc scoring system can be useful in predicting LASEC, but its predictive power may be modest [5–9]. Therefore, a new method to predict LASEC is needed. The aim of this retrospective study from a single center including 1255 non-anticoagulated patients with nonvalvular atrial fibrillation (NVAF) was to establish a novel risk score model to determine the risk of ischemic stroke associated with LASEC on transesophageal echocardiography (TEE).
Material and Methods
STUDY POPULATION:
This retrospective cross-sectional study enrolled 1255 consecutive hospitalized patients with NVAF at Beijing Anzhen Hospital between January 2019 and July 2019. All patients underwent TEE and transthoracic echocardiography (TTE) before catheter ablation or left atrial appendage (LAA) occlusion. The exclusion criteria were valvular heart disease, a history of valvuloplasty or valve replacement, complex congenital heart disease, recent ischemic stroke, deep venous thrombosis, pulmonary embolism, active inflammatory diseases, severe liver or renal dysfunction, previous long-term anticoagulant therapy, and lack of necessary data. The study was conducted in accordance with the Declaration of Helsinki and was approved by the Ethics Committee of Beijing Anzhen Hospital (approval No. 2021103X). Informed consent was obtained from all participants.
DATA COLLECTION:
Clinical characteristics were collected from the electronic medical records system of Beijing Anzhen Hospital and included the following: demographic data (age, sex, height, and weight), medical history (congestive heart failure, hypertension, diabetes mellitus, previous stroke/transient ischemic attack [TIA], vascular disease, prior myocardial infarction, and coronary artery disease), biochemical parameters (C-reactive protein [CRP], uric acid, D-dimer, creatinine, fibrinogen, and homocysteine), and echocardiographic parameters (left ventricular ejection fraction [LVEF], left atrial diameter [LAD], and left ventricular end diastolic diameter). AF was diagnosed based on the patient’s medical history and a standard 12-lead electrocardiogram and/or Holter monitoring. The definition and classification of AF was based on published guidelines [1]. Non-paroxysmal AF included persistent AF and long-standing persistent AF. The CHA2DS2-VASc score (congestive heart failure, hypertension, age ≥75 years, diabetes mellitus, stroke, vascular disease, age 65–74 years, sex category [female]), with a maximum value of 9 points, was calculated for each patient by the adding the points from the following risk factors: congestive heart failure, hypertension, age of 65–74 years, diabetes mellitus, vascular disease, or female sex (1 point each); and age ≥75 years or previous stroke, TIA, or thromboembolism (2 points each) [1]. Peripheral venous blood samples were collected after overnight fasting, and biochemical parameters were determined using standard laboratory methods at the central laboratory of Beijing Anzhen Hospital.
TTE AND TEE:
TTE and TEE were performed using a General Electric Vivid E9 ultrasound system according to standard practice guidelines [10,11]. Left atrial dimension was measured in the parasternal long-axis view at the end of left ventricular systole. LVEF was calculated using the modified Simpson’s rule in the apical 2- and 4-chamber views. Left atrial enlargement (LAE) was defined as an LAD >40 mm. Left ventricular systolic dysfunction was defined as an LVEF <50%.
Prior to TEE, patients fasted for 6 h and received local pharyngeal anesthesia. TEE was performed using a Philips X7-2t transesophageal probe inserted 25 to 35 cm into the esophagus. The left atrium (LA) and LAA were inspected in different tomographic planes, from 0° to 180°, to detect the presence of LASEC. LASEC was defined as dynamic “smoke-like” echoes in the LA chamber/LAA with characteristic swirling motions that could not be eliminated by changing the gain settings [3]. All examinations were performed by experienced echocardiographers, and all TEE images were independently reviewed by 2 experienced echocardiographers who were blinded to the study protocol.
STATISTICAL ANALYSIS:
Normally distributed continuous variables are expressed as mean±standard deviation. Non-normally distributed variables are presented as medians (interquartile ranges), and categorical variables are expressed as frequencies (percentages). Inter-group comparisons of continuous variables were performed using the
Results
CHARACTERISTICS OF THE STUDY POPULATION:
A total of 1255 non-anticoagulated patients with NVAF (68.5% men) with a mean age of 59.75±10.23 years were enrolled. The mean CHA2DS2-VASc score was 1.62±1.33. LASEC was observed in 139 (11.1%) patients. The characteristics of patients with and without LASEC are shown in Table 1. There were no significant differences between the 2 groups in terms of sex, age ≥75 years, age 65–74 years, and antiplatelet agent use or in frequency of hypertension, diabetes mellitus, vascular disease, or coronary artery disease. The patients with LASEC were relatively older, with higher body mass index and CHA2DS2-VASc scores than patients without LASEC. The frequency of non-paroxysmal AF, congestive heart failure, and previous stroke/TIA were significantly higher in patients with LASEC. In addition, patients with LASEC had higher levels of CRP, uric acid, and homocysteine, lower levels of eGFR, and similar levels of D-dimer, and creatinine, compared with patients without LASEC. Patients with LASEC also had significantly larger LAD, more LAE, and lower LVEF than patients without LASEC.
INDEPENDENT PREDICTORS OF LASEC:
The results of the univariate and multivariate logistic regression analyses are presented in Tables 2 and 3. Increased age, congestive heart failure, previous stroke/TIA, non-paroxysmal AF, LAE, LVEF <50%, and higher levels of CRP, uric acid, homocysteine, and eGFR were associated with the risk of LASEC. Furthermore, the independent predictors for LASEC were increased age, non-paroxysmal AF, previous stroke/TIA, congestive heart failure, and LAE. These variables were included in the final multivariate logistic regression model (Table 4).
CONSTRUCTION OF THE NEW RISK SCORE MODEL:
Using the independent predictors identified in the multivariable logistic regression analysis, a nomogram was generated to predict LASEC, and a weighted score ranging from 0 to 100 was assigned to each of the variables (Figure 1). To use the nomogram, each variable was located on the corresponding variable axis, and the number of points for each variable was determined by drawing a vertical line upward to the “Points” axis. Then, the total points were calculated by adding the number of points for all the variables. To locate the sum numbers on the “Total Points” axis, a vertical line was drawn down to the “Risk” axis to determine the risk of LASEC. According to the new risk score model, patients were divided into low-, moderate-, and high-risk groups (0–150, 150–200, and 200–350 points, respectively) with a LASEC incidence of 2.3%, 27.5%, and 55.3%, respectively. Patients with scores of 200 to 350 had a significantly higher risk of LASEC than patients with scores of 150–200 or 0–150 points (P<0.001) (Figure 2).
PREDICTIVE PERFORMANCE OF THE NEW RISK SCORE MODEL:
To assess the ability of the new risk score model and the CHA2DS2-VASc score to predict LASEC, ROC curve analysis was performed. The area under the curve (AUC) of the risk score model was 0.879 (95% confidence interval [CI] 0.849–0.909, P<0.001), with a sensitivity of 85.61% and specificity of 80.47. Thus, the new risk score demonstrated good predictive power for occurrence of LASEC. In contrast, the CHA2DS2-VASc score showed a relatively low predictive power (AUC 0.617, sensitivity 61.1, specificity 55.2, 95% CI 0.568–0.666, P<0.001). Pairwise comparison of the ROC curves showed that the new risk score model had a significantly larger AUC and demonstrated a better predictive value than the CHA2DS2-VASc score (AUC 0.879 vs 0.617, P<0.001) (Figure 3).
Discussion
LIMITATIONS:
The present study had several limitations. First, this was a single-center study, and the sample size was relatively small, which may have underpowered the results. In the future, multicenter studies with larger sample sizes are needed. Second, this was a retrospective, cross-sectional study, and the potential causal relationship could not be determined. Third, most of the study population was eligible for AF catheter ablation, creating a selection bias in our study; our study’s population might not represent the general population with NVAF. In addition, these patients had relatively low CHA2DS2-VASC scores and were not on anticoagulation, which would affect the correlation between the assumed predictive score model and the CHA2DS2-VASC score model. Fourth, we did not establish a validation group to verify the accuracy of the risk score model, and future external validations in a different cohort are needed.
Conclusions
In conclusion, our study demonstrated that increased age, non-paroxysmal AF, previous stroke/TIA, congestive heart failure, and LAE were independent predictors of LASEC. The new risk score model combining the above predictors could precisely predict the presence of LASEC in non-anticoagulated patients with NVAF, which may help us to optimize the stroke risk stratification and early stroke prevention in these patients. Further prospective, multicenter studies with larger populations are needed to confirm the predictive value of our new scoring model for LASEC and subsequent thromboembolic events.
Figures
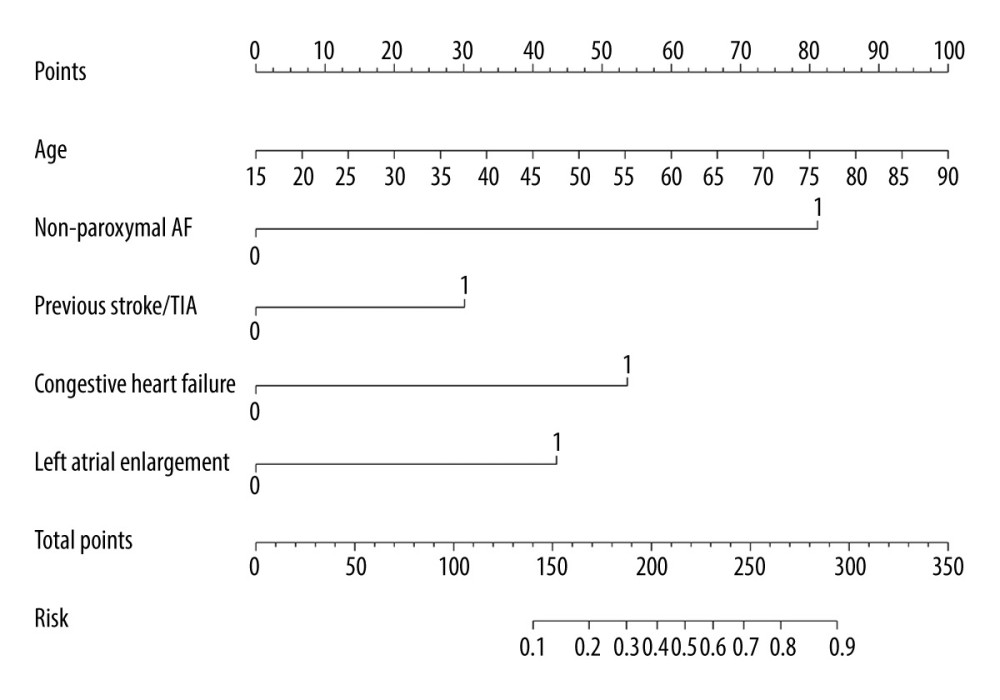 Figure 1. Nomogram for assessing the risk of left atrial spontaneous echo contrast (LASEC) in patients with nonvalvular atrial fibrillation (NVAF). To use the nomogram, each variable was located on the corresponding variable axis, the number of points for each variable was determined by drawing a vertical line upward to the “Points” axis. Then, the total points were calculated by adding the number of points for all the variables. The sum numbers were located on the “Total Points” axis, and a vertical line was drawn down to the “Risk” axis to determine the risk of LASEC. AF – atrial fibrillation; TIA – transient ischemic attack. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe Inc.).
Figure 1. Nomogram for assessing the risk of left atrial spontaneous echo contrast (LASEC) in patients with nonvalvular atrial fibrillation (NVAF). To use the nomogram, each variable was located on the corresponding variable axis, the number of points for each variable was determined by drawing a vertical line upward to the “Points” axis. Then, the total points were calculated by adding the number of points for all the variables. The sum numbers were located on the “Total Points” axis, and a vertical line was drawn down to the “Risk” axis to determine the risk of LASEC. AF – atrial fibrillation; TIA – transient ischemic attack. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe Inc.). 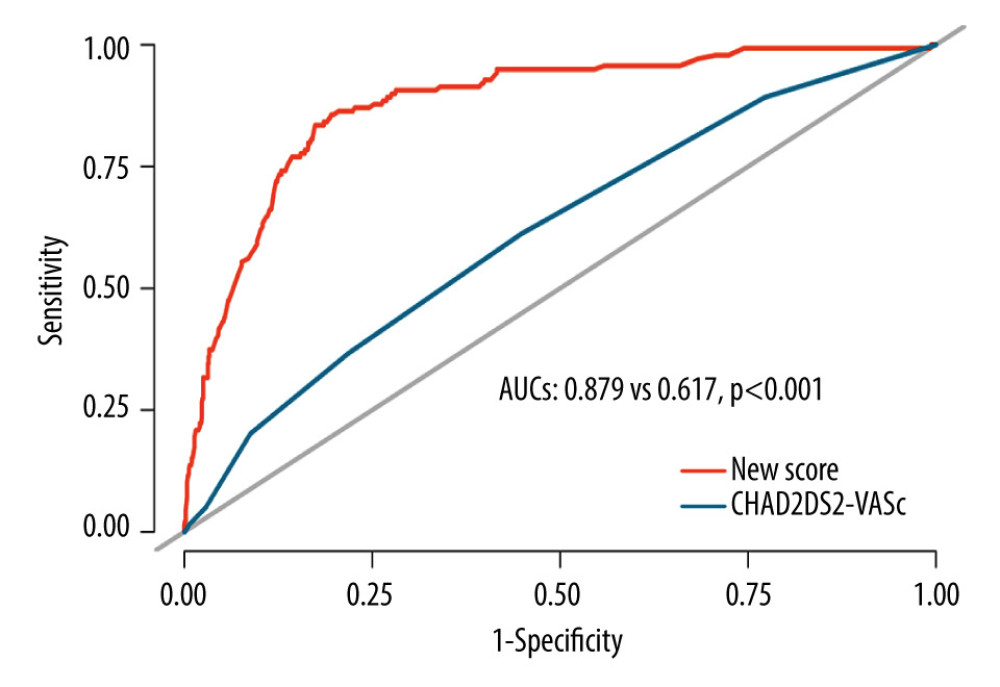 Figure 3. Receiver operating characteristic (ROC) curve analysis for assessing the predictive value of our new score and CHA2DS2-VASc score in predicting left atrial spontaneous echo contrast (LASEC). AUC – area under the curve. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe, Inc.).
Figure 3. Receiver operating characteristic (ROC) curve analysis for assessing the predictive value of our new score and CHA2DS2-VASc score in predicting left atrial spontaneous echo contrast (LASEC). AUC – area under the curve. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe, Inc.). 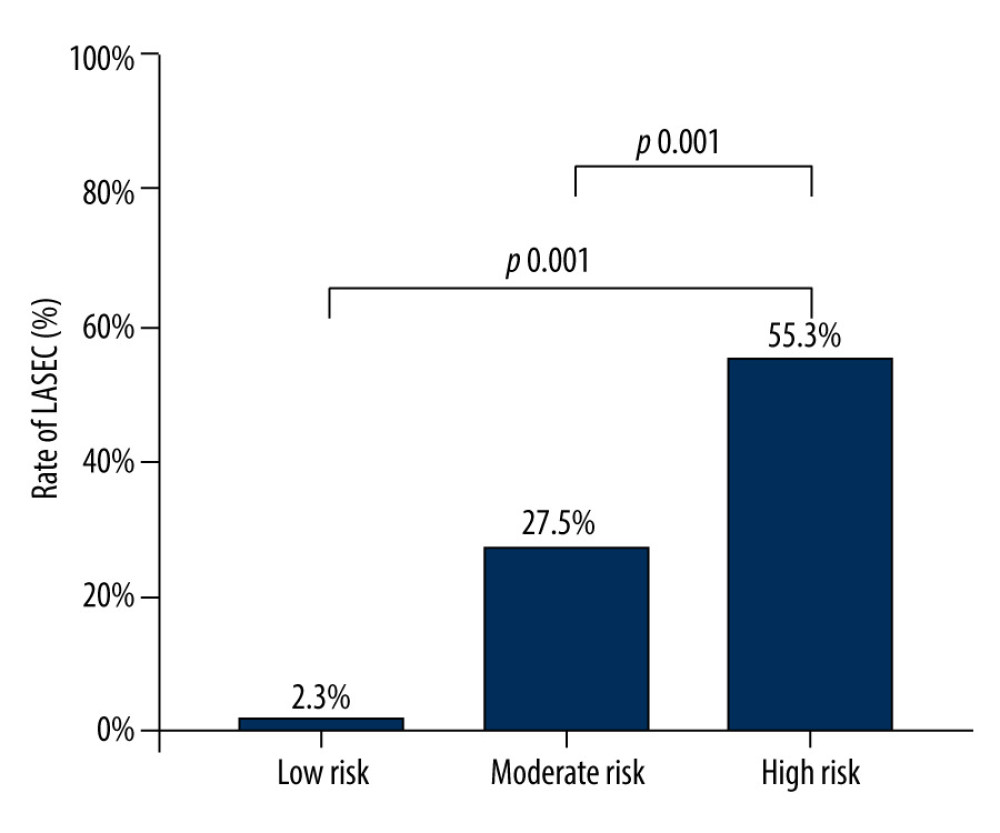 Figure 2. Incidence of left atrial spontaneous echo contrast (LASEC) stratified by 3 subgroups according to the new score levels. Low risk (0–150), moderate risk (150–200), high risk (200–350). (Adobe Illustrator, version 2020, Adobe, Inc.).
Figure 2. Incidence of left atrial spontaneous echo contrast (LASEC) stratified by 3 subgroups according to the new score levels. Low risk (0–150), moderate risk (150–200), high risk (200–350). (Adobe Illustrator, version 2020, Adobe, Inc.). Tables
Table 1. Baseline clinical characteristics of patients with and without left atrial spontaneous echo contrast.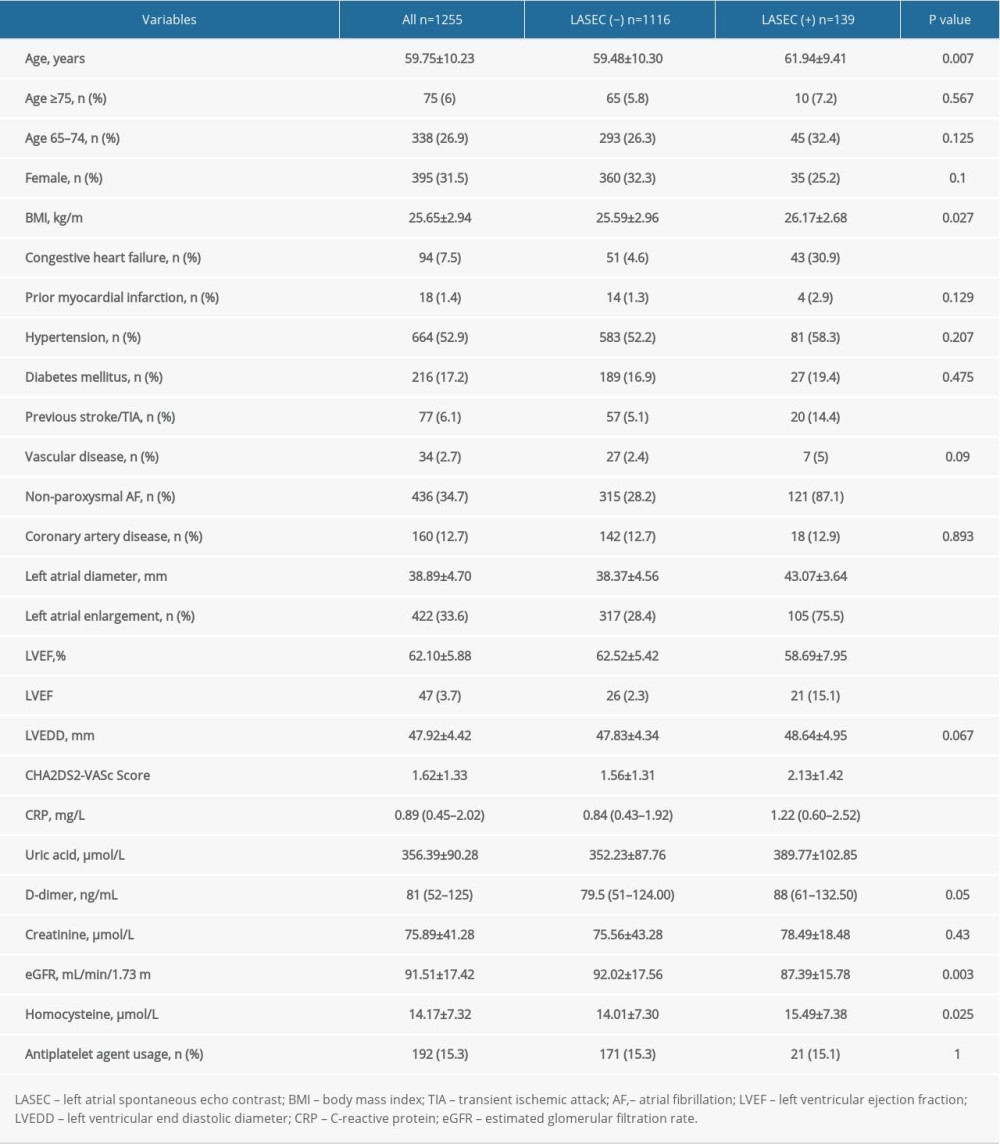 Table 2. Predictors of left atrial spontaneous echo contrast on univariate logistic analysis.
Table 2. Predictors of left atrial spontaneous echo contrast on univariate logistic analysis.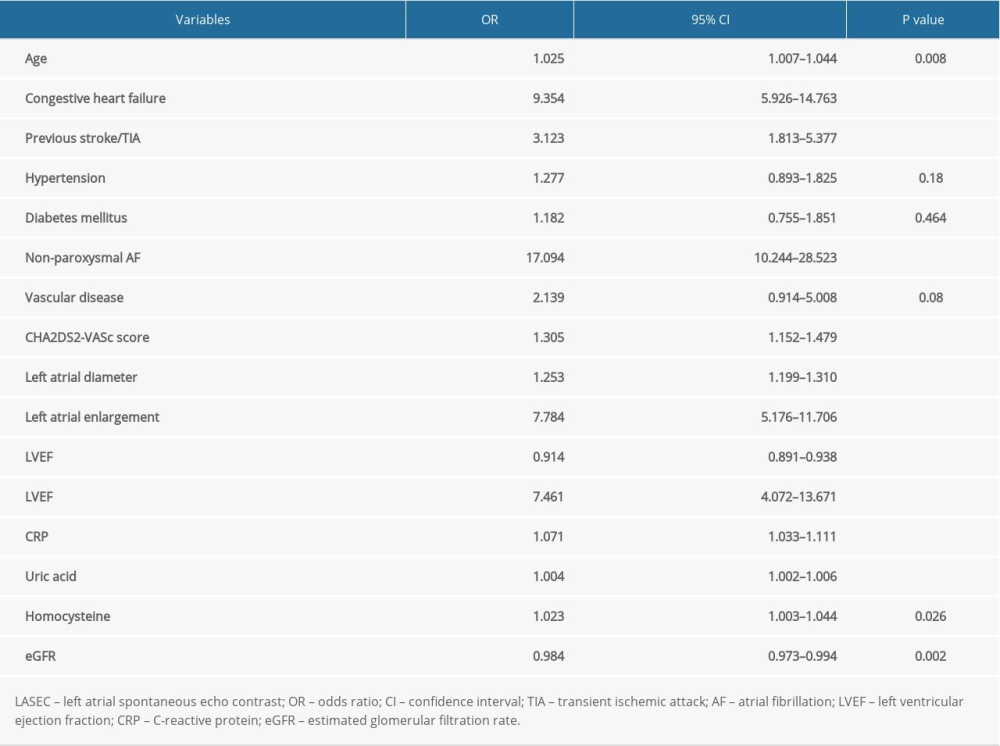 Table 3. Independent predictors of left atrial spontaneous echo contrast on multivariate logistic analysis.
Table 3. Independent predictors of left atrial spontaneous echo contrast on multivariate logistic analysis.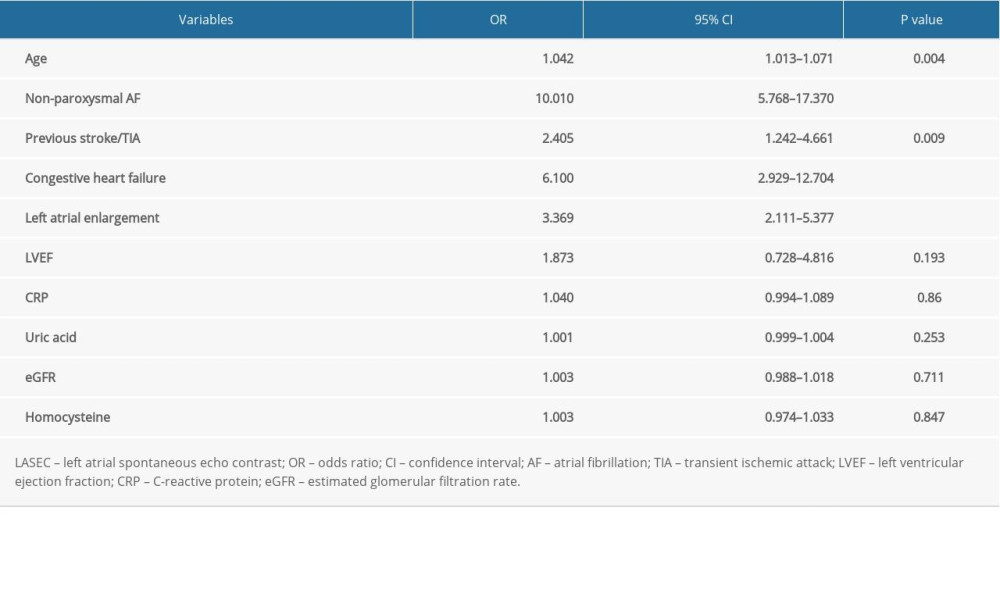 Table 4. Multivariate analysis for the construction of the new scoring model.
Table 4. Multivariate analysis for the construction of the new scoring model.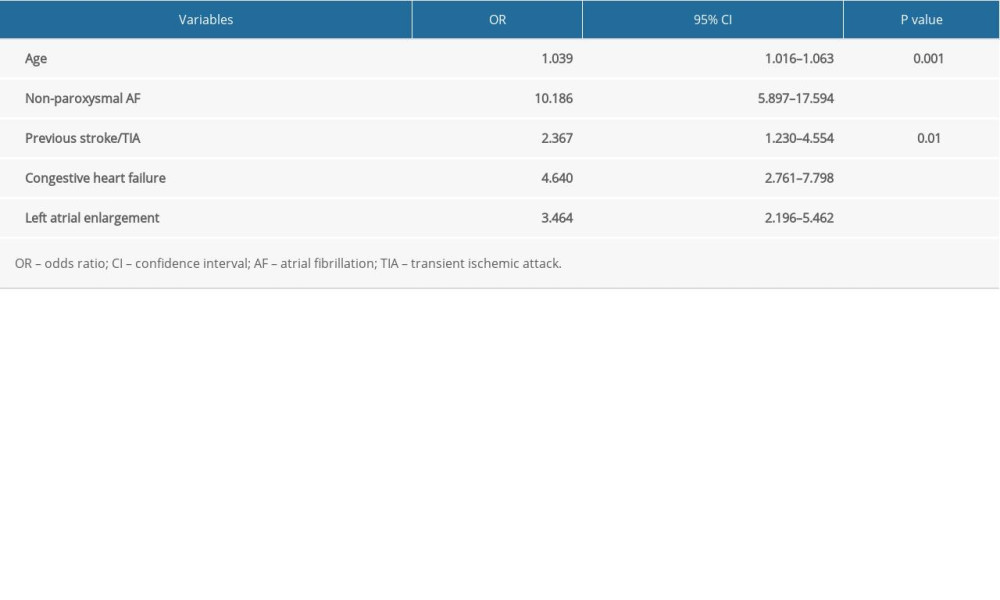
References
1. Hindricks G, Potpara T, Dagres N, 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): The Task Force for the diagnosis and management of atrial fibrillation of the European Society of Cardiology (ESC) Developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC: Eur Heart J, 2021; 42(5); 373-498
2. Hendriks JM, de Wit R, Vrijhoef HJ, An integrated chronic care program for patients with atrial fibrillation: study protocol and methodology for an ongoing prospective randomised controlled trial: Int J Nurs Stud, 2010; 47(10); 1310-16
3. Black IW, Hopkins AP, Lee LC, Walsh WF, Left atrial spontaneous echo contrast: A clinical and echocardiographic analysis: J Am Coll Cardiol, 1991; 18(2); 398-404
4. Leung DY, Black IW, Cranney GB, Prognostic implications of left atrial spontaneous echo contrast in nonvalvular atrial fibrillation: J Am Coll Cardiol, 1994; 24(3); 755-62
5. Han D, Chu Y, Wu Y, Wang X, Determinants of left atrial thrombus or spontaneous echo contrast in nonvalvular atrial fibrillation: Thromb Res, 2020; 195; 233-37
6. Huang J, Liao HT, Fei HW, Association of thromboembolic risk score with left atrial thrombus and spontaneous echocardiographic contrast in non-anticoagulated nonvalvular atrial fibrillation patients: Cardiology, 2018; 140(2); 87-95
7. Providência R, Botelho A, Trigo J, Possible refinement of clinical thromboembolism assessment in patients with atrial fibrillation using echocardiographic parameters: Europace, 2012; 14(1); 36-45
8. Mascioli G, Lucca E, Michelotti F, Severe spontaneous echo contrast/auricolar thrombosis in “nonvalvular” AF: Value of thromboembolic risk scores: Pacing Clin Electrophysiol, 2017; 40(1); 57-62
9. Ning W, Li Y, Ma C, The refinement of risk stratification for atrial thrombus or spontaneous echo contrast in nonvalvular atrial fibrillation: Int Heart J, 2017; 58(6); 885-93
10. Mitchell C, Rahko PS, Blauwet LA, Guidelines for performing a comprehensive transthoracic echocardiographic examination in adults: Recommendations from the American Society of Echocardiography: J Am Soc Echocardiogr, 2019; 32(1); 1-64
11. Hahn RT, Abraham T, Adams MS, Guidelines for performing a comprehensive transesophageal echocardiographic examination: Recommendations from the American Society of Echocardiography and the Society of Cardiovascular Anesthesiologists: J Am Soc Echocardiogr, 2013; 26(9); 921-64
12. Kodani E, Akao M, Atrial fibrillation and stroke prevention: state of the art-epidemiology and pathophysiology: New risk factors, concepts and controversies: Eur Heart J Suppl, 2020; 22(Suppl O); O1-O13
13. Fatkin D, Kelly RP, Feneley MP, Relations between left atrial appendage blood flow velocity, spontaneous echocardiographic contrast and thromboembolic risk in vivo: J Am Coll Cardiol, 1994; 23(4); 961-69
14. Bernhardt P, Schmidt H, Hammerstingl C, Patients with atrial fibrillation and dense spontaneous echo contrast at high risk a prospective and serial follow-up over 12 months with transesophageal echocardiography and cerebral magnetic resonance imaging: J Am Coll Cardiol, 2005; 45(11); 1807-12
15. Soulat-Dufour L, Lang S, Etienney A, Correlation between left atrial spontaneous echocardiographic contrast and 5-year stroke/death in patients with non-valvular atrial fibrillation: Arch Cardiovasc Dis, 2020; 113(8–9); 525-33
16. Wang F, Zhu M, Wang X, Predictive value of left atrial appendage lobes on left atrial thrombus or spontaneous echo contrast in patients with non-valvular atrial fibrillation: BMC Cardiovasc Disord, 2018; 18(1); 153
17. Kizawa S, Ito T, Akamatsu K, Chronic kidney disease as a possible predictor of left atrial thrombogenic milieu among patients with nonvalvular atrial fibrillation: Am J Cardiol, 2018; 122(12); 2062-67
18. Akamatsu K, Ito T, Ozeki M, Left atrial spontaneous echo contrast occurring in patients with low CHADS2 or CHA2DS2-VASc scores: Cardiovasc Ultrasound, 2020; 18(1); 31
19. Lin WD, Xue YM, Liu FZ, Left atrial enlargement and non-paroxysmal atrial fibrillation as risk factors for left atrial thrombus/spontaneous echo contrast in patients with atrial fibrillation and low CHA2DS2-VASc score: J Geriatr Cardiol, 2020; 17(3); 155-59
20. Kishima H, Mine T, Fukuhara E, Predictors of left atrial thrombi and spontaneous echocardiographic contrast in the acute phase after cardioembolic stroke in patients with atrial fibrillation: J Stroke Cerebrovasc Dis, 2019; 28(6); 1571-77
21. Zabalgoitia M, Halperin JL, Pearce LA, Transesophageal echocardiographic correlates of clinical risk of thromboembolism in nonvalvular atrial fibrillation. Stroke Prevention in Atrial Fibrillation III Investigators: J Am Coll Cardiol, 1998; 31(7); 1622-26
22. Black IW, Spontaneous echo contrast: Where there’s smoke there’s fire: Echocardiography, 2000; 17(4); 373-82
23. Habara S, Dote K, Kato M, Prediction of left atrial appendage thrombi in non-valvular atrial fibrillation: Eur Heart J, 2007; 28(18); 2217-22
24. Boldt A, Wetzel U, Lauschke J, Fibrosis in left atrial tissue of patients with atrial fibrillation with and without underlying mitral valve disease: Heart, 2004; 90(4); 400-5
25. Goette A, Kalman JM, Aguinaga L, EHRA/HRS/APHRS/SOLAECE expert consensus on atrial cardiomyopathies: Definition, characterization, and clinical implication: Heart Rhythm, 2017; 14(1); e3-e40
26. Daccarett M, Badger TJ, Akoum N, Association of left atrial fibrosis detected by delayed-enhancement magnetic resonance imaging and the risk of stroke in patients with atrial fibrillation: J Am Coll Cardiol, 2011; 57(7); 831-38
27. Kim YG, Shim J, Boo KY, Different influence of cardiac hemodynamics on thromboembolic events in patients with paroxysmal and non-paroxysmal atrial fibrillation: PLoS One, 2019; 14(3); e0214743
28. Li-Saw-Hee FL, Blann AD, Gurney D, Lip GY, Plasma von Willebrand factor, fibrinogen and soluble P-selectin levels in paroxysmal, persistent and permanent atrial fibrillation. Effects of cardioversion and return of left atrial function: Eur Heart J, 2001; 22(18); 1741-47
29. Frenkel D, D’Amato SA, Al-Kazaz M, Prevalence of left atrial thrombus detection by transesophageal echocardiography: A comparison of continuous non-vitamin K antagonist oral anticoagulant versus warfarin therapy in patients undergoing catheter ablation for atrial fibrillation: JACC Clin Electrophysiol, 2016; 2(3); 295-303
30. Hamatani Y, Ogawa H, Takabayashi K, Left atrial enlargement is an independent predictor of stroke and systemic embolism in patients with non-valvular atrial fibrillation: Sci Rep, 2016; 6; 31042
31. Tabata T, Oki T, Fukuda N, Influence of left atrial pressure on left atrial appendage flow velocity patterns in patients in sinus rhythm: J Am Soc Echocardiogr, 1996; 9(6); 857-64
32. Benjamin EJ, D’Agostino RB, Belanger AJ, Left atrial size and the risk of stroke and death. The Framingham Heart Study: Circulation, 1995; 92(4); 835-41
33. Gupta DK, Shah AM, Giugliano RP, Left atrial structure and function in atrial fibrillation: ENGAGE AF-TIMI 48: Eur Heart J, 2014; 35(22); 1457-65
34. Boriani G, Botto GL, Padeletti L, Improving stroke risk stratification using the CHADS2 and CHA2DS2-VASc risk scores in patients with paroxysmal atrial fibrillation by continuous arrhythmia burden monitoring: Stroke, 2011; 42(6); 1768-70
35. Lip GY, Nieuwlaat R, Pisters R, Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: The euro heart survey on atrial fibrillation: Chest, 2010; 137(2); 263-72
36. Borre ED, Goode A, Raitz G, Predicting thromboembolic and bleeding event risk in patients with non-valvular atrial fibrillation: A systematic review: Thromb Haemost, 2018; 118(12); 2171-87
37. Yang PS, Pak HN, Park DH, Non-cardioembolic risk factors in atrial fibrillation-associated ischemic stroke: PLoS One, 2018; 13(7); e0201062
38. Ito T, Suwa M, Left atrial spontaneous echo contrast: Relationship with clinical and echocardiographic parameters: Echo Res Pract, 2019; 6(2); R65-73
Figures
 Figure 1. Nomogram for assessing the risk of left atrial spontaneous echo contrast (LASEC) in patients with nonvalvular atrial fibrillation (NVAF). To use the nomogram, each variable was located on the corresponding variable axis, the number of points for each variable was determined by drawing a vertical line upward to the “Points” axis. Then, the total points were calculated by adding the number of points for all the variables. The sum numbers were located on the “Total Points” axis, and a vertical line was drawn down to the “Risk” axis to determine the risk of LASEC. AF – atrial fibrillation; TIA – transient ischemic attack. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe Inc.).
Figure 1. Nomogram for assessing the risk of left atrial spontaneous echo contrast (LASEC) in patients with nonvalvular atrial fibrillation (NVAF). To use the nomogram, each variable was located on the corresponding variable axis, the number of points for each variable was determined by drawing a vertical line upward to the “Points” axis. Then, the total points were calculated by adding the number of points for all the variables. The sum numbers were located on the “Total Points” axis, and a vertical line was drawn down to the “Risk” axis to determine the risk of LASEC. AF – atrial fibrillation; TIA – transient ischemic attack. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe Inc.). Figure 3. Receiver operating characteristic (ROC) curve analysis for assessing the predictive value of our new score and CHA2DS2-VASc score in predicting left atrial spontaneous echo contrast (LASEC). AUC – area under the curve. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe, Inc.).
Figure 3. Receiver operating characteristic (ROC) curve analysis for assessing the predictive value of our new score and CHA2DS2-VASc score in predicting left atrial spontaneous echo contrast (LASEC). AUC – area under the curve. (R programming language, version 3.6.1, R Foundation) (Adobe Illustrator, version 2020, Adobe, Inc.). Figure 2. Incidence of left atrial spontaneous echo contrast (LASEC) stratified by 3 subgroups according to the new score levels. Low risk (0–150), moderate risk (150–200), high risk (200–350). (Adobe Illustrator, version 2020, Adobe, Inc.).
Figure 2. Incidence of left atrial spontaneous echo contrast (LASEC) stratified by 3 subgroups according to the new score levels. Low risk (0–150), moderate risk (150–200), high risk (200–350). (Adobe Illustrator, version 2020, Adobe, Inc.). Tables
 Table 1. Baseline clinical characteristics of patients with and without left atrial spontaneous echo contrast.
Table 1. Baseline clinical characteristics of patients with and without left atrial spontaneous echo contrast. Table 2. Predictors of left atrial spontaneous echo contrast on univariate logistic analysis.
Table 2. Predictors of left atrial spontaneous echo contrast on univariate logistic analysis. Table 3. Independent predictors of left atrial spontaneous echo contrast on multivariate logistic analysis.
Table 3. Independent predictors of left atrial spontaneous echo contrast on multivariate logistic analysis. Table 4. Multivariate analysis for the construction of the new scoring model.
Table 4. Multivariate analysis for the construction of the new scoring model. Table 1. Baseline clinical characteristics of patients with and without left atrial spontaneous echo contrast.
Table 1. Baseline clinical characteristics of patients with and without left atrial spontaneous echo contrast. Table 2. Predictors of left atrial spontaneous echo contrast on univariate logistic analysis.
Table 2. Predictors of left atrial spontaneous echo contrast on univariate logistic analysis. Table 3. Independent predictors of left atrial spontaneous echo contrast on multivariate logistic analysis.
Table 3. Independent predictors of left atrial spontaneous echo contrast on multivariate logistic analysis. Table 4. Multivariate analysis for the construction of the new scoring model.
Table 4. Multivariate analysis for the construction of the new scoring model. In Press
Clinical Research
Institutional and Regional Variations in Access to Clinical Trials and Next-Generation Sequencing in Turkis...Med Sci Monit In Press; DOI: 10.12659/MSM.951027
Clinical Research
Low-Intensity Blood Flow-Restricted Multi-Joint Exercise Improves Muscle Function in Patients With Patellof...Med Sci Monit In Press; DOI: 10.12659/MSM.950516
Review article
Musculoskeletal Ultrasound and MRI in the Evaluation of Chemotherapy-Induced Peripheral Neuropathy: A ReviewMed Sci Monit In Press; DOI: 10.12659/MSM.951283
Clinical Research
Sensory Processing, Dissociation, and Affective Symptoms in Misophonia: A Cross-Sectional Study of 35 AdultsMed Sci Monit In Press; DOI: 10.12659/MSM.950938
Most Viewed Current Articles
17 Jan 2024 : Review article 10,187,196
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
13 Nov 2021 : Clinical Research 3,708,487
Acceptance of COVID-19 Vaccination and Its Associated Factors Among Cancer Patients Attending the Oncology ...DOI :10.12659/MSM.932788
Med Sci Monit 2021; 27:e932788
14 Dec 2022 : Clinical Research 2,341,643
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research 706,524
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387








